Open Journal of Pediatrics and Child Health
Incidence and type of electrolyte abnormalities Iranian children with acute gastroenteritis
Fateme Mosav1, Iran Malekzdeh2 and Mastaneh Moghtaderi3*
2Associated Professor of Pediatrics, Children’s Medical Center, Tehran University of Medical Science, Tehran, Iran
3Associated Professor of Pediatric nephrology, Department of pediatric nephrology, Chronic kidney disease Research Center, Children’s Medical Center, Tehran University of Medical Science, Tehran, Iran
Cite this as
Mosav F, Malekzdeh I, Moghtaderi M (2020) Incidence and type of electrolyte abnormalities Iranian children with acute gastroenteritis. Open J Pediatr Child Health 5(1): 011-015. DOI: 10.17352/ojpch.000024Background: Acute Gastroenteritis (AGE) is one of the most common pediatric disorders, causes significant morbidity and is associated with electrolyte imbalances, some of which can be too dangerous.
Materials and methods: A prospective cross-sectional study was performed on 473 children admitted to the Children’s Medical Center Hospital emergency room for gastroenteritis. These patients received various treatments for gastroenteritis, such as oral rehydration therapy, antiemetic drugs, probiotics and intravenous fluids. The serum electrolyte, urea and creatinine levels of all patients were checked regularly and recorded on the data forms.
Results: A total of 437 children participated in this study. Of these, 243 (51%) were men and 231 (49%) women. 4.4% of the patients had mild dehydration, 78.7% had moderate dehydration and 20.8% of the children had severe dehydration. The serum Na range was 116 to 156 mmol / L (mean value 136.61 ± 8.85). The serum potassium level was 3 to 6 mmol / L (mean 4.2 ± 0.64). According to this study, the prevalence of sodium disorders in the study group was 41.6% (4% of severe hyponatraemia with serum Na <120 meq / L, 23.6% with serum Na 120 meq / L at 135 meq / L and 14% hypernatremia with serum Na> 145 meq / L). In our study group there was 17.2% potassium disorder, 13% hypokalaemia (serum K <3.5 mmol / L) and hyperkalaemia 3.7% (serum K> 5.5 mmol / L).
Introduction
Diarrhea remains a major cause of child morbidity and mortality worldwide [1]. Diarrhea is a major cause of illness and death among children in developing countries, where around 1.3 billion episodes and 3.2 million deaths occur in children under 5 years of age. About 80% of deaths from diarrhea occur in the first two years of life [2]. Malnourished children are at increased risk of complications. In some countries, the rate of income increases due to gastroenteritis, malnutrition, comorbidity and electrolyte imbalances (especially hyponatremia and hypokalaemia). The length of hospital stay is also longer than that of her non-native colleagues. The costs for the gastroenteritis community are enormous, but are often underestimated. In addition, family costs, including lost work, are often not taken into account [3]. Worldwide, most cases of gastroenteritis are caused by viral infections, with rotaviruses being the most common. Viral infections damage the enterocytes of the small intestine and cause mild fever and watery diarrhea. Rotavirus infection is seasonal in temperate climates and peaks in late winter, but occurs throughout the year in the tropics. Rotavirus strains vary depending on the season and geographically within the countries [4]. Bacterial pathogens such as Campylobacter jejuni and Salmonella spp. penetrate the lining of the small and large intestine and cause inflammation. Children with bacterial gastroenteritis are more likely to have a high fever and may have blood and white blood cells in their stools. Bacterial pathogens sometimes spread systemically, especially in young children. Infection with Escherichia coli or Shigella dysenteriae, which produce Shiga toxin, can cause hemorrhagic colitis (with severe bloody diarrhea), which can be complicated by hemolytic uremic syndrome [5]. The clinical manifestations of acute diarrhea are related to the severity of the lack of water and the type of electrolyte imbalance. As a result, the clinical detection of water and electrolyte disorders, especially hyponatremic dehydration, becomes important due to their serious neurological consequences [6]. Because the osmolality and volume of extracellular fluid are determined by their sodium content, this ion plays a key role in the regulation of water and electrolytes. In this sense, the biochemical change in children suffering from dehydration can be hyponatremic, isonatremic or hypernatremic. Other observed biochemical changes are hypokalaemia and metabolic acidosis [7]. The clinical impression of the type of dehydration and electrolyte changes was fairly in agreement with the values of the serum electrolytes. Bloating and abdominal distention correlated positively with hyponatraemia and hypokalaemia. Routine monitoring of serum electrolytes is not required. However, it is important if an electrolyte imbalance is suspected for clinical reasons and if they do not respond satisfactorily with routine fluid and electrolyte therapy [8]. Disorders of sodium and potassium levels in diarrhea-related dehydration cases can be a medical emergency that requires quick and appropriate diagnosis and treatment [9].
Material and methods
This prospective cross-sectional study that was carried out on 73 children with gastroenteritis who were admitted to the emergency center of the children’s center of the medical center from July 2016 to June 2018. Acute diarrhea in this study was defined as unusually loose or watery bowel movements at least three or more times in a 24-hour period that lasted less than 14 days. All patients with acute watery diarrhea between the ages of 2 months and 14 years were examined by their pediatrician in their emergency room according to WHO criteria. The following signs were considered signs of severe dehydration: lethargy or loss of consciousness, sunken eyes, poor alcohol consumption or inability to drink, oliguria and reduced skin turgor. If at least two of these signs were present, this was referred to as severe dehydration. The story was made by highlighting whether the participants had taken oral rehydration salts with salts (ORS) or not. Blood samples were taken before each IV therapy. The levels of urea, creatinine, sodium, potassium and chloride as well as blood gases were checked with the ISE method (Prolyte machine). Age, urea, creatinine, electrolyte levels and results were recorded on an SPSS form and an information sheet (version 20) by a pediatrician who conducted the study. Potassium levels below 3.6 mmol/l and above 5.5 mmol/l were classified as hypokalaemia and hyperkalaemia, respectively. Sodium levels below 130 mmol/l and above 150 mmol/l were assumed to be hyponatremia and hypernatremia, respectively. Chloride levels below 98 mmol/l and above 108 mmol/l were classified as hypochloremia and hyperchloremia, respectively. Exclusion criteria include a history of diabetes insipidus, pituitary or hypothalamic disorders, acute or chronic lung diseases, and a history of kidney failure. Patients with bloody stools and patients who received intravenous fluids within 6 hours of the presentation or blood draw were also excluded from the study. SPSS (version 20) was used to analyze the data collected. The value of p <0.05 was considered to be statistically significant. The ethical approval was obtained from the ethics committee of the Medical University of Tehran University (Batch number: IR.TUMS.MEDICINE.REC.1397.903).
Results
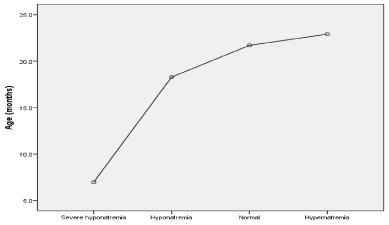
A total of 437 children met the inclusion criteria of the 510 children with diarrhea during the study period. Of these, 243 (51%) were men and 231 (49%) women. 4.4% of the patients had mild dehydration and 78.7% had moderate dehydration. 20.8% of the children suffered from severe dehydration. The youngest patient was 61 days old and the oldest was 10 years old. The mean age of the study population was 20.5 ± 25-8 months and a median of 3.6 months. The range of serum Na was 116-156 mmol / l (mean 136.61 ± 8.85). The serum potassium levels were 3 to 6 mmol / l (mean value 4.2 ± 0.64). The sexual prevalence of electrolyte imbalance in dehydrated patients is shown in Table 1. Analysis of the statistical data showed that only the Na level showed significant differences between boys and girls. In addition, according to the ANOVA analysis, there was a significant difference in serum Na and potassium levels compared to the severity of dehydration. [Na: F (2.425) = 9.596, p-value <0.001 and K: F (2.424) = 11.211, p-value <0.001]. The post-hoc test in Turkey showed that with severe dehydration, the Na and K levels were significantly more susceptible than in moderately dehydrated patients, as shown in Table 2. According to this study, the prevalence of sodium changes in the study group was 41.6% (4% of severe hyponatremia with serum Na <120 meq / l and 23.6% with serum Na 120 meq / l at 135 meq / l and hypernatremia at 14% with serum Na> 145 meq / l). In our study group there was a variation of 17.2% potassium, 13% hypokalaemia (serum K <3.5 mmol / l) and 3.7% hyperkalaemia (serum K> 5.5)). The relationship between potassium changes and patient age is shown in Figure 1. The ANOVA analysis showed that the average age is lower in hyperkalemic patients than in other patients. There is no significant difference between the other groups and reflects the small sample size. Table 3 shows the average age of the children affected. ANOVA analysis of various sodium levels has shown that there is a lower average age in hyponatremic patients, but in reality, there is no significant difference in all types of hyponatremia and may only reflect the small size of the sample population (Figure 2). Table 4 shows the average age in each patient group. Regarding sexual relationship to electrolyte abnormalities, analysis of the Ki score showed no significant relationship between sexual and potassium disorders (p-value <0.520), as shown in Table 5. In contrast in sodium changes there is a significant difference between gender and serum sodium. (P value <0.001) as shown in Table 6. Regarding the type of dehydration and the electrolyte content, there is a significant relationship between gender and sodium or potassium level (p-value <0.001) according to the Ki-square test, as shown in Tables 7,8.
Discussion
Disorder of sodium in dehydration associated with diarrhea can be a medical emergency that requires quick and appropriate diagnosis and treatment [9]. Different studies have shown a different prevalence of hyponatremia and hypernatremia in children with dehydration. A study by Samadi et al. including the children admitted for diarrhea, it was found that hyponatraemia and hypernatraemia were present in 20.8% and 6.4% of cases, respectively [10]. The study by Shah et al. showed that 56% of the cases with diarrhea and dehydration had hyponatremia, whereas hypernatremia only occurred in 10% of the cases [11]. So, his result was similar to our study. Many studies have been conducted in the past to determine the prevalence of various electrolyte disorders in children with gastroenteritis. These studies show that sodium disorders are more common in children with severe dehydration. Studies in South Asia show that hyponatremia is more common in pediatric age groups than hypernatremia. This study shows that hypernatremia is more common than hyponatremia in children with severe dehydration [12]. In particular, 89.2% of the population examined showed at least one or more forms of electrolyte imbalance [13]. Matthias Mariere Okposio and others have found electrolyte imbalance in more than three quarters of the affected children [14]. In the Ritika study, isonatremia was the most common dehydration (71.5%), followed by hyponatremic dehydration (22%) and hypernatremic dehydration (6.5%). 170 children (85%) had normokalaemia and 30 cases (15%) had hypokalaemia and none of the cases had hyperkalaemia. Six cases of hyponatraemia were associated with hypokalaemia. Of the 21 children who received appropriate ORS rehydration therapy before admission, only 5 had hyponatremia and none of them had hypernatremia. Therefore, the concentration of ORS made at home has played an important role in the electrolyte imbalances that occur with gastroenteritis. Using diluted ORS often leads to hyponatremia [2]. ORT seems to be the optimal way of rehydration for most children [14]. Dehydration and electrolyte imbalance are common complications of acute diarrhea in children [15]. In fact, children have significant physiological differences compared to adults due to their entire body surface area, immature kidney structures and endocrine systems, as well as a higher metabolic rate. Each of these factors causes them to develop fluctuations in the water and electrolyte balance [16].
Conclusion
This study, like others before, found electrolyte imbalance in more than half of the gastroenteritis children. Hyponatremic dehydration was the most common type of dehydration observed in our patients (27.5%). This has also been observed in other studies. Hyponatremic dehydration is most common in older infants and children with gastrointestinal infections [17, 18]. These children are often treated with low-sodium liquids such as water, fruit juices, ginger ale, soda or tea. In addition, the antidiuretic hormone that is released in most affected children, increases thirst and more water consumption. Most of it is also absorbed in the kidneys, which dilutes the content of intravascular solutes [19]. In summary, it can be said that electrolyte disturbances are very common in children with acute diarrhea. The degree of dehydration and the age of less than 12 months seem to be good prognostic factors for electrolyte imbalance. Early diagnosis and treatment are very important to prevent complications.
What we already know
Severe gastroenteritis can cause various electrolyte disorders, which have been reported differently in previous studies.
What this study adds
The most common electrolyte disorder in gastroenteritis is hyponatremia.
- Chola L, Michalow J, Tugendhaft A, Hofman K (2015) Reducing diarrhoea deaths in South Africa: costs and effects of scaling up essential interventions to prevent and treat diarrhoea in under-five children. BMC Public Health 15: 394. Link: https://bit.ly/2TMiXcp
- Dastidar RG, Konar N (2017) A Study of Electrolyte Disturbances in a Child Presenting with Acute Gastroenteritis, with Special Emphasis on Hyponatremic Dehydration-A Hospital based Cross-Sectional Study. Pediatr Ther 7: 2. Link: https://bit.ly/3c7yFF7
- Elliott EJ (2007) Acute gastroenteritis in children. BMJ 334: 35-40. Link: https://bit.ly/2TOgVIB
- Kirkwood CD, Bogdanovic-Sakran N, Cannan D, Bishop RF, Barnes GL (2006) National rotavirus surveillance program annual report 2004-5. Commun Dis Intell 30: 133-136. Link: https://bit.ly/2Xag72Y
- Elliott E, Robins-Browne R (2005) Hemolytic uremic syndrome. In: Moyer VA, ed. Problems in child and adolescent medicine. USA: Elsevier 35: 310-330.
- Begum JA, Hoque MM, Hussain M (2010) Impact of electrolyte disturbances in outcome of acute diarrhoea in children. DS (Child) Health J 26: 36-40.
- Canavan A, Arant BS (2009) Diagnosis and management of dehydration in children. Am Fam Physician 80: 692-696. Link: https://bit.ly/2X7rJUk
- Hartling L, Bellemare S, Wiebe N, Russell K, Klassen TP, et al. (2006) Oral versus intravenous rehydration for treating dehydration due to gastroenteritis in children. Cochrane Database Syst Rev 2006: CD004390. Link: https://bit.ly/3c7XgcP
- Petzold A (2015) Disorders of plasma sodium. N Engl J Med 372: 1267.Link: https://bit.ly/3gxkT28
- Samadi AR, Wahed MA, Islam MR, Ahmed SM (1983) Consequences of hyponatraemia and hypernatraemia in children with acute diarrhoea in Bangladesh. Br Med J (Clin Res Ed) 286: 671-673. Link: https://bit.ly/3gsYKBT
- Shah GS, Das BK, Kumar S, Singh MK, Bhandari GP (2007) Acid base and electrolyte disturbance in diarrhoea. Kathmandu Univ Med J (KUMJ) 5: 60-62. Link: https://bit.ly/3epyfLU
- Ahmad MS, Wahid A, Ahmad M, Mahboob N, Mehmood R (2016) Prevalence of Electrolyte Disorders Among Cases of Diarrhea with Severe Dehydration and Correlation of Electrolyte Levels with Age of the Patients. J Coll Physicians Surg Pak 26: 394-398. Link: https://bit.ly/3daL0tB
- Okposio MM, Onyiriuka AN, Abhulimhen-Iyoha BI (2015) Point-of-Admission Serum Electrolyte Profile of Children less than Five Years Old with Dehydration due to Acute Diarrhoea. Trop Med Health 43: 247–252. Link: https://bit.ly/3cch5Qe
- Freedman SB, Ali S, Oleszczuk M, Gouin S, Hartling L (2013) Treatment of acute gastroenteritis in children: an overview of systematic reviews of interventions commonly used in developed countries, Evid.-Based Child Health 8: 1123–1137. Link: https://bit.ly/3gzMQXc
- Webb A, Starr M (2005) Acute gastroenteritis in children. Aust Fam Physician 34: 227-231.Link: https://bit.ly/2XCLTEz
- Wade G (2009) Fluid problems in infants and children. In: Kee JL, Paulanka BJ, Polek C, eds. Handbook of fluid, electrolytes and acid-base inbalance. 3rd ed. Clifton park, New York: Delmar Cengage Learning Inc 190–240.
- Karen SP (2015) Dehydration: isonatraemic, hyponatraemic and hypernatraemic recognition and management. Pediatr Rev 36: 274-285. Link: https://bit.ly/3ephbpi
- Kocaoglu C, Solak ES, Kilicarslan C, Arslan S (2014) Fluid management in children with diarrhea-related hyponatremic hypernatremic dehydration: a retrospective study of 83 children. Med Glas (Zenica) 11: 87–93. Link: https://bit.ly/3ccgo9A
- Neville KA, Verge CF, O’meara MN, Walker JL (2005) High antidiuretic hormone level and hyponatraemia in children with gastroenteritis. Pediatrics 116: 1401–1407. Link: https://bit.ly/2X7ia7L
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
