Archives of Nursing Practice and Care
The life experience of parents of Congenital Heart Disease adolescents: A meta-synthesis
Federica Dellafiore1*, Roberta Domanico2, Serena Francesca Flocco3, Francesco Pittella4, Gianluca Conte1, Arianna Magon1, Massimo Chessa3 and Rosario Caruso1
2Renal medicine, Southend University Hospital NHS Foundation Trust, Southend-on-Sea, England, UK
3Pediatric and Adult Congenital Heart Disease Center, IRCCS Policlinico San Donato, San Donato Milanese (MI), Italy
4Nursing Degree Course, University of Milan, section of IRCCS Policlinico San Donato, San Donato Milanese (MI), Italy
*Corresponding author: Federica Dellafiore, Health Professions Research and Development Unit, IRCCS Policlinico San Donato Via Agadir, 20-24, 20097 San Donato Milanese (MI), Italy, Tel: (+39) 02 52774940; E-mail: federica.dellafiore@grupposandonato.it
Cite this as
Dellafiore F, Domanico R, Flocco SF, Pittella F, Conte G, et al. (2017) The life experience of parents of Congenital Heart Disease adolescents: A meta-synthesis. Arch Nurs Pract Care 3(1): 031-037. DOI: 10.17352/2581-4265.000022Introduction: Congenital Heart Diseases (CHD) do not preclude the possibility to become adult due to the different innovations in medical and surgical treatments. The transition from childhood to adulthood is a complex process in the life of CHD adolescents, considering the consequences of their diseases and the need to be adherent with their follow-up indications. In this process, parents play an important role, being a landmark for their children, but the experiences of CHD adolescents’ parents are little studied and the literature about their life experiences appears fragmented. Knowledge of life experience of CHD adolescents’ parents is important to address a tailored and efficient health-care delivery for the whole family. Therefore, the aim of this study is to synthesize qualitative papers of life experience of CHD adolescents’ parents.
Methods: A meta-synthesis study using Noblit and Hare’s interpretative meta-ethnography approach was conducted. Databases searched included PubMed, CINAHL, PsycINFO and Google Schoolar and keywords used are “Congenital heart disease”, “Parents”, “Adolescents” and “life experience”. The search process was performed in accordance with the PRISMA guidelines and only the qualitative papers in the last 20 years were included. Studies resulted by search process were critically appraised using the Critical Appraisal Skills Programme qualitative research appraisal tool.
Results:The search yielded 386 potentially relevant studies for screening, and only six articles met all the inclusion criteria. In accordance with the seven phases suggested by Noblit and Hare, the papers were analyzed, discussed and a qualitative meta-synthesis was performed. The meta-synthesis results showed four main themes, exploring also four main contradictions that characterize the life experiences of CHD adolescents’ parents: “fear and uncertainty of the future versus positive coping strategies”; “parents hyper-responsibility and overprotection versus adolescents’ independence desire”; “desire to give support, but not to be supported”; “normality desire versus awareness to live with particular conditions”.
Conclusions: The role of the CHD adolescents’ parents is difficult and they experience some contradictions. This study explore their life experiences in a preliminary way, but further analysis and studies are needed.
Background
Congenital heart diseases (CHD) are one of the most prevalent and serious birth defects, representing a major global health problem. With a prevalence of 9.1 for 1000 live births [1], the CHD are the leading causes of birth defects-associated morbidity, mortality, and medical expenditures [2]. Currently, 1.3 million children live with a CHD worldwide [3] and approximately 90% of them can survive into adulthood [4], due to the advances in diagnosis, medical technology, surgical interventions and treatments. It is estimated that about 2800/million adults are currently living with CHD [5], which need a lifelong follow-up [6].
The transition from childhood to adulthood is a complex process for every young person, being particularly important for CHD adolescents. In fact, the adolescence is a crucial phase for the formation of the personality [7], during which the CHD adolescents have to face with the consequences of their disease and the need to be adherent with their follow-up indications [10]. Moreover, during the transition into adulthood, CHD adolescents could be exposed to many psychological issues related to their development of self-identity, self-esteem and self-image [8] and they should learn about their disease, overcoming frustration and anxiety and developing self-care strategies [9]. For this reason, the recent clinical research focused to explore the peculiarity of the transition period from childhood to adulthood in patients with CHD, in order to develop the purposeful transition care models, which are aimed to provide self-management and to satisfy the medical, psychosocial, educational, and employment needs of CHD adolescents [1,8].
In this process, parents play a key role, being a landmark for CHD adolescents [10]. In fact, the CHD adolescents’ parents are extensively involved in care activities, such as accompanying their child to visits, always staying with them for the entire time and administering their medications every day [11]. Moreover, they could be considered to be an integral part of team members for their children [11], supporting them to develop their independence and to promote their responsibility [12].
Currently, there is a lack of information about the experiences and dilemmas of parents during the CHD transition process from childhood to adulthood. Recent findings seem to highlight that it is not easy to be a CHD adolescents’ parents, because they experience anxiety, stress, and depression [13], often feeling uncertain about their roles during transition [14]. However, knowing the experiences of CHD adolescents’ parents is important to address tailored and efficient health-care delivery for the whole family. Therefore, the aim of this study is to synthesize qualitative papers of life experience of CHD adolescents’ parents.
Materials and Methods
Review method
A literature review with meta-synthesis was undertaken to address the following research questions:
♦ What are the experiences of CHD adolescents’ parents?
♦ Which factors influence the life of CHD adolescents’ parents?
Meta-synthesis is a relatively new technique for examining qualitative research [15]. The literature shows different approaches and techniques types to conduct a meta-synthesis [16]. Noblit and Hare’s [17], meta-ethnographic approach was used to guide this meta-synthesis, subsequently adapted for health services research by Britten et al. [18]. This meta-synthesis method includes 7 phases (Table 1), that overlapping as the synthesis proceeds: phase 1 - getting started; phase 2 -
Search strategy
In accordance with phase 2 [17], a systematic search was performed in electronic databases including MEDLINE, PsycINFO, CINAHL, and Google Scholar, in December 2015. Before the begin of the systematic search process, a pilot test was carried out in electronic databases to exclude that a meta-synthesis on CHD adolescents parents was already performed and to identify the key words. The relevant key terms used to shape the queries were as follows: ‘Congenital Heart Disease’, ‘Transition’ ‘adolescents’, ‘parents’, ‘Life experience’. Indeed, the search comprised four separate search queries based on thesaurus terms, free-text terms and broad terms relevant to topics searches: (1) population-related terms (Parents, Parenting, Caregivers, Family); (2) transition phase -related terms (Adolescents, Youth, Transition phase, Transition); (3) illness - relation terms (Congenital Heart Disease, Congenital Heart Defects); (4) outcomes-related terms (Life Experiences; Perception; Life Change Events; Quality of life, Health related quality of life, Experience, Life). Afterwards, the search terms were combined using the Boolean terms ‘OR’ and ‘AND’ and further combined using free text search. The time limit was set to 1995–2015, because the advanced cardiac surgery was developed and the CHD adolescents there was not before to 20 years ago. Other search limits were the English language and the full text availability.
Inclusion and exclusion criteria
The review included primary qualitative studies about the experiences of CHD adolescents’ parents. The studies identified by queries was selected considering the following inclusion criteria: (a) qualitative studies, (b) published between January 2005 and December 2015, (c) written in English, (d) available full text, (e) focus on parents of CHD adolescents, and (f) explore their life experiences. Studies with other outcomes, with theoretical or quantitative design, in languages other than English were excluded.
Search process and quality appraisal
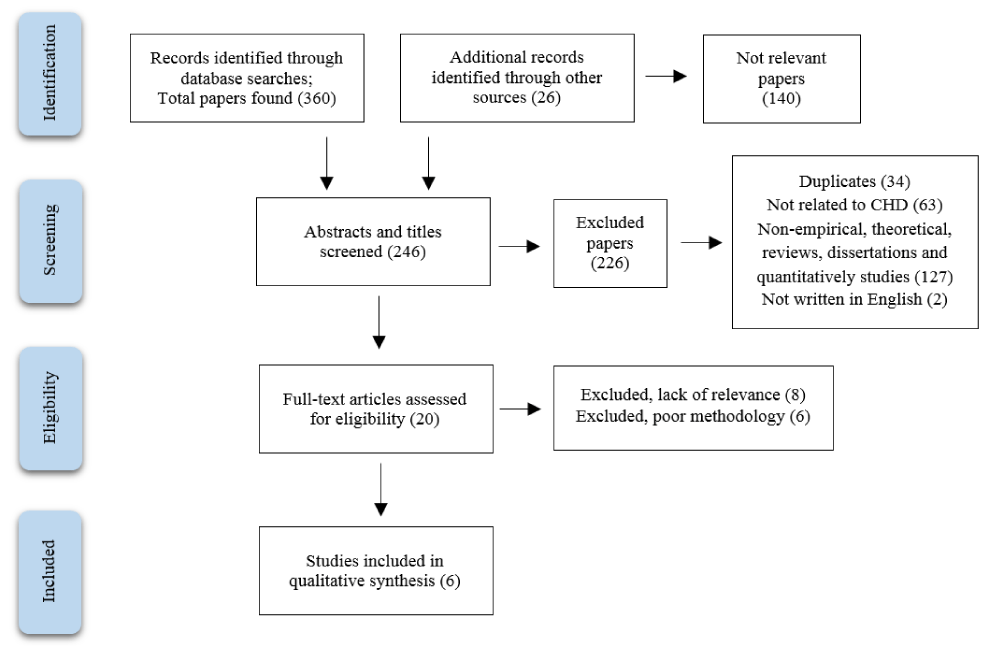
The search process was conducted by two authors (DF and DR) independently. The authors have discussed frequently to reach agreement on the search process and appraisal. The procedure to select the articles during search is summarized in the flow diagram, according to the PRISMA flow-chart (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) [19], as shown in Table 2. The depth literature search, performed using the key terms, led to identify 386 articles (identification phase). In the screening phase, 246 articles were excluded using the inclusion criteria, such as time limit, English language, title and abstract selection and deletion of duplicate. The articles were reduced to 20, and assessed for eligibility (eligibility phase). Those articles were assessed using the Critical Appraisal Skills Programme qualitative research appraisal tool [20]. Thus, after full-texts reading, only six articles were included (included phase), excluding 14 records due to they did not meet CASP assessment (poor methodology) or they did not focused on our research questions (lack of relevance), as shown in Table 2. Also data extraction and critical appraisal were undertaken independently by two researchers (DF and DR) and then discussed until to reach consensus.
Results
The included studies in this meta-synthesis are summarized in Table 3. Two studies were conducted in USA, one study in Canada and three studies in Europe. Four included papers were related to the adolescent with heart defects and CHD, while two studies focused on adolescent with chronic illness, where there also described a sub-sample of CHD adolescents. The data collection in all the studies was conducted through semi-structured interview or narrative interview, and data analysis were made by content analysis, phenomenological hermeneutic method, thematic analysis or grounded theory procedure.
The six identified papers were analyzed by the two authors (DF and DR) (phase 3 of Noblit and Hare approach) to determine the communalities between studies and to integrate the themes emerging from each one (Phase 4 of Noblit and Hare approach) [21]. Afterwards, the same authors identified new concepts and then four new themes were developed (phase 5 of Noblit and Hare approach). Those four themes were related to the synthesis of the data referred to experiences of CHD adolescents’ parents (phase 6 of Noblit and Hare approach), representing the meta-synthesis results.
Thus, each theme explored four main contradictions that characterize the life experiences of CHD adolescents’ parents: “fear and uncertainty of the future versus positive coping strategies”; “parents hyper-responsibility and overprotection versus adolescents’ independence desire”; “desire to give support, but not to be supported”; “normality desire versus awareness to live with particular conditions”. Therefore, the continuous experience of contradictions lived by parents during the transition phase of the adolescents affected by CHD is the main underpinning the meta-synthesis. Nevertheless, parents and adolescents may have different perceptions: parents could typically be anxious, whereas adolescents display a wait-and-see attitude [22,23]. A detailed description of new four themes are presented in the following sections, supported by data from the original studies.
Theme 1: fear and uncertainty of the future versus positive coping strategies
This theme described mainly the parents’ fear about their own son’s future, in term of working environment and social life, and their will to face at best the congenital heart defect: this disease is a huge part of everyday lives and parents seem to be uncertain about their roles during transition and how to promote their children [11]. “A parent never wants to have a kid die before her and that is what she (wife) was upset about. That is why I was trying to tell her to spend as much time as you can, with her (child).And just think; every waking moment that you have, spend it with her. Even if you have both of them or one by themselves, spend that time with her. I had her quit her job and that is why I work 16 hours a day. So that she can spend more time with them…” (Howard, parent) [24].
Although the predictability of their child’s future is no more uncertain than for a child without CHD, the parents struggled with the uncertainty of what impact CHD would have on their adolescent’s life [25]. During infancy and early childhood, most of the parents had been counseled about their child’s limited life span, leaving them to deal with the challenge of uncertainty. Mark’s father said of the early years, “You just never know when you’re going to wake up and find if he’s alive or not. It was terror.” John’s mother remembered, “For a while I was afraid to get attached, because I sort of felt I might lose him” [25]. This often has led the families to live experiences that they would not live: “It has caused us to do things in our lives at a different point than we would have otherwise. For example, we went to Disney World when Zoe was seven and Rick was three. We said that ‘they are well now, and we do not know how long they will be well for, so let’s go now.’ So there are things we have done in our lives, because we wanted to make sure that they had the opportunity to do those things when there were no health issues” [24].
The parents feel helpless and afraid, because their child cannot fulfill his own dreams and ambitions as their healthy peers: they are wondering how hard is to push their child to excel were areas of considerable concern for parents of adolescents. As their children progressed through adolescence into young adulthood, parents wanted their children to go to college, obtain stable jobs, move from home, and become independent. Faced with these fears and uncertainties some families have developed some approaches to cope with the future and with the illness, such as some parents have tried to put the disease into background and live as normal as possible. Other parents have instead tried to put aside uncertainties concerning the future, focusing on daily-based flexible problems scheme. An example given concerned the management of smoking as a mother says “What worries me most is smoking, because I think is the only thing I can change” [25].
Theme 2: parents’ hyper-responsibility and overprotection versus adolescents’ independence desire
This theme described the contrast between the parent’s inclination in taking charge of adolescent’s responsibilities and their wish of getting their own children more independent. Parents expressed ambivalence about whether it was appropriate to encourage their child to prepare for the working world. Jane’s mother said: “I’d like to see her graduate from eighth grade and high school. I really would like to see her have the skills she needs to pursue what she would like to do in life... I guess the health I can’t really worry about, because! Can’t do anything about it….” [25]. The transition phase included the transfer of responsibility from pediatric care to the adult one, and represented the period in which parents start to give more autonomy in decision making to the young adult. Some families consider this situation as a difficult and intense period, and they would like that their child will never grow up; but, at the same time, they realize how this transfer is considered as a fundamental step, in which they need to release responsibility and independence to their children [26,27].
Parents’ natural desire is to act as a parent: they feel the need to be involved in the care of the adolescents and feel entitled to responsibility for their adolescents’ health. They grieve the experiences that their sick children are missing because of their heart defects and mourn the tough school years that they must undergo. They also express concerns that the world would not treat the young adult fairly because of CHD [25]. Parents become aware that their children were no longer children and this could give a sense of sorrow in not being needed anymore. At the same time, this new and unknown condition could represent for parents a sort of a relief to shift responsibility.
Theme 3: desire to give support, but not to be supported
This third theme described the parents’ need to help their child with CHD and the relationship of the family with the care providers. In order to support the teenager, a parent seeks security and force by the care providers, who understand the clinical and emotional situation that the families and young must face every day. The parents feel safe when the relationship with the clinical staff is based on solid trust: the greatest desire is to feel accepted and understood not only by pediatric care but also adult’s one. Especially the latter has to provide assistance to parents, which now find themselves lost and looking for advice to better deal with the transition process and move to the new adult health care setting [14,28]. “It felt good because, in the position I was in, I needed all the information I could get, even though I might not have understood the whole thing at once. It felt good to be involved in it and not be pushed away.” [28].
Parents know how much is important the care providers’ participation, but at the same time, they underline how much their role is crucial. In fact, they are aware to be needed to their children, which may not be able to face this new reality alone. In fact, a mother of 18 year-old boy says: “Just because he is a grown up, they can’t expect that he knows everything...” [14]. For this reason the parents are willing to accept the help offered by care providers and they start to be condescending towards them in order to be considered and therefore more helped. The parents consider themselves a strong and supportive figure to their own children [25], but they can sometimes consider themselves weak when they miss a trust based relationship with the care providers. In the article of Burström et al., a mother of 16-year-old boy explains: “You know you need help as a parent... to know how to behave and help... about the heart condition or if you should you need help to step back…” [14].
Parents’ desire is to receive the most possible clinical information they can, even if these latter are frightening [28]. When parents have not been informed about the medical condition of their children, they begin to feel confusion, suffering and helplessness: in this situation they need to fight for their own children, in order to support them in the best way possible [28]. “It feels as if he is concerned about his heart. I mean before the last surgery, it was like... he asked, what if I die? …I mean straight on so you can’t hide, just have to answer...” (Mother of 16-year-old boy) [14].
Theme 4: normality desire versus awareness to live with particular conditions
The last theme analyzed during the development of this meta-synthesis illustrates the contrast between the search for normality by parents and the awareness of which limits the congenital heart disease imposes in the quality of life of adolescents and families. Martha, mother of 9-year-old Chris, described the impact of her daughter’s severe illness on the entire family: the severity of illness was perhaps the largest contributor to a sense of being not normal. “I think our other daughter has had a lot of problems through all this, because once Chris came along, it took so much of our time and so much of my energy, and so much of my worrying went into Chris. They said they didn’t expect her to live and get out of the hospital. Then they said we don’t expect her to live a year” [26].
Parents would like to be considered as a normal family: despite copious clinical visits, surgeries, or unexpected health deterioration of health, some parents attempt to adapt themselves to the new life, “normalizing” as much as possible, as suggested by health care providers [26]. Others parents, instead, tend to make a comparison between their own children and healthy peers, because schools and society are the first to define the adolescents affected by CHD as” sick” and then different [24,25]. John’s mother was frustrated by the discrimination her son encountered from a teacher: “We always said we never restricted John, we always felt that if he got tired, he would just stop doing it. And so I told the PE teacher.., and of course that didn’t fit into their way of thinking... And instead of doing PE, he was benched every time. Benching there was punishment... And I went to the teacher and I said, ‘Don’t you have anything else for him to do? Could he be your assistant? Or help with the balls?’ And she said, ‘No, no, because that would give him a favorable position. That wouldn’t be fair towards the other kids.’ So, we got out of that school.” [25].
Parents suffer thinking about the experiences their children are losing [28]: they perceive that CHD adolescents feel alienated and treated differently by teachers and coaches [29] and feel that the illness has affected all family life, even in the smallest aspects. In the articles by Gantt (2002) a mother states: “We used to go camping before he was born. We never went again. Not as a family. Not like we did with the other two kids.” [26]. Parents also ask themselves how to inform family and friends about their children’s disease; others use instead the disclosure of the disease to vent themselves and to be considered, after all, normal [25]. Most parents testified in qualitative articles of trying to live life as it is, encouraging adolescents to love and appreciate it, despite the physical and social limitations imposed by congenital heart disease: “He’s just a normal child. So, we always try to be normal with him; [or] you have to let yourself forget about the heart problem in order to go on through life; land] Live normally. Let your family continue on as normal as possible, because the rest of the world is not going to give one hoot that this kid’s got this defect, so don’t let him use it as an excuse. Think positive, hold the vision of good results.” [25].
Discussion
These six articles, analyzed by meta-synthesis approach, provide valuable information on the factors influencing the life of CHD adolescents’ parents. These information could be used to better address a tailored and efficient health-care delivery for the whole family. Currently, literature has paid little attention to this topic, in fact the scientific researches are mainly focused on quality of life of CHD patients, while the experiences of CHD adolescents’ parents are less studied. Moreover, the literature about CHD adolescents’ parent’s life experiences appears fragmented. Regarding this theme, the research strategy described in this paper, has identified only six articles that explored this topic in the last 20 years. According to Noblit and Hare’s meta-ethnographic approach [17], the synthesis of the included six qualitative papers seems to bring out a persistent experience of contradictions lived by parents during the transition phase of the adolescents affected by CHD.
Four themes emerged by the results of the six qualitative papers to synthesize the life experience of CHD adolescents’ parents: “fear and uncertainty of the future versus positive coping strategies”; “parents hyper-responsibility and overprotection versus adolescents’ independence desire”; “desire to give support, but not to be supported”; “normality desire versus awareness to live with particular conditions”. The issue of contradictions is the main feature characterizing all the peculiarities of CHD adolescents’ parents. Following the reading of the included papers, different divergent views emerged by the perspectives and experiences described in the original qualitative articles: (a) the parents wish to have a normal life, similar to life of healthy sons, but they must face every day the limitations imposed by illness on quality of life of the young and on family context; (b) they would like to support the sons but they demand to be supported by care providers; (c) they give a hyper-responsibility and overprotection to teenager but, in opposite, the adolescents would want their independence; (d) finally, they are uncertain and frightened about the future of their sons, but they can implemented the positive coping strategies to normalize the life of them and their CHD sons, as more possible.
These issues suggest that some difficults and significant dilemmas are present in the life of adolescent with CHD parents, especially during the transition phase from childhood to adulthood. Furthermore, parents highlight their need to be supported by care providers to best face the transition phase of their CHD sons. Nurses play a crucial role in this process, because their care delivery should be addressed to both adolescent patients and their parents. Moreover, nursing care could provide continued contacts between physician, patients and their families during all their lives.
According to the recent guidelines ACC/AHA for the management of patients with CHD [30], the process of transitioning should prepare young patients for successful transfer to an adult healthcare provider at a later time, and it should begin since the age of 12 [31]. Furthermore, the transition care models have to orient and to encourage a sound health-behavior, considering how those patients could be exposed to many psychological issues related to their development of self-identity, self-esteem and self-image [8].
Moreover, heavy medical expenses [32] and frequent hospitalizations [33], bring CHD adolescent patients and their family members to other types of complications, from the burden of the disease on the whole family [34], to issues related to the unknown future, treatment program or prognosis. For these reasons, the understanding of CHD parents’ needs is crucial to face the diversity and complexity of adolescents with CHD, guiding the whole care delivery.
As many studies have already shown, parents of children with CHD showed lower well-being compared to parents of healthy children [35]. These findings are amplified when children with CHD will grow up. For all these reason, the literature shows that the parental role during the transition phase is extremely difficult, being the parents a landmark for their children. They live feelings of helplessness, they are unable to relate and understand the needs of their sons, and consequently parents of CHD adolescents have a decreased well-being compared to parents of healthy adolescents.
Limitations
This meta-synthesis was developed based on data collected within original studies on the experiences of CHD adolescents’ parents. Therefore, this study’s quality is largely a product of the quality of data collected in the original studies chosen for meta-synthesis. A strength of the current study was that the two authors conducted their reviews independently and are compared for confirming data. While the integration of different individual’s perspectives and experiences has not altered the focus of this study, it produced a more complete picture of the study phenomenon. On the contrary, the inclusion of only six qualitative papers is the main limitation of this meta-synthesis, which is not intended to be comprehensive or cumulative. Nevertheless, the literature has paid little attention to date regarding this issue, also in light of the relatively new interest in this field. In other words, this meta-synthesis represent a first attempt to incentive research endeavors to study the issue around the life of adolescents with CHD and their parents.
Conclusion
This meta-synthesis help to highlight the peculiarities of adolescents with CHD, their parents and should be useful even for health providers. In fact, the role of parents is crucial in the transition to adulthood of their children with CHD, especially to personalize their clinical pathway. For this reason, the understanding of the CHD adolescent’s parents life experience is fundamental to provide nursing care focused on unanswered or hidden needs. As described in this meta-synthesis, the continuous experience of contradictions lived by CHD parents during this transition phase should be the beginning to shape personalized support programs. Moreover, those contradictions represent a real theoretical framework that have to be deeply investigated with empirical researches. In other words, the results of this meta-synthesis could help to frame the peculiarities of adolescents with CHD and parents, addressing future empirical studies and even the necessity to develop specific tools to measure each identified peculiarity.
- Chen CW, Su WJ, Chiang YT, Shu YM, Moons P (2017) Healthcare needs of adolescents with congenital heart disease transitioning into adulthood: a Delphi survey of patients, parents, and healthcare providers. Eur J Cardiovasc Nurs 16: 125–135. Link: https://goo.gl/l73pWr
- Pei L, Kang Y, Zhao Y, Yan H (2017) Prevalence and risk factors of congenital heart defects among live births: a population-based cross-sectional survey in Shaanxi province, Northwestern China. BMC Pediatrics 17: 18. Link: https://goo.gl/DcAkic
- van der Linde D, Konings EE, Slager MA, Witsenburg M, Helbing WA, et al. (2011) Birth Prevalence of Congenital Heart Disease Worldwide. J Am Coll Cardiol 58: 2241–2247. Link: https://goo.gl/0yJwOz
- van der Bom T, Zomer AC, Zwinderman AH, Meijboom FJ, Bouma BJ, et al. (2011) The changing epidemiology of congenital heart disease. Nat Rev Cardiol 8: 50–60. Link: https://goo.gl/i7IzbU
- Baumgartner H, Budts W, Chessa M, Deanfield J, Eicken A, et al. (2014) Recommendations for organization of care for adults with congenital heart disease and for training in the subspecialty of “Grown-up Congenital Heart Disease” in Europe: a position paper of the Working Group on Grown-up Congenital Heart Disease of the Euro. Eur Heart J 35: 686–690. Link: https://goo.gl/pYk5Y1
- Marelli AJ, Gurvitz M (2011) Progress in Cardiovascular Diseases 53: 239–246. Link: https://goo.gl/2DnQ7L
- Moceri P, Goossens E, Hascoet S, Checler C, Bonello B, et al. (2015) From adolescents to adults with congenital heart disease: the role of transition. Eur J Pediatr 174: 847–854. Link: https://goo.gl/2g6ZRw
- Flocco SF, Caruso R, Dellafiore F, Orlando A, Magon A, et al. (2017) Towards the Standardization of Transition Care Models for Adolescents with Congenital Heart Disease (CHD): A Perspective. Journal of Clinical & Experimental Cardiology 8: 495. Link: https://goo.gl/lFtx9H
- Chiang YT, Chen CW, Su WJ, Wang JK, Lu CW, et al. (2015) Between invisible defects and visible impact: the life experiences of adolescents and young adults with congenital heart disease. J Adv Nurs 71: 599–608. Link: https://goo.gl/8Dl1AZ
- Dellafiore F, Pittella F, Flocco SF, Caruso MP, Bersani V, et al. (2016) What about life experiences of Congenital Heart Disease adolescents’ parents? A literature review and meta-synthesis. Cardiology in the Young 26: 180. Link: https://goo.gl/LeW77S
- Clarizia NA, Chahal N, Manlhiot C, Kilburn J, Redington AN, et al. (2009) Transition to adult health care for adolescents and young adults with congenital heart disease: perspectives of the patient, parent and health care provider. Can J Cardiol 25: e317-22. Link: https://goo.gl/awllZS
- Reiss JG, Gibson RW, Walker LR (2005) Health Care Transition: Youth, Family, and Provider Perspectives. Pediatrics 115: 112–120. Link: https://goo.gl/0aPxhu
- Wei H, Roscigno CI, Hanson CC, Swanson KM (2015) Families of children with congenital heart disease: A literature review. Heart Lung 44: 494–511. Link: https://goo.gl/7Evjsh
- Burström Å, Öjmyr-Joelsson M, Bratt EL, Lundell B, Nisell M (2016) Adolescents With Congenital Heart Disease and Their Parents. The J Cardiovasc Nurs 31: 399–404. Link: https://goo.gl/LgY2js
- Jensen LA, Allen MN (1996) Meta-Synthesis of Qualitative Findings. Qualitative Health Research 6: 553–560. Link: https://goo.gl/01pHsb
- Walsh D, Downe S (2005) Meta-synthesis method for qualitative research: a literature review. J Adv Nurs 50: 204–211. Link: https://goo.gl/hHqOTU
- Noblit GW, Hare RD (1988) Meta-ethnography : synthesizing qualitative studies. (N. Park, Ed.) (1st ed.). London: Sage Publications. Link: https://goo.gl/g9ysbJ
- Britten N, Campbell R, Pope C, Donovan J, Morgan M, et al. (2002) Using meta ethnography to synthesise qualitative research: a worked example. J Health Serv Res Policy 7: 209–215. Link: https://goo.gl/E5O0tF
- Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, et al. (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ (Clinical Research Ed.) 339: b2700. Link: https://goo.gl/25KpTZ
- Critical Appraisal Skills Programme (CASP) (2014) CASP Systematic Review Checklist CASP Qualitative Checklist. Retrieved March 7: 2017. Link: https://goo.gl/N2YgSf
- Atkins S, Lewin S, Smith H, Engel M, Fretheim A, et al. (2008) Conducting a meta-ethnography of qualitative literature: lessons learnt. BMC Med Res Methodol 8: 21. Link: https://goo.gl/kcjju5
- Anthony SJ, Martin K, Drabble A, Seifert-Hansen M, Dipchand AI, et al. (2009) Perceptions of Transitional Care Needs and Experiences in Pediatric Heart Transplant Recipients. Am J Transplant 9: 614–619. Link: https://goo.gl/EyC3WW
- Moons P, Pinxten S, Dedroog D, Van Deyk K, Gewillig M, et al. (2009) Expectations and experiences of adolescents with congenital heart disease on being transferred from pediatric cardiology to an adult congenital heart disease program. J Adolesc Health 44: 316–322. Link: https://goo.gl/Rbvznq
- Moola FJ, Norman ME (2011) “Down the rabbit hole”: enhancing the transition process for youth with cystic fibrosis and congenital heart disease by re-imagining the future and time. Child Care Health Dev 37: 841–851. Link: https://goo.gl/1KEJLR
- Sparacino PS, Tong EM, Messias DK, Foote D, Chesla CA, et al. (1997) The dilemmas of parents of adolescents and young adults with congenital heart disease. Heart Lung 26: 187–195. Link: https://goo.gl/YqAUtu
- Gantt L (2002) As normal a life as possible: mothers and their daughters with congenital heart disease. Health Care Women Int 23: 481–491. Link: https://goo.gl/MNMgHi
- van Staa AL, Jedeloo S, van Meeteren J, Latour JM (2011) Crossing the transition chasm: experiences and recommendations for improving transitional care of young adults, parents and providers. Child Care Health Dev 37: 821–832. Link: https://goo.gl/dQdNTh
- Bruce E, Sundin K (2012) Experience of support for parents of adolescents with heart defects--supported to be supportive. J Pediatr Nurs 27: 366–374. Link: https://goo.gl/u9tzJ9
- Marino BS, Tomlinson RS, Drotar D, Claybon ES, Aguirre A, et al. (2009) Quality-of-life concerns differ among patients, parents, and medical providers in children and adolescents with congenital and acquired heart disease. Pediatrics 123: e708-15. Link: https://goo.gl/lYnmz5
- Warnes C, Williams R, Bashore T, Child J, Connolly H, et. al. (2008) ACC/AHA 2008 Guidelines for the Management of Adults With Congenital Heart Disease: Executive Summary: A Report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to Develop Guidelines for. Circulation 118: 2395–2451. Link: https://goo.gl/cppZlQ
- Davies H, Rennick J, Majnemer A (2011) Transition from pediatric to adult health care for young adults with neurological disorders: parental perspectives. Can J Neurosci Nurs 33: 32–39. Link: https://goo.gl/16jA8T
- Connor JA, Kline NE, Mott S, Harris SK, Jenkins KJ (2010) The meaning of cost for families of children with congenital heart disease. J Pediatr Health Care 24: 318–325. Link: https://goo.gl/xrI1NC
- Harvey KA, Kovalesky A, Woods RK, Loan LA (2013) Experiences of mothers of infants with congenital heart disease before, during, and after complex cardiac surgery. Heart Lung 42: 399–406. Link: https://goo.gl/sTr4ND
- Rychik J, Donaghue DD, Levy S, Fajardo C, Combs J, et al. (2013) Maternal psychological stress after prenatal diagnosis of congenital heart disease. J Pediatr 162: 302–307. Link: https://goo.gl/B6p2QV
- Lawoko S, Soares JJ (2002) Distress and hopelessness among parents of children with congenital heart disease, parents of children with other diseases, and parents of healthy children. J Psychosom Res 52: 193–208. Link: https://goo.gl/qTvbvA

Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.
 Save to Mendeley
Save to Mendeley
