Open Journal of Orthopedics and Rheumatology
Biomechanical assessment in HAV treatment
Ma Ángeles Rodríguez Personat*, Fernando Chacón Giráldez, Lidia Carvajal Moreno and Ana Juana Pérez Belloso
Cite this as
Rodríguez Personat MA, Giráldez FC, Moreno LC, Pérez Belloso AJ (2021) Biomechanical assessment in HAV treatment. Open J Orthop Rheumatol 6(1): 042-045. DOI: 10.17352/ojor.000037Hallux Abductus Valgus (HAV) is a pathology that affects the first metatarsophalangeal joint, in which there is a medial displacement of the metatarsal and a lateral deviation of the hallux, causing joint dysfunction and disability in the patient. There are two types of treatments for this condition (conservative and surgical), and both require an exhaustive biomechanical assessment, since biomechanics are the main cause of this deformity.
The main objective of the article is the development of a biomechanical examination and assessment algorithm to be carried out systematically in patients with HAV.
Introduction
Hallux Abductus Valgus (HAV) is a deformity that affects the forefoot in which there is a medial deviation of the first metatarsal and the lateral deviation of the first toe.
Currently this condition affects around the 26% of the adults worldwide, being 36% of those affected over 65 years. In addition, HAV has a higher prevalence in the western countries and a lower prevalence in the eastern, where it began to increase in the mid-20th century with the use of high-heeled and narrow toe-box shoes [1,2].
The etiology of HAV is biomechanical, therefore, to solve the problem we must know the cause, and so we have to carry out a good biomechanical exploration.
Static evaluation
Hip evaluation: Using the Trendelenburg test, which consists of observing the patient in a single limb-stance position on the affected limb for 30 seconds. The examiner places his hands or a levelometer on the iliac crests to observe their alignment. It is considered positive if, in the position of single leg stance, the hip falls to the opposite side. A positive sign of this test would indicate weakness of the gluteus medius and minus (hip abductors)[1].
Knee evaluation: Measured with a two-branch goniometer the knee that we are exploring and the dynamic observation of these. Observed the presence of genu varus or genu valgus, this indicates joint incongruity caused by pathological pronation. Also, we must assess if the knee flexion / extension is complete or if there is pain when moving it [2].
Ankle evaluation: Equinus deformity is the main cause of pathologies related to the gait cycle, directly linked to the ankle joint. this joint we have the Achilles tendon, one of the reasons of the equinus [3]. As a direct consequence of this equinus condition, we can also appreciate Hallux Valgus, and many other alterations in the forefoot such as hammer toes, metatarsal pain, narrow heel sign, genu recurvatum or hyperlordosis [4].
In this examination: the Silfverskjöld Test is performed. It is used to identify equinus deformity when the ankle and the knee are in extension. This situation is not perceived when the knee is flexed. Despite the clinical examination of the test, we can refer to additional clinical signs that may give us evidence of shortening of gastrocnemius [5], wherever, the Silfverskjöld Test doesn´t allow identify shortening of soleus.
To evaluate the soleus muscle: we must perform ankle dorsiflexion while keeping the knee flexed [5].
Subtalar joint evaluation: To achieve a correct function of this joint, it is required at least 8º of range of motion [6].
In this case, we assessed the clinical axis of the calcaneus. It was evaluated in a standing position and quantified the axis that was formed between the distal third of the tibia and the posterior surface of the calcaneus. The reference values are between 0º and 5º.
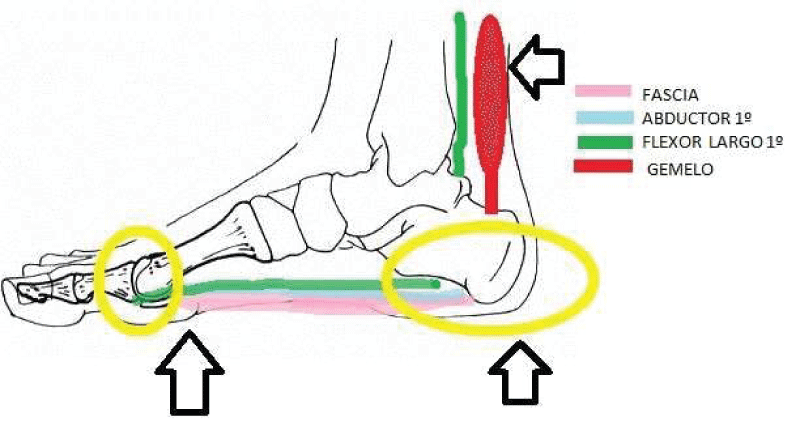
Achilles-calcaneus-plantar system evaluation: Anatomically, there is a relationship between the posterior leg muscles (gastrocnemius) and the HAV through the fascia.
This is due to the anatomical situation of the gastrocnemius (insertion in the calcaneus), the medial band of the plantar fascia (origin in the calcaneus and insertion in the 1st metatarsophalangeal joint).
To checked the correct functioning of the achilles-calcaneus-plantar system, the patient is asked to stand on tiptoe and, if this is correct, the calcaneus inverts [7].
First ray evaluation: This joint presents mobility in the 3 planes of space, so when performing dorsiflexion it is accompanied by an inversion (dorsiflexion + inversion) and when performing plantarflexion by an eversion (plantarflexion + eversion). When the 1st ray has no more dorsiflexion or inversion capacity, the subtalar joint continues pronating and the foot fully everts. The reference values are around 5 mm of dorsiflexion and 5 mm of plantarflexion [8-11].
To assess the firs ray, the subtalar joint was placed in a neutral position and the minor metatarsals are hugged with one hand and the 1st metatarsal is mobilized in dorsal flexion and plantar flexion. With the help of a goniometer, we assessed the greater range of motion and this will indicate the position of the metatarsal [8,12].
To rate the stability of the 1st metatarsal we assessed the peroneus longus muscle [13]. For this, we asked the patient to lie supine or in a sitting position, we placed the homolateral hand to the foot that we are going to explore holding the retromalleolar area, the other hand is placed in the plantar and external surface of the foot for making resistance and we ask the patient to do eversion along with plantar flexion of the ankle.
1st Metatarsophalangeal joint evaluation
For the measurement we marked two reference points. Point one, which corresponds to the midline of the medial phalanx, and point two which corresponds to the midline of the first metatarsal, both on the tibial surface of the foot. We placed the mobile and fixed branches of a goniometer respectively and did the movement of flexion and extension of the joint, so that we obtained the degrees of movement. This is done both in a standing and unloading position [8,11,14].
We need 60º of extension of this joint in order to a correct gait. When measuring metatarsophalangeal joint extension with the ankle in a 90º position to the leg, 10º less is obtained than measuring it with the ankle in a relaxed position [8]. This is determined by the relationships between the muscles of the leg, specifically the gastrocnemius, and the metatarsophalangeal joint [15].
Dinamic evaluation
Pelvis evaluationDuring heel support: We observed the lateral stabilization of the pelvis, controlled by the hip abductor muscles (gluteus medius, gluteus minimus and tensor fasciae latae)[2,16].
In the period of support: The pelvis generates maximum internal rotation and swings towards the limb that is oscillating. The abductor muscles contract to stop the pelvic swinging.
In the propulsive phase: The pelvis is in external rotation, however, in the frontal plane there is no swinging towards the contralateral limb and in the sagittal plane there is anteversion. Regarding the musculature, the hip adductors contract for the first time, together with the iliac psoas, whose function is to stop the hip hyperextension that is generated by moving the trunk forward.
Oscillation phase: The pelvis is placed back in relation to the member in question. It is the iliopsoas in charge of performing the hip flexion in order to start a new cycle.
In patients with HAV, the hip has an abnormal balance, abduction is decreased and adduction is increased, and the pelvis of the limb in which the HAV is located has a lower height [17]. Furthermore, all these abnormalities are directly related to subtalar joint pronation, thus establishing a direct relationship between HAV and pelvis, as is the case with the knee joint. [18].
Knee evaluation: Patients with HAV have a decreased maximum extension in the oscillating phase [17].
Ankle evaluation:. The center of the ankle joint determines the tendency to internal or external tibial torsion, depending on whether it is medialized or lateralized [2,14] .
In the period of heel contact: The ankle is in a slight dorsal flexion, and from this moment it begins progressively to perform plantarflexion. The muscles involved in this period are tibialis anterior (slowing plantarflexion of the ankle) and tibialis posterior (control of subtalar joint pronation)[2]. In this period, we must observe if the ankle dorsiflexion is enough and if the pronation of the subtalar joint is completely controlled by the musculature.
In the period of support: The tibia advances and is settled perpendicularly to the foot. The muscles in charge of doing this are quadriceps (indirectly stops the advance of the tibia forward), tibialis posterior (controlling the pronation of the subtalar joint) and the peroneus both brevis and longus, which control lateral internal tibial displacement caused by pelvic swing of the oscillating limb.
In the propulsive period: The tibia advances and is preceded by an elevation of the heel. The muscles involved here will be triceps surae (plantarflexion of the foot), flexors (enhance action of the triceps surae) and peroneus (generating pronation of the forefoot that allows stability of M1 and propulsion).
In patients with HAV, the ankle dorsiflexion movement is decreased[17,19]. This situation is caused by a shortening of the gastrocnemius (mainly the medial one), which are anatomically related to the metatarsophalangeal joint throughout the achilles-calcaneus-plantar system [5,20].
In addition, the shortening of the posterior muscles would be one of the causes of HAV in young patients and relates the medial band of the fascia, the abductor of the 1st finger and the flexor longus of the 1st finger (structures that are inserted at the level of the first toe) as aggravating the pathology and not as causing it [5,21] Figure 1.
Foot evaluation
o In the contact period: The calcaneus is inverted, and the subtalar joint is fully supinated. As it goes on, a subtalar joint pronation is generated whose main objective is to cushion the forces of the floor and adapt the foot to the ground. At the same time, a greater movement is generated in the forefoot, in order to the peroneal edge of the forefoot (5th metatarsal) contacts the ground earlier.
o In the single limb-stance: subtalar joint is pronated and from this moment on a progressive supination is generated. In turn, at the end of this period, the forefoot generates a supination, the objective of which is to get the head of the 1st metatarsal to the ground and begin to receive all the weight. In this phase, full contact of the toes happens and the metatarsophalangeal and interphalangeal joints are neutral.
o In the propulsive period: The tibia produces an external rotation that is brought with it to the subtalar joint, where a supination movement is generated. At this time, the hindfoot is in inversion regarding the forefoot, where the weight falls on the head of the 1st metatarsal and the foot takes off as a rigid and propulsive lever [2,16].
In patients with HAV, there is an excessive pronation of the subtalar joint or an abnormality of this during any stage of the gait cycle, mainly in the propulsive period. As a result, it produces an abnormal function of the peroneus longus muscle and an instability of the first ray during the propulsion [22-26].
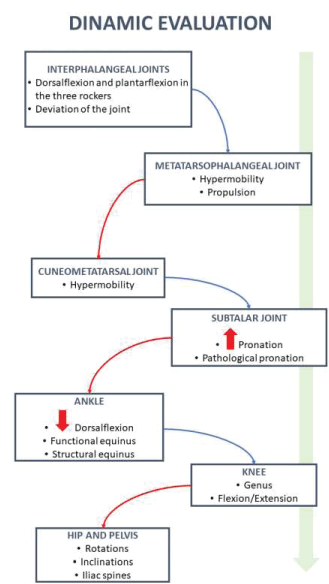
Evaluation algorithm
Figures 2,3
- Gogu S, Viraj N (2020) Gandbhir. Trendelenburg Sign. 2020. Link: https://bit.ly/34OE3vT
- Moreno de la Fuente JL (2009) Cinética de la marcha y protocolo de exploración. En podologia general y biomecánica. 402–407.
- Johnson KL, Degnan KA, Ross Walker J, Ingram GC (2005) AtDEK1 is essential for specification of embryonic epidermal cell fate. Plant J 44: 114-127. Link: https://bit.ly/3cb8SyC
- Colombier JA (2012) Brièveté des gastrocnémiens dans les métatarsalgies. In Brièveté des gastrocnémiens: de l’anatomie au traitement. Sauramps Montpellier (France) 285-294.
- Barouk P, Barouk LS (2014) Clinical diagnosis of gastrocnemius tightness. Foot Ankle Clin 19: 659-667. Link: https://bit.ly/3yTZlFR
- Moreno de la Fuente JL (2009) Parámetros clínicos normales y patológicos. En Pología general y biomecánica 272-281.
- Moreno de la Fuente JL (2009) Estudio de las articulaciones del pie. En Pología general y biomecánica. Barcelona: Masson 285-294.
- Munuera-Martínez PV (2009) Exploración biomecánica del primer radio y primera articulación metatarsofalángica. In El primer radio: biomecánica y ortopodología 105-126. Link: https://bit.ly/3uEuqKz
- Ebisui JM (1968) The first ray axis and the first metatarsophalangeal joint: an anatomical and pathomechanical study. J Am Podiatry Assoc 58: 160-168. Link: https://bit.ly/3yNEa8J
- Munuera-Martínez PV, Távara-Vidalón P, Monge-Vera MA, Sáez-Díaz A, Lafuente-Sotillos G (2020) The Validity and Reliability of a New Simple Instrument for the Measurement of First Ray Mobility. Sensors 20: 2207. Link: https://bit.ly/3i8mS04
- Tavara-Vidalón SP, Monge-Vera MÁ, Lafuente-Sotillos G, Domínguez-Maldonado G, Munuera-Martínez PV (2018) Static range of motion of the first metatarsal in the sagittal and frontal planes. J Clin Med 7: 456. Link: https://bit.ly/3fSC7as
- Glasoe WM, Michaud TC (2019) Measurement of dorsal first ray mobility: a topical historical review and commentary. Foot Ankle Int 40: 603-610. Link: https://bit.ly/34yLaZ9
- Glasoe WM (2016) Treatment of progressive first metatarsophalangeal hallux valgus deformity: a biomechanically based muscle-strengthening approach. J Orthop Sports Phys Ther 46: 596-605. Link: https://bit.ly/3fBxB1l
- del Amo Lorente AL, Reye RC, Munuera PV, Martínez RGÚ, Macías JLS (2013) Cuál es el protocolo de exploración más adecuado a la hora de valorar la primera articulación metatarsofalángica?. Revista española de podología 24: 25-29. Link: https://bit.ly/3pb30KZ
- Barouk LS (2014) The effect of gastrocnemius tightness on the pathogenesis of juvenile hallux valgus: a preliminary study. Foot Ankle Clin 19: 807-822. Link: https://bit.ly/3wN6034
- Moreno de la Fuente JL (2009) La marcha humana. En Podología general y biomecánica. Barcelona: Masson 387–401.
- Klugarova J, Janura M, Svoboda Z, Sos Z, Stergiou N, et al. (2016) Hallux valgus surgery affects kinematic parameters during gait. Clin Biomech 40: 20-26. Link: https://bit.ly/3uz8T5W
- Márquez AM (2015) Relationship between the pronation of the foot and the syndrome of the pyramid in the corridor. Lect Educ física y Deport 14. Link: https://bit.ly/3vEF2KQ
- Moerenhout K, Chopra S, Crevoisier X (2019) Outcome of the modified Lapidus procedure for hallux valgus deformity during the first year following surgery: A prospective clinical and gait analysis study. Clin Biomech 61: 205-210. Link: https://bit.ly/3yVjtr8
- Blackwood S, Gossett L (2018) Hallux Valgus/Medial Column Instability and Their Relationship with Posterior Tibial Tendon Dysfunction. Foot Ankle Clin 23: 297-313. Link: https://bit.ly/3uz95lG
- Steinberg N, Siev-Ner I, Zeev A, Dar G (2015) The association between hallux valgus and proximal joint alignment in young female dancers. Int J Sports Med 36: 67-74. Link: https://bit.ly/3i8nfI4
- Lucaccini C, Zambianchi N, Zanotti G (2008) Distal osteotomy of the first metatarsal bone in association with sub-talar arthroerisis, for hallux valgus correction in abnormal pronation syndrome. Chir Organi Mov 92: 145-148. Link: https://bit.ly/3wLOP1z
- Smith BW, Coughlin MJ (2008) The first metatarsocuneiform joint, hypermobility, and hallux valgus: what does it all mean?. Foot Ankle Surg 14: 138-141. Link: https://bit.ly/3fX8pkR
- Singh D, Biz C, Corradin M, Favero L (2016) Comparison of dorsal and dorsomedial displacement in evaluation of first ray hypermobility in feet with and without hallux valgus. Foot Ankle Surg 22: 120-124. Link: https://bit.ly/2RaXMCF
- Li Y, Zhao L, Yu D, Ding G (2018) The prevalence and risk factors of dyslipidemia in different diabetic progression stages among middle-aged and elderly populations in China. PLoS One 13: e0205709. Link: https://bit.ly/34xd1Jc
- Guo J, Wang L, Ma R, Chang C, Wen J, et al. (2018) Biomechanical evaluation of the first ray in pre-/post-operative hallux valgus: a comparative study. Clin Biomech 60: 1-8. Link: https://bit.ly/3i5455B
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
