Open Journal of Orthopedics and Rheumatology
Uncovering secrets of the beauty bone: A comprehensive review of anatomy and regional anesthesia techniques of clavicle surgeries
Kartik Sonawane1*, Hrudini Dixit2, J.Balavenkatasubramanian 3 and Palanichamy Gurumoorthi4
2Fellow in Regional Anesthesia, Department of Anesthesiology, Ganga Medical Centre & Hospitals, Pvt. Ltd., Coimbatore, Tamil Nadu, India
3Senior Consultant, Department of Anesthesiology, Ganga Medical Centre & Hospitals, Pvt. Ltd., Coimbatore, Tamil Nadu, India
4Consultant, Department of Anesthesiology, Ganga Medical Centre & Hospitals, Pvt. Ltd., Coimbatore, Tamil Nadu, India
Cite this as
Sonawane K, Dixit H, Balavenkatasubramanian J, Gurumoorthi P (2021) Uncovering secrets of the beauty bone: A comprehensive review of anatomy and regional anesthesia techniques of clavicle surgeries. Open J Orthop Rheumatol 6(1): 019-029. DOI: 10.17352/ojor.000034The clavicle is the most frequently fractured bone in humans. General anesthesia with or without Regional Anesthesia (RA) is most frequently used for clavicle surgeries due to its complex innervation. Many RA techniques, alone or in combination, have been used for clavicle surgeries. These include interscalene block, cervical plexus (superficial and deep) blocks, SCUT (supraclavicular nerve + selective upper trunk) block, and pectoral nerve blocks (PEC I and PEC II). The clavipectoral fascial plane block is also a safe and simple option and replaces most other RA techniques due to its lack of side effects like phrenic nerve palsy or motor block of the upper limb. We present a comprehensive review of anatomy and RA techniques of clavicle surgeries. This review will help readers understand the functional anatomy and nature of clavicle fractures, and apply an algorithmic approach to procedure-specific blocks for complexly innervated structures like clavicle.
Introduction
GA: General Anesthesia; RA: Regional Anesthesia/Analgesia; SCUT block: Supraclavicular + Upper Trunk block; PEC: Pectoral Nerve block; ISB: Interscalene Block; CPB: Clavipectoral Fascial Plane Block; SCN: Supraclavicular Nerve; AC joint: Acromioclavicular joint; SIA: Single-Injection Approach; DIA: Double-Injection Approach; TIA: Triple-Injection Approach
Introduction
The name ‘clavicle’ is derived from the Latin word Clavicula, which means “little key” because it rotates along its axis like a key when the shoulder is abducted. Fractures of the clavicle are relatively common, accounting for up to 10% of all fractures [1]. Clavicle surgeries can be done under Regional Anesthesia (RA) with or without general anesthesia (GA), depending on the fracture site. Analgesia for clavicle fractures can be challenging for anesthesiologists due to the complex and varied innervation in this region.
Many RA techniques, either individually or in combinations, have been used for perioperative analgesia for clavicle surgeries. Some of these techniques include Interscalene Block (ISB) [2], combined ISB with superficial cervical plexus block [3], cervical plexus block [4], a combination of supraclavicular nerve and upper (superior) trunk (SCUT) block [5], a combination of a pectoral nerve (PEC) I block with selective supraclavicular nerve block [6], modified PEC II block [7] and Clavipectoral Fascial Plane Block [8-11] (CPB). We present a comprehensive review of the clavicle anatomy, its innervation, and different RA techniques used for clavicle surgeries.
Knowledge of functional anatomy and the surgical procedure helps in planning the procedure-specific RA technique for the patient. There is a paucity of literature on the innervations, associated pathologies, and optimal RA techniques for clavicle fractures. This review will help readers understand the clavicle anatomy and nature of fractures and apply an algorithmic approach to procedure-specific blocks for complexly innervated structures like clavicle.
Functional anatomy of clavicle
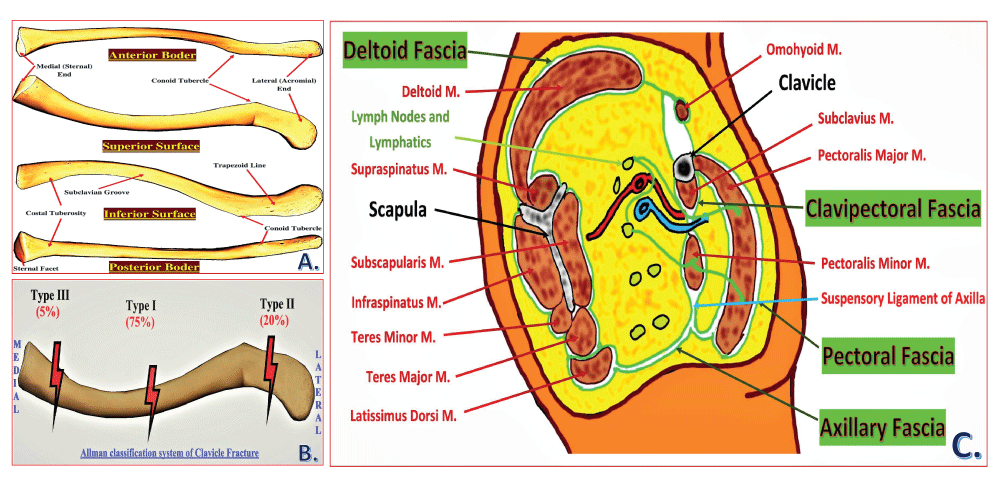
The clavicle, or collarbone, is also referred to as “beauty bone” because of its prominent body location. It is the only long bone that lies horizontally in the body. The shape of the clavicle appears elongated ‘S’ due to its unique anterior and posterior curvatures. It can appear long and slender, thick and short, or any combination due to its complex shape. It consists of spongy cancellous bone within the compact bone shell, forming a periosteal collar. It is the only membranous bone outside the skull and is uniquely pierced through-and-through by the Supraclavicular Nerve (SCN) [12]. Thus, it is also referred to as dermal bone. It follows the “rule of two,” i.e., two in number, having two primary ossification centers, two borders, two curvatures, two ends, two surfaces, and two articulations/joints. (Figure 1A).
• Two primary ossification centers: The clavicle is the first bone to begin the ossification process during the development of the embryo (5th-6th weeks of gestation) and one of the last bones to finish ossification (21-25 years of age).
• Two borders: The anterior and the posterior borders give origin to the deltoid muscle and insertion to the trapezius muscle in the lateral 1/3rd, respectively.
• Two curvatures: The anterior curvature in the medial 2/3rd and the posterior curvature in the lateral 1/3rd of the clavicle.
• Two ends: The lateral acromial end is broad, flat, and formed by intramembranous ossification. The medial sternal end is round, pyramidal-like, and formed by endochondral ossification.
• Two surfaces:
1. Superior surface: It has a smooth appearance bearing the acromial facet at the acromial end to form an acromioclavicular joint. The superior surface of the medial 2/3rd of the clavicle gives origin to the clavicular head of the sternocleidomastoid. It is covered by platysma muscle under which the supraclavicular nerves lie, providing sensory innervation to the overlying skin.
2. Inferior surface: It is rough, with many prominent lines formed due to muscles and ligamentous attachment. It has three bony landmarks: the sternal facet forming the sternoclavicular joint, the costal tuberosity for the costoclavicular, and the conoid tubercle for conoid ligaments attachments.
• Two Articulations/Joints: It is also called a ‘double plane joint’ as a layer of articular cartilage separates two joint cavities.
1. Acromioclavicular (AC) joint is a plane synovial joint formed by the acromial end of the clavicle and the acromion of the scapula, connected by the acromioclavicular ligament. It supports the function of muscles that move the clavicle.
2. Sternoclavicular joint is a saddle-type synovial joint formed by the sternal end of the clavicle and the manubrium sterni, joined by sternoclavicular ligaments, anterior and posterior interclavicular ligaments. The anterior interclavicular ligament prevents clavicle dislocation upon shoulder depression, whereas the posterior interclavicular (costoclavicular) ligament prevents clavicle dislocation upon shoulder elevation. Primarily, it allows elevation and depression of the shoulder joint. Blood supply to the clavicle is mainly derived from the thoracoacromial and suprascapular arteries, and rarely from the internal mammary artery. There is a rich blood supply in the middle third and no supply on the posterior or inferior surfaces, leading to an increased risk of nonunion in high-energy midshaft fractures. The detailed innervation of the clavicle is discussed in the later section of this article.
Variations
• Males have longer and more massive clavicles than females.
• The right clavicle is usually stronger and shorter than the left clavicle [13,14].
• An autosomal dominant congenital disability like cleidocranial dysplasia is associated with a partly or completely absent clavicle.
The levator claviculae muscle is present in 2–3% of people. It originates from the upper cervical vertebrae’s transverse processes and inserts over the lateral half of the clavicle [15, 16].
Functions of the clavicle [17]
• Adaptation to perform tasks: The well-developed clavicles and scapulae in humans and other brachiating mammals are an adaptation to perform tasks using hands well away from the body and climb, swing and grasp distant objects.
• Acts as a strut: The clavicle helps to position the arm away from the trunk by providing a stable strut between the arm and the axial skeleton. It allows the muscles to generate adequate power to perform reaching and elevation tasks.
• Scapular rotation: Out of the total 60° rotation of the scapula during the abduction of the arm, 30° comes purely from the lateral clavicle, and the remaining 30° comes from angulation of the whole clavicle and scapula together at the sternoclavicular joint.
Fascias related to the clavicle (Figure 1C)
Deltoid fascia: It is a fibrous membrane over the outer aspect of the deltoid muscle. Superiorly, it is attached to the clavicle, acromion, and the crest of the scapular spine. Inferiorly, it is continuous with the brachial fascia of the arm. Posteriorly, it is continuous with the posterior infraspinatus fascia. Anteriorly, it unifies with the pectoral fascia at its frontal-most edge.
Pectoral fascia: It is a thin layer of fascia covering the pectoralis major muscle. It is attached medially to the sternum superiorly to the clavicle, and inferolaterally, it is continuous with the fascia of the thorax, shoulder, and axilla. At its most lateral section, it forms the floor of the axilla as the axillary fascia.
Axillary fascia: The classic bowl-like appearance of the armpit results primarily via the action of axillary fascia in tethering the skin to the floor of the axilla. It is frequently referred to as the suspensory ligament of the axilla. In females, it is pierced by the tail of the breast (aka the tail of Spence). This fascia surrounds the latissimus dorsi muscle laterally and envelops the pectoralis minor muscle medially before becoming the clavipectoral fascia at the upper edge of it.
Clavipectoral fascia: The clavipectoral fascia is a strong fascia situated posterior to the clavicular part of the pectoralis major muscle. It extends superiorly from the clavicle, medially from the costochondral joints, and superolaterally from the coracoid process. Inferiorly, it converges in the axilla, where it acts as a protective structure over the neurovascular structure of the axilla. It lies between the pectoralis minor and subclavius muscles, protecting the axillary nerve and vessels. Superiorly, it splits to enclose the subclavius muscle before attaching to the clavicle. Its posterior layer fuses with the deep cervical fascia, which connects the omohyoid muscle to the clavicle. Medially, it is attached to the first rib before blending with the fascia over the first two intercostal spaces. Laterally, it is attached to the coracoid process before blending with the coracoclavicular ligament. The fascia often thickens to form a whiter and denser band, the costocoracoid ligament/membrane, between the first rib and coracoid process. Inferiorly, the fascia becomes thin, splits around pectoralis minor, and descends to blend with the axillary fascia and laterally with the fascia over the short head of biceps. It is pierced by CALL [cephalic vein, artery (thoracoacromial), lateral pectoral nerve, lymphatics]. The clavipectoral fascia completely surrounds the clavicle, and the nerve endings of the clavicle penetrate this fascia [18].
Clavicle fractures
Incidence
• Clavicle fractures represent 5-10% of all fractures [19] and account for 35% of scapular girdle injuries [20].
• There is a bimodal distribution of the clavicle fractures, with the two peaks being younger men (due to sports injury) and patients older than 55 years of age (due to osteoporosis and fall) [21].
• Clavicle fractures are prevalent injuries in adults (2-5%) and children (10-15%) [22] and represent 44-66% of all shoulder fractures [23].
Mechanism:
• Clavicle fractures are often caused by a direct impact on the outer aspect of the shoulder, typically from a fall, injury and trauma in motor vehicle accidents or sports.
• Clavicle fractures represent 95% of fractures seen during childbirth while passing through the birth canal [24].
• It can easily be fractured due to impact to the shoulder from the force of falling on outstretched arms or by a direct hit [25].
Classification
Allman classification system [26] is based on the anatomical location of the fracture, as shown in Figure 1B.
A. Type I involves the middle third of the clavicle, which constitutes around 75% of all clavicular fractures. Being the region with the narrowest cross-sectional diameter and lack of muscular and ligamentous attachment, the middle third of the clavicle becomes more vulnerable to the bending movements exerted by the structures attached. They are generally stable but may be associated with significant deformity.
B. Type II involves the lateral third of the clavicle and constitutes around 20% of all clavicular fractures. They are more common in elderly patients or those with co-morbidities, although they do occur in all age groups. When displaced, these types are often unstable.
C. Type III involves the medial third of the clavicle and constituting around 5% of all clavicular fractures. It is commonly associated with multi-system polytrauma. It can be associated with neurovascular compromise, pneumothorax, or hemothorax.
Associated injuries
Neurovascular injury
a) Type I fractures are associated with injury to the SCN (intermediate branch), which pierces the clavicle in 1% to 4% of the population and innervates the proximal half of the clavicle [27].
b) The ulnar nerve is the most commonly injured peripheral nerve in clavicle fractures as it is close to the middle and medial third junction.
c) The brachial plexus lies as close as 12 mm from the medial end of the clavicle [28]. Thus, direct injury to the vessels and brachial plexus can occur at the time of fracture or iatrogenically during surgery with 0-15% incidence [29,30].
d) Vascular injury (due to fracture or surgery) leads to arteriovenous fistula formation, pseudoaneurysm, or air embolism.
Polytrauma: Type III fractures are associated with multi-system polytrauma with neurovascular compromise, pneumothorax, or hemothorax.
Management
Most clavicle fractures can be treated conservatively as most of them with significant deformity (>90%) unite despite displacement. Conservative treatment options include using a sling, ‘figure-of-eight’ bandage, and a well-supported elbow to improve the deformity. Early movement of the shoulder joint is recommended to prevent the development of a frozen shoulder. Medial clavicle fractures need to be considered in the broader context of associated injury, such as traumatic lung injury, and managed accordingly. Surgical intervention is mainly needed in open comminuted fractures, significantly shortened fractures, and bilateral fractures to permit weight-bearing. An open reduction and internal fixation will be necessary for fracture nonunion, usually performed at 2-3 months post-injury.
Types of clavicle surgery
The standard surgical options of clavicle fractures include open reduction and plate fixation, intramedullary fixation (TENS nailing, Steinman pin application), tension band wiring mainly for AC joint disruption or lateral end fracture, simple screw fixation for less displaced fractures, and implant removal. All open surgeries involve incision along the fracture line, whereas closed surgeries (intramedullary fixation) typically use a smaller incision, usually away from the fracture site. Closed surgeries cause fewer disturbances to the surrounding soft tissues. Clavicle surgeries are mainly done in a supine or modified beach-chair position, which is relatively comfortable for all patients. Many centers prefer GA with or without RA due to complex innervations and lack of available literature about the most suitable techniques.
RA techniques for clavicle surgeries
The pain generating structures in clavicle surgeries include the skin over the incision area and richly innervated periosteum. So, the planned RA technique should cover all the innervations of these pain generators. Due to the complex innervation of the clavicle, a 3-step algorithmic approach, ‘Identify-Select-Combine’ [31] can be applied to determine the most suitable procedure-specific RA option.
Identifying target nerves for clavicle surgery
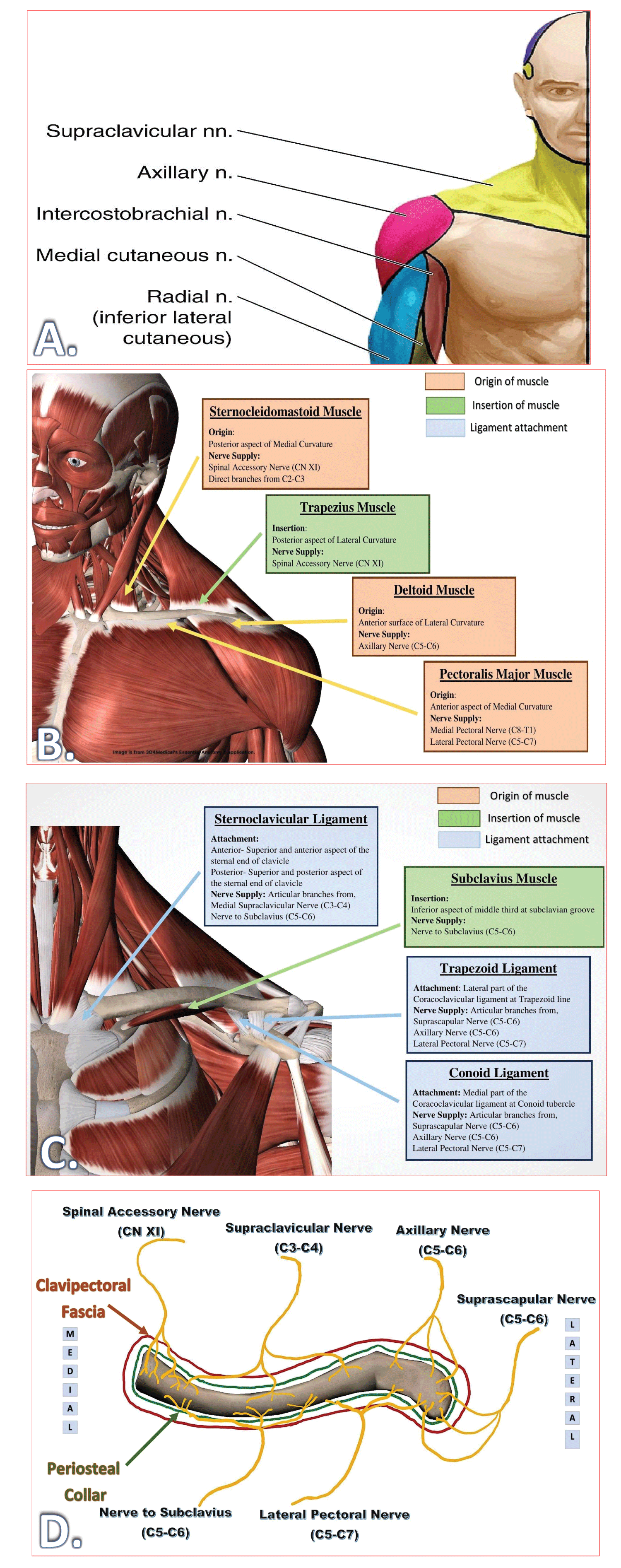
The clavicle derives its sensory innervation from the cervical plexus and the brachial plexus. Due to the superficial and anterior location of the clavicle, all the innervations come from the anterior rami of the spinal nerves (C3-C7) without any contribution from the posterior rami. The clavicle receives its innervation from the nerves lying in the vicinity, either supplying skin, muscles, joints, or ligaments. The anterosuperior portion of the clavicle is bare and lies directly under the skin and subcutaneous tissue. The cutaneous branches supplying skin over the clavicle, i.e., supraclavicular nerves, also supply the clavicle at different levels. The procedure-specific RA option should cover all essential innervations of skin (dermatomes), muscles (myotomes), and bone (osteotomes) of the clavicle (Figure 2) as per the surgery involved.
The sensory innervation of the clavicle and the overlying skin is not clearly identified, and it varies depending on the source between C3 and C6 [4,32-34]. The C3-C5 roots contribute to the dermatomal innervations, whereas the C3-C7 roots contribute to the myotomal and osteotomal innervations. Four muscles arise from, and two muscles insert into the clavicle, as shown in Table 1.
The periosteum of any bone is richly innervated by the nerve fibers that stem from different sources [33] like terminal branches of motor nerves (‘Muscle-Areas’ of periosteum) and joint nerves (‘Capsule-Adjacent-Areas’), branches of cutaneous nerves (‘Muscle-Free-Areas’), and branches of nerves following nutrient arteries (‘Nutrient-Foramina-Areas’). Likewise, the osteotomal innervation [34] of the clavicle includes,
1. “Muscle-Area”: Subclavian nerve (subclavius), spinal accessory nerve and trapezius branch of cervical plexus (trapezius), and lateral pectoral nerve (pectoralis major).
2. Capsule-Adjacent-Area: Suprascapular nerve (AC joint).
3. ‘Muscle-free-Areas’: Medial and Intermediate supraclavicular nerves (anterior and superior area).
4. ‘Nutrient-Foramina-Areas’: Lateral pectoral nerve.
The acromioclavicular joint is innervated by the suprascapular nerve (C5-C6) and lateral pectoral nerve (C5-C7). The sternoclavicular joint is innervated by the medial SCN (C3-C4) in the superficial part and the nerve to subclavius (C5-C6) in the deeper part.
The target nerves to cover dermatomes, myotomes, and osteotomes of the surgical areas are shown in Table 2.
Selecting procedure-specific target blocks
A procedure-specific approach should be applied to target specific nerves as per the surgical steps to involve the innervation (Table 3) of all the pain generating components. Since all nerves supplying the clavicle enters the clavipectoral fascia surrounding it, it is possible to block these nerves by depositing drug between this fascia and the periosteal collar. Such a fascial plane block is a relatively simple and safe option available for awake clavicle surgeries.
The target blocks, which can include all selected target nerves, are as follows:
A. Plexus blocks
• Interscalene block
• Superficial cervical plexus block
• Selective superior trunk block [35]
• Selective supraclavicular nerve block [36].
B. Fascial plane block
• Clavipectoral fascial plane block
Combining selected target blocks
After selecting all the target blocks, the following combinations can be considered as per the patient’s suitability and the surgery involved.
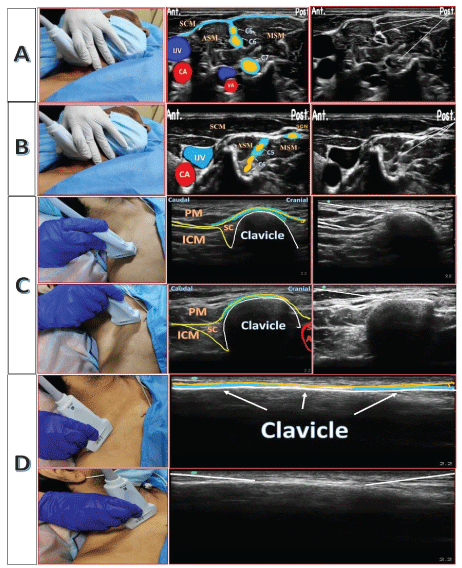
A. Single-injection Approach (SIA): (Figure 3A, B)
• Interscalene block + superficial cervical plexus
• Selective superior trunk block + selective supraclavicular nerve block
B. Dual-injection Approach (DIA): (Figure 3C, D)
• Clavipectoral fascial plane block
C. Triple-injection Approach (TIA)
• Modified clavipectoral fascial plane block
Although the most common RA technique used in clavicle surgery is interscalene block [2], it is not without its undesirable effects or complications, such as phrenic nerve palsy, recurrent laryngeal nerve block, Horner syndrome, total spinal anesthesia, and cardio/neurotoxicity [37,38]. Furthermore, interscalene blockade now has one of the highest rates of post-blockade nerve dysfunction, with an incidence ranging from 3% to 10% [38]. The combination of superficial and deep cervical plexus block [4] is also associated with unwanted side effects. The cervical plexus block is given mainly to target the SCN. However, the complications associated with the entire cervical plexus blockade can be avoided by targeting the SCN selectively under ultrasound guidance.
Attention has shifted to safer and simpler options like a fascial plane block to avoid such side effects and complications. Before discussing the fascial plane block for clavicle surgery, it is essential to know different fascias related to the clavicle (Figure1 C) to understand the spread of drugs around the clavicle and neural structures.
Clavipectoral fascial plane block [8-11,39-42]
The CPB was first described in 2017 by Valdés [39] as a simple and highly safe procedure for anesthesia and analgesia for clavicle surgeries. With this distinct advantage and its analgesic effectiveness for clavicle surgery, CPB may be an alternative to ISB. CPB can be given under ultrasound guidance or using a simple landmark technique. This block aims to create a field block around the clavicle and involves all neural structures innervating the clavicle. For that, the local anesthetic drug has to be deposited on the medial and lateral third of the clavicle between the fascia around (clavipectoral fascia) and the periosteum of the clavicle (periosteal collar). The deposited drug surrounds the clavicle, involving all the nerves piercing the fascia to enter into the clavicle.
The success of the fascial plane block depends on the integrity of the fascia and the potentiality of the interfascial plane. The integrity of the fascia may be lost due to the disruption of fascias and soft tissues during injury and surgical procedure. In the case of displaced or comminuted fractures, the potentiality of the interfascial plane may be lost due to the possible breach in the continuity of the fascia around the clavicle over the fracture site. Thus, the deposited drug may not spread entirely around the clavicle. An additional injection over the periosteum of the clavicle at the fracture site (like “hematoma block”) [43,44] may improve the quality of the block. Also, the skin over the clavicle can be included by giving an additional infiltration in the subcutaneous plane over the clavicle. This modification of the CPB is required to cover all necessary innervations and avoid sparing.
The post-traumatic or post-surgical healing process [45,46] involves the formation of fibrosis, scar tissues, and multiple adhesions around the bone. This disrupts the typical myofascial plane architecture, leading to loss of potentiality of the space between the fascia and periosteum of the bone. These changes may cause an inadequate drug spread around the clavicle, causing the possibility of patchy, partial, or failed blocks. Extrapolating from this hypothesis, the CPB may not be entirely effective in cases of revision surgery, implant removal surgery, or when the time between trauma and surgery is delayed. Thus, such conditions may make CPB a secondary choice over other available choices. However, there is a lack of literature support comparing one block over others. The comparison of essential RA techniques used in clavicle surgery is shown in Table 4 and their choices as per the type of surgery are shown in Table 5.
The CPB requires further discussion and studies to address the following concerns:
1. Hyperalgesia and pain perceptions: The analgesic efficacy of CPB may get affected due to primary hyperalgesia in the damaged tissues, leading to a change in pain perception, which has to be studied further.
2. Change in pH: After the injury, local tissue inflammation causes a change in the pH, altering the local anesthetic effect.
3. Effect of myofascial plane disruption and loss of potentiality on the success of the block.
Summary
The RA choice for clavicle surgery depends on the knowledge of surgical steps, the innervation of the various involved structures, and the comfort level of the patient and surgeon. Knowledge of associated injuries will help refine the proposed anesthesia plan to improve the patient’s comfort. The fractures or incisions involving the medial end can be tackled with local anesthetic infiltration over the skin and periosteal collar. The fascial plane block is a newer but promising motor-sparing, phrenic-sparing, and procedure-specific option for clavicle surgeries. However, CPB is insufficient to provide analgesia for associated scapula fracture, making the patient uncomfortable while undergoing surgery. Other options like ISB with SCN block can be considered for such associated fractures as it covers most of the scapular innervations. CPB can be considered the first choice only for acute trauma surgeries of the clavicle. Other suitable RA options need to be considered for chronic trauma surgeries, revision surgeries, nonunion/malunion surgeries after the complete healing process, and implant removal surgeries.
Using the novel “Identify-Select-Combine” approach, a procedure-specific RA technique for a complexly innervated structure like a clavicle can be planned. There is still much to explore in the field of RA for clavicular surgery.
We thank Dr. Dheenadhayalan J., Senior Consultant, Orthopedics and Traumatology, for sharing surgical information and radiological images. We also thank 3D4Medical from Elsevier for granting permission to use and modify images from the Essential Anatomy Application.
Contributorship statement
KS: Designed this algorithmic strategy for complexly innervated structures like clavicle. With the guidance and approval of JB and PG, formulate a possible combination of blocks. Involved in reference collection and sorting work with the help of HD. Designed manuscript content and co-wrote the paper. Took the lead in manuscript writing and illustrations compilation.
HD: Involved in the anatomical description and information collection required for the manuscript writing. Co-wrote and proofread the manuscript.
JB: Approved idea by KS and provided scientific guidance for manuscript writing. Guided the content of the manuscript and Co-wrote the paper. Approved final version of the manuscript.
PG: Approved idea by KS and provided scientific guidance for manuscript writing.
All authors provided critical feedback and helped shape the manuscript.
- Ropars M, Thomazeau H, Huten D (2017) Clavicle fractures. Orthop Traumatol Surg Res 103: S53-S59. Link: https://bit.ly/3sYBu4K
- Brull R, McCartney CJL, Sawyer RJ, von Schroeder HP (2004) The indications and applications of interscalene brachial plexus block for surgery about the shoulder. Acute Pain 6: 57-77. Link: https://bit.ly/3dFJD7N
- Banerjee S, Acharya R, Sriramka B (2019) Ultrasound-Guided Inter-scalene Brachial Plexus Block with Superficial Cervical Plexus Block Compared with General Anesthesia in Patients Undergoing Clavicular Surgery: A Comparative Analysis. Anesth Essays Res 13: 149–154. Link: https://bit.ly/3rSi4gl
- Choi DS, Atchabahian A, Brown AR (2005) Cervical plexus block provides postoperative analgesia after clavicle surgery. Anesth Analg 100: 1542–1543. Link: https://bit.ly/2Q482vm
- Pinto L, Silva C, Gonçalves P, Valadares RJ (2019) Bloqueio do nervo supraclavicular e do tronco superior para tratamento cirúrgico de fratura de clavícula em paciente portador de doença de Steinert – Relato de caso [Supraclavicular nerve and superior trunk block for surgical treatment of clavicle fracture in a patient with Steinert's disease - Case report. Rev Bras Anestesiol 69: 99–103. Link: https://bit.ly/3rRcnPS
- Sanllorente-Sebastián R, Wilk P, Garcés-Pérez GM, Arias-Rodríguez L, Andrés-Pedrosa M, et al. (2020) Awake clavicle surgery with PECS1 and ultrasound selective supraclavicular nerve block combination. J Clin Anesth 66: 109937. Link: https://bit.ly/3urLd3K
- Schuitemaker RJB, Sala-Blanch X, Rodriguez-Pérez CL, Mayoral RJT, López-Pantaleon LA, et al. (2018) The PECS II block as a major analgesic component for clavicle operations: A description of 7 case reports. Bloqueo PEC II como componente mayor analgésico para operaciones de clavícula: descripción de 7 casos y revisión de la literatura. Rev Esp Anestesiol Reanim 65: 53–58. Link: https://bit.ly/2PXJTqp
- Ince I, Kilicaslan A, Roques V, Elsharkawy H, Valdes L (2019) Ultrasound-guided clavipectoral fascial plane block in a patient undergoing clavicular surgery. J Clin Anesth 58: 125-127. Link: https://bit.ly/3fTm8uv .
- Ueshima H, Ishihara T, Hosokawa M, Otake H (2020) Clavipectoral fascial plane block in a patient with dual antiplatelet therapy undergoing emergent clavicular surgery. J Clin Anesth 61: 109648. Link: https://bit.ly/3uvrXCE .
- Yoshimura M, Morimoto Y (2020) Use of clavipectoral fascial plane block for clavicle fracture: Two case reports. Saudi J Anaesth 14: 284–285. Link: https://bit.ly/3sSbjwt .
- Atalay YO, Mursel E, Ciftci B, Iptec G (2019) Clavipectoral Fascia Plane Block for Analgesia after Clavicle Surgery. Bloqueo del plano de la fascia clavipectoral para analgesia tras cirugía de clavícula. Rev Esp Anestesiol Reanim 66: 562–563. Link: https://bit.ly/3cVE5GY
- de la Caffinière JY, Konsbruck R (1979) Trajet anormal transclaviculaire d'une branche des nerfs supraclaviculaires (foramen nervi supraclavicularis) (à propos d'un cas) [Abnormal transclavicular course of a branch of the supraclavicular nerve (foramen nervi supraclavicularis) (one case) (author's transl)]. Chirurgie pediatrique 20: 379–381.
- Moore Keith L, Dalley Arthur F (1999) Clinically Oriented Anatomy (4th ed.). Lippincott Williams & Wilkins.
- Bernat A, Huysmans T, Van Glabbeek F, Sijbers J, Gielen J, Van Tongel A (2014) The anatomy of the clavicle: a three-dimensional cadaveric study. Clinical Anatomy (New York, N.Y.) 27: 712-723. Link: https://bit.ly/3wIknqf
- Natsis K, Apostolidis S, Nikolaidou E, Noussios G, Totlis T, Lazaridis N (2009) Levator claviculae muscle: a case report. Cases Journal 2: 6712. Link: https://bit.ly/3dKtz4m
- Odate T, Kawai M, Iio K, Funayama S, Futamata H, et al. (2012) Anatomy of the levator claviculae, with an overview and a literature survey. Anat Sci Int 87: 203–211. Link: https://bit.ly/2PYsSMO
- Britannica T Editors of Encyclopaedia (2020) Clavicle. Encyclopedia Britannica. Link: https://bit.ly/2Q4lBex
- Drake R, Vogl AW (2014) A. Mitchell Gray’s anatomy for students (4th ed.), Churchill Livingstone/Elsevier, Edinburgh.
- Robinson CM (1998) Fractures of the clavicle in the adult. Epidemiology and classification. J Bone Joint Surg Br 80: 476–484. Link: https://bit.ly/3fMejXp
- Tran DQ, Tiyaprasertkul W, González AP (2013) Analgesia for clavicular fracture and surgery: a call for evidence. Reg Anesth Pain Med 38: 539–543. Link: https://bit.ly/2Q73ODa
- Wiesel B, Nagda S, Mehta S, Churchill R (2018) Management of Midshaft Clavicle Fractures in Adults. J Am Acad Orthop Surg Glob Res Rev 26: e468–e476. Link: https://bit.ly/3wB9A0D
- van der Meijden OA, Gaskill TR, Millett PJ (2012) Treatment of clavicle fractures: current concepts review. J Shoulder Elbow Surg 21: 423-429. Link: https://bit.ly/3muZolN
- Toogood P, Horst P, Samagh S, Feeley BT (2011) Clavicle fractures: a review of the literature and update on treatment. The Phys Sportsmed 39: 142-150. Link: https://bit.ly/31PmQRo
- Hughes K, Kimpton J, Wei R, Williamson M, Yeo A, et al. (2018) Clavicle fracture nonunion in the paediatric population: a systematic review of the literature. J Child Orthop 12: 2-8. Link: https://bit.ly/3sTcAmW
- Landin LA (1983) Fracture patterns in children. Analysis of 8,682 fractures with special reference to incidence, etiology and secular changes in a Swedish urban population 1950-1979. Acta Orthop Scand Suppl 202: 1-109. Link: https://bit.ly/2PKJKqq
- Allman FL (1967) Fractures and ligamentous injuries of the clavicle and its articulation. J Bone Joint Surg Am 49: 774-784. Link: https://bit.ly/3sXYO2u
- Tubbs RS, Salter EG, Oakes WJ (2006) Anomaly of the supraclavicular nerve: case report and review of the literature. Clin Anat (New York, N.Y.) 19: 599–601. Link: https://bit.ly/3sY88U5
- Lo EY, Eastman J, Tseng S, Lee MA, Yoo BJ (2010) Neurovascular risks of anteroinferior clavicular plating. Orthopedic 33: 21. Link: https://bit.ly/3dG5Pyy
- Tse DH, Slabaugh PB, Carlson PA (1980) Injury to the axillary artery by a closed fracture of the clavicle. A case report. J Bone Joint Surg 62: 1372–1374. Link: https://bit.ly/3wA8EKg
- Wijdicks FJ, Van der Meijden OA, Millett PJ, Verleisdonk EJ, Houwert RM (2012) Systematic review of the complications of plate fixation of clavicle fractures. Arch Orthop Trauma Surg 132: 617-625. Link: https://bit.ly/3moJ8Tx
- Sonawane K, Balavenkatasubramanian J, Dixit H, Tayi H, Goel VK (2021) Regional anesthesia for scapular fracture surgery: an educational review of anatomy and techniques. Reg Anesth Pain Med 46: 344-349. Link: https://bit.ly/3fN2C2T
- Balaban O, Dülgeroğlu TC, Aydın T (2018) Ultrasound-Guided Combined Interscalene-Cervical Plexus Block for Surgical Anesthesia in Clavicular Fractures: A Retrospective Observational Study. Anesthesiol Res Pract 7842128. https://bit.ly/2Q0Uh0z
- Grant JCB (1948) in Method of Anatomy, Toronto.
- Moriggl B (2019) ESRA19-0712 Clavicle innervation and implications for regional anaesthesia Reg Anesth Pain Med 44: A63-A64.
- Gurumoorthi P, Mistry T, Sonawane KB, Balasubramanian S (2019) Ultrasound guided selective upper trunk block for clavicle surgery. Saudi J Anaesth 13: 394–395. Link: https://bit.ly/3myT2lC
- Valdés-Vilches LF, Sánchez-del Águila MJ (2014) Anesthesia for clavicular fracture: selective supraclavicular nerve block is the key. Reg Anesth Pain Med 39: 258–259. Link: https://bit.ly/3mrTa67
- Bilbao Ares A, Sabaté A, Porteiro L, Ibáñez B, Koo M, et al. (2013) Complicaciones neurológicas asociadas a bloqueos interescalénico y supraclavicular guiados con ecografía en cirugía electiva de hombro y extremidad superior. Estudio observacional prospectivo en un hospital universitario [Neurological complications associated with ultrasound-guided interscalene and supraclavicular block in elective surgery of the shoulder and arm. Prospective observational study in a university hospital]. Rev Esp Anestesiol Reanim 60: 384–391. Link: https://bit.ly/3cUolUI
- Auroy Y, Benhamou D, Bargues L, Ecoffey C, Falissard B, et al. (2002). Major complications of regional anesthesia in France: The SOS Regional Anesthesia Hotline Service. Anesthesiol 97: 1274-1280. Link: https://bit.ly/3fQl9uX
- Valdés L (2017) As part of the lecture: analgesia for clavicular surgery/fractures 36th annual ESRA Congress, Lugano, Switzerland.
- Atalay YO, Ciftci B, Ekinci M, Yesiltas S (2020) The effectiveness of clavipectoral fascia plane block for analgesia after clavicle surgery: a report of five cases. Minerva Anestesiol 86: 992–993. Link: https://bit.ly/31VgsI9
- Kukreja P, Davis CJ, MacBeth L, Feinstein J, Kalagara H (2020) Ultrasound-Guided Clavipectoral Fascial Plane Block for Surgery Involving the Clavicle: A Case Series. Cureus 12: e9072. Link: https://bit.ly/3s3j1mo
- Escolar VE (2020) Clavipectoral fascial plane block (CPB) for clavicle surgery. Link: https://bit.ly/39Nycti
- Ogunlade SO, Omololu AB, Alonge TO, Salawu SA, Bamgboye EA (2002) Haematoma block in reduction of distal radial fractures. West Afr J Med 21: 282–285. Link: https://bit.ly/3uvrYGs
- Tseng P, Leu T, Chen Y, et al. (2018) Hematoma block or procedural sedation and analgesia, which is the most effective method of anesthesia in reduction of displaced distal radius fracture?. J Orthop Surg Res 13: 62. Link: https://bit.ly/3rXobjx
- Olmarker K (2010) Reduction of adhesion formation and promotion of wound healing after laminectomy by pharmacological inhibition of pro-inflammatory cytokines: an experimental study in the rat. European spine Journal: official publication of the European Spine Society, the European Spinal Deformity Society, and the European Section of the Cervical Spine Research Society 19: 2117–2121. Link: https://bit.ly/2Ov5B4M .
- Hoffeberg H (2020) Whiplash Injuries in Motor Vehicle Accidents. 2. Link: https://bit.ly/31QwJxZ
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
