Open Journal of Pediatrics and Child Health
Perrotta Autism Spectrum Disorders Questionnaire for infants and young adolescents (PASD-Qy)
Giulio Perrotta*
Cite this as
Perrotta G (2022) Perrotta Autism Spectrum Disorders Questionnaire for infants and young adolescents (PASD-Qy). Open J Pediatr Child Health 7(1): 031-033. DOI: 10.17352/ojpch.000043Copyright
© 2022 Perrotta G. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Building on the concept of “Autism Spectrum Disorder”, as framed in the DSM-V, and taking up studies on the new etiological theory (PETA) focusing on the developmental model of the neurobiological matrix (PEMA) and related questionnaire (PTAS-Qa), in this research a new questionnaire is proposed that can focus on the presence or absence of 4 functional areas (interactional and movement, language, and communication, ideational and social, emotional and behavioral) and 25 type-deficit traits, grading the impairment according to a precise 5-level severity scale (PASSy). The new questionnaire (Perrotta Autism Spectrum Disorders Questionnaire for infants and young adolescents, PASD-Qy), is composed of 25 items, on a binary S/N scale and based on a total score of 10/10, for a population between 18 months and < 16 years, thus offering a structured view of the individual’s cognitive organization, avoiding diagnostic fragmentations that might be inconsistent with the nosographic framework. By exemplifying the category, it is then possible to more easily frame the patient, who would thus be analyzed from a strictly functional point of view, also facilitating the preparation of therapeutic interventions, according to models already known in the literature (e.g., ABA), exactly as for the questionnaire dedicated to late adolescents and adults.
Introduction
General profiles and definitions
The autism spectrum has a high degree of heterogeneity that makes it difficult to understand, especially before 24 months of age, how to recognize whether a child has autism. The individual with autism can have features and symptoms ranging from very mild to very severe and marked and can occur in all ethnic, socioeconomic, and age groups. Males also are four times more likely to have autism than females. Some children with autism then appear homotypic, before the age of one or two, and then suddenly “regress” by going on to lose the language or social skills they had previously acquired. The heterogeneity of the symptoms and characteristics of the autism spectrum determines the fact that the signs and signals of autism that allow for early diagnosis are also variable among themselves, heterogeneous, and difficult to detect and interpret correctly. These aspects place at the center of the process toward early diagnosis the role of the parent in recognizing the signs of autism that will need to be reported to the clinical team, starting with the pediatrician and ending with the specialized services that will set up and implement individualized rehabilitation treatment. As a parent, you are in the best position to detect early signs and signals of autism. If autism is recognized during childhood, treatment can take full advantage of the remarkable plasticity of a child’s brain and the effectiveness of the latest and most up-to-date behavioral intervention techniques. Although an autism spectrum disorder is difficult to recognize and diagnose before 24 months of age, signs of autism often emerge between 12 and 18 months of age. Early signs of autism involve the absence of normal behaviors, not the presence of abnormal behaviors, and for this reason, they can be quite difficult to detect and interpret correctly; in some cases, early symptoms of autism can even be misinterpreted as signs of a “good child” or a child’s particularly quiet temperament, as the child may appear calm, independent, and undemanding. However, alarm bells can be detected early if one knows what to look for, and that is the main focus of this informative article. Typical signs detectable early (by age two) by the parent, in interaction with their child, include the following: do not smile at you when you smile at him (poor emotional reciprocity); does not look at you while you feed him (limited or absent eye contact); does not respond to his name or the sound of a familiar voice; does not imitate your movements and facial expressions; does not share or present reciprocity of interest and enjoyment; does not visually follow objects or your gesture when you point things out (lack of shared attention); does not greet or use other gestures to communicate; does not make noises or vocalizations to get your attention; does not seek cuddles or seek to be picked up. Clinical signs, on the other hand, typical during outpatient visits with the pediatrician, always under 24 months, and unless otherwise indicated, are the following: by 6 months, no big smiles or other positive emotional expressions of amusement; by 9 months, no sharing of sounds, smiles or other facial expressions; by 12 months, no gestures of social reciprocity such as pointing or showing; by 12 months, no vocalizing; by 12 months, lack of response to name (no turning to voice); by 14 months, the child does not point to distant objects; by 16 months, no “simple words” spoken; by 24 months, no meaningful two-word phrases that do not involve mere imitation or repetition. As children grow older, the signs of autism become more articulated and heterogeneous, and the criteria for recognizing autism revolve around impaired social skills, difficulty with nonverbal communication, rigidity of thought and behavior (which can cause major problem behaviors, and difficulty with language (in case it is present, even if in partial form). Concerning social and interaction skills the main signs of autism beyond the age of two years may be (and unless otherwise clinically indicated): difficulty in understanding feelings or talking about them; lack of participation in group play; difficulty in the ability to imitate the behavior of others; total or partial lack of attention when others talk to him; lack of sharing his interests and what arouses his attention with others; disinterest or unawareness of other people’s behavior; difficulty in the ability to establish contact with age peers in playing or making friends; refusal or disinterest in physical contact; lack of imaginative play (e.g. making a plane with a fork, using games to simulate a story). Concerning nonverbal communication, the main signs of autism may be a failure to understand the meaning and message of facial expressions, tone of voice, and gestures of others; poor use of gestures (e.g., pointing with hands); avoidance of eye contact or, in any case, poor and elusive eye contact in many cases; poor or incorrect emotional expressiveness through facial expressions. Such communication impairment and difficulty further impact difficulties in the area of social skills. With respect to rigidity of thought and behavior, the main signs of autism may be: showing great interest in certain unusual areas (e.g., numbers, symbols, train schedules or sports statistics); spending long periods watching moving objects focusing on a specific part of that object (e.g., fan, washing machine, ...); frequently repeating the same actions or movements; reacting unusually or excessively to images, smells, textures and sounds (e.g., “I’m not sure if I’m sensitive to the same thing. may be particularly sensitive to loud noises and cover his ears when he hears them); unresponsive to people entering/leaving the room, as well as to others’ efforts to get the child’s attention; abnormal postures, clumsiness or eccentric ways of moving (e.g., walking exclusively on tiptoes); following a rigid routine and needs to do things the same way all the time (e.g., insists on taking a specific route to school); difficulty adapting to changes in the program or environment (e.g., shows annoyance if the arrangement of furniture, his toys, or the organization of the day is changed); showing great interest in unusual or strange objects such as keys, light switches, or rubber bands with which he interacts all the time; obsessive alignment of things or arrangement in a certain precise order. Concerning language difficulties (in cases where language is present, even if impaired), the main signs of autism may be: using language incorrectly (grammatical errors, misspelled words); referring to himself in the third person (pronominal inversion or confusion in the use of pronouns); taking what is said literally (literal interpretation of language); speaking in an abnormal tone of voice or rhythm; repeating the same words or phrases with high frequency, often without communicative intent; responding to a question by repeating it, instead of answering it. However, in some special cases, such as in Asperger’s syndrome, language acquisition may be early and the child presents good vocabulary and sentence syntax while maintaining difficulties with prosody, intonation, and literal interpretation [1,2].
Perrotta Autism Spectrum Disorders questionnaire for infant and young adolescent adults (PASD-Qy)
Taking a cue from the questionnaire for late adolescents and adults [2] The present research work proposes to extend the analysis of autistic traits to populations under 16 years of age as well, but structuring the questionnaire based on functional areas (and not based on dysfunctional traits); in this way, adhering to the clinical approach that in childhood and youth the issue is not to identify dysfunctional traits but rather the areas of competence that by age should be met, it is possible to derive the PASD-Qy questionnaire, to be administered by the health professional, an individual between 18 months and < 16 years of age, slightly readjusting the severity scale, this time on a 10/10 basis (unlike that of adults which is 11/11). The following scale grading and questionnaire construction are to be considered working proposals, which are in the process of validation to search for the population sample for a clinical study.
The questionnaire (modeled based on the PICI) [3-8] is structured in two parts: the first part (Section A) is devoted to preliminary data about the patient; the second part (Section B), the other hand, is devoted to the actual questionnaire, and specifically, the questionnaire consists of 25 items (divided into nine subject areas related to the nine dysfunctional traits), on a binary yes/no scale. The sum of the relative scores, concerning yes answers only, determines the final score, and this also determines the severity of the autistic condition:
a) The minimum score is 0/10; the maximum score is 10/10, but the diagnosis of “Autism Spectrum Disorder” is determined only if all three of the following conditions will be met: The final score must be at least 4.1/10 or higher;
b) The following sub-items must have been answered positively: 1.5, 1.7, 1.12, 1.13, 1.17, 1.20, 1.24;
c) There must be no other diagnostic hypotheses that explain the symptoms differently.
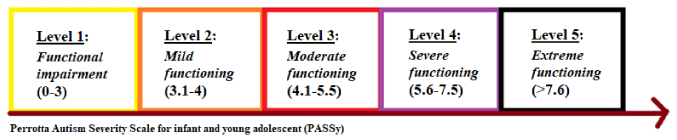
Below is the evaluation grid for the final diagnosis:
Conclusion
The proposed questionnaire (and its severity scale adapted to the target population), provides the therapist with an accurate snapshot of both the presence of certain autistic traits and the possible diagnosis of “Autism Spectrum Disorder” for infants and young adolescents, while also offering a structured view of the patient’s cognitive and psychological organization, avoiding diagnostic fragmentations that might not be consistent with the nosographic picture and therefore not perfectly framed. By exemplifying the category, it is, therefore, possible to more easily frame the patient, who would thus be analyzed from a strictly functional point of view, also facilitating the therapeutic interventions to be prepared, according to models already known in the literature (e.g. ABA).
- Perrotta G. Autism Spectrum Disorder: Definition, contexts, neural correlates and clinical strategies. J Neurol Neurother. 2019; 4(2):136. doi: 10.23880/NNOAJ-16000136.
- Perrotta G. New Evolutionary Model on “Autistic Spectrum Disorder” (PEMA), the severity scale (PASS) and the clinical questionnaire for the late teenage years and adults (PTAS-Qa). Open J Pediatr Child Health. 2022; 7(1). doi: 10.17352/ojpch.000041.
- Perrotta G. The structural and functional concepts of personality: The new Integrative Psychodynamic Model (IPM), the new Psychodiagnostic Investigation Model (PIM) and the two clinical interviews for the analysis of personality disorders (Perrotta Integrative Clinical Interview or PICI) for adults and teenagers (1TA version) and children (1C version), Psychiatry Peertechz, E-book. 2020. doi: 10.17352/ebook10118.
- Perrotta G. First revision of the Psychodiagnostic Investigation Model (PIM-1R) and elaboration proposal of a clinical interview for the analysis of personality disorders (Perrotta Integrative Clinical Interview or PICI-1) for adults, teenagers and children, Psychiatry Peertechz, E-book. 2020. doi: 10.17352/ebook10119.
- Perrotta G. Perrotta Integrative Clinical Interview (PICI-1): Psychodiagnostic evidence and clinical profiles in relation to the MMPI-II, Ann Psychiatry Treatm. 2020; 4(1): 062-069. doi: 10.17352/apt.000022.
- Perrotta G. Perrotta Integrative Clinical Interview (PICI) for adults and teenagers (1TA version) and children (1C version): new theoretical models and practical integrations between the clinical and psychodynamic approach. Ann Psychiatry Treatm. 2021; 5(1): 001-014. doi: 10.17352/ apt.000024.
- Perrotta G. Perrotta Integrative Clinical Interview (PICI-1): a new revision proposal for PICI-1TA. Two single cases. Glob J Medical Clin Case Rep. 2021; 8(1):041-049. doi: 10.17352/2455-5282-000125.
- Perrotta G. Perrotta Integrative Clinical Interviews (PICI-2): innovations to the first model, the study on the new modality of personological investigation, trait diagnosis and state diagnosis, and the analysis of functional and dysfunctional personality traits. An integrated study of the dynamic, behavioural, cognitive and constructivist models in psychopathological diagnosis. Ann Psychiatry Treatm. 2021; 5(1): 067-083. doi: 10.17352/apt.000033.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
