Open Journal of Tropical Medicine
How to avoid being re-hospitalized for patients with COVID-19
Li Shi1*, Jie Chen2 and Jiqing He1
2Acupuncture and Massage Institute, the Guangzhou University of Chinese Medicine, Guangzhou Guangdong 510405, China
Cite this as
Shi L, Chen J, He J (2021) How to avoid being re-hospitalized for patients with COVID-19. Open J Trop Med 5(1): 010-020. DOI: 10.17352/ojtm.000020Aim: How to avoid being re-hospitalized for patients with 2019 Novel Coronavirus (COVID-19) were studied.
Method: A total of 260 patients diagnosed as COVID-19 were studied with serial follow-up chest chest Computed Tomography (CT) scans and Reverse-Transcriptase–Polymerase-Chain-Reaction (RT-PCR).
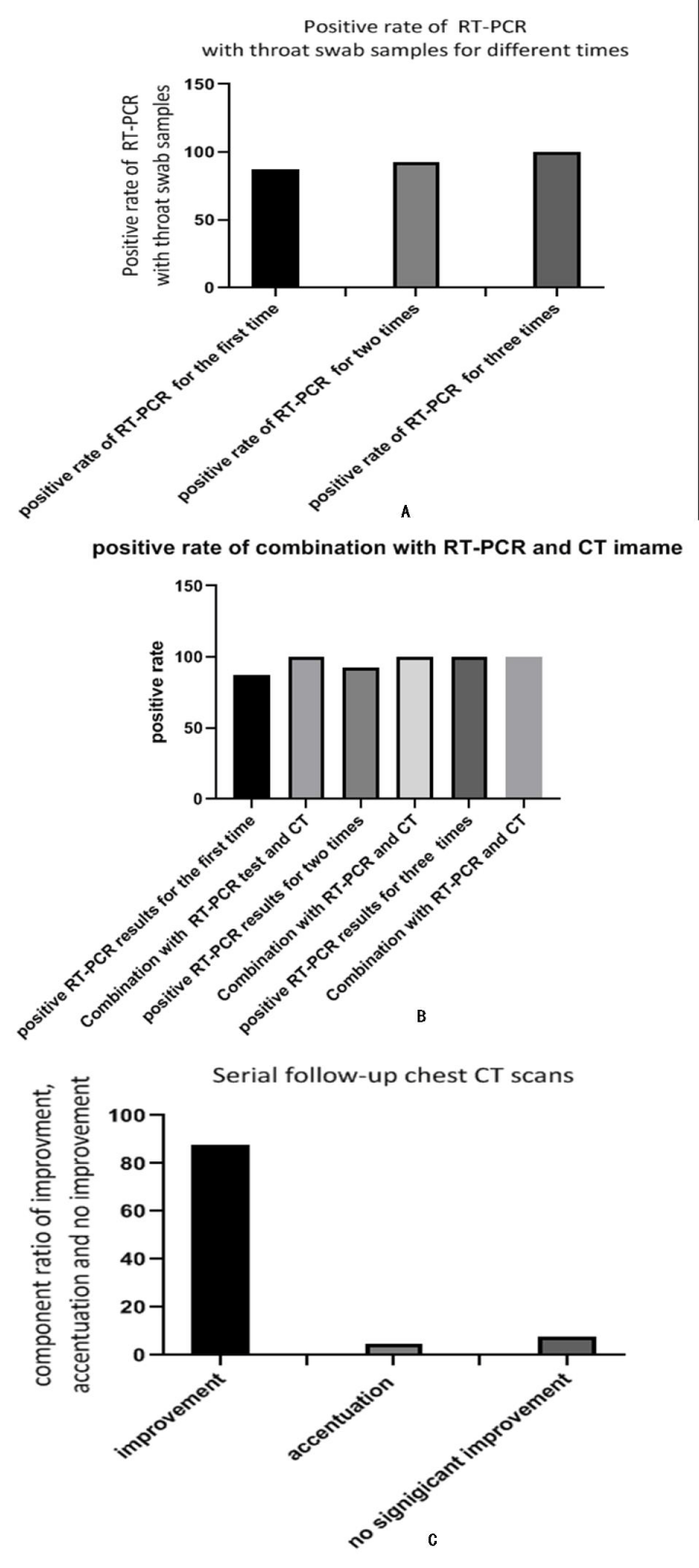
Result: Positive rates of chest CT imaging were 96.99% (252/260). Positive rates of RT-PCR were 87.70% for the first time, 92.30% for two times and 100% for three times. Multiple RT-PCR assay tests resulted in a high positive rate of RT-PCR. Combination of chest CT scans, RT-PCR lead to positive rate of 100% even for the first testing, which is conducive to COVID-19 diagnosis Two patients with COVID-19 were discharged from hospital with false-negative results of RT-PCR using the oropharyngeal swab. There was a significant progression on CT images as well as an increase in infective markers during their second admission to hospital, which indicated the progressing inflammation. Patients with complete recovery were selected. Symptoms were relieved; dissipation almost completely disappeared on CT image; infective markers significantly decreased to normal levels, which indicated that the inflammation was not progressing. Lymphocyte (LYM) percent increase to normal level.
Conclusion: Serial follow-up chest CT scans are quite important for confirming the patients with COVID-19 who resulted negative for RT-PCR of COVID-19 nucleic acid. A combination of the RT-PCR test for COVID-19 nucleic acid and other detective methods such as CT imaging are conducive to diagnosis. The roadmap how to avoid being re-hospitalized for patients with COVID-19 was provided. Patients, were not allowed to be discharged from hospital even with negative result of RT-PCR of COVID-19 nucleic acid:
Abbreviations
COVID-19: 2019 Novel Coronavirus; RT-PCR: Reverse-Transcriptase–Polymerase-Chain-Reaction; RNA: Ribonucleic Acid; COVID-19: Corona Virus Disease 2019; NCP: Novel Coronavirus Pneumonia; NCP: Novel Coronavirus Pneumonia; CFDA: the China Food and Drug Administration; CDC: the Centers for Disease Control; ARDS: Acute Respiratory Distress Syndrome; MOF: Multiple Organ Function Failure; ACE-2: Angiotensin-Converting Enzyme-2; BALF: Bronchoalveolar Lavage Fluid; WBC: White Blood Cell; NE: neutrophile Granulocyte; CRP: C-Reactive Protein; PCT: Procalcitonin; CT: Computed Tomography; LYM: Lymphocyte
Introduction
Since December 2019, Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2) caused by 2019 Novel Coronavirus (COVID-19) has generated over 89000 cases of Corona Virus Disease 2019 (COVID-19), formerly known as Novel Coronavirus Pneumonia (NCP) in China, including 2450 deaths (National Health Commission of the People’s Republic of China, 2020). In the meantime, the epidemic has spread to the other 25 countries. On January 30, 2020, WHO declared that the outbreak of COVID-19 constitutes a Public Health Emergency of International Concern. Respiratory droplets and contact are considered the main routes of transmission.
According to the diagnostic criteria (General Office of National Health Commission and General Office of National Administration of Traditional Chinese Medicine, 2020), the diagnosis of COVID-19 is confirmed by the positive result of a COVID-19 nucleic acid test of a swab sample, as the key indicator for isolation or hospitalizations.
RT-PCR tests are the most widely used method for nucleic acid assay. However, it is possible for samples obtained via throat swab to give false-negative results of RT-PCR. Thus, suspected or affected patients should be isolated until receiving two consecutive COVID-19 nucleic acid negative results.
Chest CT is a typical, routine tool used for diagnosing COVID-19, which can be immediately performed. Dynamic changes on the serial follow-up chest CT scans have not been reported for the patients with positive RT-PCR tests that turned negative, especially for the patients with false-negative results of RT-PCR. Serial follow-up chest CT scans with time-interval of 3 days or more are quite essential to confirm the patients with negative results of RT-PCR for COVID-19 nucleic acid, which is conducive to the diagnosis of COVID-19.
In the present study, we used RT-PCR as a reference standard against which we tested the performance of follow-up chest CT in diagnosing COVID-19. The dynamic conversion of RT-PCR results was studied and compared with the serial follow-up chest CT scans.
Materials and methods
Patients
By the time of April 30, 2020, a total of 260 patients who were diagnosed with COVID-19 and were subsequently admitted to and discharged from our hospital, underwent both chest CT and RT-PCR tests for several times between January 21 and March 6, 2020. The repeated RT-PCR tests were conducted up to and including one day after the initial test was performed.
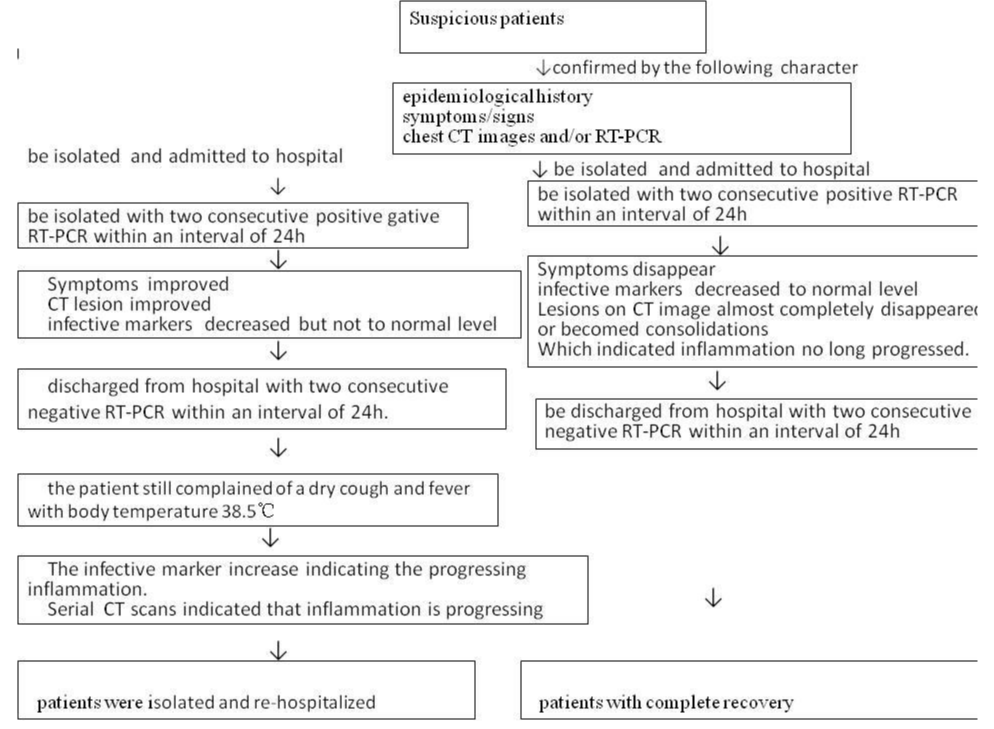
According to the latest guidelines of Diagnosis and Treatment of COVID-19 (trial seventh version) published by the China government, the diagnosis infection of COVID-19 must be confirmed by the positive result of epidemiological history, symptoms and signs, chest CT images and/or RT-PCR or gene sequencing of COVID-19 nucleic acid (Figure 1). In addition, the patients with COVID-19 could be discharged from hospital following the improvement of their clinical character and lesions on CT scan, and two consecutive negative results of COVID-19 nucleic acid.
RT-PCR assay
The RT-PCR assays were performed by using TaqMan One-Step RT-PCR Kits, which were approved by the China Food and Drug Administration (CFDA). Using viral nucleic acid extracted from oropharyngeal swab, RT-PCR assay was carried out. To accurately determine the detection limits, we serially tested diluted positive control plasmids with a dynamic range of at least seven orders of magnitude (2 x 10−4-2000 TCID50/reaction) in these assays. In our preliminary trial, reactions with ≥10 copies of this positive control plasmid were consistently positive. The amplification efficiencies of RT-PCR assay were proven. RT-PCR assay of COVID-19 nucleic acid tested using the oropharyngeal swab interval were carried out ever 24 hours.
CT scan
All chest CT images were obtained on the CT system (Optima 660, GE, America or Somatom Definition AS+, Siemens Healthineers, Germany) with patients in the supine position and adopting following parameters: tube voltage of 120 kVp, automatic tube current modulation between 30 and 70 mAs), a pitch between 0.99 and 1.22 mm, matrix with 512 × 512, slice thickness with 10 mm, a field of view with 350 mm × 350 mm.
Images were reconstructed with a slice thickness between 0.625 and 1.250 mm with the same increment. Serial follow-up chest CT scans were carried out ever 1 week interval.
Statistical analysis
All statistical analyses were performed using SPSS 21.0. Quantitative data were presented as the mean ± standard deviation (minimum-maximum) and the counting data were presented as the percentage of the total.
Result
The cases in our study were confirmed for COVID-19 by the positive result of epidemiological history, symptoms, and signs (fever, cough, fatigue and/or shortness of breath), chest CT images and/or RT-PCR or gene sequencing of COVID-19 nucleic acid. The positive rates of chest CT imaging in our cohort were 96.99% (252/260) for patients with positive and negative RT-PCR results. The typical characteristics found on chest CT in patients with COVID-19 include ground-glass 4 opacities, multifocal patchy consolidation, and/or interstitial changes with a peripheral distribution. If patients were initially positive or negative for RT-PCR, typical imaging features were observed on the chest CT scan before or within six days of the initial positive RT-PCR results in all cases. Serial follow-up chest CT scans with time-interval of three days, or more are crucial for confirming the patients with negative results of RT-PCR for COVID-19 nucleic acid, which is conducive to the diagnosis of COVID-19. In our study, follow-up chest CT scans showed improvement in 87.7% (228/260) cases(improvement(the lesions on CT image improved) or significant improvement(dissipation almost completely disappeared on CT image); progression in 4.61% (12/260) cases(progression of the lesions on CT image) and especially in 2 patients who were discharged from hospital with false-negative of RT-PCR(significant progression of the lesions or pulmonary fibrosis structural changes in the lungs), accentuations were observed; while in 7.69% (20/260) cases, there was no significant improvement. 96.99% (252/260) cases had initial positive CT consistent with or parallel to the diagnosis of COVID-19 (Figure 1 roadmap for diagnosis of COVID-19 infection, roadmap for patients second admitted to hospital, roadmap for patients with complete recovery.
The RT-PCR test for COVID-19 nucleic acid with samples obtained via throat swab has become the standard method for diagnosis of COVID-19, which have many limitations such as high false negative rate. Among 260 patients in the present study, 87.70% (228/260) showed positive RT-PCR results for the first time, 92.30% (240/260) had positive RT-PCR results for two times, and 100% (260/260) had positive RT-PCR results for three times. Multiple RT-PCR assay tests may result in a high positive rate of RT-PCR. Combination of chest CT scans, RT-PCR lead to positive rate of 100% even for the first testing, which is conducive to COVID-19 diagnosis (Figure 2 Combination of chest CT scans, single/multiple RT-PCR assays lead to positive rate of 100%).
By analyzing serial RT-PCR assays and CT scans, the mean interval time between initial positive RT-PCR test and subsequent negative RT-PCR result was 10.6 ± 1.7 days with a range of 9-15 days (n =65) for 260 patients discharged from our hospital. For the two patients who were discharged from hospital with false-negative RT-PCR results, the mean interval time between initial positive result to the negative result was 10 and 5 days and 4 and 9 days, respectively, during the second being admitted to our hospital ((Figure 2 Combination of chest CT scans, single/multiple RT-PCR assays lead to positive rate of 100%).
Case presentation
Case 1
The patient suffered from slight nausea and discomfort for 5 days without vomiting, abdominal pain, diarrhea, cold, fever, obvious cough.
The epidemiological history
The patient`s cousin came back from Wuhan on 17 January 2020. His aunt suffered from fever and was diagnosed with COVID-19 following positive test for RT-PCR of COVID-19 nucleic acid using the oropharyngeal swab test.
Past medical history
The patient was diagnosed with colorectal cancer, for which he was receiving chemoradiotherapy treatment.
Clinical examination and treatment
On admission, physical examination revealed normal vital signs. Lung auscultation revealed no rhonchi. The patient was negative for influenza A and B, parainfluenza, respiratory syncytial virus, adenovirus, Mycoplasma pneumoniae, Chlamydia pneumoniae, Rickettsia burnetii, and Legionella pneumophila. Chest CT showed double pulmonary ground-glass 4 opacities and multifocal patchy consolidation, which suggested viral pneumonia. He was positive for the RT-PCR assay of COVID-19 nucleic acid that was tested using the oropharyngeal swab by the Centers for Disease Control (CDC).
The patient was diagnosed with COVID-19 on February 6th, 2020 based on the epidemiological history, the clinical character of the respiratory tract, chest CT image, RT-PCR assay of COVID-19 nucleic acid tested using the oropharyngeal swab.
Oseltamivir, arbidol, lopinavir/ritonavir, and moxifloxacin were given. Two weeks after being admitted to hospital, the symptoms and CT lesion improved and the body temperature was back to normal. RT-PCR of COVID-19 nucleic acid with the oropharyngeal swab tests was repeatedly performed for surveillance, which resulted in negative two times during 24 hours interval. According to the criteria on discharge from hospitals in China (General Office of National Health Commission and General Office of National Administration of Traditional Chinese Medicine, 2020), the patient was discharged from hospital on January 29th.
After returning home, the patient still complained of a dry cough and fever with the highest body temperature reaching 38.5℃, for which he was admitted to our hospital on February 23, 2020. The RT-PCR of COVID-19 nucleic acid with the oropharyngeal swab test resulted in positive for 2 consecutive times (more than 1 day apart). The patient was admitted to our department for confirmation of COVID-19. The patient was re-hospitalized for low fever and occasional cough with two consecutive positive RT-PCR tests within 24 hours interval (Figure 3 roadmap for patients second admitted to hospital).
One day later, his body temperature decreased to 37.3℃. One week after being admitted to hospital, the symptoms and CT lesions improved.
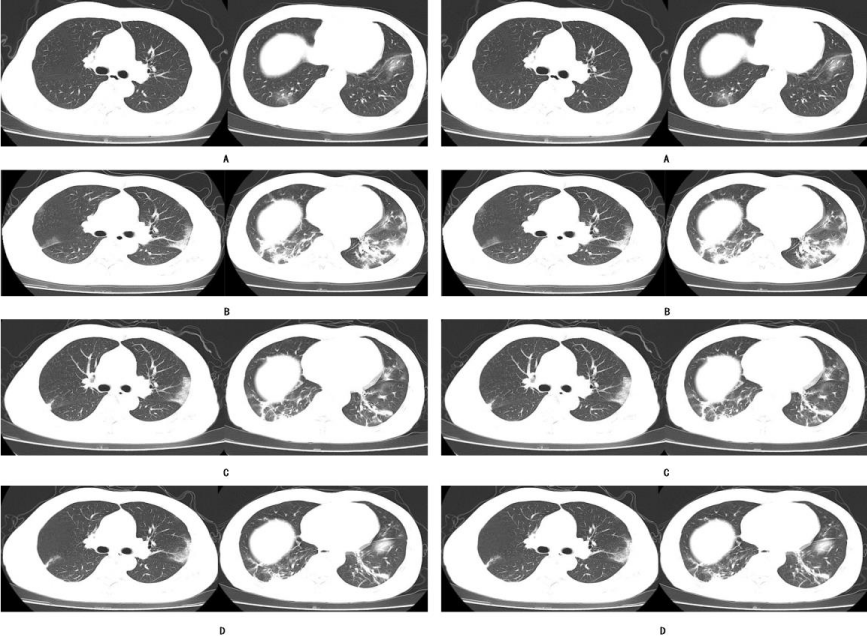
Serial CT scans (Figure 3 Serial follow-up chest CT scans of the re-hospitalized patients ------------- Left Serial follow-up chest CT scans of the first patient).
During the second admission to our hospital, follow-up chest CT scans showed more consolidation, ground-glass shadow and nodules with absorbing and reducing the area, which indicated that the inflammation was still progressing. The fifth scan (2020-02-27) showed consolidations with air-bronchogram inside with absorbing and reducing the area. By this time, the inflammation was not progressing.
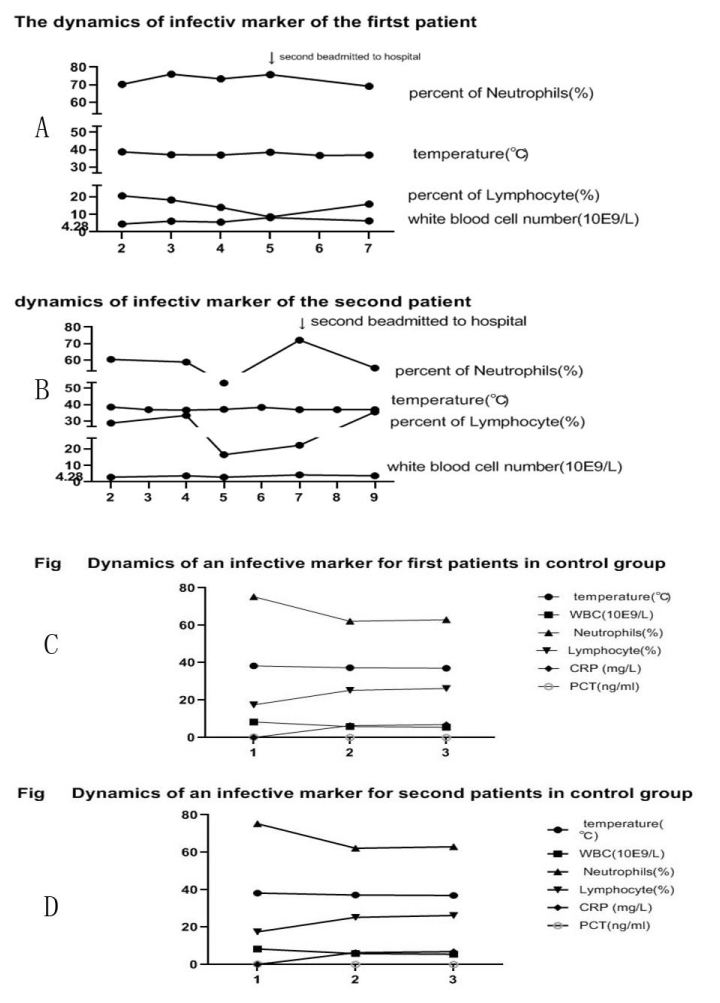
The infective marker such as procalcitonin (PCT), white blood cell number (WBC), percent of neutrophils (NE %) increase during re-hospitalization were compared with those during the first admission to our hospital (Figure 4 Dynamics of an infective marker A the first patient, who was second admitted to hospital)): WBC number, NE percent increased from 5.61 10E9/L to 8.19 10E9/L respectively with the highest body temperature at 38.5℃. PCT(ng/ml) and CRP (mg/L) increased from 0.076 ng/ml, 19.63 mg/L to 0.304 ng/ml, 119.27 mg/L respectively, which further confirmed that the inflammation was progressing.
After being admitted to hospital, the symptoms and CT lesion improved and the body temperature was back to normal. RT-PCR of COVID-19 nucleic acid using the oropharyngeal swab test was repeatedly performed for surveillance, resulting in negative for two consecutive times (more than one day apart). According to the discharge criteria of hospitals in China, the patient was again discharged on March 1st.
The patient, in general, were not allowed to be discharged from hospital with the false-negative of RT-PCR of COVID-19 nucleic acid and the progressing inflammation for the first time of admission to hospital.
Case 2
The second patient suffered from fever for 1 day that reached the highest peak of 38.8℃. He also experienced headache, chest tightness, chills, cough, stuffy and runny nose, muscle aches without nausea, vomiting, and slight pharyngitis. He came to the fever clinic at our Hospital. He showed no obvious abnormalities during the physical examination with reference to liver function, renal function, myocardial enzymes, electrolyte, and serum procalcitonin. He was negative for the influenza A and B, parainfluenza, respiratory syncytial virus, adenovirus, Mycoplasma pneumoniae, Chlamydia pneumoniae, Rickettsia burnetii, and Legionella pneumophila. CT showed double pulmonary exudative lesions in multiple ground glass samples, suggesting viral pneumonia.
The epidemiological history
The patient came from Wuhan on January 19. He was positive for the RT-PCR of COVID-19 nucleic acid using the oropharyngeal swab test by the CDC.
Clinical examination and treatemnt
The patient was diagnosed with COVID-19 on February 6th, 2020 based on the epidemiological history, the clinical character of the respiratory tract, chest CT image, and RT-PCR assay of COVID-19 nucleic acid that was tested using the oropharyngeal swab.
Oseltamivir, arbidol, Lopinavir/ritonavir, and moxifloxacin were given. One day later, the patient’s body temperature decreased to 37.0℃u. One week after being admitted to hospital, the symptoms and CT lesions improved. RT-PCR of COVID-19 nucleic acid using the oropharyngeal swab tests were repeatedly performed for surveillance, resulting negative for two consecutive times within 24 hours interval. According to the discharge criteria of hospitals in China, the patient was discharged from hospital on January 29th.
After returning home, the patient still complained of low fever with an occasional cough. He was re-admitted to our hospital on January 31th with the highest body temperature reaching 38.0℃. The RT-PCR of COVID-19 nucleic acid obtained using the oropharyngeal swab test was positive for 2 times during 24 hours interval. The patient was admitted to our department for confirmation of COVID-19.
The patient was re-hospitalized for low fever and occasional cough with two consecutive positive RT-PCR tests within 24 hours interval (Figure 3 roadmap for patients second admitted to hospital (Figure 1 roadmap for diagnosis of COVID-19 infection, roadmap for patients second admitted to hospital, roadmap for patients with complete recovery).
Serial CT scans ((Figure 3 Serial follow-up chest CT scans of the re-hospitalized patients ------------- Right Serial follow-up chest CT scans of the second patient)).
During the second admission to our hospital, follow-up chest CT scans showed multiplepatchy consolidations in both lungs and grid-like thickness of interlobular septa(Rapid progression stage), which indicated that the inflammation was still progressing. The fifth scan (2020-02-27) showed consolidations with air-bronchogram inside with absorbing and reducing the area. By this time, the inflammation was not progressing.
Clinical examination
The infective marker such as PCT, WBC number, NE percent were high during re-hospitalization (Figure 4 Dynamics of an infective marker B the second patient, who was second admitted to hospital), which indicated the progressing inflammation. The isolation was not recommended, and the patient was not allowed to being discharged from hospital with the false-negative of RT-PCR of COVID-19 nucleic acid.
After being admitted to hospital, the symptoms and CT lesion improved and the body temperature was back to normal. RT-PCR of COVID-19 nucleic acid using the oropharyngeal swab test was repeatedly performed for surveillance, resulting in negative for two consecutive times (more than one day apart).
The patient, in general, were not allowed to be discharged from hospital for the first time of admission to hospital with the false-negative of RT-PCR of COVID-19 nucleic acid and the progressing inflammation of chest CT scans and infective marker.
Patients with complete recovery on serial CT scans
In order to further study the relation between the dynamics of the infective marker and serial CT scans, patients with complete recovery on Serial CT scans were selected, who were matched for age, gender and disease severity compared with the above patients.
First patient
The first patient was diagnosed with COVID-19 on January 22, 2020 based on epidemiological history, the clinical character of the respiratory tract, chest CT image, RT-PCR assay of COVID-19 nucleic acid obtained via the oropharyngeal swab. The patient came to our hospital with fever and discomfort for 5 day with the highest temperature reaching 38.1℃, chills, cough, stuffy nose, slight pharyngitis, and muscle aches. There was a significant progression of symptoms, progression on CT image, increase of infective marker (WBC number, NE percent, temperature and PCT), which indicated that the inflammation was progressing. The patient was negative for influenza A and B, parainfluenza, respiratory syncytial virus, adenovirus, Mycoplasma pneumoniae, Chlamydia pneumoniae, Rickettsia burnetii, and Legionella pneumophila. CT showed scattered consolidation, ground glass shadow and nodules in the upper and lower lobes of the left lung, which suggested viral pneumonia.
The patient came from Wuhan on January 15. He tested positive for the RT-PCR of COVID-19 nucleic acid performed with the oropharyngeal swab test by the CDC for two consecutive times. The patient was confirmed as having COVID-19.
Oseltamivir, arbidol, lopinavir/ritonavir, and moxifloxacin were given. One day later, the body temperature decreased to 37.5℃. After admission to hospital, the symptoms improved. Accentuations of CT lesion were observed, which indicated pathological changes in the progression stage. Twelve days after being admitted to hospital, the CT lesions improved.
RT-PCR of COVID-19 nucleic acid using the oropharyngeal swab tests was repeatedly performed for surveillance, resulting negative for two times within 24 hours interval. According to the discharge criteria of hospitals in China, the patient was discharged on February 2th.
Clinical examination
During being admission to our hospital increase of infective marker(WBC number , NE percent, LYM percent, CRP and PCT) were observed, which indicated that the inflammation was progressing ((Figure 4 Dynamics of an infective marker C the first patient, who was patient with complete recovery).
After being discharged from hospital, the levels of infective markers returned to normal and never increased, which indicated that the inflammation was no longer progressing.
Serial CT scans (Figure 5 Serial follow-up chest CT scans of the second patients with complete recovery Right).
Photo E (2020-03-07): there were less consolidation with increasing density (Dissipation stage). By the time the inflammation is not progressing. Photo F(2020-04-03):lesions on CT image almost completely disappeared.
The patient was allowed to be discharged from hospital with the negative result of RT-PCR of COVID-19 nucleic acid and no progressing inflammation.
Second patient
The second patient was diagnosed with COVID-19 on January 18, 2020 based on the clinical character of the respiratory tract, chest CT image, RT-PCR assay of COVID-19 nucleic acid obtained via the oropharyngeal swab and epidemiological history. There was a significant progression of symptoms, progression on CT image, increase of infective marker such as WBC number, NE percent, LYM percent, temperature and PCT, which indicated that the inflammation was progressing. The patient was negative for influenza A and B, parainfluenza, respiratory syncytial virus, adenovirus, Mycoplasma pneumoniae, Chlamydia pneumoniae, Rickettsia burnetii, and Legionella pneumophila. CT showed scattered consolidation, ground glass shadow and nodules in the upper and lower lobes of the left lung, which suggested viral pneumonia.
The patient came from Wuhan on January 14. He tested positive for the RT-PCR of COVID-19 nucleic acid performed with the oropharyngeal swab test by the CDC for two consecutive times. The patient was confirmed as having COVID-19.
Oseltamivir, arbidol, lopinavir/ritonavir, and moxifloxacin were given. After admission to hospital, the symptoms improved. Accentuations of CT lesion were observed during the 2 weeks, which indicated pathological changes in the progression stage. Soon after, the CT lesions improved. RT-PCR of COVID-19 nucleic acid using the oropharyngeal swab tests was repeatedly performed for surveillance, resulting negative for two times within 24 hours interval. According to the discharge criteria of hospitals in China, the patient was discharged on February 2th.
Clinical examination
During being admission to our hospital increase of infective marker(WBC number , NE percent, LYM percent, CRP and PCT) were observed, which indicated that the inflammation was progressing (Figure 4 Dynamics of an infective marker D the second patient with complete recovery).
After being discharged from hospital, the levels of infective markers returned to normal and never increased, which indicated that the inflammation was no longer progressing.
Serial CT scans (Figure 5 Serial follow-up chest CT scans of the second patients with complete recovery Right). Photo D (2020-02-02): there were less consolidation with increasing density (Dissipation stage). By the time the inflammation is not progressing.Photo E(2020-02-06): lesions on CT image almost completely disappeared.
The patientwas allowed to be discharged from hospital with the negative result of RT-PCR of COVID-19 nucleic acid and no progressing inflammation.
Discussion
COVID-19 disease caused by COVID-19 constitutes a Public Health Emergency [1]. It is transmitted by respiratory droplets and contact.
COVID-19 might rapidly progress to acute respiratory distress syndrome (ARDS) and/or multiple organ function failure (MOF) with highly contagious transmission and mortality rates that reach as high as 5-10%. Patients infected with COVID-19, asymptomatic carriers, patients in the incubation period and patients discharged from hospital positive for COVID-19 nucleic acid by RT-PCR are the primary source of infection [2]. According to the guidelines(General Office of National Health Commission and General Office of National Administration of Traditional Chinese Medicine, 2020), patients with COVID-19 should be isolated until obtaining two consecutive negative COVID-19 nucleic acid tests within an interval of at least 24h [3]. Yet, it is possible to obtain false-negative results of RT-PCR for COVID-19 nucleic acid using samples obtained via throat swab. In our study, regardless of whether patients initially had positive or negative results of RT-PCR, typical imaging features were observed in almost all cases 96.99% (252/260) on the chest CT scan before or within 6 days of the positive RT-PCR results. Serial follow-up chest CT scans are quite important for confirming the patients with COVID-19 who resulted negative for RT-PCR of COVID-19 nucleic acid. A combination of the RT-PCR test for COVID-19 nucleic acid and other detective methods such as CT imaging are conducive to diagnosis [4].
In our study, two patients with COVID-19 were discharged from hospital after receiving two consecutive negative results on RT-PCR testing of nCoV nucleic acid using the oropharyngeal swab within an interval of at least 24 h. Their symptoms and CT lesions improved, and their body temperature maintained normal. According to the guideline, patients were discharged from hospital. After returning home, the patients still complained of low fever with an occasional cough. Their RT-PCR test of COVID-19 nucleic acid obtained using the oropharyngeal swab resulted positive for two consecutive times, which indicated that patients could still transmit COVID-19 to other people. The period during the first being discharge from hospital and the second being admitted to hospital were less than the incubation latent period of COVID-19, which indicated recurrence rather than reinfection of COVID-19.
Readmission and isolation were requested. There was a significant progression observed on CT images as well as an increase in infective markers during their second admission to hospital, which indicated the progressing inflammation. After being discharged from hospital for second time, the lesions on CT image improved significantly and levels of infective markers (WBC count, NE percent, temperature, PCT and CRP) returned to normal level and never increased, which indicated that the inflammation was not progressing. LYM percent increase to normal level, which indicated that CD4 and CD8 lymphocyte level increase to normal level. Immune recovery occurred, which was impaired by the infection of COVID-19.
The period between the first discharge from hospital and the second admission to hospital was shorter than the latent incubation period of COVID-19, which indicated recurrence rather than reinfection of COVID-19. The isolation was not an option, and patients could not be discharged from hospital for the false-negative of RT-PCR of COVID-19 nucleic acid obtained using the oropharyngeal swab.
In order to further study the relation between the dynamics of the infective marker and serial CT scans, patients with complete recovery were selected, who were matched for age, gender and disease severity compared with the above patients. There was a significant progression of symptoms, progression on CT image, increase of infective markers (WBC number, NE percent, LYM percent, temperature, CRP and PCT) during admission, which indicated the progressing inflammation. After a period of therapy, symptoms were relieved; dissipation almost completely disappeared on CT image; infective markers significantly decreased to normal levels, which indicated that the inflammation was not progressing. LYM percent increase to normal level, which indicated that CD4 and CD8 lymphocyte level increase to normal level. Immune recovery occurred, which was impaired by the infection of COVID-19. After being tested negative for RT-PCR of COVID-19 nucleic acid for two consecutive times (more than one day apart), the patients were subsequently discharged.
We assume that false-negative results of RT-PCR with the oropharyngeal swab were obtained due to the following reasons: the limitations of sample collection, transportation, and kit performance. The total positive rate of RT-PCR with samples obtained via throat swab was reported to be about 30% to 60% at the initial presentation, while the contagious period of COVID-19 has not yet been specified. COVID-19 nucleic acid from respiratory tract specimens may be persistent or recurrently positive during the course of COVID-19, even during recovery. Patients, asymptomatic carriers, and patients in convalescence positive for COVID-19 nucleic acid are all infectious and should remain in isolation until obtaining two consecutive negative results on COVID-19 nucleic acid test [5,6].
In our study, two patients with COVID-19 were discharged from hospital with false-negative results of RT-PCR of COVID-19 nucleic acid testing performed using the oropharyngeal swab. Their CT images revealed significant progression and pulmonary fibrosis structural changes in the lungs, where there may be a lot of hidden COVID-19.
Angiotensin-Converting Enzyme-2 (ACE-2), identified as the cell entry receptor of COVID-19, is highly expressed in the lungs rather than in the upper respiratory tract, such as oropharyngeal or nasopharyngeal tract. RT-PCR of COVID-19 nucleic acid may give false negatives when testing is performed using the oropharyngeal swab, which can be overcome using the Bronchoalveolar Lavage Fluid (BALF) specimen but with a higher exposure risk [6].
Regardless of patients initially had positive or negative results of RT-PCR, typical imaging features were observed in almost all cases 96.99% (252/260) on the chest CT scan before or within 6 days of the positive RT-PCR results. Serial follow-up chest CT scans were carried out in our patients, which is conducive to the diagnosis of COVID-19. Combination with the RT-PCR test for COVID-19 nucleic acid and other detective methods such as CT imaging are also conducive to diagnosis [4]. Monitor of infective markers (WBC number, NE percent, LYM percent, temperature, CRP and PCT) , serial follow-up chest CT scans are very important for the patients discharged from hospital with negative RT-PCR results for two consecutive times. All the discharged patients should be home-quarantined for at least 14 days and regularly tested.
Conclusion
Our results confirmed the roadmap for diagnosis of 2019-nCoV infection. Moreover, the roadmap for patients with second admission to hospital with the false-negative of RT-PCR was confirmed, in which follow-up chest CT scans (a significant progression) and increase of infective markers showed that the inflammation was still progressing.
A combination of RT-PCR test with serial follow-up chest CT scans is conducive to COVID-19 diagnosis. Monitoring infective markers (WBC number, NE percent, LYM percent, temperature, CRP and PCT) and serial follow-up of chest CT scans are very important for the patients discharged from hospital with negative RT-PCR results for two consecutive times.
Declaration of interests
Ethics approval and consent to participate: The patient in the case report was available to consent. The case has been discussed with the most senior member of staff in charge of the patient’s care, who has provided consent for this, and consent was obtained for use of accompanying radiological images from the consultant radiologist. The study was reviewed and approved by the Hainan Provincial People’s Hospital Institutional Review Board.
Consent for publication: all authors clarify consent for publication.
Availability of data and materials: The Accession Numbers of any nucleic acid sequences oratomic coordinates cited in the manuscript can be found in GeneBank of Medline.
Authors’ contributions: Li Shi and Jie Chen participated in the design of the study, carried out the molecular genetic studies, participated in the sequence alignment and drafted the manuscript; Jiqing He performed the statistical analysis.
At the point of finishing this paper, I’d like to express my sincere thanks to all those who have lent me hands in the course of my writing this paper. I’d like to express my gratitude to my supervisor and my classmates who offered me references and information on time. Without their help, it would be much harder for me to finish my study and this paper.
- Peng Z, Lou XY, Xian-Guang W, Ben H, Lei Z, et al. (2020) A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature 579: 270-273. Link: https://go.nature.com/2CFn9oR
- Camilla R, Mirjam S, Peter S, Gisela B, Guenter F, et al. (2020) Transmission of COVID-19 infection from an asymptomatic contact in Germany. N Engl J Med 382: 970-971. Link: https://bit.ly/3wB3z2U
- Zhao JY, Yan JY, Qu JM (2020) Interpretations of "Diagnosis and Treatment Protocol for Novel Coronavirus Pneumonia (Trial Version 7)". Chin Med J 133: 1347-1349. Link: https://bit.ly/3AUmZ6d
- Zu ZY, Jiang MD, Xu PP, Chen W, Ni QQ, et al. (2020) Coronavirus Disease 2019 (COVID-19): A Perspective from China. Radiology 296: E15-E25. Link: https://bit.ly/3wwbgYl
- Roujian L, Xiang Z, Juan L, Peihua N, Bo Y, et al. (2020) Genomic characterization and epidemiology of 2019 novel coronavirus: implications for virus origins and receptor binding. Lancet 395: 565-574. Link: https://bit.ly/3uR6yUb
- Zhang H, Zhou P, Wei Y, Yue H, Wang Y, et al. (2020) Histopathologic Changes and SARS-CoV-2 Immunostaining in the Lung of a Patient With COVID-19. Ann Intern Med 172: 629-632. Link: https://bit.ly/3ebjwqn
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
