Open Journal of Orthopedics and Rheumatology
Evaluation of the SARS-CoV-2 infection rate in patients undergoing Total Hip Arthroplasty by the Anterior Approach using a Rapid Recovery Protocol during a COVID-19 pandemic in a Public Hospital in the State of São Paulo
Marco Aurélio Silvério Neves1-3, Victor Edmond Seid1, Leandro Gregorut Lima1,3, Gustavo Rocha Santos1,3, Dimas Vicente Terra Santos1, Bruno da Silva Ivo1, Ivan Espuri2 and Barbara Fialho Carvalho Sampaio1-3*
2Arthron Medical Services, Brazil
3School of Medicine, University of Sao Paulo, Brazil
Cite this as
Silvério Neves MA, Seid VE, Lima LG, Santos GR, Carvalho Sampaio BF, et al. (2021) Evaluation of the SARS-CoV-2 infection rate in patients undergoing Total Hip Arthroplasty by the Anterior Approach using a Rapid Recovery Protocol during a COVID-19 pandemic in a Public Hospital in the State of São Paulo. Open J Orthop Rheumatol 6(1): 067-072. DOI: 10.17352/ojor.000041Copyright
© 2021 Silvério Neves MA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.The World Health Organization (WHO) declared, on January 30, 2020, that the outbreak of the disease caused by the new Coronavirus (COVID-19) constitutes a Public Health Emergency of International Importance - the highest level of alert of the Organization, as provided for in the International Health Regulations. On March 11, 2020, COVID-19 was characterized by the WHO as a pandemic and since then the world has been going through an unprecedented period. The pandemic is interfering with all aspects of everyday life, especially in the area of health. Surgical practice was directly affected by the suspension of elective procedures and the prioritization of urgent and emergency surgeries as a way to free up beds for patients infected with the disease. New coronavirus. The script for resumption of elective surgery after this COVID-19 pandemic must be progressive and cautious. Elective surgery should be performed in COVID-free facilities and the hospital stay should be as short as possible. For safety reasons, patients considered for surgery should be carefully selected according to status/exposure to COVID-19 infection, age, ASA physical status/risk factor classification system, socio-professional status and surgical indication. Therefore, in this study, we will demonstrate the positive impact on surgical resumption using a rapid recovery protocol combined with a minimally invasive technique (AMIS) for total hip arthroplasty during the period of worldwide pandemic for SARS-CoV-2.
Introduction
Since December 2019, pneumonia is caused by the RNA virus called COVID-19, belonging to the Coronaviridae family. COVID-19 infection can range from a common cold-like symptomatology to severe viral pneumonia or the occurrence of acute respiratory distress syndrome, which can be potentially fatal [1].
The main transmission routes are respiratory, through the inhalation of droplets and aerosols eliminated through coughing or sneezing, as well as through the aerosolization of bodily substances during procedures that manage the airways, such as intubation, extubating, aspiration, cardiopulmonary resuscitation, non-invasive ventilation and bronchoscopy [2,3]. However, the transmissibility of the virus through bodily secretions is not well established. There is evidence of the presence of viral load in saliva, tears, and eye secretions from patients with conjunctivitis and in feces [4-6].
Surgical practice was directly affected and infection prevention and control measures should be implemented by professionals working in surgical centers and with surgical patients, to avoid or reduce as much as possible the transmission of microorganisms during any health care provided [7].
Thus, the planning for the maintenance and resumption of surgical procedures, in general, should be based on new protocols and practices for the prevention and control of the transmission of the new coronavirus (SARS-CoV-2) within operating rooms [8] to avoid contamination of surgical teams, care and also other hospitalized patients.
The patient should be screened preoperatively (eg, by tele or videoconference) with a detailed question about their current health and including questions related to COVID-19 such as symptoms, exposure, previous tests performed. Patients must understand all aspects of their medical care that may change due to the current health emergency situation and also be aware of the limited but existing risks of COVID-19 infection during surgery or hospitalization. Despite all the preventive measures put in place by the facility to avoid COVID-19 infections during surgery or hospitalization, the risk of infection cannot really be 100% excluded [9].
The patient must agree to undergo surgery under these conditions, as well as additional preoperative screening. If COVID-19 is suspected or confirmed after preoperative screening, surgery should be postponed.
In the initial phase of reintroduction of elective surgical cases, the selection of patients must respect criteria, avoiding known risk groups with high mortality for SARS Cov-2, in addition to the indication for surgery.
Currently, the viral concentration of SARS Cov-2 in particular, periarticular and bone tissues and fluids of infected patients is currently unknown. However, it is reasonable to assume that it is lower in musculoskeletal tissues than in respiratory or digestive tissues. Given these uncertainties, it is recommended to minimize procedures that generate a large amount of aerosols, such as the use of electrocautery, the use of oscillating saws and pulse washing procedures [10].
In the absence of well-established scientific criteria, minimally invasive and arthroscopic procedures may present a lower risk of infection and currently appear to be safer. They should be considered a priority if elective surgeries are resumed. Surgical procedures followed by a hospital stay of no more than two to three days should initially be favored. Surgeries with a greater degree of invasiveness and blood loss can occur later, avoiding prolonged hospitalization or the need to use a place in the Intensive Care Unit.
Optimizing the allocation of resources and spaces, especially intensive care beds, for the orthopedic surgical demand is essential during the pandemic. Therefore, it is of paramount importance to use rapid recovery protocols, which in line with minimally invasive techniques will be essential for safe resumption in elective surgeries.
In conventional approaches for total hip arthroplasty, the patient is usually referred to the ICU after surgery, due to the risk of postoperative bleeding and to monitor vital parameters. From the third or fourth day after surgery, the patient is encouraged to get out of bed and start walking with the walker, being discharged to the ward. After the patient adapts to his new condition, using the walker, he is discharged from the hospital with a series of restrictions such as avoiding crossing his legs, sitting on low chairs or armchairs, using a raised toilet seat and walking with the walker until the third month postoperative period with the intention of reducing the chance of dislocation of the prosthesis until all the structures, sectioned or resected in the conventional lateral and posterior access routes, are healed.
Usually, the average length of hospital stay in patients varies from 5 to 7 days [11], which may increase the risk of contamination by SARS-CoV-2 due to the long stay in the hospital.
Total hip arthroplasty is a cost-effective treatment for degenerative joint disease, with up to 90% of patients reporting return of joint function, pain relief, and improved quality of life [12,14]. The introduction of joint care programs and rapid or fast track recovery protocols has reduced the length of stay (LOS - Length of Stay) for total hip and knee arthroplasty from 7 to 10 days to 2 to 4 days in recent decades [15-18].
The standardization of minimally invasive operating techniques, such as the direct anterior approach (DDA), in combination with fast-track principles (Rapid Recovery Protocols) based on medical procedures guided by scientific evidence, reduced the hospital stay without compromising safety of the patient [19]. It should be noted that organizational issues pre-admission and during the interaction period, together with extensive pre-operative patient information to implement and execute the time-based rapid recovery protocol, require a lot of clinical and organizational effort from everyone involved.
The use of a Rapid Recovery Protocol or fast-track improves the patient's prognosis and reduces morbidity and mortality, thus demonstrating the importance of using these protocols during this period of the COVID-19 pandemic. We believe that, in most cases, this type of focused care is adequate and completely safe. Patients should receive the best treatment available, which requires optimized logistics to allow for early discharge, resulting in less patient exposure to other infectious agents in the hospital.
The advantages of performing total hip arthroplasty via an anterior approach using the AMIS technique (Anterior Minimaly Invasive Surgery) are described as reduced tissue trauma, reduced blood loss, less postoperative pain, shorter hospital stay, better aesthetic appearance and shorter postoperative recovery time [18-20].
All these facts presented here demonstrate the positive impact on surgical resumption when using a rapid recovery protocol combined with a minimally invasive technique (AMIS). This combination of rapid recovery protocol together with minimally invasive techniques will be decisive for surgical resumption during the period of worldwide pandemic by SARS-CoV-2.
Aim
Primary: Evaluate the following admission data for patients undergoing elective total hip arthroplasty surgery via anterior access using the AMIS technique and undergoing a rapid recovery protocol during the hospital stay:
- Hospitalization time
- Need and time of ICU use
- Use of Blood Derivatives Intra and Postoperative
- Immediate Postoperative Complications such as Deep Vein Trombosis (DVT), Pulmonary Trhromboendarterectomy (PTE), Postoperative Bleeding, Neurological Injury and Implant Instability
Secondary: Evaluate the rate of patients with flu-like symptoms and/or diagnosed with COVID 19, fifteen days after the surgical procedure.
Materials and methods
Prospective and retrospective cohort study conducted at Hospital Regional São José dos Campos during 2020 and 2021.
The inclusion criteria for data collection and active search for cases with flu-like symptoms by telephone contact will be patients with primary osteoarthrosis of the hip joint under the age of 55 years and who were on the waiting list to undergo total hip arthroplasty. All participants in the study provided a consent form for the study. The exclusion criteria were patients who did not sign the Free and Informed Consent Form.
Thirty patients underwent total hip arthroplasty via AMIS included in the Rapid Recovery Program, operated by a single specialist hip surgeon, with experience in the anterior access technique/AMIS, from September 2020 to March 2021.
Demographic data, medical history, smoking, alcohol consumption, comorbidities, length of stay, need to use ICU, use of blood products, immediate postoperative complications such as Deep Vein Trombosis (DVT), Pulmonary Trhromboendarterectomy (PTE), Postoperative Bleeding, Neurological Injury and Implant Instability were removed from the medical record.
The BMI is a convenient rule of thumb used to broadly categorize a person as underweight, normal weight, overweight, or obese based on tissue mass (muscle, fat, and bone) and height. Major adult BMI classifications are underweight (under 18.5 kg/m2), normal weight (18.5 to 24.9), overweight (25 to 29.9), and obese (30 or more).
The investigation of post-surgical flu-like symptoms and diagnosis of COVID-19 infection was carried out by telephone 15 days after the surgical procedure.
All data obtained were analyzed using the GraphPad Prism statistical platform (GraphPad software, Inc. San Diego, California, USA) and Excel ® (Microsoft), so that the correlations could be analyzed and evaluated.
Results
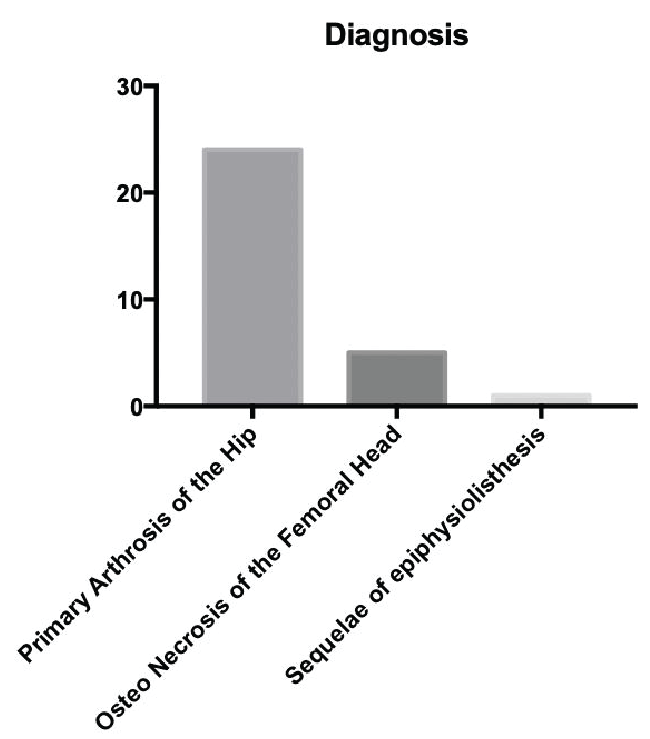
Thirty patients were included in this study, 13 females and 17 males, with a mean age of 48 years. The main indication for surgery was Primary Hip Arthrosis, as shown in Figure 1.
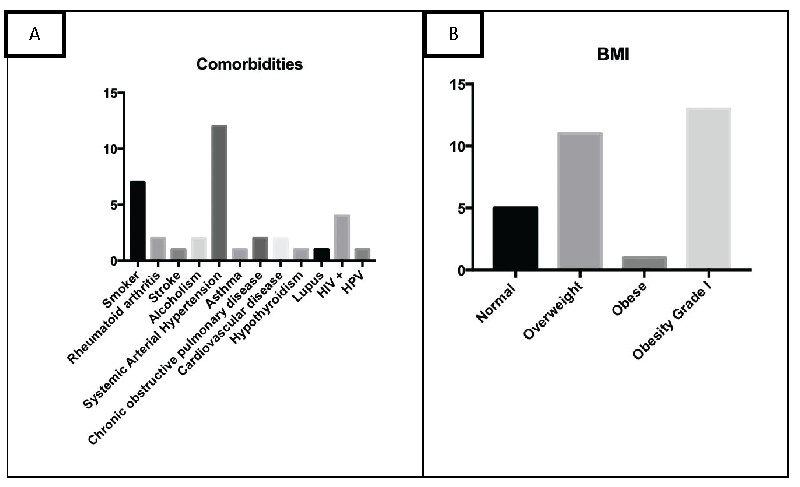
Study patients had the following comorbidities: Smoking – 6 patients (20%); Systemic Arterial Hypertension (SAH) – 12 patients (40%); HIV (Human Immunodeficiency Virus) – 4 patients (13%); Rheumatoid Arthritis – 3 patients (10%); Cardiovascular Disease (CVA) or Acute myocardial infarction (AMI) – 4 patients (13%); Alcoholism – 3 patients (10%), as shown in Figure 2A.
According to Body mass index (BMI) classification; 5 patients (17%) were of normal weight; 11 patients (37%) were overweight and 14 patients (47%) were obese grade 1, Figure 2B.
The average time of surgery was 1 hour and 18 minutes (78 minutes) and no patient required transfusion of blood products.
As for immediate Postoperative complications, we had no events for PTE, DVT, Neurological Injury and Implant Instability. Only 1 patient (3%) had postoperative bleeding requiring dressing change and no patient needed to be referred to the ICU postoperatively.
All 30 patients (100%) had full weight bearing on the operated limb on the same day of surgery.
The average length of stay was 1.37 days with 20 patients (67%) staying 1 day in the hospital, 9 patients (30%) staying 2 days in the hospital and 1 patient (3%) staying 3 days in the hospital.
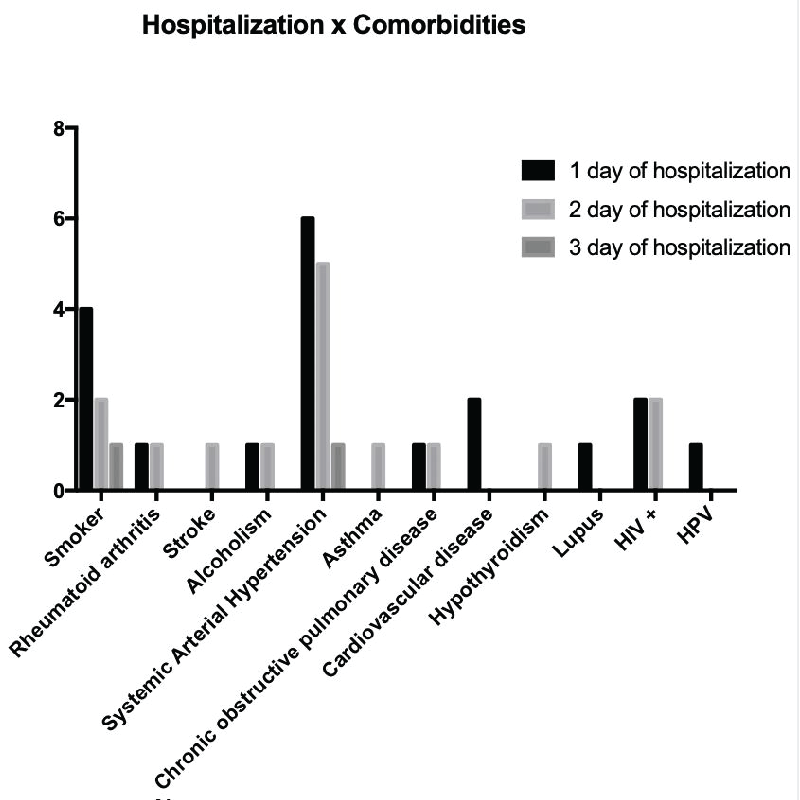
As can be seen in Figure 3, patients with SAH(5), smoking(4) and HIV+(4 ) had a longer hospital stay compared to the general population of the study.
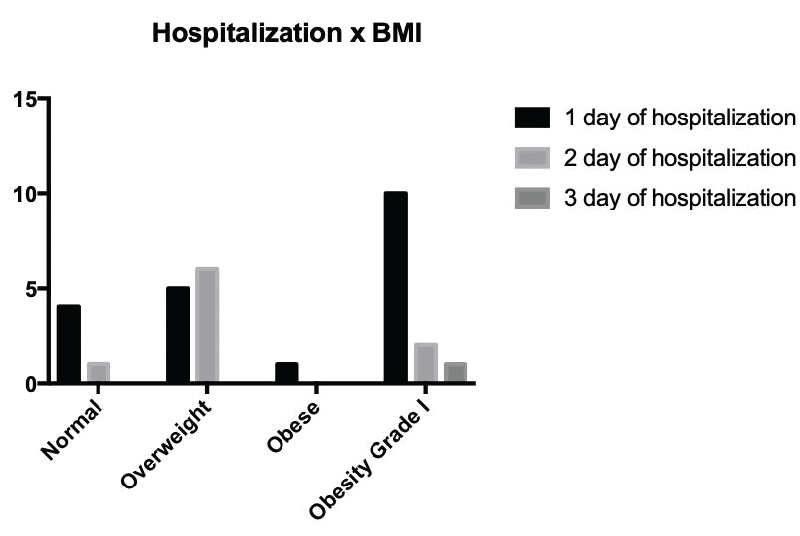
When we evaluated the body mass index and length of stay, we noticed that overweight(7) and obese(2) patients had an average hospital stay of 1 day longer compared to patients with normal BMI, as can be seen in Figure 4.
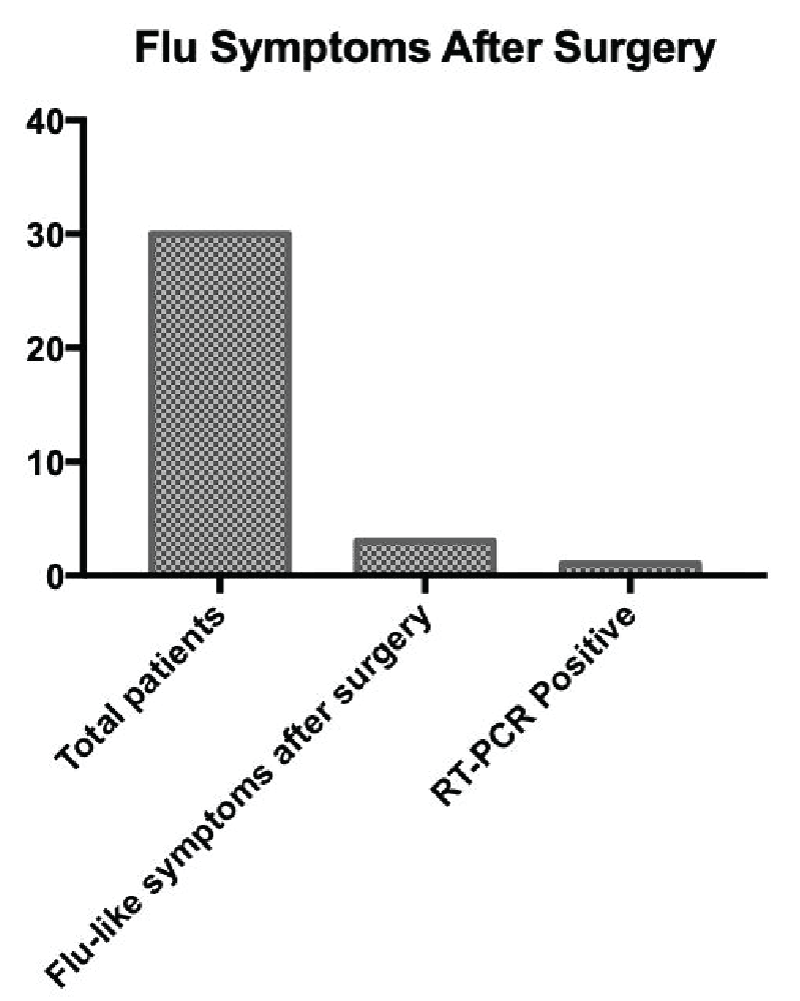
After 15 days of the surgical procedure, the active telephone survey showed that 3 patients (10%) had flu-like symptoms and underwent the RT-PCR test for COVID-19, and only 1 patient (3%) tested positive for COVID-19, Figure 5.
Discussion
According to national law, state and municipal governments are empowered to define when and how to resume elective medical procedures [21]. As a result, health services are planning alternatives to start the new phase of coping with the pandemic and to mitigate the possibility of viral transmission from person to person. This is done, above all, to avoid the transmission of patients without previous infection who will undergo non-emergency procedures and are subject to possible SARS-CoV-2 transmission from asymptomatic patients.
Currently minimally invasive or arthroscopic surgery may have the lowest risk for both patients and surgeons. A strategy to resume elective surgery can, therefore, be envisaged considering these types of minimally invasive surgeries for patients under 60 years old, without comorbidity and hospital stay for a maximum of 3 days [22]. Preoperative screening of patients and proper scheduling should be done according to COVID-19 status, when we align this schedule with rapid recovery protocols, it can bring more safety to the entire surgical procedure.
In the initial phase of reintroduction of elective surgical cases, patient selection should also include indication for surgery. Currently, the viral concentration of SARS Cov-2 in particular, periarticular and bone tissues and fluids of infected patients is currently unknown. However, it is reasonable to assume that it is lower in musculoskeletal tissues than in respiratory or digestive tissues. Given these uncertainties, it is recommended to reduce the types of surgeries that generate a large amount of aerosols, such as electrocautery, working with oscillating saws and pulse washing procedures [10]. In the absence of well-established scientific criteria, minimally invasive and arthroscopic procedures may present the lowest risk of infection and currently appear safer. They should be considered a priority if elective surgeries are resumed. Surgical procedures followed by a hospital stay of no more than two to three days should initially be favored. Surgeries with a greater degree of invasiveness and blood loss may occur later.
As well demonstrated by our team, even working with young patients, we observed high rates of comorbidities in patients: 20% were smokers, 40% had SAH, 13%; Rheumatoid Arthritis 10%, Cardiovascular Disease (CVA or AMI) 13% and Alcoholism 10%.
The optimization of the allocation of resources and spaces, especially intensive care beds, for the orthopedic surgical demand is essential during the pandemic [22]. Several countries with epidemiological curves similar to the Brazilian one presented saturation of medical care capacity during this period and during the entire surgical period we did not use vacancies in the ICU, and no patient used bags of blood products.
Reducing elective activity, including outpatient surgery, has some key benefits, freeing up ward and ICU beds, increasing capacity for patients infected with COVID-19. However, as demonstrated by our results, using a minimally invasive technique, we did not occupy any ICU bed.
When we reach this critical point, it is essential that we start planning a return to a more normal health reality. Health care and orthopedic surgery will be an important component of the population's economic and social recovery [23].
The combined use of a minimally invasive technique and the rapid recovery protocol seem to reduce the hospital stay of patients undergoing total hip arthroplasty, without increasing the risk of complications from SARS-CoV-2. The beneficial effects of the rapid recovery protocol appear to be amplified and are synchronized with operating requirements in the era of a pandemic.
Conclusion
As the global crisis caused by the pandemic, most orthopedic activities were abruptly stopped, both in the outpatient clinic and in the operating room, now with a greater understanding of COVID-19, a progressive onset scenario needs to be planned. Once the restrictions are lifted, the clinical and surgical volume will progressively increase. This article demonstrates a very promising and favorable experience, bringing security to the resumption of elective surgeries in orthopedics, using a minimally invasive technique combined with a rapid recovery protocol. Some ground rules and possible strategies to provide the highest level of safety to the orthopedic patient and orthopedic team, including minimally invasive techniques combined with rapid recovery protocols will be essential.
- Beeching NJ, Fletcher TE, Fowler R, Petri WA, Zhang X, et al. (2020) Coronavirus (covid-19): latest news and resources. BMJ Best Practices. Link: https://bit.ly/3hWtk9s
- Brasil (2018) Ministério da Saúde. Agência Nacional de Vigilância Sanitária. 76.
- Center for Diseases Control and Prevention (CDC) (2018) Recommended guidance for extended use and limited reuse of N95 filtering facepiece respirators in healthcare settings.
- Center for Diseases Control and Prevention (CDC) (2020) Interim U.S. guidance for risk assessment and public health management of healthcare personnel with potential exposure in a healthcare setting to patients with coronavirus disease (COVID-19).
- To KK, Tsang OT, Yip CC, Chan KH, Wu TC, et al. (2020) Consistent Detection of 2019 Novel Coronavirus in Saliva. Clin Infect Dis 71: 841-843. Link: https://bit.ly/3Axtify
- Xia J, Tong J, Liu M, Shen Y, Guo D (2020) Evaluation of coronavirus in tears and conjunctival secretions of patients with SARS-CoV-2 infection. J Med Virol 92: 589-594. Link: https://bit.ly/3AAgxB0
- Center for Diseases Control and Prevention (CDC) (2020) What healthcare personnel should know about caring for patients with confirmed or possible COVID-19 Infection.
- Ti LK, Ang LS, Foong TW, Ng BSW (2020) What we do when a COVID-19 patient needs an operation: operating room preparation and guidance. Can J Anaesth 67: 756-758. Link: https://bit.ly/3EQLDqy
- Clinical management of severe acute respiratory infection when COVID-19 is suspected. Link: https://bit.ly/3AAgeGm
- Hirschmann MT, Hart A, Henckel J, Sadoghi P, Seil R, et al. (2020) COVID-19 coronavirus: recommended personal protective equipment for the orthopaedic and trauma surgeon. Knee Surg Sports Traumatol Arthrosc 28: 1690-1698. Link: https://bit.ly/2W46BRa
- AAOS guidelines for elective surgery - American Academy of Orthopaedic Surgeons. Link: https://bit.ly/2XGJ0XG
- Husted H, Hansen HC, Holm G, Bach-Dal C, Rud K, et al. (2006) Length of stay in total hip and knee arthroplasty in Danmark I: volume, morbidity, mortality and resource utilization. A national survey in orthopaedic departments in Denmark. Ugeskr Laeger 168: 2139– 2143. Link: https://bit.ly/3CBWgeI
- Husted H, Holm G, Jacobsen S (2008) Predictors of length of stay and patient satisfaction after hip and knee replacement surgery: fast-track experience in 712 patients. Acta Orthop 79: 168-173. Link: https://bit.ly/3kx8z5K
- Husted H, Hansen HC, Holm G, Bach-Dal C, Rud K, et al. (2010) What determines length of stay after total hip and knee arthroplasty? A nationwide study in Denmark. Arch Orthop Trauma Surg 130: 263–268. Link: https://bit.ly/3lKULUJ
- Husted H, Lunn TH, Troelsen A, Gaarn-Larsen L, Kristensen BB, et al. (2011) Why still in hospital after fast-track hip and knee arthroplasty? Acta Orthop 82: 679–684. Link: https://bit.ly/3hXW8hP
- Husted H, Jensen CM, Solgaard S, Kehlet H (2012) Reduced length of stay following hip and knee arthroplasty in Denmark 2000-2009: from research to implementation. Arch Orthop Trauma Surg 132: 101-104. Link: https://bit.ly/2ZbGSHy
- Glassou EN, Pedersen AB, Hansen TB (2014) Risk of re-admission, reoperation, and mortality within 90 days of total hip and knee arthroplasty in fast-track departments in Denmark from 2005 to 2011. Acta Orthop 85: 493–500. Link: https://bit.ly/39pn851
- Howell JR, Masri BA, Duncan CP (2004) Minimally invasive versus standard incision anterolateral hip replacement: a comparative study. Orthop Clin North Am 35: 153-162. Link: https://bit.ly/2XGtgDi
- Sendtner E, Borowiak K, Schuster T, Woerner M, Grifka J, et al. (2011) Tackling the learning curve: comparison between the anterior, minimally invasive Micro-hip®) and the lateral,transgluteal (Bauer) approach for primary total hip replacement. Arch Orthop Trauma Surg 131: 597-602. Link: https://bit.ly/3zu5nMM
- Bergin PF, Doppelt JD, Kephart CJ, Benke MT, Graeter JH, et al. (2011) Comparison of minimally invasive direct anterior versus posterior total hip arthroplasty based on inflammation and muscle damage markers. J Bone Joint Surg Am 93: 1392-1398. Link: https://bit.ly/3EG5GrG
- Conselho Federal de Medicina. Combate à COVID-19 (2020) Recomendação aos CRMs sobre avaliação dos atendimentos eletivos. Link: https://bit.ly/3lP2C3z
- Mouton C, Hirschmann MT, Ollivier M, Seil R, Menetrey J (2020) COVID-19 - ESSKA guidelines and recommendations for resuming elective surgery. J Exp Orthop 7: 28. Link: https://bit.ly/3nVhUXj
- Center for Medicare and Medicaid Services National health expenditure data. CMSGov. Link: https://go.cms.gov/3EQLqDR
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
