Archives of Clinical Nephrology
Peritoneal catheter survival: The impact of unroofing
Barone RJ1-3*, Beresan M3, Pattin M2, Gimenez NS2, Berga G3, Santopietro M2 and Ramirez L2
2Ex Renal Therapy Services Hurlingham SRL, Buenos Aires, Argentina
3Center for Kidney Diseases and Arterial Hypertension (CEREHA), Argentina
Cite this as
Barone RJ, Beresan M, Pattin M, Gimenez NS, Berga G, et al. (2017) Peritoneal catheter survival: The impact of unroofing. Arch Clin Nephrol 3(1): 053-056. DOI: 10.17352/acn.000027Background: Unroofing is a controversial procedure to avoid catheter removal in the treatment of the chronic exit site and tunnel infection, but is now rarely recommended. Here we aimed to evaluate the effects of the unroofing procedure on peritoneal catheter survival.
Methods: From our database, we prospectively evaluated the outcome of 139 peritoneal catheters placed in 121 patients (1.14 catheters per patient, 73 female, 48 male) from 08-03-1993 to 12-31-2016. Twenty-three infected catheters needed surgical unroofing of the tunnel tract. We calculated the cumulative catheter survival rates (Kaplan-Meier) of 1) overall catheters and 2) not unroofed catheters, considering catheter removal as an endpoint. We also calculated 3) the unroofed catheter survival, considering the date of unroofing or catheter removal as the endpoint and, 4) continuity of the unroofed catheters post-unroofing, considering the unroofing date as if it were a new catheter and catheter removal as the endpoint. Likewise, we compared the survival of: a) unroofed catheters vs. continuity of the unroofed catheters and, b) no unroofed catheters vs. continuity of the unroofed catheters (Log-rank test) (significance value P< 0.05).
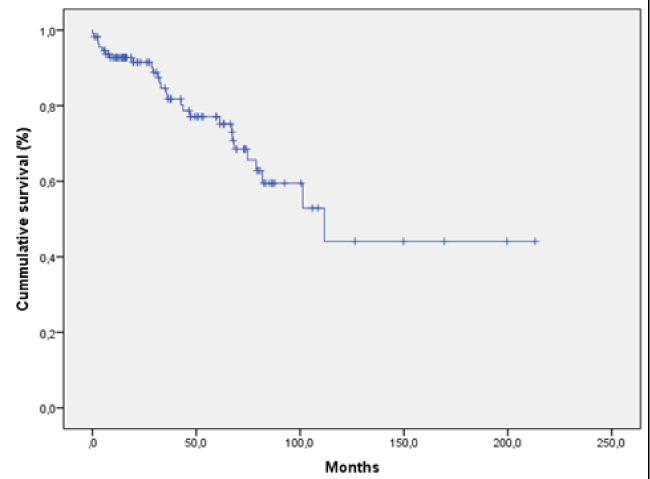
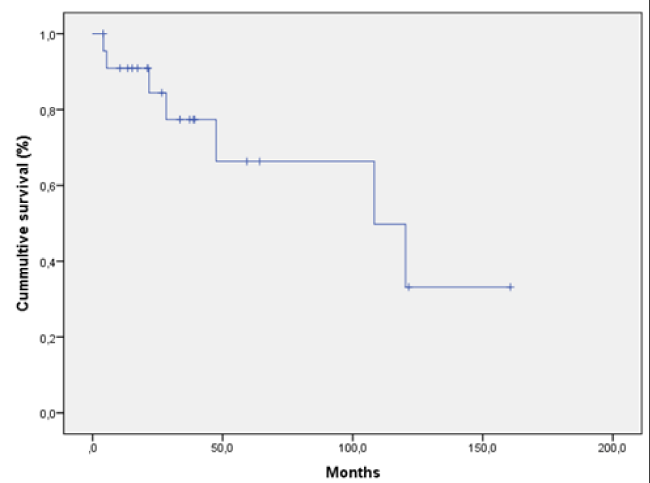
Results: 1) The overall catheter survival rates were 94%, 84%, 76%, 55%, 40% and 26% at 12, 36, 60, 84, 120 and 210 months respectively. 2) The not unroofed catheter survival rates were 93%, 83%, 77%, 59%, 44% and 44% at 12, 36, 60, 84, 120 and 210 months respectively. 3) The unroofed catheter survival rates were 84%, 53%, 31%, 23% and 9% at 12, 36, 60, 84 and 120 months respectively. 4) The post-unroofed catheters survival rates were 91%, 77%, 66%, 66%, 50% and 33% at 12, 36, 60, 84, 120 and 160 months respectively. We detected a statistical significance when comparing unroofed catheters vs. continuity of the unroofed catheters and no statistical significance was observed when comparing not unroofed catheters vs. continuity of the unroofed catheters post-unroofed.
Conclusion: The overall catheter survival was satisfactory. Unroofing contributed significantly in the lifespan of the catheters.
Introduction
Infection of the peritoneal catheter during peritoneal dialysis can facilitate entry of microorganisms into the peritoneal cavity, leading to peritonitis. Failure to cure these infections can lead to the removal of the peritoneal catheter and, thus, technique failure or other more severe scenarios. Likewise, frequent infections of the exit site, often chronic, generate the continuous use of antibiotics, facilitating the appearance of Gram-negative exit site infections and fungi peritonitis [1]. In the latest recommendations for International Society for Peritoneal Dialysis (ISPD) infectious complications for the catheter exit site, there is no mention of how to avoid the removal of peritoneal catheters in cases of chronic infections [2-4]. This procedure, known as unroofing of the peritoneal catheter, is nowadays rarely recommended.
Some articles have described the technical characteristics of the procedure and their outcomes in adult and paediatric patients, as well as other subcutaneous surgical techniques to avoid catheter removal, but no articles have investigated the long-term durability of unroofed catheters [5-9]. In this work, we share our experience of many years of follow-up in the evolution of our peritoneal catheters and the impact of the unroofing on catheter survival.
Materials and Methods
From our database, we prospectively evaluated the outcomes of 139 peritoneal catheters (34 Tenckhöff straight, 104 Swan Neck and 1 Missouri) placed in 121 adult patients (1.14 catheters per patient); 73 female, 48 male; mean age 52.97 ± 15.32-years-old; time at risk 6672 ± 48 patient months; 19% diabetics) during the period 08-03-1993 up to 12-31-2016. Twenty-three persistently infected catheters needed surgical unroofing of the tunnel tract. The unroofing procedure essencially consist by incising the skin from above the superficial cuff and the exteriorization of the subcutaneous external cuff removing the infected tissue many times helped by an electrosurgical knife. After sanitized the wound, absorbent monofilament threads are used to repair the subcutaneous tissue, finally, suture the skin [5]. In our protocol we do not shaving the exteriorized cuff.
We calculated the cumulative catheter survival using the Kaplan-Meier method of: 1) overall catheters, 2) not unroofed catheters, considering in (1) and (2) the catheter removal as an endpoint. Also, we measured 3) the unroofed catheter survival (considering the date of unroofing or catheter removal as an endpoint) and 4) continuity of the unroofed catheters post-unroofing, considering the unroofing date as if it were a new catheter and catheter removal as the endpoint. Death of the patients, renal transplant or transfer to another dialysis centre were censored. We compared the survival of: a) unroofed catheters vs. continuity of the unroofed catheters and b) no unroofed catheters vs. continuity of the unroofed catheters. To compare the survival curves, we used the log-rank test (significance value P< 0.05). We also used the Chi-Square test to analyse the proportion of unroofing between Tenckhöff and Swan Neck catheters (significance value P < 0.05). Data were analysed using the software IBM-SPSS statistic, version 24.
Results
Of the 139 peritoneal catheters placed during the study period, 23 (16.54%) with chronic refractory infection were unroofed. The overall catheter survival was 94%, 84%, 76%, 55%, 40% and 26% at 12, 36, 60, 84, 120 and 210 months respectively, (median survival time, 105.8 months; 95%CI, 74.5–137) (Figure 1). The survival rates of the not unroofed catheters were 93%, 83%, 77%, 59%, 44% and 44% at 12, 36, 60, 84, 120 and 210 months respectively (median survival time, 111.7 months; 95%CI, 70.4–153) (Figure 2). Unroofed catheter survival, using the date of unroofing or catheter removal as the endpoint, was 84%, 53%, 31%, 23% and 9% at 12, 36, 60, 84 and 120 months respectively (median survival time, 44.3 months; 95%CI, 27.3–61.2) (Figure 3). The evaluation of the post-unroofed catheters survival was 91%, 77%, 66%, 66%, 50% and 33% at 12, 36, 60, 84, 120 and 160 months respectively (median survival time, 108.3; 95%CI, 32.7–184) (Figure 4).
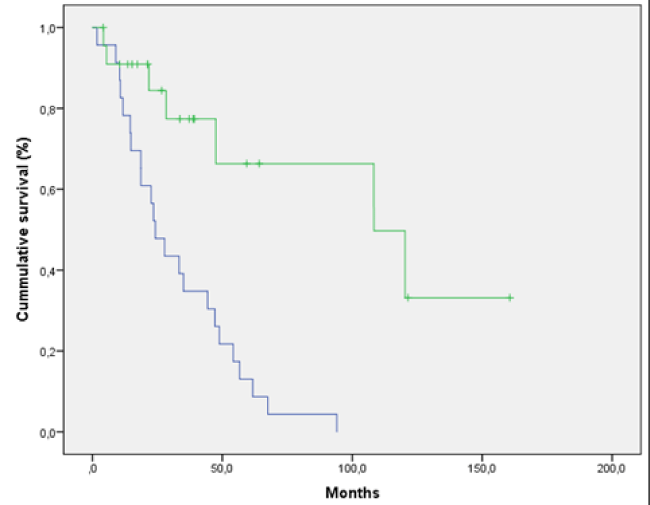
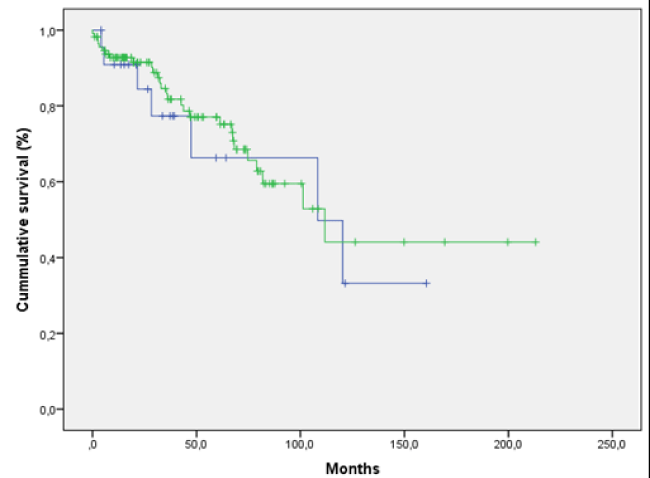
An important statistical significance was observed when comparing catheters before unroofing vs. continuity of these unroofed catheters post-unroofed (P <0.05) (Figure 5). No statistical significance was observed when comparing not unroofed catheters vs. continuity of the unroofed catheters post-unroofed (P = 0.64) (Figure 6).
Twelve out of 34 straight Tenckhöff and 11 of 104 Swan neck catheters required unroofing. Therefore, there was a greater need for this procedure in the former than the later catheters (χ² P <0.05).
Discussion
Similar to arteriovenous fistula survival for haemodialysis, catheter lifespan is an important indicator of the quality of the peritoneal dialysis programs. In patients undergoing chronic haemodialysis, the creation of a new arteriovenous fistula following vascular access failure likely has a different body sensation and uncertainty compared to the placement of a new peritoneal catheter for patients on peritoneal dialysis, especially when the indication of peritoneal dialysis was made because of the impossibility of continuing in haemodialysis. Since the beginning of the chronic peritoneal dialysis, the characteristic of the peritoneal catheters (length, shape, gauge, material, cuffs number, etc.), as well as their placement and survival, have been studied [9-11]. On the other hand, it is interesting to note that the survival rates of peritoneal catheters are equivalent to the survival of arteriovenous fistulas for haemodialysis [12-16].
During chronic treatments in which access to therapy depends on an artificial device, complications related to the material and methodology are inevitable. During peritoneal dialysis, patient compliance to the guidelines of care taught during the training of the technique is important.
Exit site infection is an important threat to catheter survival and, therefore, of the continuity of treatment in peritoneal dialysis. The therapy of this infection has been extensively studied in numerous articles and guidelines of the ISPD [17,18]. However, a known procedure to safeguard the peritoneal catheter, known as unroofing, has been little recommended due to disparate results, small samples of patients, and short follow-up periods [19-25].
During the evolution of our peritoneal dialysis program, we performed a thorough follow-up of catheter survival and the impact of the unroofing on the extension of the useful life of the catheters. We found that long-term overall catheter survival is satisfactory [9,26,27]. The survival of unroofed catheters (considering the date of the procedure as if day-zero of a new catheter) was similar to that of not unroofed catheters. Thus, there was a positive contribution of this procedure to the overall survival of catheters.
It is recognised that there are no differences in the outcomes when comparing different types of peritoneal catheters [28,29]. Shape memory of the peritoneal catheters has been implicated in the catheter migration process [30]. In a prospective randomised study, Lye and co-workers observed that the Swan neck configuration resulted in a significant reduction in the rate of exit-site infection [31]. In our study, it is important to highlight that the Tenckhöff catheters had the highest proportion of infected catheters that required unroofing; it seems likely that catheter migration related to the shape memory of the straight catheters will have facilitated the exit site erosion and secondary infection.
Conclusion
The overall long-term catheter survival rate was satisfactory. Unroofing contributed significantly to the lifespan of the catheters. This simple procedure should be considered in persistently infected catheters before deciding to remove the catheter.
- Piraino B, Bernardini J, Florio T, Fried L (2003) Staphylococcus aureus prophylaxis and trends in gram-negative infections in peritoneal dialysis patients. Perit Dial Int 23: 456-459. Link: https://goo.gl/f2Hvuq
- Li PK1, Szeto CC2, Piraino B3, de Arteaga J4, Fan S, et al. (2016) ISPD Peritonitis recommendations: 2016 update on prevention and treatment. Perit Dial Int 36: 481-508. Link: https://goo.gl/88B83p
- Nichols WK, Nolph KD (1983) A technique for managing exit-site and cuff infection in Tenckhöf catheter. Perit Dial Int 3: S 4-5.
- Andreoli SP, West KW, Grosfeld JL, Bergstein JM (1983) A technique to eradicate tunnel infection without peritoneal dialysis catheter removal. Perit Dial Int 1983; 3: S 4-5. Link: https://goo.gl/965a8K
- Terawaki H, Nakano H, Ogura M, Kadomura M, Hosoya T, Nakayama M (2013) Unroofing surgery with en bloc resection of the skin and tissues around the peripheral cuff. Perit Dial Int 33: 573-576. Link: https://goo.gl/pr24gL
- Sakurada T, Okamoto T, Oishi D, Koitabashi K, Sueki S, et al. (2014) Subcutaneous pathway diversion for peritoneal dialysis catheter salvage. Adv Perit Dial 30: 11-14. Link: https://goo.gl/pqzkAD
- Macchini F, Testa S, Valadè A, Torricelli M, Leva E, et al. (2009) Conservative surgical management of catheter infections in children on peritoneal dialysis. Pediatr Surg Int 25: 703-707. Link: https://goo.gl/ab7mKy
- Glickman JD1, Rafanello T, Gerhardt RE, Ntoso KA, Koethe JD, et al. (1996) Surgical treatment of persistent exit-site infections. Adv Perit Dial 12: 209-210. Link: https://goo.gl/fUUJqq
- Burkart JM (1988) Strategies for optimizing peritoneal dialysis catheter. Outcomes: Catheter implantation issues. J Am Soc Nephrol 9: S130-S136. Link: https://goo.gl/BvZ6ff
- Strippoli GF, Tong A, Johnson D, Schena FP, Craig JC (2004) Catheter-related interventions to prevent peritonitis in peritoneal dialysis: a systematic review of randomized, controlled trials. J Am Soc Nephrol 15: 2735-2746. Link: https://goo.gl/zfX8SS
- Hagen SM, Lafranca JA, IJzermans J NM, Dor F (2014) A systematic review and meta-analysis of the influence of peritoneal dialysis catheter type on complication rate and catheter survival. Kidney Int 85: 920-932. Link: https://goo.gl/dk8LdD
- Shrestha PC, Asher J, Shrestha SM, Jenner S, Wilson C, et al. (2007) Survival of arteriovenous fistula for dialysis at different centers in the North of England. J Vasc Access 8: 231-234. Link: https://goo.gl/6ks9vC
- Erkut B, Unlü Y, Ceviz M, Becit N, Ateş A, et al. (2006) Primary arteriovenous fistulas in the forearm for hemodialysis: effect of miscellaneous factors in fistula patency. Ren Fail 28: 275-281. Link: https://goo.gl/wm9pWw
- Prischl FC, Kirchgatterer A, Brandstätter E, Wallner M, Baldinger C, et al. (1995) Parameters of prognostic relevance to the patency of vascular access in hemodialysis patients. Am Soc Nephrol 6: 1613-1618. Link: https://goo.gl/hNGAwZ
- Rayner HC, Ronald L, Gillespie BW, Goodkin DA, Akiba T, et al. (2003) Creation, cannulation and survival of arteriovenous fistulae: Data from the Dialysis Outcomes and Practice Patterns Study. Kidney Int 63: 323–330. Link: https://goo.gl/W417t9
- Al-Jaishi AA, Oliver MJ, Thomas SM, Lok CE, Zhang JC, et al. (2014) Patency Rates of the Arteriovenous Fistula for Hemodialysis: A Systematic Review and Meta-analysis Patency Rates of the Arteriovenous Fistula for Hemodialysis: Am J Kidney Dis 63: 464-478. Link: https://goo.gl/r4U7Na
- Li PK, Szeto CC, Piraino B, Bernardini J, Figueiredo AE, et al. (2010) Peritoneal dialysis-related infections recommendations: 2010 update. Perit Dial Int 30: 393-423. Link: https://goo.gl/bdgSTj
- Akoh JA (2012) Peritoneal dialysis associated infection: An update on diagnosis and management. Wordl J. Nephrol 6: 106-122. Link: https://goo.gl/mPmg1X
- Piraino B, Bernardini J, Peitzman A, Sorkin M (1987) Failure of the peritoneal catheter cuff shaving to eradicate infection. Perit Dial Bull 7: 179-182. https://goo.gl/12eKFH
- Carranza L, Martínez CV, Garófalo R, Antonelli J, Barrón C, et al. (2015) Eficacia del destechado del túnel en infección crónica del catéter peritoneal. Revista de Nefrología, díálisis y trasplante 35: 65-69. Link: https://goo.gl/pgUi78
- Yoshino A, Honda M, Ikeda M, Tsuchida S, Hataya H, et al. (2004) Merit of the cuff-shaving procedure in children with tunnel infection. Pediatr Nephrol 19: 1267–1272. Link: https://goo.gl/sA495u
- Scalamogna A, De Vecchi A, Maccario M, Castelnovo C, Ponticelli C (1995) Cuff-shaving procedure. A rescue treatment for exit-site infection unresponsive to medical therapy. Nephrol Dial Transplant 10: 2325-2327. Link: https://goo.gl/S5fHX7
- Hussain MI, Al-Salamah SM, Aziz R, Al-Qahatani HH, Al-Ohay NY, et al. (2013) Outcome of open Tenckhoff catheter insertions: 5 years experience in a major tertiary centre in Central Saudi Arabia. J Ayub Med Coll Abbottabad 25(3-4). Link: https://goo.gl/Hf8CK6
- Suh H, Wadhwa NK, Cabralda T, Bonanno J, Wasiluk A, et al. (1997) Persistent exit-site/tunnel infection and subcutaneous cuff removal in PD patients. Adv Perit Dial 13: 233-236. Link: https://goo.gl/eCVef9
- Crabtree JH, Burchette RJ (2005) Surgical salvage of peritoneal dialysis catheters from chronic exit-site and tunnel infections. Am J Surg 190: 4-8. Link: https://goo.gl/kfNqmW
- Singh N1, Davidson I, Minhajuddin A, Gieser S, Nurenberg M, et al. (2010) Risk factors associated with peritoneal dialysis catheter survival: a 9-year single-center study in 315 patients. J Vasc Access 11: 316–322. Link: https://goo.gl/xqH7wr
- Apostolidis NS, Panoussopoulos DG, Manouras AJ, Pararas BN, Voudiklari SG, et al. (1998) The use of TWH catheters in CAPD patients: fourteen-year experience in technique, survival, and complication rates. Perit Dial Int 18: 424–428. Link: https://goo.gl/LAaWpB
- Figueiredo A, Goh BL, Jenkins S, et al. (2010) International Society for Peritoneal Dialysis. Clinical practice guidelines for peritoneal access. Perit Dial Int 30: 424-429. Link: https://goo.gl/HY8pGA
- Gallieni M, Giordano A, Pinerolo C, Cariati M (2015) Type of peritoneal dialysis catheter and outcomes. J Vasc Access 16: 68-72. Link: https://goo.gl/75E6bm
- Briggs VR, Shrestha BM, Wilkie ME (2014) Respecting shape memory to optimize peritoneal dialysis catheter outcomes. Kidney Int 86: 880–882. Link: https://goo.gl/fuCe4L
- Lye WC, Kour NW, van der Straaten JC, Leong SO, Lee E JC (1996) A prospective randomized comparison of the Swan neck, coiled and straight Tenckhöff catheters in patients on CAPD. Perit Dial Int 16 (S1) S 333-S 335. Link: https://goo.gl/swfLZJ

Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
