Journal of Cardiovascular Medicine and Cardiology
Complete Left Pericardial Agenesis associated with Ventricular Septal Defect
Gopi Nallaiyan*
Cite this as
Nallaiyan G (2018) Complete Left Pericardial Agenesis associated with Ventricular Septal Defect. J Cardiovasc Med Cardiol 5(1): 003-004. DOI: 10.17352/2455-2976.000058Case Report
9 years old male patient admitted to our department with complaints of recurrent respiratory tract infection since 2 years of age. No History of cyanosis His left eye is absent and it was the abnormality at birth.
On physical examination, there was no cyanosis or clubbing. Left eye Enopthalmous was present. Pulse rate was 88 per minute and regular. Blood pressure on Right upper limb in sitting position was 100/60 mm Hg. Apical impulse was displaced and prominent down and out with prominent systolic thrill. On Auscultation, first and second heart sounds were normal and 4/6 pan systolic murmur was heard on the left lower border of the sternum.
Electrocardiography showed features of Normal sinus rhythm, Left axis deviation, Left ventricular hypertrophy.
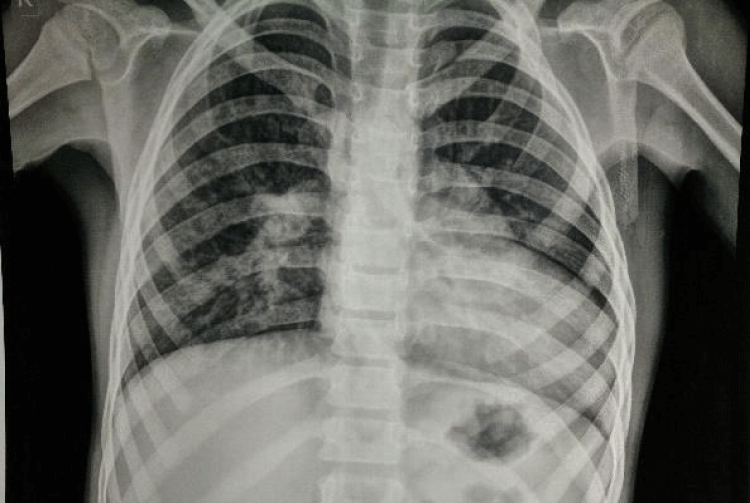
Chest X-Ray Postero anterior View showed the following features (4)
• Cardiomegaly with Cardiothoracic ratio of 0.6.
• Prominent pulmonary bay.
• Lung shadow between Pulmonary artery and Aorta.
• Straight Left heart border (Figure 1 ).
2D Echocardiography revealed Perimembranous VSD with intact Inter Atrial septum, pulmonary stenosis with gradient of 50 mm Hg across the pulmonary valve and Good biventricular function.
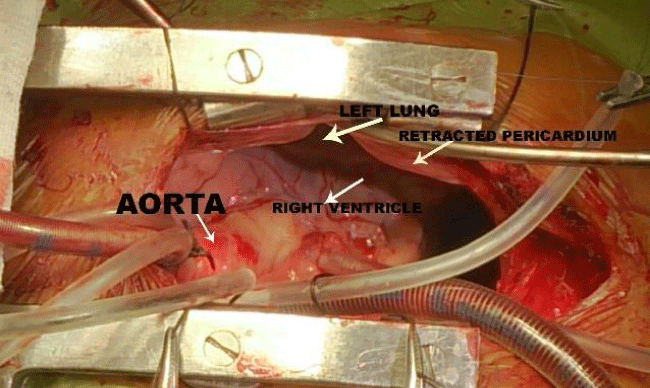
Intra operatively, both heart and left lung were seen after opening the anterior pericardium. There was no separate pericardial cavity with absent posterior pericardium and it was continuous with left pleural cavity – Complete left pleruopericardial agenesis (Figure 2).
There was a Restrictive Perimembranous VSD of 5 mm diameter partially closed by the septal leaflet of Tricuspid valve. Pulmonary valve was dysplastic with valvular pulmonary stenosis.
Transatrial 0.6 mm Polytertafluroethylene patch closure of VSD and open pulmonary valvotomy was done. No surgical correction done for left pleuropericardial ageniesis as there was no major herniation of the heart in to the left pleural cavity.Chest tubes were placed in the mediastinum and pericardium. Post-operative course was uneventful and patient discharged on 6th post-operative day with stable hemodynamics. There were no symptoms post operatively at 6 month follow up of the patient. 2D ECHO at the time of review showed intact IVS with no gradient across the pulmonary valve.
Discussion
A congenital pericardial defect is a rare clinical condition, involving the left (86%) more than the right [1-3]. Males are more commonly affected than females (3:1). In most of the cases, the anomaly is asymptamatic. The reported incidence of isolated congenital pericardial defects is 1/14000 [1].
The main cause is due to the premature atrophy of the left duct of Curvier, which leads to the persistence of the left pleuropericardial foramen [2].
Chest pain is the commonest symptom, which is typically precipitated by left lateral decubitus position and relieved by turning to the right [4]. Sudden death is reported [1]. Chest pain symptoms are often attributed to coronary ischemia from the torsion of great vessels, herniation of cardiac structures through the pericardial defect and tension of pleuropericardial adhesions [4]. The reasons for sudden death may the herniation of the left ventricle, left appendage and the involvement of left circumflex artery [1].
On chest X-Ray film, the following features can be seen
1) Shifting of heart to the left and hence irregular left side border of the heart and loss of right side border of the heart due to its superimposition over the spine.
2) Air shadow between the aorta and pulmonary bay due to the presence of lung tissue.
On echocardiography, right ventricular dilatation and paradoxical septal motion are commonly seen, but ventricular function is usually normal [5].
At cardiac catheterization, one can detect protruding of left atrial appendage through the defect [4,6]. Magnetic resonance imaging is the most useful diagnostic test. It determines the extent of the defect, excludes herniation of cardiac structures and any additional defects [7,8]. Video assisted thorocoscopy can also be helpful.
If the patient is symptomatic or the defect is associated with other cardiac defects, surgery might be indicated. Because of the rarity of congenital pericardial defects and variability of their presentation, no standard surgical approach has been recommended. Surgical closure techniques consist of primary closure, patch closure, widening of the defect depending on the anatomic size and location of the defect. If there is acute apical appendage strangulation, left atrial appendectomy is also might be considered [4]. Larger defects are typically well tolerated and repair can be technically difficult. Reconstruction is not recommended for such large defect like in our case because heart typically adapts to the distorted anatomy and corrective attempts may result in unstable flow patterns.
- Rusk RA, Kenny A (1999) Congenital pericardial defect presenting as chest pain. Heart 81: 327-328. Link: https://goo.gl/hFWcdN
- Lu C, Ridker PM (1994) Echocardiographic diagnosis of congenital absence of the pericardium in a patient with VATER association defects. Clin Cardiol 17: 503-504. Link: https://goo.gl/1VahZS
- Mashru MR, Amin SR, Desai AG, Daniwalla DF, Shah KD (1985) Absent left pericardium. J Assoc physiciains India 33: 539-541. Link: https://goo.gl/QwAfNh
- Gatzoulis MA, Munk MD, Merchant N, Van Arsdell GS, McCrindle BW, et al. (2000) Isolated congenital absence of pericardium: clinical presentation, diagnosis, management. Ann Thorac Surg 69: 1209-1215. Link: https://goo.gl/tUP6xm
- Nicolosi GL, Borgioni L, Alberti E, Burelli C, Maffesant IM, et al. (1982) M Mode and two dimensional echocardiography in congenital absence of the pericardium. Chest 81: 610-613 Link: https://goo.gl/TNZN81
- Candan I, Erol C, Sonel A (1986) Cross sectional echocardiographic appearance in presumed congenital absence of the left pericardium. Br Heart J 55: 405-407 Link: https://goo.gl/GdoYTo
- Schiavone WA, O Donnell JK (1985) Congenital absence of the left portion of parietal pericardium demonstrated by nuclear magnetic resonance imaging. Am J Cardiol 55: 1439-1440 Link: https://goo.gl/tt5b2U
- Sechtem U, Tscholakoff D, Higginis CB (1986) MRI of the normal pericardium. AJR Am J Roentgenol 147: 239-244 Link: https://goo.gl/4Uptgq

Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.
 Save to Mendeley
Save to Mendeley
