Archives of Clinical Gastroenterology
Surgically curable Pancreas Enigma: Solid Pseudopapillary Tumor. Report of a case and literature review
Kurşat Rahmi Serin, Muharrem Oner and Nadir Adnan Hacım*
Cite this as
erin KR, Oner M, Hacım NA (2018) Surgically curable Pancreas Enigma: Solid Pseudopapillary Tumor. Report of a case and literature review. Arch Clin Gastroenterol 4(3): 029-031. DOI: 10.17352/2455-2283.000055Solid pseudopapillary tumor (SPT) is a rare pancreatic neoplasm, classified as low-grade malignant tumor by the World Health Organization in 2000. Surgical treatment usually provide curative intent. Here in we report a 30 years-old woman whom had been operated upon possible benign pancreatic head mass diagnosed histopathologically as solid pseudopapillary tumor. And we aimed to review the literature on the basis of the case. In conclusion, solid pseudopapillary tumors are slow-growing tumors, with unpredictable potential for malignancy. Aggressive surgery yields favorable results even in the presence of vascular invasion and metastatic disease.
Introduction
Solid pseudopapillary tumor (SPT) is a rare neoplasm of the exocrine pancreas. The incidence of this tumor is rises from 0.5% to 2.7% of all pancreatic tumors in recent years depend on the recognition of the clinicians and the development of radiologic modalities [1,2]. It was first described by Frantz in 1959 and it is also known as Frantz’s tumor [3,4]. It was renamed as SPTs and categorised under exocrine pancreatic tumors by the World Health Organization in 2000 [5]. It predominantly affects young women and children [3,4]. The tumor may progress to very large dimension (30 cm) without any metastasis or ascites. Cure had been reported even in the basis of very large dimention or metastasis [3,4,6-9]. As well, liver transplantation for liver metastasis of SPT had been reported previously [10].
Case
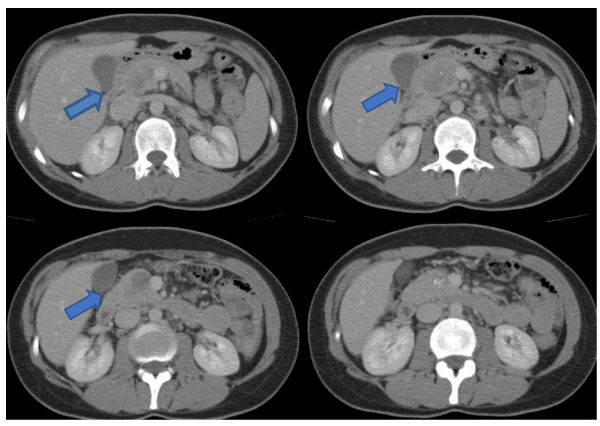
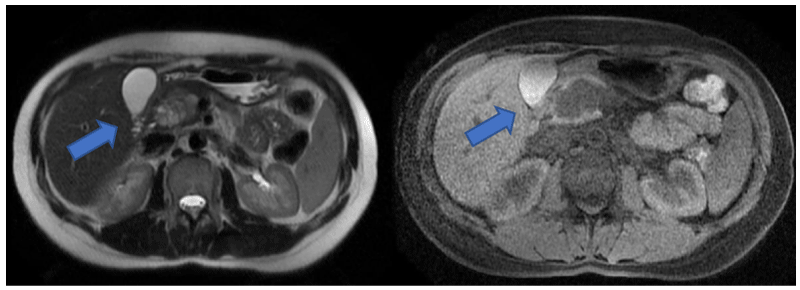
Patient: Thirty years-old woman admitted to our clinic after the diagnosis of pancreatic head mass by computed tomography (CT) in another hospital. When she came to our clinic her biochemical tests, tumor markers CEA, CA 19-9 and neuron specific enolase (NSE) levels are all in normal range and hypervascular, cystic and solitary well-capsulated roundy 4 cm pancreatic head mass was seen in the contrast enhanced abdominal CT. She was very young, she had no malignancy risk, the mass is wellshaped (not seem infiltratively and invaded any structure) with cystic parts. So the diagnosis is the possible benign or premalignant behavior pancreatic mass. Solid pseudopapillary tumor or neuroendocrine tumor are the suspicious diagnosis. Findings are the similar in magnetic resonance ımaging (MRI). When CT (Figure 1) and MRI (Figure 2) evaluated upon surgical decision there is no neighbor organ infiltration or vasculary invasion, surgical removal with negative surgical margins should be possible, so we did not prefer to take potential risk of biopsy, even endoscopically. Whipple operation performed with the pylorus preservation. Pathology reported that the tumor was well differentiated, well circumferentially solid pseudopapillary tumor of the pancreas, resected with all negative surgical margins and without any lymph node metastasis. At the 44th month of the surgery she is following up without any recurrent disease.
Discussion
SPT has shown a progressive increase in incidence, from 0.2-2.7 % of all exocrine tumors of the pancreas in the 1980’s, to 6% in more recent reports, being higher in Asia [1,11,12]. Some authors have related this effect to specialization, improvement in diagnostics and wider recognition of the disease [10]. Although male patients have been reported, it predominantly affects young women, especially black and Asian, between 20 and 30 years of age [1,9,13,14]. Our patient was 30 years-old woman with mild symptoms at the diagnosis.
SPT is often asymptomatic until the tumor reaches larger size. In our case, she had 4 cm mass at the pancreatic head without any specific symptom and without invasion to surrounding structures. Abdominal pain or tenderness, palpable mass and jaundice are the most common reported symptoms [9,11,15-17]. Preoperatively, radiological diagnosis can be possible, a well localized and encapsulated, complex large masses (with solid and cystic components) without dissemination may encountered a suspicion [2,9,13,18,19]. In some patients all the tumor could be seem solitary, cystic part is not a rule. These findings especially in young females recedes experiments from adenocarcinoma, and also from neoadjuvant treatment choice.
Percutaneous biopsy may facilitate preoperative diagnosis [9,16,20,21]. But we know that it is not an easy and uncomplicated procedure such an complex-risky area, some authors reported the potential role of previous biopsy or trauma (drainage because of misdiagnosis etc.) in seeding and development of peritoneal carcinosis in pancreatic tumors [22,23]. And also additional contribution to the biopsy in this situation is contrary.
The treatment choice is basicly focused on the removal of the tumor totally. Reports have demonstrated resectability and long term survival with isolated portal vein and arterial resection and reconstruction [1,24].
Local invasion of peripancreatic tissue is the most common malignant pathologic feature [8,2,5]. Although angioinvasion and perineural invasion are regarded as evidence of malignant potential according to the WHO classification [5]. Old age, male sex, and tumor size larger than 5 cm has been reported as predictor factors of the malignant form [25,26].
Local recurrence or metastasis is unusual, and have been reported to be particularly rare in elderly patients [8,14]. The most common organ for metastasis is the liver, but lymph node, adrenal or peritoneal metastases have been reported [1,8,10,13,27]. Even in the presence of disseminated disease, patients have a good prognosis as long as the lesions are resected completely [1,10,27]. Tang et al. reported that the overall 5 year survival was 97% when metastases were removed successfully [14]. A case of liver transplantation was reported from Nagoya for unresectable multiple liver metastases of SPT (at the second year of the operation, she was disease free) [10].
In conclusion, due to the slow-growing character and low malignant potential, and favorable prognosis even in the presence of dissemination, an aggressive surgical approach from metastasectomy to liver transplantation, is advisable and removal of the tumors with negative surgical margins may result in curable disease [24,28,29]. Resectability rate and expectance for disease-free survival is high even in the presence of major vascular invasion or distant metastases [10,24,28,30]. Late recurrences were reported and this may indicate long term follow-up for these patients [9].
- Martin RC, Klimstra DS, Brennan MF, Conlon KC (2002) Solid pseudopapillary tumor of the pancreas: A surgical enigma? Ann Surg Oncol. 9:35-40. Link: https://goo.gl/1C46kq
- Kim CW, Han DJ, Kim J, Kim YH, Park JB, et al. (2011) Solid pseudopapillary tumor of the pancreas: Can malignancy be predicted? Surgery. 149:625-34. Link: https://goo.gl/iyrVzY
- Chao HC, Kong MS, Lin SJ, Lou CC, Lin PY (2000) Papillary cystic neoplasm of the pancreas in children: Report of three cases. Acta Peadiatr Taiwan. 41:101-105. Link: https://goo.gl/GUhevS
- Frantz VK (1959) Papillary tumors of the pancreas: Benign or malignant? Tumors of the pancreas. In: Atlas of Tumor Pathology, Section 7, Fascicles 27 and 28.Washington, DC, USA: Armed Forces Institute of Pathology. 32-3.
- Kloppel G, Luttges J, Klimstra D (2000) Solid-pseudopapillary neoplasm. In: Hamilton SR, Aaltonen LA, eds. World Health Organization Classification of Tumours: Pathology and Genetics of Tumours of the Digestive System. Lyon, France: IARC Press. 246-8.
- Compagno J, Oertel JE, Kremzar M (1979) Solid and papillary epithelial neoplasms of pancreas, probably of small duct origin. A clinicopathologic study of 52 cases. Lab İnvest. 40:248.
- Klöppel G, Morohoshi T, John HD, Oehmcihen W, Opitz K, et al. (1981) Solid and cystic acinar cell tumor of the pancreas: A tumor in young women with favourable prognosis. Virchows Arch A Pathol Anat Histopathol. 392:171-183.
- Hassan I, Celik I, Nies C, Zielke A, Gerdes B, et al. (2005) Succesful treatment of solid pseudopapillary tumor of the pancreas with multiple liver metastases. Pacreatology. 5:289-294. Link: https://goo.gl/bqCCFv
- Romics L Jr, Oláh A, Belágyi T, Hajdú N, Gyurus P, et al. (2010) Solid pseudopapillary neoplasm of the pancreas--proposed algorithms for diagnosis and surgical treatment. Langenbecks Arch Surg. 395:747-55. Link: https://goo.gl/5XBhHF
- Sumida W, Kaneko K, Tainaka T, Ono Y, Kiuchi T, et al. (2007) Liver transplantation for multiple liver metasases from solid pseudopapillary tumor of the pancreas. J Pediatr Surg. 42: e27-31. Link: https://goo.gl/WfDHe3
- Chen X, Zhou GW, Zhou HJ, Peng CH, Li HW (2005) Diagnosis and treatment of solid pseudopapillary tumors of the pancreas. Hepatobil Panc Dis Int. 4:456-459.
- Siquini W, Marmorale C, Guercioni G, Stortoni P, Bearzi I, et al. (2006) Solid pseudopapillary tumour of the pancreas. A report of three cases and a review of the literature. Chir Ital. 58:235-245.
- Bhanot P, Nealon WH, Walser EM, Bhutani MS, Tang WW, et al. (2005) Clinical, imaging, and cytopathological features of solid pseudopapillary tumor of the pancreas: a clinicopathologic study of three cases and review of the literature. Diagn Cytopathol. 33:421-428. Link: https://goo.gl/nGtCmD
- Tang LH, Aydın H, Brennan M, Klimstra DS (2005) Clinically aggressive solid pseudopapillary tumors of the pancreas: A report of two cases with component of undifferentiated carcinoma and a comparative clinicopathologic analisys of 34 conventional cases. Am J Surg Path. 29:512-519. Link: https://goo.gl/UAscAA
- Kosmahl M, Pauser U, Peters K, Sipos B, Lüttges J, (2004) Cystic neoplasms of the pancreas and tumor like lessions with cystic features: a review of 418 cases and a classification proposal. Virchows Arch. 445:168-178. Link: https://goo.gl/m79AR4
- Zeytunlu M, Fırat O, Nart D, Coker A, Yüzer Y, et al. (2004) Tekesin O, Ozutemiz O, Killi R: Solid and cystic papillary neopasms of the pancreas: Report of four cases. Turk J Gastroenterol. 15:178-182. Link: https://goo.gl/NZH9Tb
- Adamthwaite JA, Verbeke CS, Stringer MD, Guillon PJ, Menon KV (2006) Solid pseudopapillary tumour of the pancreas: Diverse presentation, outcome and histology. J Pancreas. 7: 633-64. Link: https://goo.gl/nBa4Jg
- Kang WM, Liao Q, Zhao YP, Hu Y (2004) Diagnosis and surgical treatment of solid pseudopapillary tumor of the pancreas. Zhongguo Yi Xue Ke Xue Yuan Xue Bao. 26:310-312. Link: https://goo.gl/qeemQt
- Yang F, Jin C, Long J, Yu XJ, Xu J, et al. (2009) Solid pseudopapillary tumor of the pancreas: a case series of 26 consecutive patients. Am J Surg. 198:210-5. Link: https://goo.gl/6VutiL
- Huang HL, Shih SC, Chang WH, Wang TE, Chen MJ, et al. (2005) Chan YJ: Solid pseudopapillary tumor of the pancreas: Clinical experience and literature review. World J Gastroenterol. 11:1403-1409. Link: https://goo.gl/bxjpXJ
- Jani N, Dewitt J, Eloubeidi M (2008) Endoscopic ultrasound-guided fine-needle aspiration for diagnosis of solid pseudopapillary tumors of the pancreas: a multicenter experience. Endoscopy. 40:200-3. Link: https://goo.gl/VXoDQV
- Levy P, Bougaran J, Gayet B (1997) Diffuse peritoneal carsinosis of pseudo-papillary and solid tumor of the pancreas. Role of abdominal injury. Gastroenterol Clin Biol. 21:789-93. Link: https://goo.gl/zBduAr
- Alahyane A, Echarrab M, Lachkar A, Belmir H, Fahssi M, et al. (2009) Ne pas biopsier les tumeurs pseudopapillaires et solides du pancreas. Gastroenterol Clin Biol. 33:501-2.
- Bilge O, Tekant Y, Emre A, Acarlı K, Alper A, et al. (1995) Solid and cystic tumors of the pancreas: A report of two cases. J Hep Bil Pancr Surg. 2:431-34. Link: https://goo.gl/fiEH3t
- Kang CM, Kim KS, Choi JS, Kim H, Lee WJ, et al. (2006) Solid pseudopapillary tumor of the pancreas suggesting malignant potential. Pancreas. 32:276-280. Link: https://goo.gl/z1xJFE
- Lam KY, Lo CY, Fan ST (1999) Pancreatic solid-cystic-papillary tumor:clinicopathologic features in eight patients from Hong Kong and review of the literature. World J Surg. 23:1045-50. Link: https://goo.gl/m1HR18
- Gonzalez-Campora R, Martin JJR, Rodriguez JLV, Salaverri OC, Vazquez HA, et al. (1995) Papillary cystic neoplasm of the pancreas with liver metastasis coexisting with thyroid papillary carcinoma. Arch Pathol Lab Med. 119:268-73. Link: https://goo.gl/6MtZCL
- Yoon DY, Hines OJ, Bilchik AJ, Lewin K, Cortina G, et al. (2001) Reber HA: Solid and papillary epithelial neoplasms of the pancreas: aggressive resection for cure. Am Surg. 67:1195-1199. Link: https://goo.gl/kVFhMi
- Das G, Bhuyan C, Das B, Sharma J, Saikia B, et al. (2004) Spleen preserving distal panreatectomy following neoadjuvant chemotherapy for papillary solid and cystic neoplasm of pancreas. Indian J Gastroent. 23:188-189. Link: https://goo.gl/9JrKSV
- Mete Ö, Yegen G, Güllüoglu MG, Kapran Y, Klöppel G (2011) An unusual clinical presentation of pancreatic solid pseudopapillary tumor with ovarian metastases: a diagnostic dilemma. Int J Surg Pathol. 19:342-5. Link: https://goo.gl/KqCLN4
- Yagihashi S, Sato I, Kaimori M, Matsumoto J, Nagai K (1988) Papillary and cystic tumor of the pancreas. Two cases indistinguishable from islet cell tumors. Cancer. 61:1241-1247. Link: https://goo.gl/aVHPAE
- Wang KS, Albanese C, Dada F, Skarsgard ED (1998) Papillary-cystic neoplasm of pancreas: A report of three pediatric cases and literature review. J Pediatr Surg. 33:842-845. Link: https://goo.gl/QGcao3
- Strauss JF, Hirsch VJ, Rubey CN, Pollock M (1993) Resection of a solid and papillary epithelial neoplasm of the pancreas following treatment with cisplatinum and 5-FU: A case report. Med Pediatr Oncol. 21:365-367. Link: https://goo.gl/HgGJ3A
- Freid P, Cooper J, Balthazar E, Fazzini E, NewallJ (1985) A role for radiotherapy in the treatment of solid and papillary neoplasms of the pancreas. Cancer. 56:2783-2785. Link: https://goo.gl/BMphv6
- Campanile M, Nicolas A, Lebel S, Delarue A, Guys JM, et al. (2010) de Lagausie P. Frantz's tumor: Is mutilating surgery always justified in young patients? Surg Oncol.
- Serra S, Chetty R (2008) Revision 2: an immunhistochemical approach and evaluation of solid pseudopapillary tumour of the pancreas. J Clin Pathol. 61:1153-59.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
