Open Journal of Orthopedics and Rheumatology
Treatment of Trans-Scaphoid Perilunate Injuries of the Wrist using a Nitinol Staple for Fixation
Alec J Talsania1*, Christine B Novak2 and Miguel A Pirela-Cruz3
2PhD, Department of Surgery, University of Toronto, Toronto. ON, USA
3MD, F.A.C.S., Professor. of Orthopedic Surgery, Texas Tech University Paul L. Foster School of Medicine. El Paso, Texas, USA
Cite this as
Talsania AJ, Novak CB, Pirela-Cruz MA (2020) Treatment of Trans-Scaphoid Perilunate Injuries of the Wrist using a Nitinol Staple for Fixation. Open J Orthop Rheumatol 5(1): 009-013. DOI: 10.17352/ojor.000021Treatment of trans-scaphoid perilunate injuries of the wrist presents a clinical challenge for patients and the treating hand surgeon. In the past, traditional treatment consisted of combined volar and dorsal approaches, repair of all of the involved ligaments, screw fixation of the scaphoid fracture, and immobilization until the scaphoid is radiographically united. We describe a volar approach that allows for decompression of the carpal tunnel, repair of the rent in the Space of Poirier, and direct internal fixation of the scaphoid fracture with a staple (scaple) that allows for early range of motion. We have used this approach in 18 patients at a Level 1 Trauma Center with satisfactory clinical outcomes.
Introduction
The efficacy of staples for treating scaphoid fractures has been well documented, however its application in perilunate injuries has not be well elucidated [1]. The purpose of this paper is to review the technique of treating perilunate fractures with a nitinol staple. We have used this technique in 18 patients to treat 19 perilunate fractures at a Level 1 Trauma Center and have obtained satisfactory clinical results.
Perilunate fracture dislocations are uncommon, but usually occur in young patients who sustain high energy trauma or falls on outstretched hands. Mayfield first described the mechanism of perilunate dislocation occurring with extension, ulnar deviation, and intercarpal supination [2]. This sequence of events leading to the injury has been described as a four-step process, starting with a radial force passing through the scaphoid causing a fracture, transmission of the force through the lunocapitate joint causing the lunate to project through the space of Poirier, dislocation of the other carpal bones around the lunate, and disruption of the lunotriquetral joint [3,4]. The lunate, however, remains attached to the short radiolunate ligament, allowing surgical access to the lunate via the carpal tunnel.
The diagnosis of this complex injury may be missed in up to 25% of the patients, and up to 50% of patients may present with acute carpal tunnel symptoms [5-7]. Early diagnosis and treatment is essential to avoid long term disability, as delayed treatment is associated with poor outcomes [5,8,9].
Treatment of perilunate fracture dislocations of the wrist is a challenging problem for patients and the hand surgeons [10,11]. Various surgical treatment options have been advocated, including a volar approach, dorsal approach, and combined approaches to address all of the injured structures on the palmar and dorsal aspects of the wrist [11-19].
One of the clinical sequelae resulting from treatment of this injury is the degree of stiffness that occurs in the fingers and wrist after prolonged immobilization following surgical repair of the bone and ligaments [20]. Many patients require extensive rehabilitation to obtain a functional range of motion after the structures are healed [21].
In our experience, a combined approach and repair of all of the involved structures, has resulted in dissatisfaction with the outcome due to the amount of time the patients require to regain function. Additionally, the limited range of motion that is finally achieved by these patients was often suboptimal for performing even basic activities of daily living [22].
The current approach described for treatment of these trans-scaphoid perilunate injuries is one that is practical and allows for stable fixation of the scaphoid fracture, reduction of the lunate, decompression of the carpal tunnel, and repair of the rent involving the palmar ligaments including the radioscaphocapitate and ulnocapitate ligaments.
Relevant anatomy
The volar surface of the scaphoid is concave, and therefore the scaphoid tends to volar flex, creating a humpback deformity. A scaphoid fracture may collapse to a humpback deformity due to shortening of the volar cortical length and can cause dorsal intercalated segment instability (DISI) [23]. Placing fixation on the palmar aspect of the scaphoid helps to prevent the humpback deformity, in essence, acting as an I-beam to counteract the deformity forces.
Intrinsic and extrinsic ligaments provide support and stability to the wrist, with the volar ligaments being more important stabilizers than the dorsal ligaments. The scapholunate ligament is one of the important volar ligaments and is the primary stabilizer of the scapholunate joint (and wrist). The space of Poirier is a weakened area of the volar wrist capsule, at the proximal capitate, between the radioscaphocapitate and the long radiolunate ligaments (Figure 1). This is an intrinsically weak region, especially with the wrist in hyperextension that allows the lunate to undergo palmar flexion and dislocation into the carpal tunnel.
Indications/Contraindications
Since the majority of trans-scaphoid perilunate fracture dislocations result from high energy injuries, such as falls from heights and motor vehicle accidents, a comprehensive evaluation for other major injuries should be performed following the ABC’s of trauma. The initial evaluation of the injured wrist should include assessment of open wounds, edema or deformity, and alignment with the forearm. An examination of the peripheral nerves, particularly the median nerve, is essential considering the high association with acute carpal tunnel syndrome [24].
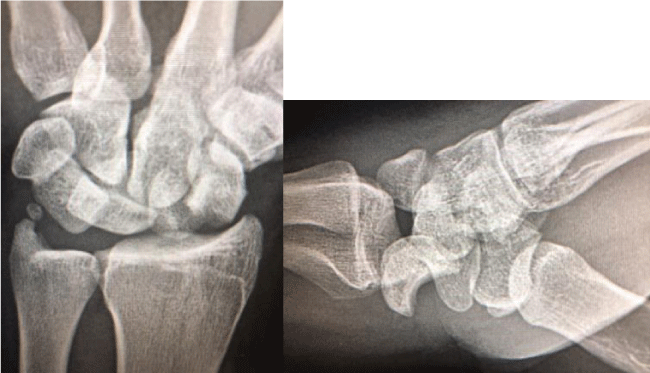
Radiographic evaluation should include a postero-anterior (PA) and true lateral views (Figure 2). On a PA view with a perilunate dislocation, the carpal height ratio will be less than 0.5 and there can be overlap of the lunate and capitate, and one may see a disruption in Gilula’s lines (Figure 3). The pie in the sky sign may also be visualized on the PA view, which is a triangular appearance of the lunate due to its palmar flexed posture. On the lateral view with a perilunate injury, the lunate may or may not be positioned in the lunate fossa colinear with the radius, depending on the stage of the dislocation (Figure 4).
Early reduction is essential to reduce pressure on the median nerve and surrounding soft tissues. Factors that have been shown to influence outcomes include open injury, delay in diagnosis and treatment, and non-anatomical reduction [5].
Non-operative treatment includes closed reduction and casting [25]. Bagheri et. al showed higher Mayo wrist scores and greater range of motion in operative management over non-operative management [26]. The goal of operative management is to achieve early mobilization and allow for a quick return of functional use of the hand.
The primary indication for performing this technique was mid-waist fracture of the scaphoid. Proximal pole and distal pole fractures were excluded since they cannot accommodate a staple due to the limited amount of space. Furthermore, a prerequisite for using a staple for mid-waist fractures of the scaphoid is at least three millimeters (mm) of bone on each side of the fracture site. If there is a potential for impingement of the staple against the lip of the radius, then a trough is made that allows for the staple to be recessed in the bone and prevent impingement or electively plan for staple removal once union has occurred. In cases of fracture comminution (radial or dorsal sides of the scaphoid) supplemental bone graft may be needed. Additionally, supplemental bone graft may be added at the fracture site prior to the insertion of the staple if needed.
Technique
Setup: The patient is placed in a supine position with the operative extremity on a hand table. Regional or general anesthesia is provided. Appropriate perioperative antibiotics are administered. Surgery is performed under tourniquet control. The extremity is prepped and draped in a normal fashion. The surgeon is seated on the ulnar side of the hand. Towels are placed under the wrist in a supine position to allow for wrist extension.
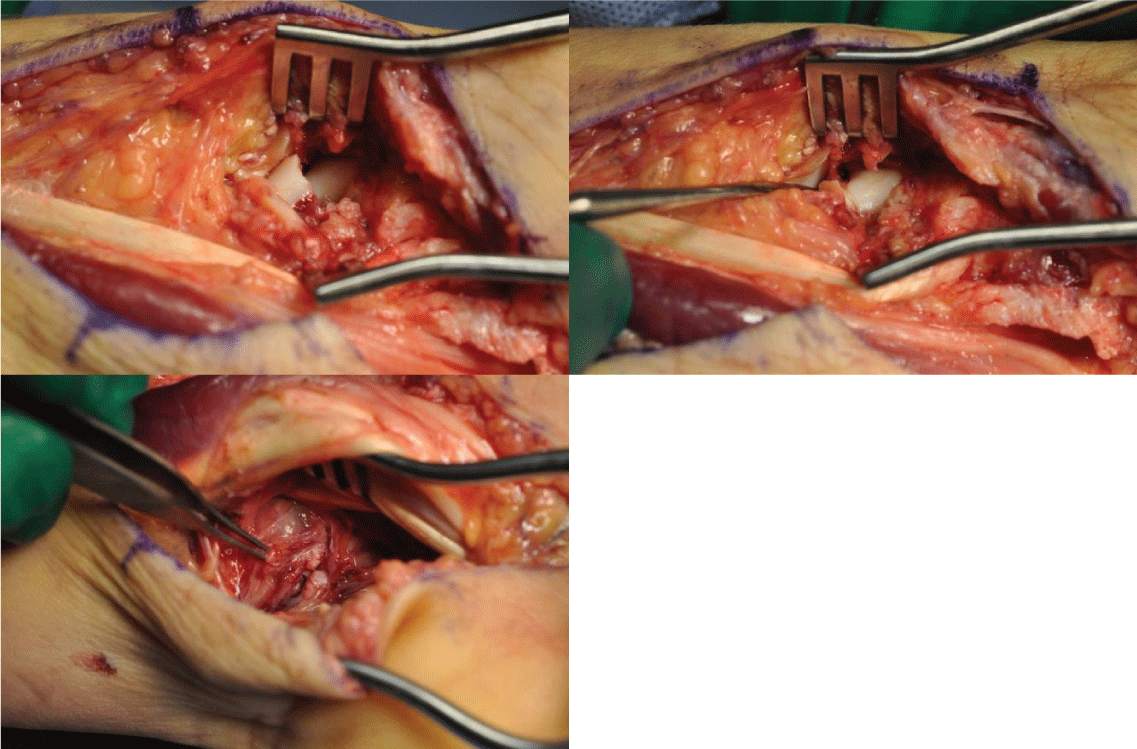
Incision: The incision provides access for open reduction and internal fixation of the scaphoid, as well as decompression of the carpal tunnel and repair of the rent in the space of Poirier.The incision begins in the distal forearm and follows a course between the flexor carpi radialis (FCR) tendon and the palmaris longus (PL) tendon until approximately one centimeter (cm) proximal to the flexor crease of the wrist (Figure 5). A sharp radial turn is made, and the incision extends towards the base of the thumb until the flexor crease.From the flexor crease, another turn is made back to the midline of the palm, ending one centimeter (cm) distal to the flexor crease of the wrist. The last turn is made at the palmar midline region and is extended distally to allow for decompression of the carpal tunnel and repair of the rent located on the floor of the tunnel. The large incision is required to gain access to the volar ligaments. Care is taken to protect all the critical structures in this region including the radial artery and the palmar cutaneous branch of the median nerve.
Volar ligaments: The radiocarpal ligaments (radioscaphocapitate and the long radiolunate ligaments) are incised using a method that allows for easy repair after fixation of the scaphoid. Failure to repair the palmar ligaments can contribute to additional instability of the carpus with ulnar translation [27].
Scaphoid fixation (Repair): Many different implants have been advocated for internal fixation of the scaphoid fracture, such as Kirschner wires, Acutrak screws, and plate fixation. We have found the Nitinol staple to be a reasonable implant for fixation of the mid-waist scaphoid fracture (Nitinol Staple, DePuy-Synthes, West Chester, PA).The nitinol staple has the following advantages:
1. Ease of insertion
2. Constant compression at the fracture site
3. The ability of the staple to prevent the palmar flexion at the fracture site (i.e., humpback deformity) when placed on the volar surface of the scaphoid
4. Surgery is performed under direct vision to visualize the fracture site and the implant (Figure 6).
Closure: Volar ligaments are repaired on the way out with non-absorbable sutures. Tourniquet is released. Hemostasis is achieved, and skin is closed with 4-0 Nylon. A post-operative dressing is applied with a short arm thumb spica to immobilize the wrist and thumb.
Postoperative management and rehabilitation
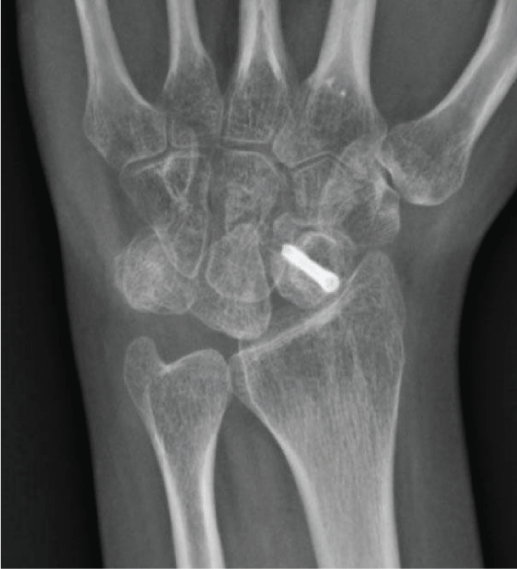
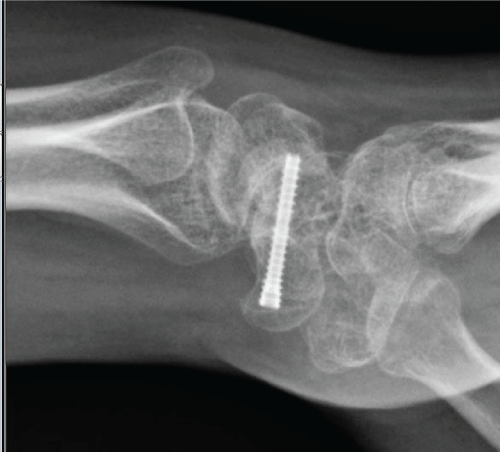
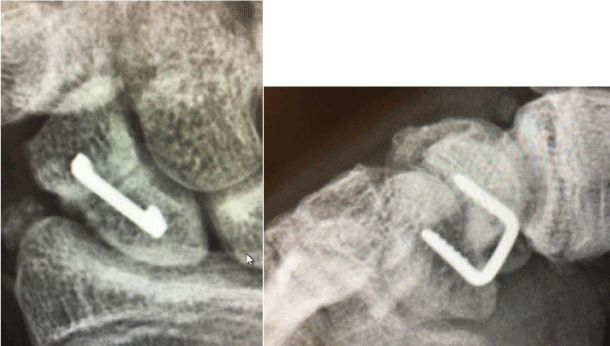
Rehabilitation: Patients return in 10-14 days following surgery for removal of the post-operative dressing, wound check, and radiographs (Figure 7). A short arm thumb spica cast is applied for an additional 3-4 weeks. Patients are encouraged to move shoulder, elbow, forearm and fingers (Figure 8). A CT scan is obtained at 3 months following the surgery. Patient works on range of motion of the fingers and wrist in therapy, as well as modalities for pain (Figure 9). We use a conventional push-up as a good indicator of clinical union (Figure 10).
Those with scapholunate advanced collaspsed (SLAC) or scapholunate nonunion advanced collapse (SNAC) wrist tend to avoid this motion by modifying their push-ups with a closed fist or by performing them on their fingertips.
Expected outcomes and complications
The single volar approach has allowed for earlier mobilization and decreased stiffness over the combined dorsal and volar approach. The volar approach also allows for easier repair of the more important stabilizing ligaments of the wrist, as well as release of the carpal tunnel compared to the dorsal approach. Although this repair requires a large incision, we have not seen complications due to large incision size, including restenosis of the carpal tunnel in our experience. Volar operative approach is also less disruptive of the blood flow to the proximal pole of the scaphoid. Performing the surgery with the staple (scaple) allows for easy insertion, constant compression at the fracture site, and prevents the humpback deformity of the scaphoid.
One major disadvantage associated with the use of the nitinol staple for these grossly unstable injuries is the fact that a skilled surgical assistant is often required to maintain the reduction of the scaphoid while the surgeon inserts the staple. Alternatively, provisional fixation can sometimes be obtained with smooth k-wires to allow for insertion of the staple, but a skilled surgical assistant is usually better for maintaining the reduction while the scaphoid is drilled and the staple is inserted. Other potential complications of the trans-scaphoid perilunate injury include post traumatic arthritis, non-union, carpal instability, and carpal malalignment [5,811,21,22].
In our experience with 18 patients, one patient failed treatment with Nitinol staple fixation and was subsequently treated with excision of the scaphoid and four-corner fusion.
- Dunn J, Kusnezov N, Fares A, Mitchell J, Pirela-Cruz M (2017) The scaphoid staple: A systematic review. HAND (NY) 12: 236-241. Link: https://bit.ly/2XpHwhz
- Mayfield JK, Johnson RP, Kilcoyne RK (1980) Carpal dislocations: Pathomechanics and progressive perilunar instability. J Hand Surg 5: 226-241. Link: https://bit.ly/2TYvolf
- Muppavarapu RC, Capo JT (2015) Perilunate dislocations and fracture dislocations. Hand clinics 399-408. Link: https://bit.ly/2zFiMc4
- Herzberg G, Comtet JJ, Linscheid RL, Amadio PC, Cooney WP, et al. (1993) Perilunate dislocations and fracture-dislocations: A multicenter study. J Hand Surg 18: 768-779. Link: https://bit.ly/2BiXjWB
- Herzberg G, Forissier D (2002) Acute dorsal trans-scaphoid perilunate fracture-dislocations: Medium-term results. Journal of hand surgery (Edinburgh, Scotland) 27:498-502. Link: https://bit.ly/36MX8hY
- Hildebrand KA, Ross DC, Patterson SD, Roth JH, MacDermid JC, et al. (2000) Dorsal perilunate dislocations and fracture-dislocations: Questionnaire, clinical, and radiographic evaluation. J Hand Surg Am 25: 1069-1079. Link: https://bit.ly/2Mj5BAg
- Krief E, Appy-Fedida B, Rotari V, David E, Mertl P, et al. (2015) Results of perilunate dislocations and perilunate fracture dislocations with a Minimum 15-year follow-up. J Hand Surg 40: 2191-2197. Link: https://bit.ly/2zGxpvL
- Griffin M, Roushdi I, Osagie L, Cerovac S, Umarji S (2016) Patient-reported outcomes following surgically managed perilunate dislocation: Outcomes after perilunate dislocation. Hand (New York, N.Y.) 11: 22-28. Link: https://philips.to/3cmwWfk
- Wu JC, Mills A, Grant KD, Wiater PJ (2019) Fracture fixation using shape-memory (ninitol) staples. Orthop Clin North Am 50: 367-374. Link: https://bit.ly/2Xlz3vN
- Tang JB, Giddins G (2016) Why and how to report surgeons’ levels of expertise. J Hand Surg Eur 41: 365-366. Link: https://bit.ly/2TZRp34
- Bagheri F, Taraz-Jamshidi MH, Birjandinejad A, Sharifi-Daloei SR, Mirkazemi M, et al. (2013) Trans-scaphoid perilunate fracture-dislocation and isolated perilunate dislocations; surgical versus non surgical treatment. Arch Bone Jt Surg 1: 74-77. Link: https://bit.ly/3ct5OLT
- Herbert TJ, Fisher WE (1984) Management of the fractured scaphoid using a new bone screw. J Bone Joint Surg Br 66: 114-123. Link: https://bit.ly/2TYwA8m
- DiGiovanni B, Shaffer J (1995) Treatment of perilunate and transscaphoid perilunate dislocations of the wrist. Am J Orthop (Belle Mead N.J) 24: 818-826. Link: https://bit.ly/3eE1CdE
- Knoll VD, Allan C, Trumble TE (2005) Trans-scaphoid perilunate fracture dislocations: Results of screw fixation of the scaphoid and lunotriquetral repair with a dorsal approach. J Hand Surg Am 1145-1152. Link: https://bit.ly/3cnIWxc
- Capo JT, Corti SJ, Shamian B, Nourbakhsh A, Tan V, et al. (2012) Treatment of dorsal perilunate dislocations and fracture-dislocations using a standardized protocol. Hand 7: 380-387. Link: https://bit.ly/3gGifXI
- Sotereanos DG, Mitsionis GJ, Giannakopoulos PN, Tomaino MM, Herndon JH (1997) Perilunate dislocation and fracture dislocation: A critical analysis of the volar-dorsal approach. J Hand Surg Am 22: 49-56. Link: https://bit.ly/2yQaE7W
- Trumble T, Verheyden J (2004) Treatment of isolated perilunate and lunate dislocations with combined dorsal and volar approach and intraosseous cerclage wire. J Hand Surg Am 29: 412-417. Link: https://bit.ly/36P1vZT
- Blazar PE, Murray P (2001) Treatment of perilunate dislocations by combined dorsal and palmar approaches. Tech Hand Up Extrem Surg 5: 2-7. Link: https://bit.ly/2U1g9bs
- Garcia-Elias M, Vall A, Salo JM, Lluch AL (1988) Carpal alignment after different surgical approaches to the scaphoid: A comparative study. J Hand Surg Am 13: 604-612. Link: https://bit.ly/2XMv6iB
- Hildebrand KA, Ross DC, Patterson SD, Roth JH, MacDermid JC,et al. (2000) Dorsal perilunate dislocations and fracture-dislocations: Questionnaire, clinical, and radiographic evaluation. J Hand Surg Am 25: 1069-1079. Link: https://bit.ly/2Mj5BAg
- Krief E, Appy-Fedida B, Rotari V, David E, Mertl P, et al. (2015) Results of perilunate dislocations and perilunate fracture dislocations with a Minimum 15-year follow-up. J Hand Surg 40: 2191-2197. Link: https://bit.ly/2zGxpvL
- Griffin M, Roushdi I, Osagie L, Cerovac S, Umarji S (2016) Patient-reported outcomes following surgically managed perilunate dislocation: Outcomes after perilunate dislocation. Hand (N.Y.) 11: 22-28. Link: https://bit.ly/3eBVIcP
- Kawamura K, Chung KC (2008) Treatment of scaphoid fractures and nonunions. J Hand Surg 33: 988-997. Link: https://bit.ly/3cgUWQY
- Wickramasinghe NR, Duckworth AD, Clement ND, Hageman MG, McQueen MM, et al. (2015) Acute median neuropathy and carpal tunnel release in perilunate injuries can we predict who gets a median neuropathy? J Hand Microsurg 7: 237-240. Link: https://bit.ly/2yQvMLk
- Najarian R, Nourbakhsh A, Capo J, Tan V (2011) Perilunate injuries. Hand (N.Y.) 6: 1-7. Link: https://bit.ly/36N3Cxk
- Bagheri F, Taraz-Jamshidi MH, Birjandinejad A (2013) Trans-scaphoid perilunate fracture-dislocation and isolated perilunate dislocations; surgical versus non surgical treatment. Arch Bone Jt Surg 1: 74-77. Link: https://bit.ly/3ct5OLT
- Garcia-Elias M (1997) The treatment of wrist instability. J Bone Joint Surg 79: 684-690. Link: https://bit.ly/2XNbo6m
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.






 Save to Mendeley
Save to Mendeley
