Archives of Otolaryngology and Rhinology
Early clinical experience using the maxillary sinus antrostomy in “office rhinology”- currently dominated by balloon sinus dilation
Gary J Nishioka*
Cite this as
Nishioka GJ (2018) Early clinical experience using the maxillary sinus antrostomy in “office rhinology” - currently dominated by balloon sinus dilation. Arch Otolaryngol Rhinol 4(2): 044-047. DOI: 10.17352/2455-1759.000074Background: Is there a role for the maxillary sinus anstrostomy (MSA) in office rhinology which currently is dominated by balloon dilation (BSD)?
Introduction: The objective of this study was to retrospectively examine “office rhinology” patients who underwent in-office MSAs and identify relevant qualitative differences when compared to patients who underwent a maxillary BSD procedure, “independent” of clinical outcome or efficacy.
Methods: A retrospective chart review was performed over a two-year interval and 5 patients were identified who underwent bilateral MSAs (10 sides total) as an office rhinology procedure for CRS without nasal polyps refractory to medical management with paranasal sinus CT scans showing persistent maxillary sinus radiographic changes. All patients underwent concomitant anterior ethmoidectomies with no other procedures performed, and were followed for a minimum of 4 months. A randomly selected cohort of patients who underwent office maxillary BSD procedures and partial anterior ethmoidectomies were used as a historical reference.
Results: 1) MSAs were easily performed and no intraoperative or postoperative complications were encountered. All patients could return to light activity within 48 hrs. 2) Removal of the uncinate process with the MSA provided superior visualization and access to the anterior ethmoid sinuses compared to the maxillary BSD patients. 3) The intact and often medialized uncinate process in maxillary BSD patients made examination of the maxillary sinus dilation site very difficult postoperatively, even with very angled endoscopes. In MSA patients endoscopic inspection of the antrostomy and sinus was very easy. 4) Removal of the uncinate process with the MSA procedure permited easy instrument access into the maxillary sinus if needed. In maxillary BSD patients instrument access into the maxillary sinus was essentially impossible.
Conclusion: Evolution of office rhinology with increased surgeon comfort with a wider range of procedures gives the MSA a useful place in office rhinology alongside BSD.
Introduction
Balloon sinus dilation (BSD) or balloon sinuplasty (BSP) was introduced in September 2005 as a minimally invasive mucosal sparing alternative to traditional endoscopic sinus surgery in which sinus ostia or sinus outflow tracts are dilated with a small balloon catheter [1]. One major change with BSD is its transition from the operating room to office setting in selected adult patients. BSD as an office procedure has seen a dramatic rise [2-4], although the data supporting BSD is still reported to be “incomplete 5. Despite numerous publications the accumulated data remains inadequate for development of clinical guidelines, but a clinical consensus statement for balloon dilation of the paranasal sinuses has been recently published [6].
As an office procedure BSD of the sphenoid and frontal sinuses are relatively easy to perform and appear to have significantly less patient morbidity than a surgical sphenoidotomy (with tissue removal to create an antrsotomy) and Draf 2a frontal sinusotomy [7], respectively.
Although the gold standard maxillary sinus antrostomy (MSA) performed in the operating room setting has been briefly described as a potential office procedure in 2005 by Amstrong [8], it has largely been avoided perhaps because it has been beyond the comfort zone of most surgeons. Consequently, with BSD dominating sinus procedures in office rhinology the MSA has not been looked at as a feasible procedure in the office setting, being perceived as more difficult and invasive because it does require some tissue removal. As surgeons have become comfortable with office BSD procedures, surgeon comfort in performing other surgical office rhinology procedures encompassing both bone as well as soft tissue has been reported [9].
A recent article [10] describing a modified maxillary BSD procedure, incorporating a partial or complete uncinectomy, demonstrates further expansion of office rhinology in sub-groups of patients needing post-procedure sinus cavity monitoring and access, sharing some surgical technique qualities with the MSA. As office rhinology develops the surgical difficulty between the maxillary BSD and the MSA has narrowed considerably for the office setting.
The objective of this study was to retrospectively examine “office rhinology” patients who underwent in-office MSAs and identify what qualitative differences were seen when compared to patients who underwent a maxillary BSD procedure, “independent” of clinical outcome or efficacy.
Material and Methods
A retrospective chart review was performed from January 2015 through January 2017. 5 patients, 3 females and 2 males, ages 18-65, were identified who underwent bilateral MSAs (10 sides total) as an office rhinology procedure for CRS without nasal polyps refractory to medical management with paranasal sinus CT scans showing persistent maxillary sinus radiographic scores of 1 or greater using a modified Lund-MacKay scoring system [11]. All patients underwent their procedures in a dedicated office surgery suite with monitoring using an anesthesia regimen consisting of oral sedation (with monitoring), and topical and infiltrative local anesthesia [12]. All patients underwent concomitant anterior ethmoidectomies but no other procedures and were followed for a minimum of 4 months.
Using a 00 or 300 rigid nasal endoscope, with camera and video stack, the uncinate process was visualized. The maxillary anstrostomy procedure began with placing a maxillary sinus ball tip seeker into the infundibular space around the posterior edge of the uncinate process. The uncinate process was then mobilized medially increasing the infundibular space for greater access. Using a rotating micro-backbiting forcep a modified partial or complete uncinectomy was performed. Byun et al [13] in 2014 showed that a partial uncinectomy can be used successfully and without adverse sequela for maxillary antrostomies in patients with localized maxillary sinus pathology. Performing an “office” maxillary sinus antrostomy with a modified partial uncinectomy (with additional tissue removed as needed to allow full visualization of the bulla ethmoidalis) was easier and less invasive than a complete uncinectomy. A small olive-tip curved suction was then placed through the maxillary sinus natural ostia and the posterior fontanelle was pushed posteriorly enlarging the opening to the maxillary sinus cavity. Using a small rotating backbiting forcep soft tissue was removed from the anterior portion of the maxillary sinus natural ostia if needed. Using 0° and 45° thru biting forceps further enlargement of the maxillary sinus antrostomy posteriorly was performed if needed. Inspection of the maxillary sinus cavity was then performed, and if instrument access into the maxillary sinus to remove fluid or tissue was needed it was performed at this time. Although not essential for completing the maxillary sinus antrostomy, a powered microdebrider used for the anterior ethmoidectomy was available and could be utilized for the maxillary antrostomy if desired; such as refinement of the uncinectomy or enlargement of the antrostomy site. Bipolar and monopolar suction cautery were also available if needed.
A randomly selected cohort of patients who underwent office maxillary BSD procedures and partial anterior ethmoidectomies were used as a historical reference. An IRB exemption was obtained from IntegReview IRB, Austin, Texas for this study.
Results
Several observations were made with performing the standard MSA procedure versus the maxillary sinus BSD procedure as an office procedure, using prior experience with BSD as a reference.
1. Although the MSA required some tissue removal, the MSA was easily performed without difficulty. No intraoperative or postoperative complications were encountered. All patients could return to light activity within 48 hours, and all of these patients underwent partial anterior ethmoidectomies.
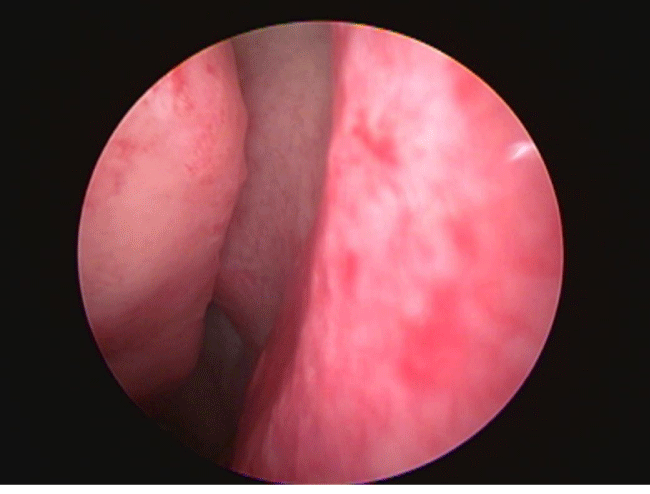
2. Removal of the uncinate process with the MSA provided superior visualization and access to the bulla ethmoidalis and anterior ethmoid sinuses both intra-operatively and postoperatively, compared to maxillary BSD patients with an intact uncinate process figure 1.
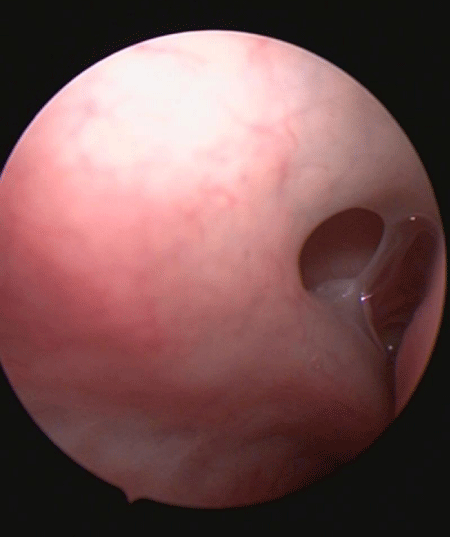
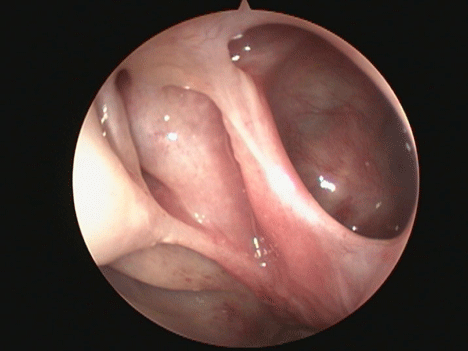
3. In maxillary BSD patients the intact and often medialized uncinate process made examination of the maxillary sinus dilation site very difficult, even with very angled endoscopes figure 2. In MSA patients, endoscopic inspection of the antrostomy opening and sinus cavity was comparatively very easy and comfortable for the patient figure 3.
4. Removal of the uncinate process with the MSA procedure permitted easy instrument access into the maxillary sinus (if needed) both at the time of the procedure and at all postoperative follow-up appointments. In maxillary BSD patients access into the maxillary sinus was essentially impossible.
Discussion
As office rhinology evolves and surgeon comfort increases the surgical technique difficulty gap between the MSA and maxillary BSD procedure has closed considerably. Furthermore, “independent” of clinical outcome and efficacy, although the MSA requires some tissue removal it is still minimally invasive with very low morbidity and rapid recovery. Although the MSA surgical technique used in this retrospective study is presented, variations in surgical technique among surgeons would not be a significant factor in the findings observed.
Several distinct potential advantages of the MSA compared to the maxillary BSD procedure revolves around removal of the uncinate. If ethmoid surgery is to be concomitantly performed removal of the uncinate process with the MSA procedure increases surgical visibility and access to the bulla ethmoidalis and anterior ethmoid sinuses.
Intraoperative and postoperative examination of the maxillary sinus and access into the maxillary sinus is much better with the MSA procedure. The intact uncinate process makes inspection of the maxillary sinus dilation site in BSD patients difficult even with very angled endoscopes, and instrument access into the sinus cavity impossible. If instrument access were attempted in the maxillary BSD patient lateralization of the uncinate process and compression of the infundibular space could occur potentially resulting in an adverse sequela.
Conclusion
Office rhinology is evolving and with increased surgeon comfort in performing office rhinology procedures, the gold standard MSA procedure (with the described potential advantages compared to the maxillary BSD procedure) could have a useful role to play if added to the surgeons “office rhinology” armamentarium in selected patients. There may be times based on the needs and goals of the surgeon that the MSA would be a preferred choice over the maxillary BSD, and the surgeon can have confidence the procedure could easily be performed in the office setting versus the operating room with very low patient morbidity and rapid recovery.
- Stewart AE, Vaughan WC (2010) Balloon sinuplasty versus surgical management of chronic rhinosinusitis. Curr Allerg Asthma Rep 10: 181-187. Link: https://tinyurl.com/yaqyvzp4
- Sikand A, Silvers SL, Pasha R, Shikani A, Karanfilov B, et al. (2015) Office-based sinus dilation: 1 follow-up of a prospective, multicenter study. Ann Otol Rhinol Laryngol Link: https://tinyurl.com/y8p5j8zw
- Gould J1, Alexander I, Tomkin E, Brodner D (2014) In-office, multisinus balloon dilation: 1-year outcomes from a prospective, multicenter, open label trial. Am J Rhinol Allergy 28: 156-163. Link: https://tinyurl.com/ya6rz7zt
- Karanfilov B, Silvers S, Pasha R, Sikand A, Shikani A, et al. (2013) Office-based balloon sinus dilation: a prospective, multicenter study of 203 Patients. Int Forum Allerg Rhinol 3: 404-410. Link: https://tinyurl.com/y8z2yoo6
- Levy JM, Marino MJ, McCoul ED (2016) Paranasal sinus balloon catheter dilation for treatment of chronic rhinosinusitis: A systemic review and meta-analysis. Otolaryngol Head Neck Surg 154: 33-40. Link: https://tinyurl.com/yccrj922
- Piccirillo JF, Payne SC, Rosenfeld RM, Baroody FM, Batra PS, et al. (2018) Clinical consensus statement: Balloon dilation of the sinuses.? Otolaryngology- Head Neck Surg 203-214. Link: https://tinyurl.com/yc3x2t6v
- Hathorn IF, Pace-Asciak P, Habib AR, Sunkaraneni V, Javer AR (2015) Randomized controlled trial: hybrid technique using balloon dilation of the frontal sinus drainage pathway. Int Forum Allergy Rhinol 5: 167-173. Link: https://tinyurl.com/y7e829lm
- Armstrong M Jr (2015) Office-based procedures in rhinosinusitis. Otolaryngol Clin N Am 38: 1327-38. Link: https://tinyurl.com/y7e829lm
- DelGaudio JM, Ochsner MC v(2015) Office surgery for paranasal sinus recirculation. Int Forum Allergy Rhinol 5: 326-8. Link: https://tinyurl.com/ybookdcb
- (2018) modified in-office maxillary balloon sinus dilation for post-procedure sinus monitoring and access. Int Arch Otorhinolayngol 22: 68-72. Link: https://tinyurl.com/y89mdkoj
- Okushi T, Nakayama T, Morimoto S, Arai C, Omura K, et al. (2013) A modified Lund-MacKay system for radiological evaluation of chronic rhinosinusitis. Auris Nasus Larynx 40: 548-53. Link: https://tinyurl.com/yb4yqzh6
- Nishioka GJ (2017) the maxillary nerve block for in-office hybrid balloon sinus dilation procedures: A preliminary study. Ear Nose Throat J 96: 31-35. Link: https://tinyurl.com/y7y9pvy9
- Byun JY, Lee AY (2014) Usefulness of partial uncinectomy in patients with localized maxillary sinus pathology. Am J Otolaryngol 35: 594-595. Link: https://tinyurl.com/ydxsczmm

Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.
 Save to Mendeley
Save to Mendeley
