Open Journal of Tropical Medicine
Henoch-Schonlein Purpura with multiple renal calculi with hydronephrosis-A Case Report
Kriti Mohan1*, Swathi Chacham2, Ajay Bharti1 and Balram Ji Omar3
2Department of Pediatrics, All India Institute of Medical Sciences, Rishikesh, Dehradun, Uttarakhand PIN- 249003, India
3Department of Microbiology, All India Institute of Medical Sciences, Rishikesh, Dehradun, Uttarakhand PIN- 249003, India
Cite this as
Mohan K, Chacham S, Bharti A, Omar BJ (2020) Henoch-Schonlein Purpura with multiple renal calculi with hydronephrosis -A Case Report. Open J Trop Med 4(1): 004-006. DOI: 10.17352/ojtm.000012Henoch-Scholein Purpura (HSP) is one of the most common vasculitic disorder of childhood and is characterised by the presence of nonthrombocytopenic purpura (and usually) palpable purpura, transient arthralgia (occasionally arthritis), abdominal symptoms and renal involvement. Here we are reporting a previously healthy adolescent male child who presented with skin, joint and gastrointestinal manifestations of HSP as well as coincidental finding of multiple calculi in right kidney causing obstructive hydronephrosis on ultrasonography. Renal calculi with HSP can be a coincidental finding but it can create diagnostic dilemma on clinical and laboratory grounds especially due to abdominal colic and other renal manifestations. So we tried to bring this case into light because this dilemma may be responsible for sufferings for the patient without timely diagnosis and treatment.
Introduction
Henoch-Scholein Purpura (HSP) occurs worldwide and affect all ethnic groups but is more common in white and Asian populations. The incidence of HSP is estimated at 14-20/100,000 children per year and affects males more often than females, with a 1.2-1.8:1 male: female ratio. Henoch–Schönlein purpura is a disease that presents with purple spots on the skin, joint pain, gastrointestinal problems, and glomerulonephritis [1]. CNS vasculitis, coma, Guillian-Barre syndrome, pulmonary haemorrhage, carditis and orchitis are rare manifestations [2]. Life threatening complications include intestinal perforation and end stage renal disease [1]. Renal calculus is neither a manifestation nor a complication of HSP as per literature but in our case renal calculi with hydronephrosis was the coincidental finding with HSP. As abdominal pain and renal involvement in the form of hypertension, hematuria and proteinuria occur in ~50% and ~25-50% of patients of HSP respectively [3], these features are found very frequently in patients with renal calculi also especially when it is associated with frequent urinary tract infection. So this may lead to confusion among treating physician and leads to delay in reaching the diagnosis and proper management.
Case report
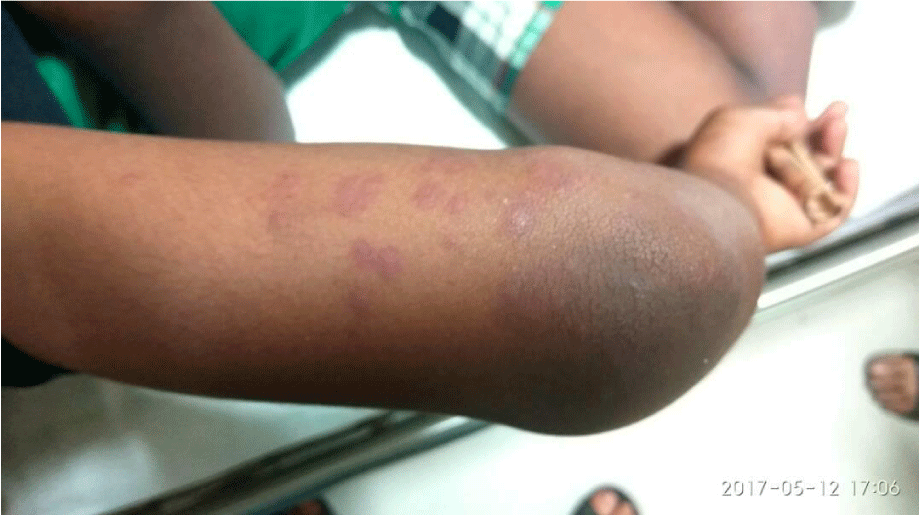
A 11 years old male child presented to the outpatient department with complaint of pain and swelling of joints, backache and non-pruritic skin rashes over feet and lower limbs (Figure 1) for the past 10 days and acute onset abdominal pain of 2days duration. Joint pain and swelling were gradual in onset and were associated with restricted mobility predominantly elbow, knee and foot joints on both sides and lumber spine were affected. Skin rashes were maculopapular, reddish- purple involving extensor surface of lower legs and feet. One week later child developed acute, severe, colicky and intermittent periumbilical abdominal pain. On physical examination vitals including blood pressure (based on childhood normative data) were normal. Tenderness and swelling were present on the affected joints including lumber spine. Rashes were palpable over lower extremities. On abdominal examination abdominal tenderness was present in periumbilical region but no organomegaly was there. However other systems were normal. There were no urinary signs or symptoms. Genitals were also normal.
Investigations
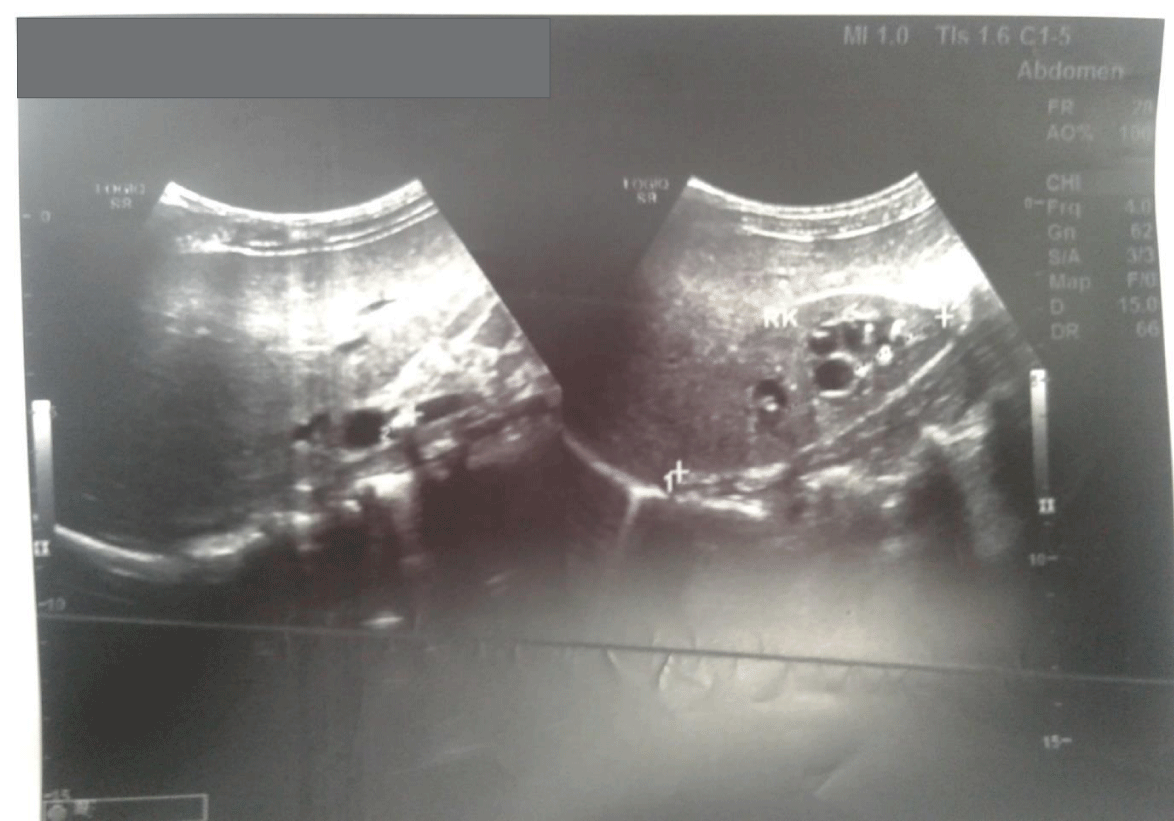
CBC revealed hemoglobin of 10.3 gm/dl and microcytic hypochromic picture. Total leukocyte count including platelets, were normal. ESR and CRP were raised. Stool blood was negative for occult blood. Renal function tests were normal with S. creatinine of 0.61mg/dl. Urine routine microscopic examination showed no hematuria or proteinuria. On ultrasonography of abdomen multiple echogenic foci with posterior acoustic shadow were seen in lower and upper pole calyx. A 6 mm. size calculus was noted in Pelvic Ureteric Junction (PUJ) of right kidney with renal parenchymal disease and with loss of cortico-medullary differentiation (Figure 2). S. total calcium and uric acid were within normal range. Skin biopsy report was consistent with IgA vasculitis with leukocytoclastic picture having 2+ granular deposits of IgA in wall dermal vessel activity. How-ever colonoscopy and colon biopsy could not be performed.
Treatment
The patient was diagnosed with HSP as per American College of Rheumatology and European League Against Rheumatism and Pediatric Rheumatology Society criteria. Patient was kept nil per orally and received intravenous fluids, analgesics and antacids for 24 hours. He was started with steroids in the form of oral prednisolone 20 mg per day. Resolution of symptoms occurred within 24 hours of starting steroids. CRP and ESR showed decreasing trend. Patient was discharged from the hospital and referred to pediatric surgery for further management of renal comorbidity where after intravenous pyelography, Retrograde Intrarenal Surgery (RIRS) with ureteroscopy was planned and successfully performed 6 weeks later, after discharge from pediatric department . Steroids were given for 2weeks and later tapered and stopped. Follow up visits at 2 weeks, 4 weeks and 12 weeks after treatment showed no recurrence of symptoms and urinalysis was normal.
!-- Main BodyText Start here -->Discussion
HSP is one of the most common vasculitic disorder of childhood with unknown etiology. Its incidence is about 1:10 000. It is characterized by the presence of nonthrombocytopenic palpable purpura, transient arthralgia or arthritis and abdominal pain, Gastrointestinal (GI) bleeding, and nephritis [4]. The most serious long-term complication from Henoch–Schönlein purpura is progressive renal failure, which occurs in 1–2% of patients. In 1837, Johann Schönlein described a syndrome of purpura associated with joint pain and urinary precipitates in children. Eduard Henoch, a student of Schönlein demonstrated the association of abdominal pain and renal involvement with this syndrome. Abdominal pain is a common complaint in children with HSP and frequently necessitates evaluation [5]. The pain is usually periumbilical, colicky in nature and non-specific. In most cases it responds to simple analgesia. The most common abdominal complication requiring surgical intervention in HSP is intussusception it occurs in about 5% of patients [6]. Unlike in idiopathic intussusception, the location is most often ileoileal, and more frequent in children >3 years of age. Other severe abdominal complications of HSP include intestinal ischaemia and perforation, and GI bleeding [7]. However, these are very rare. But nowhere in the literatures renal colic was described as the cause of abdominal pain or as complication of HSP [8]. In our case also we considered abdominal colic as ischemic bowel pain and not considered any other differential for abdominal pain as the clinical criteria were fulfilled as per the American College of Rheumatology (ACR) criteria. But luckily patient was diagnosed as having renal calculi with complication also as loss of corticomedullary differentiation hydronephrosis in kidney on ultrasonography. Even the incidence of renal calculi among children is 1/1000 to 1/7500 among hospital admissions in children [9], we didn’t consider abdominal colic as of renal origin. Although a case report describes a 75 years old male patient with HSP with pre-existing renal stones which posed diagnostic dilemma in colicky pain due to renal stones at the time of presentation with HSP [10]. But as in the current case dramatic resolution of symptoms with steroid therapy suggests, that symptomatic presentation of abdominal pain was more likely due to HSP rather than Calculi itself. So as a physician we should not always have the tubular vision for any case regarding diagnosis and management of the illness even if patient presents with classical symptoms of any common disease rather we should have open mind for possibilities of other comorbidities especially if patient behaves unusually during the course of illness or management.
Conclusion
We brought this report into light in which an adolescent male presented with HSP and renal calculi in right kidney, a rare comorbidity which is coincidental but due to presence of abdominal colic, hypertension, hematuria, proteinuria and deranged renal function in both, can cause suffering in patient as a result of delay in diagnosis and management of the disease and comorbidity irrespective of which one is performing the role of presenting disease.
- Stachy P (2016) Edwards Fels. In: Nelson Textbook of Pediatrics. First South Asia ed. Kliegman RM, Behrman RE, Geme JW, Stanton BF, Schor NF editors. Philadelphia, PA: Saunders Elsevier Vasculitis syndromes.
- Singh S (2013) In: Ghai essential Pediatrics. 8 ed. Paul VK, Bagga A editors. CBS Publishers, 2013Rheumatological disorders Bloch DA, Michel BA, Hunder GG.
- Henoch-Scholein purpura-Clinical practice guideline by Royal children”s hospital, Melbourne. Link: https://bit.ly/2RMbdWL
- Leavitt RY, Fauci AS, Bloch DA, Michel BA, Hunder GG, et al. (1990) The American College of Rheumatology 1990 Criteria for the Classification of Vasculitis. Patients and Methods. Arthritis Rheum 33:1101-1107. Link: https://bit.ly/2XOrVsg
- Choong CK, Beasley SW (1998) Review intra-abdominal manifestations of Henoch-Schönlein purpura. J Paediatr Child Health 34: 405-409
- Weiss P (2012) Pediatric vasculitis. Pediatr Clin North Am 59: 407-423. Link: https://bit.ly/3ap5xs9
- Saulsbury F (2007) Clinical update: Henoch-Schonlein purpura. Lancet 369: 976-978. Link: https://bit.ly/3cu4add
- Dalpiaz A, Schwamb R, Miao Y, Gonka J, Walzter W, et al. (2015) Urological manifestations of Henoch-Schönlein purpura: A Review. Curr Urol 8: 66-73. Link: https://bit.ly/3ajtC3H
- Gillespie RS, Stapleton FB (2004) Nephrolithiasis in children. Pediatr Rev 25: 131-139. Link: https://bit.ly/3cu3Efh
- Cheungpasitporn W, Jirajariyavej T, Howarth CB, Rosen RM (2011) Henoch Schonlein purpura in an older man presenting as rectal bleeding and IgA mesangioproliferative glomerulonephritis: A case report. J Med Case Rep 5: 364. Link: https://bit.ly/34RHl0d
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
