Global Journal of Medical and Clinical Case Reports
An Unusual Case of Melioidosis with Psoas Abscess
Prijesh Janardanan1*, PC Easaw2 and Abdul Rahiman3
2Senior Consultant & HOD, Department of General Medicine, MIMS, Calicut, India
3Senior Consultant, Department of General Medicine, MIMS, Calicut, India
Cite this as
Janardanan P, Easaw PC, Rahiman A (2017) An Unusual Case of Melioidosis with Psoas Abscess. Glob J Medical Clin Case Rep 4(1): 015-017. DOI: 10.17352/2455-5282.000036Melioidosis is an infection caused by a gram negative bacterium .We report a case of FUO which upon investigation revealed muscle abscess and subsequent pus culture revealed melioidosis. This case is reported since melioidosis can often mimic other diseases and in rare instances present with psoas abscess.
Highlights:
* Melioidosis is an infrequent cause of FUO in the Indian subcontinent
* Prolonged back pain in a case of melioidosis warrants imaging if deemed necessary
Introduction
Melioidosis, an infection caused by a facultative intracellular gram-negative bacterium, B.pseudomallei, occurs predominantly in South-east Asia, northern Australia, South Asia (including India), and China. It is often a cause for fever of unknown origin (FUO) and poses a diagnostic challenge to the treating physician.
Case Presentation
71 yr old Indian male, retired Government employee, presented with high grade intermittent fever since the last 20 days with rigors and chills. He also complained of intermittent productive cough of 2 weeks duration. He had dull aching back pain with no radiation or weakness of the lower limbs. No history of trauma or other joint pains. There were no significant respiratory symptoms other than already mentioned. No bowel or bladder symptoms. No significant weight loss. There was no history of recent exposure to pulmonary tuberculosis. He was a known case of diabetes since the last 30 years and on insulin since last 5 years. He was also a hypertensive since the last 2 years and was on olmesartan and amlodipine. There was no history of malignancies in the family. He was not a smoker or an alcoholic. He was treated initially with antibiotics for the same but complaints persisted. On examination, he had pallor. His vitals were stable and examination of the systems revealed no further clues. His chest was clear. Skull and spine were normal. Haemogram showed polymorphonuclear leucocytosis with elevated ESR of 114 and CRP of 32.RBS was 215 at the time of admission. He had albuminuria. His creatinine levels were borderline and A/G reversal (2.8/4.2). HbA1c levels were elevated (12.8). His Chest x ray was normal. USG abdomen showed mild pleural effusion and mild ascites. ECHO was normal. The possibilities considered in this elderly diabetic male with fever, cough, and back pain with no examination findings were tuberculosis, brucellosis, multiple myeloma, lymphoma and other solid tumors. Atypical pneumonia IgM done was negative. Blood culture showed no growth. In view of these findings, possibility of mutiple myeloma was considered and so serum electrophoresis was sent which was normal. IgG quantification showed no elevated immunoglobulin levels. CT thorax showed bilateral pleural effusion with basal atelectasis and multiple small mediastinal lymph nodes. A contrast tomography (CT) abdomen was performed which showed multiple small mesenteric lymph nodes and solitary lytic lesion in iliac side of right SI joint. To look for other lytic lesions a bone scan was performed which was normal. Pleural fluid study revealed exudative nature of fluid with predominant neutrophils, adenosine deaminase (ADA) negative, acid fast bacilli (AFB) was not detected and did not grow any organisms on culture. Urine culture revealed growth of extended spectrum betalactamase (ESBL) E-coli and so culture sensitive meropenem was started. Following this he became afebrile and his symptoms improved. He was discharged in afebrile state after a course of meropenem.
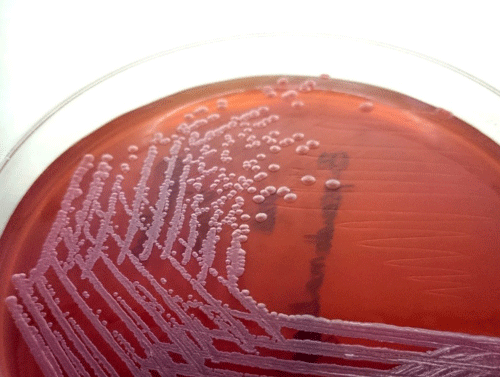
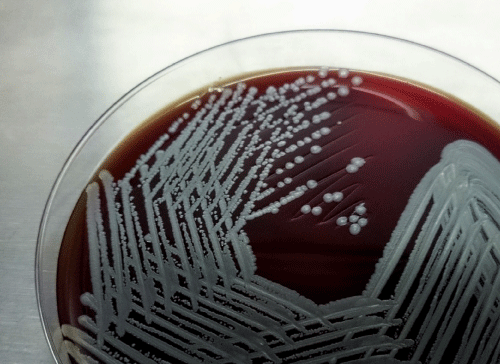
He returned to the outpatient (OP) department a week later with high grade fever, chills, generalised tiredness, back pain and pain in the left thigh. His vitals were stable, general and systemic examination revelaed no new findings. Haemogram showed polymorphonuclear leucocytosis with elevated ESR and creatinine remained at a stable level of 1.4.Revisiting the history and findings the possibilities considered were tuberculosis, melioidosis and connective tissue disorders. Sputum smear examination failed to demonstrate AFB. Mantoux test was negative. Anti-nuclear antibody (ANA) was negative. Magnetic Resonance Imaging (MRI) showed multiple peripheral enhancing lesion in left psoas and erector spinalis with extension into epidural space which was suggestive of abscess, shown in Figures 1a,b. CT guided aspiration of the pus was done. Pus showed no microorganisms on gram stain and AFB staining. On culture, B. pseudomallei grown on Mac conkey and blood agar, shown in Figures 2a,b.
The patient was diagnosed as melioidosis based on the clinical presentation and pus culture from the lesion. He was started on parenteral ceftazidime for 2 weeks followed by 6 weeks of oral cotrimoxazole.His symptoms were relieved after starting antibiotics. Fever disappeared and cough subsided. USG was repeated to look for the pus collection which showed marked resolution. His improvement and response to antibiotics further confirmed the diagnosis of melioidosis.
Discussion
Meliodosis may present in acute form or chronic. Chronic infection is when the disease duration is more than 2 months. Melioidosis can occur in a variety of forms. Most B.pseudomallei infections are subclinical. The most common clinical manifestations are pneumonia and localized skin infection. Less commonly, bacteremic spread of the organism can result in clinical manifestations involving virtually any site.
Pneumonia is the most common clinical presentation of melioidosis. Acute presentation may consist of high fever, cough, sputum, chills, rigors, and respiratory distress with or without shock. A subacute or chronic presentation may consist of cough, purulent sputum production, hemoptysis, and night sweats, suggestive of tuberculosis [1,2]. Abscesses in internal organs are well recognized, especially in the spleen, kidney, prostate and liver. Fevers, chills, and rigors with or without hypotension are common, but localizing symptoms are often absent [3,4].
Chronic melioidosis is characterized by abscesses and suppurative lesions, which can occur in a variety of organs. Although the liver, spleen, skeletal muscle and prostate gland are affected most often, lesions can occur in any organ including the skin, lung, myocardium, bone, joints, lymph nodes and testes [5]. The organism is variably sensitive to antibiotics. Hence the therapy requires either ceftazidime (40 mg/kg,t.i.d.) and co-trimoxazole (10/50 mg/kg) b.i.d. for 2-4 weeks, or meropenem (25 mg/kg t.i.d. for 2 weeks) followed by cotrimoxazole for 12-20 weeks [6].
This case is reported because of the rarity of finding skeletal abscesses especially psoas abscess in a case of melioidosis. The case also emphasies the need to take a closer look on even such subtle symptoms such as back pain which is often ignored owing to back pain of old age. There is need to locate and search for potential abscesses in such atypical sites. The conclusion is that, rarely melioidosis can lead to psoas abscess and may present as back pain with constitutional symptoms. Recurrence of the illness after treatment with routine antibiotics should raise the suspicion of melioidosis and must be investigated promptly.
Discussion
This is the first report of closed simultaneous avulsion of FDS and FDP in a little finger. There was no preceding synovitis, or previous injury. The decision to repair only FDP in a little finger where both are divided is accepted practice () in the presence of an intact volar plate, and led to an excellent outcome.
- Cheng AC, Currie BJ (2005) Melioidosis: epidemiology, pathophysiology, and management. Clin Microbiol Rev 18: 383-416. Link: https://goo.gl/8Qdcjg
- Dance DA (1991 Melioidosis: the tip of the iceberg? Clin Microbiol Rev 4: 52-60. Link: https://goo.gl/sI6214
- dÍ Melioidosis P (1989) Review of 686 cases and presentation of a new clinical classification: In: Punyagupta S, Sirisanthana T, Stapatayavong B, eds. Melioidosis. Bangkok: Bangkok Medical. 1989: 217-229 Link:
- Currie BJ, Fisher DA, Howard DM, Burrow JN, Lo D, et al. (2000) Endemic melioidosis in tropical northern Australia: a 10-year prospective study and review of the literature. Clin Infect Dis 31: 981-986. Link: https://goo.gl/EgyFmE
- Pattamapaspong N, Muttarak M (2011) Musculoskeletal melioidosis. InSeminars in musculoskeletal radiology. Thieme Medical Publishers 15: 480-488. Link: https://goo.gl/oUQy1D
- Inglis TJ, Rolim DB, Rodriguez JL (2006) Clinical guideline for diagnosis and management of melioidosis. Revista do Instituto de Medicina Tropical de São Paulo 48: 1-4. Link: https://goo.gl/g83wAK

Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
