Open Journal of Trauma
Intrapancreatic Lesion of Biliary Duct Following a Blunt Trauma: A Rare Entity Difficult to Identify with Conservative Management
M Jiménez-Fuertes1*, J Ruiz-Tovar1, M. Durán-Poveda1 and D García-Olmo2
2Cirugía General y Digestiva. Hospital Fundación Jiménez-Díaz. Madrid, Spain
Cite this as
Jiménez-Fuertes M, Ruiz-Tovar J, Durán-Poveda M, García-Olmo D (2017) Intrapancreatic Lesion of Biliary Duct Following a Blunt Trauma: A Rare Entity Difficult to Identify with Conservative Management. Open J Trauma 1(1): 003-006. DOI: 10.17352/ojt.000002Lesions of the biliary duct following a blunt abdominal trauma occurs infrequently, and even more so when it occurs in the intrapancreatic biliary duct. With the increase of conservative treatment in blunt abdominal trauma, the diagnosis of this entity can be difficult and delayed.
We present the case of a lesion of the intrapancreatic biliary duct following a blunt trauma.
A 51-year-old male patient was treated following a bicycle accident. Initial CT scan showed multiple bilateral rib fractures and grade 2 liver injury in segment VII. On the basis of these findings and the stability of the patient, a conservative treatment was adopted. On the 9th day following admission he developed a progressive jaundice. This prompted a Doppler ultrasonography of the liver, showing no abnormalities in the pedicle or hepatic vessels, as well as an MR-cholangiography, which only revealed an increased amount of abdominal fluid without dilatation of the bile duct and without apparent injury of the duct. Upon the onset of fever and general worsening of the patient’s condition, an exploratory laparotomy was performed on the 16th day following admission, revealing plenty of intraperitoneal bile fluid, but a visual examination of the bile duct failed to determine the site of injury. An intraoperative ERCP was performed, revealing a lesion of the intrapancreatic bile duct, after which a biliary stent was inserted. In the early postoperative period the patient developed a leak through the external biliary drains placed during laparotomy. A new ERCP was therefore performed, together with the insertion of a coated metal prosthesis, after which the patient progressed satisfactorily.
Damage to the intrapancreatic bile duct by blunt abdominal trauma is a rare entity, difficult to diagnose, especially with the increase of conservative treatment of associated injury such as liver damage. MR cholangiography and ERCP play a fundamental role in the diagnosis and actual endoscopic treatment of these injuries (with or without a surgical cavity wash) and, when feasible, this constitutes the best option for treatment.
Introduction
Lesions of the biliary duct following a blunt abdominal trauma occurs infrequently, and even more so when it occurs in the intrapancreatic biliary duct. Normally it is associated with injuries in adjacent organs, most notably the liver, pancreas, duodenum and main arteries. With the increase of conservative treatment for lesions resulting from a blunt abdominal trauma, like in hepatic trauma, diagnosis can be difficult, and - in the majority of cases – it can be delayed.
We present the case of a lesion of the intrapancreatic biliary duct following a blunt trauma.
Clinical Case
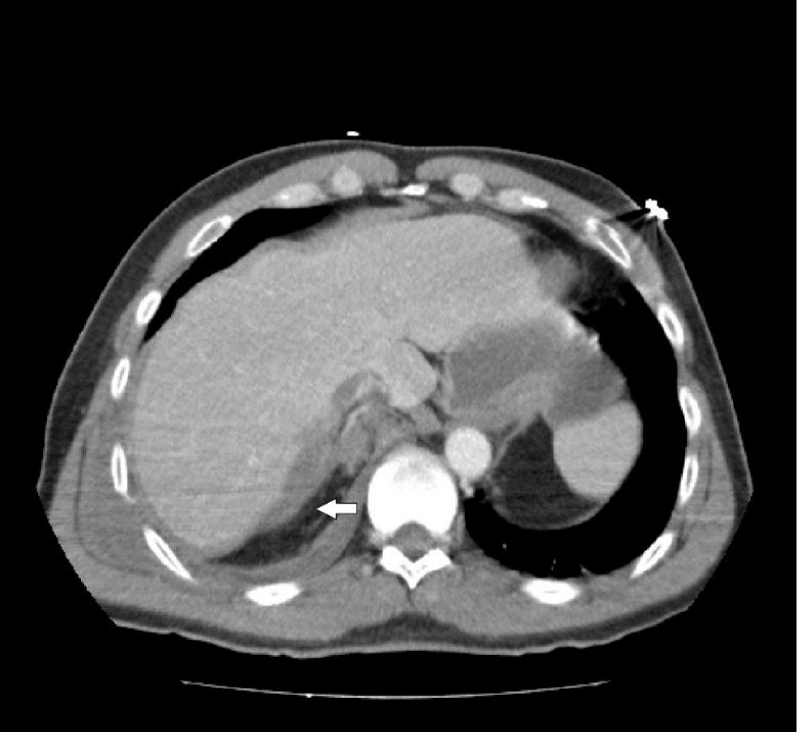
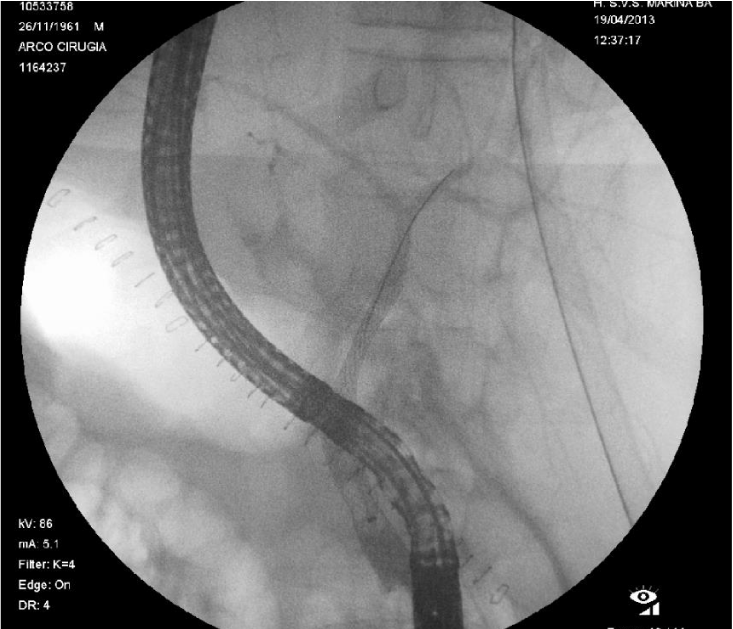
A 51-year-old male patient was treated in the emergency room following a bicycle accident. The initial treatment was administered according to the ATLS protocols. Since the patient exhibited normal haemodynamics, a thoracoabdominal-pelvic CT was performed, revealing multiple bilateral rib fractures and grade 2 liver injury in segment VII, along with a minimal amount of free abdominal fluid (Figure 1). On the basis of these findings and the stability of the patient, a conservative treatment was adopted, together with observation in the Intensive Care Unit. The patient progressed satisfactorily, displaying, however, gradually elevated levels of bilirubin up to a maximum of 8.8 mg/dl on the 9th day following admission as well as progressive jaundicing of the skin. This prompted a Doppler ultrasonography of the liver, showing no abnormalities in the pedicle or suprahepatic vessels, as well as an MR-cholangiography, which only revealed an increased amount of abdominal fluid without dilatation of the bile duct and without apparent injury of the duct. Upon the onset of fever and general worsening of the patient’s condition, an exploratory laparotomy was performed on the 16th day following admission, revealing plenty of intraperitoneal bile fluid, but a visual examination of the bile duct failed to determine the site of injury. An intraoperative ERCP was performed, revealing a lesion of the intrapancreatic bile duct, after which a plastic biliary stent was inserted (QuickPlace V® 10 Fr, Olympus) (Figure 2). In the early postoperative period the patient developed a leak through the external biliary drains placed during laparotomy. A new ERCP was therefore performed, together with the insertion of a coated metal prosthesis (WallflexTM biliary fully covered stent, 10 mm diameter, 60 mm length, Boston Scientific) (Figure 3), after which the patient progressed satisfactorily. The stent was removed 6 months after, without problems. The patient remains asymptomatic 2 years later.
Discussion
In the last two decades, the development of techniques such as CT imaging for patients that are haemodynamically stable following a blunt abdominal trauma have aided the precise diagnosis of certain lesions, such as hepatic lesions, thereby increasing the number of cases treated conservatively.
But a side effect of this conservative approach is an increase in the occurrence of associated lesions that are diagnosed late (as a result of their being initially radiologically undetected) after complications related to them emerge - as occurs in some situations related to biliary tract injuries. The incidence of bile duct injury following a blunt trauma is less than 0.5% for patients undergoing laparotomy for blunt abdominal trauma, and this incidence is much lower when the lesion is located in the intrapancreatic common bile duct [1,2]. Unlike bile duct injuries after laparoscopic cholecystectomy, most lesions of the extrahepatic bile duct related to blunt trauma are distal to the confluence (type I lesions as classified by Bismuth) [3]. The incidence of extrahepatic biliary duct injury following a blunt trauma has been reported to be as low as 1 in 10.500 trauma cases [4], and complete common bile duct transection is particularly rare too [5]. There are only 46 cases of isolated extrahepatic bile duct rupture due to blunt abdominal trauma (clearly and well-documented cases without other significant associated intra-abdominal injuries in English language, in PubMed) [6-18].
The mechanism of injury is unclear, although compression-stretching forces acting on the external biliary duct have been suggested, which, following a direct impact on the abdominal wall, raise the liver in a cephalic direction, thereby shearing the bile duct in the pancreas as a consequence of the relatively fixed position of the duodenum and pancreas. One would expect this mechanism to produce the concomitant injury of the portal vein and the hepatic artery, but we pose that their absence in our particular case is a result of their greater elasticity and length as compared to the bile duct [19].
The clinical pattern of progression is characteristic: after the initial trauma accompanied by symptoms related to associated injuries (if they exist), the patient undergoes a symptomless period as in the case presented here, that can vary from several hours to several months [20], followed by a progressive elevation of bilirubin levels and symptoms associated with the intraperitoneal leakage of biliary fluids (pain, fever, etc.).
In the majority of cases, this kind of intrapancreatic lesion cannot be easily identified during an initial laparotomy performed as a result of trauma, nor by imaging, as in our case, when the lesion could not be identified on the initial CT scan. As in most cases reported in the literature [21], the lesion could not be suspected and identified until the gradual elevation of bilirubin levels, and jaundice became apparent, prompting an MR cholangiography that further revealed biliary ascites. In these cases, ERCP plays a diagnostic as well as a therapeutic double role, since the insertion of stents for this kind of lesion has proved to be an effective treatment [22]. Together with ERCP, one can also perform, as in the present case, laparoscopic surgery or a laparotomic cavity wash to remove the existing biliary ascites, or a percutaneous drainage depending on the extent of the biliary ascites. At any rate, when confronted with free biliary fluid in the abdominal cavity without evidence of injury, it is necessary to perform an intraoperative cholangiography, whether transcystic or via ERCP, to locate the existing injury or injuries.
Treatment must be determined by the type of injury and the haemodynamic condition of the patient. Feliciano described 5 factors determining whether to perform surgical treatment: the haemodynamic condition of the patient, the presence of injury associated with the right upper quadrant, the location and extent of the injury, the small duct size, and the blood flow to the ducts [23].
Given that these kinds of injury cannot be identified at an early stage and given the small diameter of the biliary duct that one encounters in these cases – as compared to the size of normal biliary ducts – a good alternative is the ERCP-assisted insertion of a stent, together with a laparoscopic or laparotomic cavity wash, following a delayed diagnosis as in the present case [24]. The stent isolates the injured area from passing biliary fluid, which facilitates healing; moreover, this prevents cicatricial stenosis at the injury site [25].
If this option is not feasible, the surgical alternatives will depend, as mentioned, on the haemodynamic condition of the patient and on the associated injuries. If the patient is haemodynamically unstable, the objective would then be to control haemorrhaging and infection, which can be simply done by placing external drainage with or without attempts to perform a primary repair if the injury affects less than 50% of the circumference, or by performing T-tube drainage. For stable patients, options include end-to-end anastomosis (with high rate of stenosis), choledochoduodenostomy and Roux-Y choledochojejunostomy – this last being the preferred treatment in the literature [26], and the Whipple procedure, which is reserved for associated complex pancreatoduodenal injury. Surgical repair, however, is associated with a high morbidity. Surgical complications include anastomotic leakage and infection, and in the long run, the appearance of stenosis cholangitis, biliary cirrhosis and portal hypertension. Morbidity is also related to the presence of other lesions and to the delay in diagnosis.
In conclusion, damage to the intrapancreatic bile duct by blunt abdominal trauma is a rare entity, difficult to diagnose, especially with the increase of conservative treatment of associated injury such as liver damage. MR cholangiography and ERCP play a fundamental role in the diagnosis and actual endoscopic treatment of these injuries (with or without a surgical cavity wash) and, when feasible, this constitutes the best option for treatment.
- Kaul S, Homnick A, Livingston D (2002) Intrapancreatic bile duct injury: case report. J Trauma 52: 786-788. Link: https://goo.gl/b3G4E0
- D'Amata G, Rahili A, Habre J, Karimdjee B, Sanchez Bueno F, et al. (2006) Traumatic avulsion of the intrapancreatic common bile duct: case report. G Chir 27: 27-30. Link: https://goo.gl/YZM39n
- Thomson BN, Nardino B, Gumm K, Robertson AJ, Knowles BP, et al. (2012) Management of blunt and penetrating biliary tract trauma . J Trauma Acute Care Surg 72: 1620-1625. Link: https://goo.gl/8tf1Bv
- D.L. Dawson, K.H. Johansen, G.J. Jurkovich (1991) Injuries to the portal triad. Am J Surg 161: 545–551. Link: https://goo.gl/hvM1Ol
- Posner MC, Moore EE (1985) Extrahepatic biliary tract injury: operative management plan. J Trauma 25: 833–837. Link: https://goo.gl/ocBzya
- Balzarotti R, Cimbanassi S, Chiara O, Zabbialini G, Smadja C (2012) Isolated extrahepatic bile duct rupture: a rare consequence of blunt abdominal trauma. Case report and review of the literature. World J Emerg Surg 7: 16. Link: https://goo.gl/7CbNw4
- Mandal N, Mandal R, Ranjan R (2013) Complete transection of common bile duct after blunt trauma abdomen--a case report. J Indian Med Assoc 111: 560-561. Link: https://goo.gl/QW6c9u
- Fiocca F, Salvatori FM, Fanelli F, Bruni A, Ceci V, Corona M, et al. (2011) Complete transection of the main bile duct: minimally invasive treatment with an endoscopic-radiologic rendezvous. Gastrointest Endosc 74: 1393-1398. Link: https://goo.gl/gWNb2F
- de Mestral C, Razek T, Khwaja K, Fata P (2008) Blunt Left Extrahepatic Bile Duct Injury: Case Report and Literature Review. Eur J Trauma Emerg Surg 34: 595-600. Link: https://goo.gl/UyoVvg
- Melton SM, McGwin G Jr, Cross JM, Davidson J, Waller H, et al. (2003) Common bile duct transection in blunt abdominal trauma: case report emphasizing mechanism of injury and therapeutic management. J Trauma 54: 781-785. Link: https://goo.gl/iGlj8n
- Sharpe RP, Nance ML, Stafford PW (2002) Nonoperative management of blunt extrahepatic biliary duct transection in the pediatric patient: case report and review of the literature. J Pediatr Surg 37: 1612-1616. Link: https://goo.gl/jGlLnV
- Miyakawa S, Mizuno K, Horiguchi A, Hayakawa M, Ishihara S, Miura K (1996) Complete transection of the left hepatic duct due to blunt abdominal trauma. Hepatogastroenterology 43: 1395-1398. Link: https://goo.gl/2z5ZHj
- Sofianos C, Naidu M (1994) Complete transection of the common bile duct following blunt abdominal trauma. A case report. S Afr J Surg 32: 44-45. Link: https://goo.gl/xU5gl2
- Chung YC, Lee PH, Huang MT, Chang CN (1993) Complete transection of common bile duct due to blunt abdominal trauma: a case report and literature review. J Formos Med Assoc 92: 78-81. Link: https://goo.gl/rrYTMu
- Kernohan RM, Humphreys WG (1985) Closed abdominal trauma in a child causing avulsion of the common bile duct and gastric stasis. Injury 16: 235-237. Link: https://goo.gl/PlnVj5
- Rydell WB Jr (1970) Complete transection of the common bile duct due to blunt abdominal trauma. Arch Surg 100: 724-728. Link: https://goo.gl/pqnfuD
- Moffat RC, Lucas RJ (1969) Transection of the common bile duct as an isolated injury following blunt trauma. Can J Surg 12: 334-335. Link: https://goo.gl/n6orYW
- Dobbie RP Jr, Stormo AC (1968) Complete transection of the common bile duct, the sole sequela of blunt abdominal trauma. J Trauma 8: 9-18. Link: https://goo.gl/A1qgug
- Ito T , Yamamoto M , Machida H , Hashiguchi Y , Yatsuda N , et al. (1993) Complete avulsion of the papilla of Vater and gastroduodenal artery due to blunt abdominal trauma: report of a case. Surg Today 23: 172-175. Link: https://goo.gl/KhDyuU
- Balzarotti R, Cimbanassi S, Chiara O, Zabbialini G, Smadja C (2012) Isolated extrahepatic bile duct rupture: a rare consequence of blunt abdominal trauma.Case report and review of the literature. World J Emerg Surg 7: 16. Link: https://goo.gl/OZFo4L
- Khodadadi J, Mihich M, Finally R, Milleritzky M (1983) Avulsion of common bile duct after blunt abdominal injury: a review of the literature. Injury 14: 447-450. Link: https://goo.gl/8icMHF
- Michelassi F , Ranson JH (1985) Bile duct disruption by blunt trauma. J Trauma 25: 454-457. Link: https://goo.gl/UNrHZm
- Wong VW, Gee A, Hansen P, Michaels A (2012) Isolated avulsion of the common hepatic duct from blunt abdominal trauma Case Rep Surg 2012: 254563. Link: https://goo.gl/1X1hnJ
- Feliciano DV (1994) Biliary injuries as a result of blunt and penetrating trauma. Surg Clin North Am 74: 897-907. Link: https://goo.gl/2MMHzS
- Goldman R , Zilkoski M , Mullins R , Mayberry J , Deveney C , et al. (2003) Delayed celiotomy for the treatment of bile leak, compartment syndrome, and other hazards of nonoperative management of blunt liver injury. Am J Surg 185: 492-497. Link: https://goo.gl/wM4sRS
- Sharma BC, Mishra SR, Kumar R, Sarin SK (2009) Endoscopic management of bile leaks after blunt abdominal trauma . J Gastroenterol Hepatol 24: 757-761. Link: https://goo.gl/fiKeoz
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
