Global Journal of Perioperative Medicine
A case report on Anaesthesia and Ventriculo-Peritoneal Shunt with Hydrocephalus
Yilkal Tadesse Desta*
Cite this as
Desta YT (2022) A case report on Anaesthesia and Ventriculo-Peritoneal Shunt with Hydrocephalus. Glob J Perioperative Med 6(1): 001-004. DOI: 10.17352/gjpm.000010Copyright License
© 2022 Desta YT. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Introduction
Childhood hydrocephalus is a common disorder in which too much Cerebrospinal Fluid (CSF) accumulates within the ventricles (fluid-containing spaces) of the brain and is usually the-ted by cerebrospinal fluid shunting using a ventriculoperitoneal or ventriculoarterial shunts. The most common condition is hydrocephalus, where there is dilation of the ventricular system due to an obstruction in the flow of CSF or decreased absorption of CSF by the arachnoid villi. Shunting of CSF is the treatment of choice in childhood hydrocephalus.
Hydrocephalus which is not caused by any of the production or absorption extrinsic causes is regarded as congenital hydrocephalus with some underlying genetic pathology. X-linked hydrocephalus is associated with aqueductal stenosis, which forms one of the most common hereditary forms of hydrocephalus affecting 10% of males with isolated idiopathic hydrocephalus. In addition to these causes, neural tube defects also cause hydrocephalus [1].
Causes
The CSF is the clear, and colorless fluid that cushions and protects the spinal cord and brain. The CSF circulates through the ventricles and bathes the brain and spinal cord after which it is reabsorbed into the bloodstream [2]. The production of CSF is performed by the ependymal cells in the choroid plexus of the lateral ventricles of the brain [3]. Under physiologic conditions, the same amount of CSF is produced and absorbed daily. Yet, when there is a disruption in the normal flow or absorption of CSF, a buildup of CSF can result. This can impair the functioning of the brain due to elevated pressure from the CSF buildup and can result in brain damage, and in severe conditions, death [4].
Case history
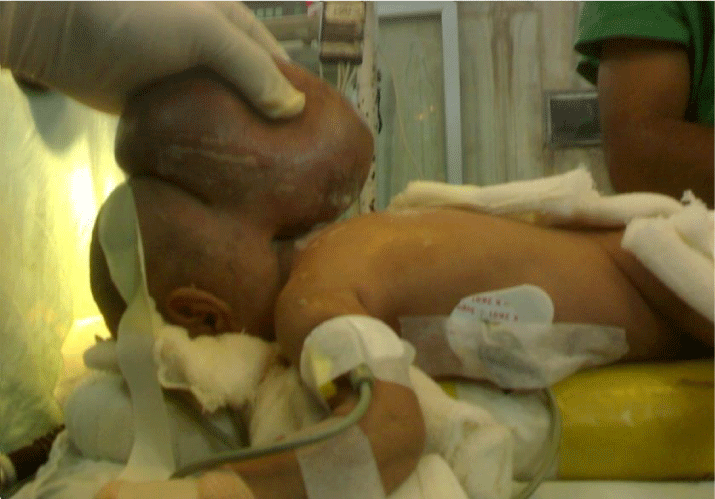
A 2 & 1/2-year old male child with mid occipital swelling, congenital hydrocephalus was admitted for surgery in Tibebe Gihon Specialized Hospital, Bahirdar, Ethiopia.
The patient underwent a right frontal craniotomy and had a right-sided ventriculoperitoneal shunt.
Hx
➔ The patient had no other coexisting medical or surgical illness previously
➔ He has no Hx of prev. anesthetic/surgical exposure
➔ No Hx of any allergy noticed from the family
➔ At the time of admission he have had Hx of diuretics (mannitol) medication but no other Figure 1.
Ixs
❊ CBC, OFT ➔ all normal range
❊ Electrolyte: all normal range
❊ Coagulation profile: all normal
❊ Ultrasonographic examination revealed the hydrocele without hernia.
❊ Blood grouping and cross-match was done
P/E
G/A: Healthy looking
V/S: BP- 90/65, PR- 96, RR-24, T0-ATT HEENT; pink conj, NIS,
LGS: No LAP
Resp: Clear & resonant
CVS: S1 &S2 well heard
NS: GCS ➔ 15/15
Clinical features of hydrocephalus widely vary according to the age of the patient and the rate of progression [3].
- Clinical features of hydrocephalus before the closure of the cranial sutures (<2 years of age ) include macrocephaly, increasing the head circumference of the head, sunsetting sign, distend scalp veins, developmental delay, poor feeding, and regression.
- After the closure of cranial sutures, the acute presentation includes headache, vomiting, drowsiness, papilledema, and coma in extreme cases.
- Chronic presentation and clinical features of normal pressure hydrocephalus include incontinence cognitive impairments and gait disturbances.
Non-surgical management
Nonsurgical management is a symptomatic treatment for hydrocephalus. Medications such as Acetazolamide or Isosorbide are used temporarily to reduce CSF production, also increase CSF absorption by producing hyperosmotic diuresis [5].
Surgical management
Babies born or children who have developed hydrocephalus usually require swift treatment to reduce the pressure on their brains. If the condition is not treated, the increase in pressure will damage the brain. Both congenital and acquired hydrocephalus can be treated with shunt surgery or neuro endoscopy [5].
Shunt surgery
Shunt surgery consists of inserting a thin tube (a shunt) in the brain, which is used to remove excess fluid from the brain. There are two major types of shunt surgeries namely ventriculoatrial shunt, ventriculoperitoneal shunt, and lumbo peritoneal shunt.
Ventriculoperitoneal shunt
With the proximal catheter being inserted into the cerebral ventricle, the distal catheter is placed into the peritoneal cavity.
Procedures
- The patient is taken into the OR; not crying and he was calm, positioned supine on the blanket like heater (says huger on it), it has also a headcover.
- Intubated under GA with smooth induction (induced with) while an assistant was also supporting for the mass
- After all, things fixed and we were happy, the patient was positioned again prone (so that the cranial incision and abdominal incision are aligned in the same plane)
- The abdomen was free (rolls under chest and pelvis applied), extremities relaxed and padded, eyes protected with ointment and thick pads
- The scalp is shaved (usually over the frontal or parietal region), and a continuous surgical field is created from head to abdomen
- The cranial incision is made over the intended region of cannulation of the ventricle, and a burr hole is made in the cranium. A subgaleal pocket is created for the valve, usually behind the ear. A separate incision is made in the abdomen, and the dissection is carried down to the level of the peritoneum. A catheter is then passed subcutaneously from the abdominal incision to the cranial incision with a special tunneling instrument (the catheter can be threaded from the cranial incision to the abdominal incision as the surgeon said)
- A ventricular catheter is then inserted into the ventricle and a small amount of CSF is drained to check the placement and patency of the catheter. The ventricular catheter is then connected to the valve, and CSF flow through the entire shunt system is checked by draining some CSF from the distal end of the peritoneal catheter
- The distal end is then placed into the peritoneal cavity and all wounds are closed
- Blood loss was not excessive ( about 30 ml, or 10% of blood volume)
- His vital sign was stable until emergency time, ETT is removed at the conclusion of the anesthetic, and transferred to PACU, just nearby the main OR .
- Post-op oxygen and regular pain relief was continued in PACU
- The temperature was maintained all the perioperative period Figure 2.
Discussion
Many are now scheduled electively before birth for repair because the defect is usually apparent on prenatal ultrasonography. Intubation is a challenge, in most cases, the options are; Supine position- with sac resting in a donut-shaped cushioned ring and weight of child supported on pelvis and portions of the spine not involved with the defect, for large defects, Lateral position- with head held in the midline by an assistant [6]. These patients are at high risk of developing allergic reactions to latex [4]; due to repeated exposure to latex products during surgery, or repeated bladder cauterizations which might manifest as hypotension and wheezing with or without rash. The discussion below implies important points regarding the optimal anesthetic approaches and considerations of this specific procedure in general.
Anesthetic technique: GETA
Summary
Ventricular shunts are inserted to ameliorate hydrocephalus or cyst formation, which may be either congenital or acquired. Many conditions exist where it is necessary to shunt CSF from the ventricles to another body cavity where it can be absorbed readily. Hydrocephalus is commonly treated by diverting CSF to the peritoneal cavity via a ventriculoperitoneal shunt (VP shunt). Patients have multisystem diseases that result from a severe injury to the developing CNS early in gestation and Intubation may also be difficult in these cases. conditions should be repaired as soon as possible to prevent complications The most common complications are the mechanical malfunction of the shunt being either by disconnection or blockage of its components Rupture of sac during the birth process, CSF leak, raised ICP (vomiting, convulsions, altered sensorium, irritability) and shunt infection (fever, unconsciousness, altered sensorium, meningitis). Regardless of the different surgical management, children with hydrocephalus still have some disabilities. Therefore, early involvement with physiotherapists via different methods of rehabilitation is essential, whether surgical or non-surgical management is required. Additionally, successful shunting is usually related to more obvious and rapid improvements in rehabilitation efforts [3]. Specific treatment procedures are numerous, functional training for activities of daily living; therapeutic exercise; manual techniques such as mobilization and stretching; and therapeutic modalities [7].
Physiotherapy goals are aimed at
- Promoting physical milestones of achievement such as sitting, crawling, standing
- Optimizing mobility independence
- Improving balance and coordination via exercise
- Stretching tight muscles via exercise
- Strengthening weak muscles via exercise
- Improving endurance and exercise tolerance.
Conclusion
- Premedication is usually not required; should be avoided in patients with ↑ ICP.
- Prophylactic antiemetics (e.g., metoclopramide 10–20mg and ondansetron 4 mg) should be given 30 min before extubation.
- Assistant must be available to maintain the head in midline position and also to ensure that no physical trauma to neuro plaque occurs
- These patients are at high risk for developing a hypersensitivity to latex
- Prone position has its own hazards and precautions to be taken, excessive rotation/flexion of the neck avoided ❊ brainstem compression, rise in ICP.
- Steinberg GK, Stoodley MA (2000) Surgical management of intracranial arteriovenous malformations. In Operative Neurosurgical Techniques, 4th edition. Schmidek HH, ed. WB Saunders, Philadelphia 1363-1391.
- Steinberg GK, Chang SD, Gerwitz RJ, Lopez JR (2000) Microsurgical resection of brain stem, thalmic and basal ganglia angiographically occult vascular malformation. Neurosurgery 46: 260-270. Link: https://bit.ly/35mKYzA
- Jaffe RA, Samuels SI (2019) Anaesthesilogists manual of surgical procedures. Neurosurgery 4th; 15-61.
- Davidson RI (1976) Peritoneal bypass in the treatment of hydrocephalus: historical review and abdominal complications. J Nuerol Neurosurg Psychiatry 39: 640-646. Link: https://bit.ly/35h9VfX
- Hashimoto T, Young WL (2001) Anesthesia-related considerations for cerebral arteriovenous malformations. Neurosurg Focus 11: e5. Link: https://bit.ly/3vaYDov
- Jerffreys RY (1987) Hydrocephalus. In Miller JD red: Northfields surgery of the central nervous system. ed 2,Oxford: Blackwell 567.
- Albala DM, Danaher JW, Huntsman WT (1989) Thomas Huntsman: Ventriculoperitoneal shunt migration into the scrotum. Am Surg 55: 685-688. Link: https://bit.ly/3pb6oHk

Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.
 Save to Mendeley
Save to Mendeley
