Open Journal of Trauma
Brodie’s abscess associated with soft tissue swelling in an athlete in Abidjan (Ivory Coast)
Kone Seydou Gnombena N’golo*, Kone Samba, Dogba Eric, Ouihahi Djekoury Yves Christian, Bana Abdoulaye and Agoh Serge
Cite this as
Gnombena N’golo KS, Samba K, Eric D, Yves Christian OD, Abdoulaye B, et al. (2020) Brodie’s abscess associated with soft tissue swelling in an athlete in Abidjan (Ivory Coast). Open J Trauma 4(1): 001-003. DOI: 10.17352/ojt.000023Introduction: As very few African publications are found in the literature concerning Brodie’s abscesses, we report a rare case of the association of a Brodie’s abscess with soft tissue swelling in a sportsman in Abidjan (Ivory Coast).
Report case: A 30-year-old patient presented knee pain associated with swelling of the distal third of the thigh as a result of a sports trauma. The diagnosis of a Brodie’s abscess was made. Surgical treatment combined with antibiotic therapy was performed. The evolution was favourable.
Conclusion: Brodie’s abscess is a subacute osteomyelitis that can pose a diagnostic problem with bone tumors. Magnetic Resonance Imaging has a place in the diagnosis. Patient management must be multidisciplinary.
Introduction
Brodie’s abscess is a subacute form of osteomyelitis, presenting as a collection of pus on the bone [1]. The onset is often insidious with clinical signs and deceptive imaging that may mimic a bone tumor [2]. Publications concerning Brodie’s abscess come mainly from developed countries. There are very few publications from Africa [1]. We report a rare case of the association of a Brodie’s abscess with a swelling of the soft tissues in a sportsman in Abidjan (Ivory Coast).
Report case
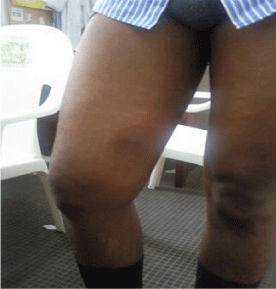
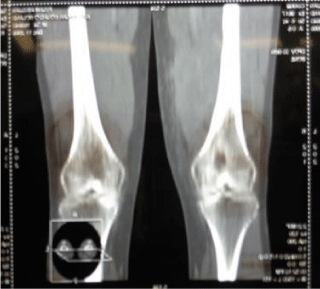
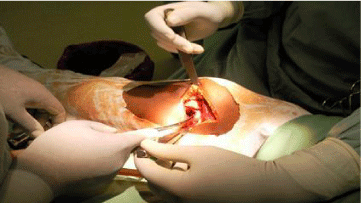
30-year-old sports patient with no particular history who consulted in November 2018 for the management of right knee pain associated with swelling of the distal third of the thigh. The patient had presented two months prior to a right knee trauma during a football match. He did not seek medical attention and began self-medication with analgesics and anti-inflammatory drugs. The symptomatology gradually worsened to the point of limping, leading the patient to consult. Clinical examination revealed an inflammatory swelling on the inner side of the distal third of the thigh with a painful limitation of the knee joint amplitudes (Figure 1). Elsewhere, the patient was apyretic with a good general condition and the rest of the examination was unremarkable. The biological assessment showed a slight increase in SV and CRP without hyperleukocytosis. The standard radiographic workup, followed by CT scan, revealed a lacunar metaphyseal image of the distal femur delimited by a thick, sharply contoured osteocondensation (Figures 2,3). This radiological aspect led us to make the diagnosis of either a bone tumour or a Brodie’s abscess. Surgery was therefore performed. The approach was centered on the swelling on the inner side of the distal third of the thigh. We found approximately 300cc of pus extending from the soft tissue to the bone gap. After removal of the pus and washing with saline, we proceeded to curettage and excision of the osteitis (Figure 4). Samples were taken for bacteriological and pathological examination. Suturing of the incision was done on a suction drain.
Post-operative antibiotic therapy was given with ceftriaxone 2g intravenously per day. In view of the result of the bacteriological examination which isolated a staphylococcus aureus sensitive to this antibiotic, we continued the antibiotic therapy until D 10. The anatomopathological examination ruled out any tumour process. The postoperative evolution was satisfactory with a drying of the suppuration. At the patient’s discharge, the antibiotic therapy was relayed per os with cefixime. Healing was achieved and the patient was able to resume almost all his activities after 60days.
Discussion
This observation was of a young adult athlete with a Brodie’s abscess associated with soft tissue swelling, a condition described as rare [3]. In this case, the falsely incriminated trauma led to delayed diagnosis. The radiological diagnosis of the distal metaphyseal osteolytic lesion of the femur was made in our context with standard radiography and CT scan. We were unable to perform magnetic resonance imaging (MRI) because this examination was expensive for our patient. MRI is the diagnostic test of choice in this case, highlighting the abscess as a circumscribed image appearing as a hyposignal image in T1 and a hypersignal image in T2 [4]. Brodie’s abscess often poses a diagnostic problem because the clinical and radiological signs may mimic a bone tumour or other bone pathology (ostoid osteoma, osteoblastoma, eosinophilic granuloma, tuberculosis, chondrosarcoma, etc.) that warrants further investigation [2,5,6]. Management must be multidisciplinary, involving the surgeon, radiologist, infectiologist and pathologist [2]. The treatment, as was the case in our patient, is surgical (drainage of pus and bone excision) combined with antibiotic therapy [1]. Staphylococcus aureus was isolated from our patient. This germ is most often found in the literature [1]. The low number of African publications on the subject should not lead us to underestimate the prevalence of this form of osteomyelitis [7] among the large number of chronic osteomyelitis in sub-Saharan Africa [8].
Conclusion
Brodie’s abscess, which is subacute osteomyelitis, can be a diagnostic problem with bone tumours. The evolution is favourable under surgical treatment combined with antibiotic therapy.
- Van der Naald N, Smeeing DPJ, Houwert RM, Hietbrink F, Govaert GAM, et al. (2019) Brodie’s Abscess: A Systematic Review of Reported Cases. J Bone Jt Infect 4: 33‑39. Link: http://bit.ly/39Nnj8B
- Gomez-Brouchet A (2008) Role of the pathologist in the management and diagnosis of a bone infection. Médecine Nucl 32: 138‑141.
- Gabbott B, Faria G, Lawson G (2018) A Brodie’s abscess with soft tissue collection—complicating an already difficult diagnosis. Journal of Surgical Case Reports 2018: rjx263. Link: http://bit.ly/2SGqwkH
- Dutronc H, Bocquentin F, Dupon M (2004) Contribution of imaging to the diagnosis of osteoarticular infection. Médecine Mal Infect 34: 257‑263.
- Schlur C, Bachy M, Wajfisz A, Pointe HD le, Josset P, et al. (2013) Osteoid osteoma mimicking Brodie’s abscess in a 13-year-old girl. Pediatr Int 55: e29‑31. Link: http://bit.ly/2V6nIie
- Chang WF, Hsu YC, Wu YD, Kuo CL, Huang GS (2016) Localized Langerhans cell histiocytosis masquerading as Brodie’s abscess in a 2-year-old child: a case report. EXCLI J. 15: 33‑37. Link: http://bit.ly/2SUZepG
- Manandhar RR, Lakhey S, Panthi S (2017) Arthroscopically assisted evacuation of brodie’s abscess of distal femur. Cureus 9: e959. Link: http://bit.ly/2V4U2SQ
- Nacoulma SI, Ouedraogo DD, Nacoulma EWC, Korsaga A, Drabo JY (2007) Chronic osteomyelitis at the Ouagadougou University Hospital (Burkina Faso). Retrospective study of 102 cases (1996-2000). Bull Soc Pathol Exot 100: 264-268. Link: http://bit.ly/2vIIA4y
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
