Rheumatica Acta: Open Access
Laryngeal Primary Amyloidosis: Differential Diagnosis of Localized Granulomatosis with Polyangiitis. Report of Two Cases
Clarissa de Queiroz Pimentel2, Luciana Depiere Lanzarin2, Frederico Adão de Oliveira Santana2, Rosa Maria Rodrigues Pereira1, Maurício Levy-Neto1 and Samuel Katsuyuki Shinjo1*
2Division of Pathology, Hospital das Clinicas HCFMUSP, Faculdade de Medicina, Universidade de Sao Paulo, Sao Paulo, Brazil
Cite this as
de Queiroz Pimentel C, Lanzarin LD, de Oliveira Santana FA, Rodrigues Pereira RM, Levy-Neto M, et al. (2017) Laryngeal Primary Amyloidosis: Differential Diagnosis of Localized Granulomatosis with Polyangiitis. Report of Two Cases. Rheumatica Acta: Open Access 1(1): 017-019. DOI: 10.17352/raoa.000004Primary laryngeal amyloidosis (PLA) and granulomatosis with polyangiitis (GPA) can present rarely with the isolated symptom of dyspnea and/or dysphonia, affecting exclusively the larynx.
Granulomatosis with polyangiitis is one of the anti-neutrophil cytoplasmatic antibodies (ANCA) associated vasculitis. It may be limited to the airways including may be exclusively laryngeal. This localized form of GPA has a difficult diagnosis because the biopsy rarely does the diagnosis and the ANCA tests are frequently negative.
In the aim of emphasizing the importance of this rare entity as a differential diagnosis of localized granulomatosis with polyangiitis, we report two cases of PLA treated in our Service.
Introduction
Primary laryngeal amyloidosis (PLA) is a rare condition with an annual incidence of 5-10 cases per million [1-3]. PLA occurs at a gender ratio of three males to one female, typically between the fourth and sixth decades of life [1-7]. It accounts for 0.5-1% of all benign tumors of the larynx, and may present with isolated symptoms of dysphonia and/or dyspnea [1-3].
As a rare entity, and with the objective of emphasizing its importance of this entity as one of the differential diagnoses of granulomatosis with localized polyangiitis (GPA), we report two cases of PLA seen at our service.
Case Reports
Case 1
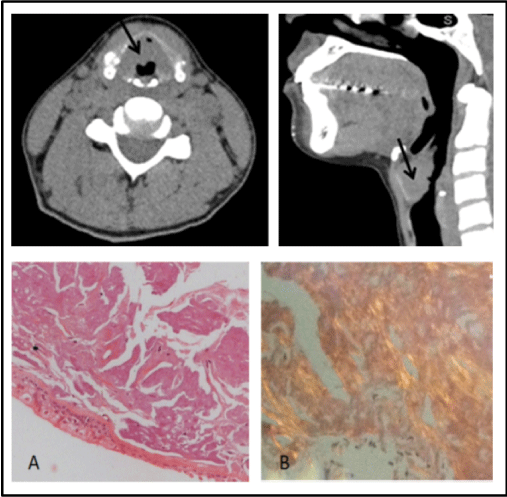
A Caucasian 40-year-old female patient was referred for rheumatologic evaluation due to suspicion of GPA. The patient had a 6-year history of progressive dysphonia, dry cough and dyspnea. She reported no systemic symptoms, comorbidities, nor prior or current history of smoking, and had no relevant family history. Physical examination was unremarkable. General laboratory exams, including serum protein electrophoresis, urinalysis, neutrophil anti-cytoplasmic autoantibody (cANCA) screening, and investigation of lower airways and sinuses were normal. Cervical computed tomography disclosed thickening of the right epiglottis, aryepiglottic folds and ventricular bands, sometimes with nodular morphology and reduction of airway lumen on topography of the ventricular bands (Figure 1A). The patient underwent videolaryngoscopy and biopsy that resulted in mucosa with extensive deposition of amphiphilic particulate matter in one membrane, affecting cartilaginous tissues of intermediate and seromucous glands, with Congo-red staining showing apple-green refringence compatible with laryngeal amyloidosis (Figure 1B). Surgical excision of the lesion was performed, with partial improvement of airway symptoms. Out-patient follow-up until the present time has revealed no further complications.
Case 2
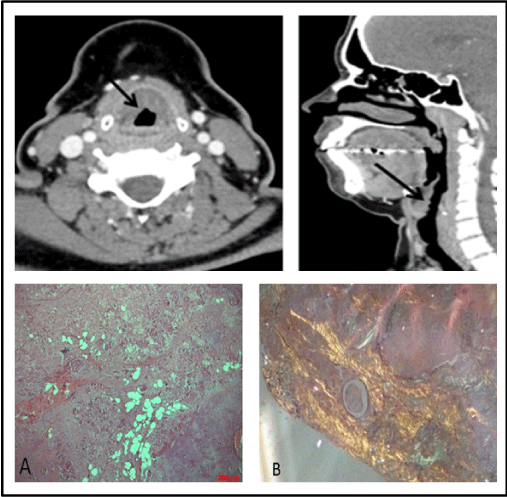
A Caucasian 41-year-old female patient was referred for rheumatologic evaluation due to suspected GPA. The patient had a 3-year history of dysphonia and had presented progressive dyspnea and wheezing for the past year. She reported no other systemic symptoms or comorbidities, with no relevant family history or history of smoking. Physical examination was unremarkable. General laboratory tests were normal, including serum protein electrophoresis, urinalysis, neutrophil anti-cytoplasmic autoantibody (cANCA) screening. Cervical computed tomography disclosed diffuse irregular thickening of the laryngeal mucosa, affecting the aryepiglottic folds, ventricular bands, vocal cords, anterior commissure and all the walls of the infraglottic larynx (Figure 2A). The patient was submitted to videolaryngoscopy and biopsy of the lesion, which demonstrated mucosa with extensive deposition of amphiphilic particulate material in the membrane, affecting cartilaginous tissue of the middle and seromucous glands, showing amyloid deposition by apple-green refringence on Congo-red staining (Figure 2B). Lesion excision was performed with good clinical evolution and no signs of systemic disease. Outpatient follow-up up to the present time has revealed no further complications.
Discussion
We report two rare, defined cases of PLA, both with initial suspicion of GPA.
Laryngeal amyloidosis is a type of amyloidosis in situ that is rarely associated with systemic disease [3,4]. The larynx is the main site affected by amyloidosis of the upper aerodigestive tract and lesions occur mainly in the vestibular fold (55%), presenting as a subepithelial nodule or edema [2,3]. The lesion is due to the extracellular deposition of amyloid fibrils, derived from immunoglobulin light chains produced by clonal plasma cells in the vicinity of the lesion, but the exact pathophysiology is unclear [1,2,4,7].
The main symptoms of the disease are: dysphonia, stridor, local pain and dyspnea, with dysphonia being the most common symptom [1,3,5]. The main differential diagnoses are: polyps, neoplasms, saccular cysts, sarcoidosis and GPA [3]. Imaging tests, such as computed tomography and magnetic resonance imaging, aid the detection of lesions, but definitive diagnosis is reached by biopsy of the lesion, with Congo red staining showing apple-green birefringence in polarized light. Systemic disease should be investigated in all cases [2-5]. Treatment consists of removal of the lesion by techniques ranging from microsurgery (method of choice) to laryngectomy, depending on the extent of the condition. The prognosis is generally good, but there is risk of relapse, and therefore patients require long-term follow-up of at least 5-7 years [1-7].
In the cases reported, the patients presented chronic airway symptoms (dysphonia, cough and dyspnea) with cervical tomography disclosing nodular lesions in the larynx with mucous thickening. The patients were evaluated by other medical specialties. Having the initial diagnostic hypothesis of GPA, the patients were subsequently referred for rheumatologic evaluation.
In cases of GPA, 80%-95% of patients present with head and neck otorhinolaryngology manifestations as initial symptoms, and this is the only involvement associated with the disease in some cases of granulomatosis with localized GPA. The larynx and trachea can also be affected with the formation of nodules, ulcers and/or stenosis. Laryngeal and tracheal cancers may be present in 25% of patients. The main symptoms include dysphonia, cough, hemoptysis, dyspnea, stridor and wheezing. In these cases, ANCA is positive in only 46-70% of cases. Although imaging tests may suggest involvement of GPA, definitive diagnosis is based on histopathology with the presence of granulomas in the vascular or perivascular region of arterioles. It is important to emphasize that this diagnosis should be considered in cases of recurrent upper respiratory tract infections, airway infections, otitis, mucosal ulcers and laryngitis. Proper diagnosis and early treatment are essential to prevent irreversible damage in cases of GPA [8,9].
Through these reports, we have shown the importance of investigating patients with chronic upper airway symptoms, considering PLA as a differential diagnosis in these conditions. Anatomopathological assessment is essential for defining these cases, including differentiation with localized GPA. In view of this, adequate diagnosis, with proper therapy and long-term follow-up allow better management of these patients, with increased likelihood of recovery, symptom reduction and improvement in quality of life.
- Valera FCP, Fomin, DS, Maggioni Jr GS, Grellet M (2004) Amiloidose localizada laríngea: relato de caso e revisão de literatura. Rev Bras Otorrinolaringol 70: 423-426. Link: https://goo.gl/FmRaSv
- Hazenberg, AJC, Hazenberg BPC, Dikkers FG (2016) Long-term follow-up after surgery in localized laryngeal amyloidosis. Eur Arch Otorhinolaryngol 273: 2613-2620. Link: https://goo.gl/DplTbg
- Szocs M, Muhlfay G, Mocan SL, Balazs A, Neagoe RM (2015) Localized laryngeal amyloidosis – a case report. Rom J Morphol Embryol 56: 597-600. Link: https://goo.gl/mDQodj
- Wang Q, Chen H, Wang S (2014) Laryngo-tracheobronchial amyloidosis: a case report and review of literature. Int J Clin Exp Pathol 7: 7088-7093. Link: https://goo.gl/nW7JAk
- Neto JC, Alves, NSC, Gondra, LA (2015) Laryngeal amyloidosis presenting as false vocal fold bulging: clinical and therapeutic aspects. Braz J Otorhinolaryngol 81: 219-221. Link: https://goo.gl/SHiIxC
- Bozkus F, Ulas T, Iynen I, Ozardali I, Sans I (2013) Primary localised laryngeal amiloidosis. J Pak Med Assoc 63: 385-386. Link: https://goo.gl/AEwj1M
- Park JH, Cheng HM (2013) Isolated laryngeal amyloidosis in a patient with a hoarse voice. BMJ Case Rep. Link: https://goo.gl/Uiu6aD
- Wojciechowska J, Krajewski W, Krajewski P, Kręcicki T (2016) Granulomatosis with polyangiitis in otolaryngologist practice: a review of current knowledge. Clin Exp Otorhinolaryngol 9: 8-13. Link: https://goo.gl/uO7ZDZ
- Trimarchi M, Sinico RA, Teggi R, Bussi M, Specks U, et al. (2013) Otorhinolaryngological manifestations in granulomatosis with polyangiitis (Wegener's). Autoimmun Rev 12: 501-505. Link: https://goo.gl/ueEpt4
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
