Open Journal of Orthopedics and Rheumatology
Universal S-shaped Lateral Approach of the Ankle and Hind foot: Technical Tip
Christophe Vercruysse* and Vandeputte Geoffroy
Cite this as
Vercruysse C, Geoffroy V (2020) Universal S-shaped Lateral Approach of the Ankle and Hind foot: Technical Tip. Open J Orthop Rheumatol 5(1): 006-008. DOI: 10.17352/ojor.000020Introduction
The operative treatment of the unstable cavovarus foot is a multi-level procedure and comprises of a combination of osteotomies and soft tissue procedures. After correctionof the bony deformity the soft tissues are balanced via soft tissue procedures and lastly ancillary procedures can be performed. There is evidence that in patients with cavovarus malalignment in combination with ankle. Instability due to lateral ligament insufficiency, an isolated lateral ligament reconstruction will fail over time [1-3]. Moreover, degenerative ankle arthritis and peroneal tendon pathology can be associated in patients with chronic ankle instability and cavovarus malalignment [4].
There is however no consensus on the operative technique since more than 80 lateral ligament repair procedures have been described to restore ankle stability [5]. In addition, there is no literature to date that describes a singular approach that combines the reconstruction of the lateral ligaments with a corrective osteotomy of the calcaneus and treatment of peroneal tendon pathology.
In order to avoid multiple lateral hindfoot incisions we propose a universal Sshaped lateral approach of the hindfoot where one incision gives access and a good visualization of the calcaneus, the lateral malleolus, the lateral ankle ligaments, talar neck and peroneal tendons.
In case of a cavovarus foot with lateral ligament instability, a lateralising calcaneal osteotomy, repair of the peroneal tendons and lateral ankle ligament reconstructionaugmentation can be performed using the same incision. If necessary, a peroneus longus to brevis tranfer can be done simultaneously.
Operative technique
In our institute a preoperative planning is done with standing X-ray. Coleman block test is performed to assess hindfoot versus forefoot driven cavovarus. Only patients with a passively correctable deformity are candidates for ligament reconstruction and corrective osteotomies. In cases of severe cavovarus and rigid or arthritic hindfoot an arthrodesis is done.
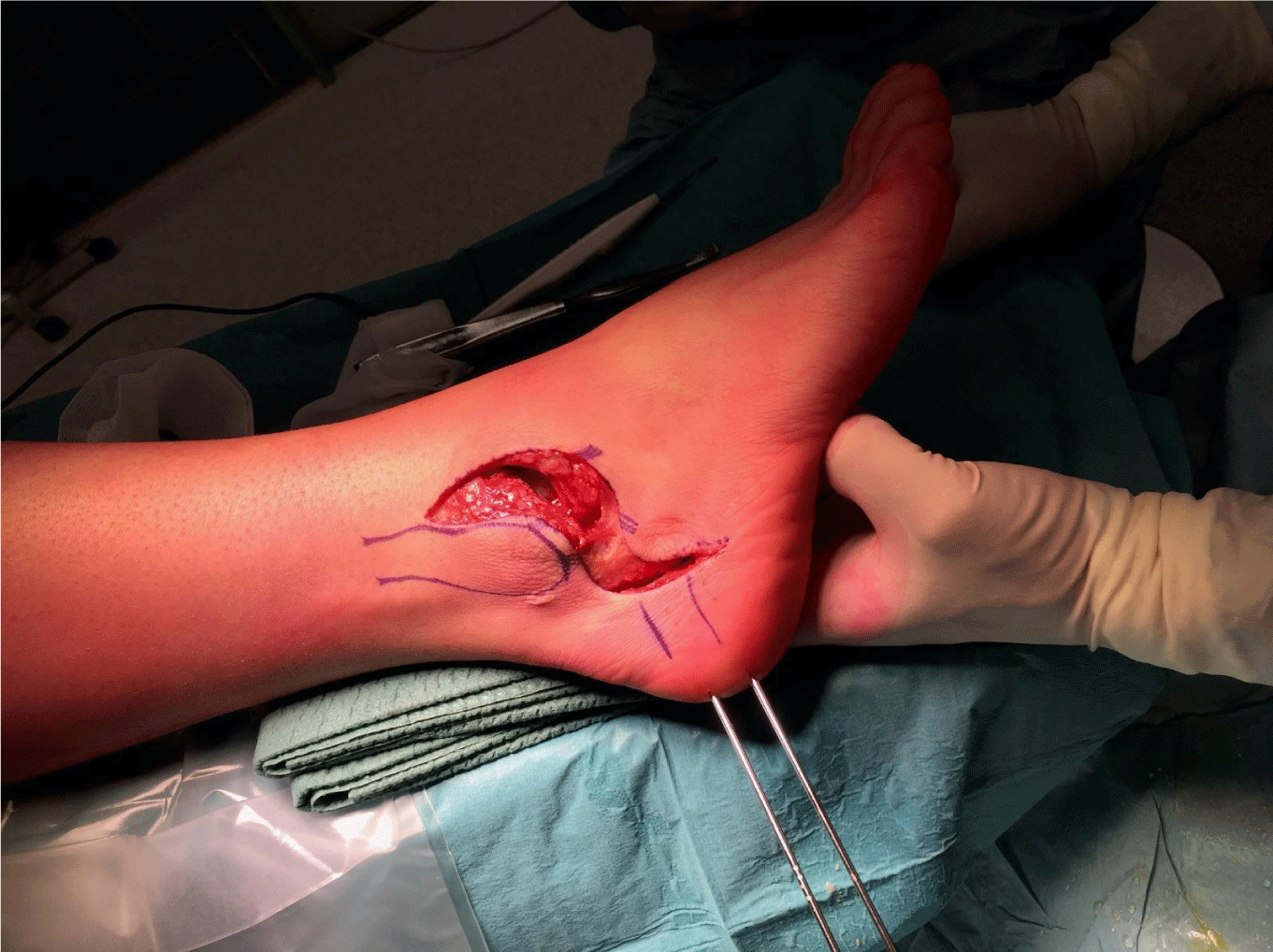
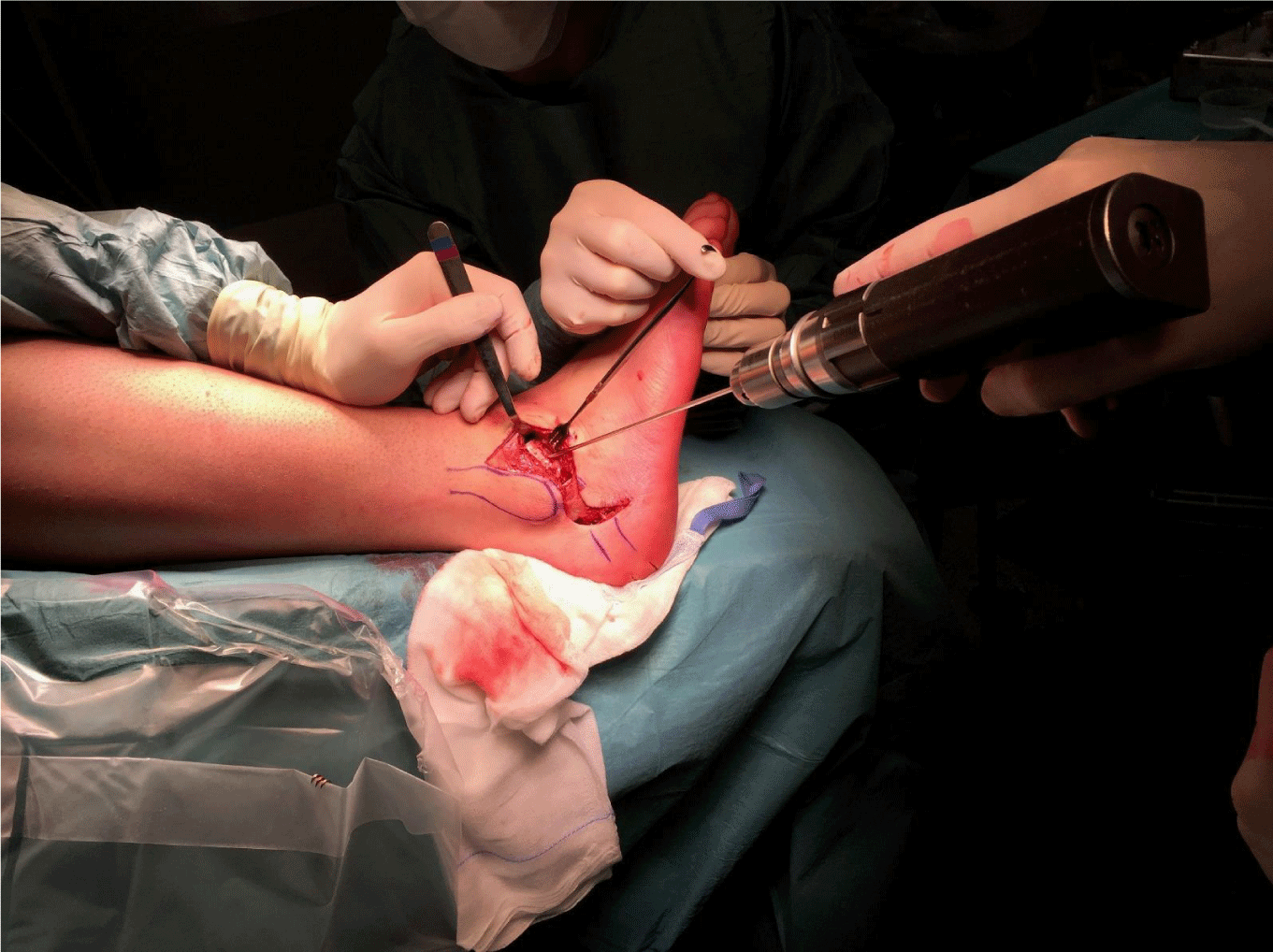
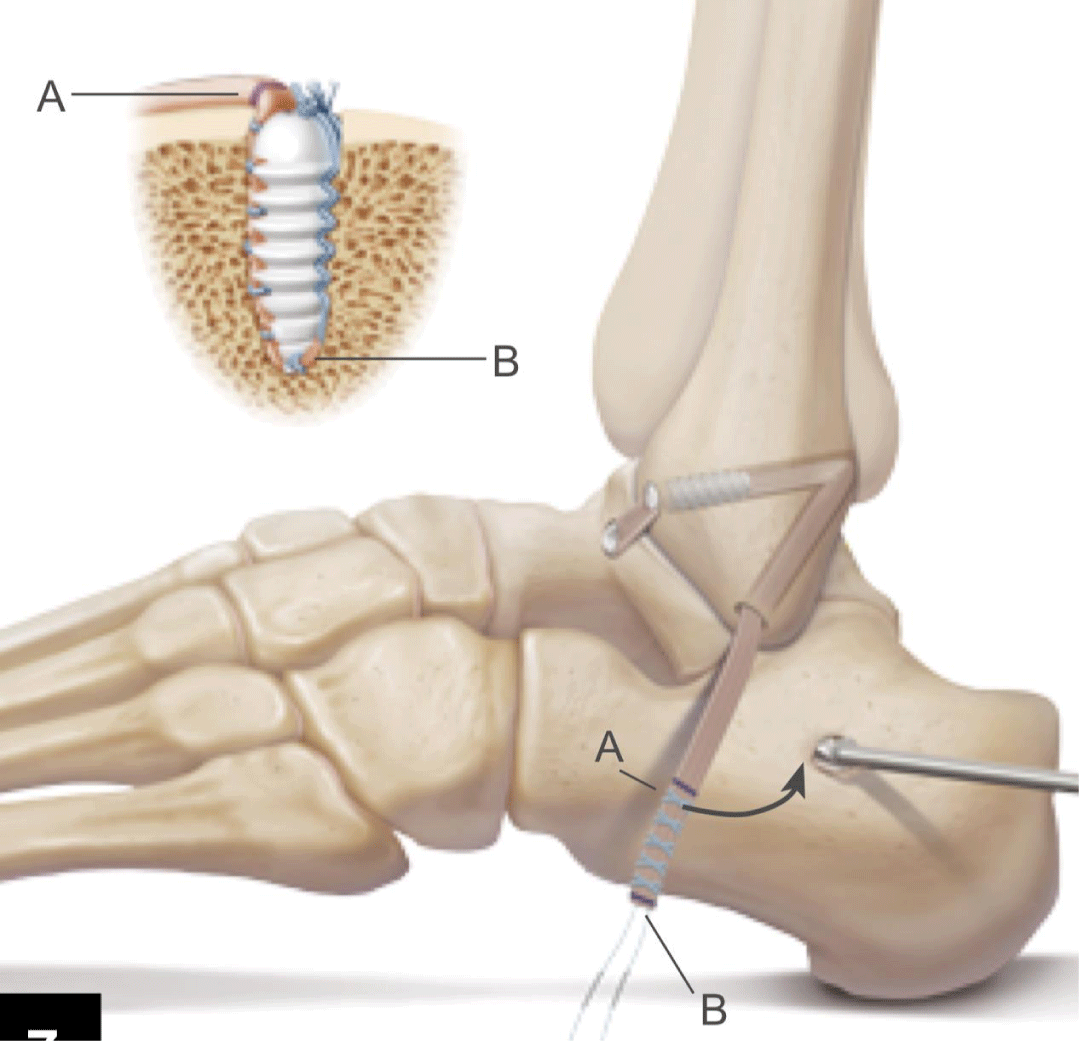
The patient is given a popliteal block followed by a general anesthesia with the patient in supine position with hip and knee in flexion. A cushion is placed underneath the ipsilateral hip to optimize access of the lateral hindfoot. After administrating the prophylactic antibiotics, the extremity is exsanguinated and a thigh tourniquet is inflated to 300mmHg. An S-shaped incision is made from the anterior border of the distal fibula along the lateral malleolus until the tip of the distal fibula, where the incision bends back to anterior to the calcaneus (Figure 1). Two skin flaps are created and provide a good view from the talar neck over the lateral malleolus to the lateral aspect of the calcaneus (Figure2). First of all, the sural nerve is visualised and protected. The peroneal tendons are then released under the distal peroneal retinaculum. Most often we find a degenerative rupture of the peroneus brevis tendon. This is debrided and at the end of the procedure a transfer of the peroneus longus to brevis tendon distally is performed. The varus deformity of the calcaneus is corrected via a Dwyer closing wedge lateralising calcaneal steotomy (Figure 2). Translation is performed and two cannulated screws are inserted. In cases with a longstanding lateral ankle instability we prefer to reconstruct the lateral ankle ligaments with a gracilis autograft tendon (Figure 3). The aim is to anatomically reconstruct the anterior talofibular ligament (ATFL) andthe calcaneofibular ligament (CFL). This autograft is first fixed in a blunt tunnel in the talar neck (origin of the ATFL), then passed through two fibular tunnels and finally fixated in a blunt tunnel in the calcaneus footprint of the CFL) (Figure 4). The subcutaneus tissue is closed loosely with an absorbable suture. The two skinflaps are realigned and the skin is closed tensionless with staples (Figure 5).
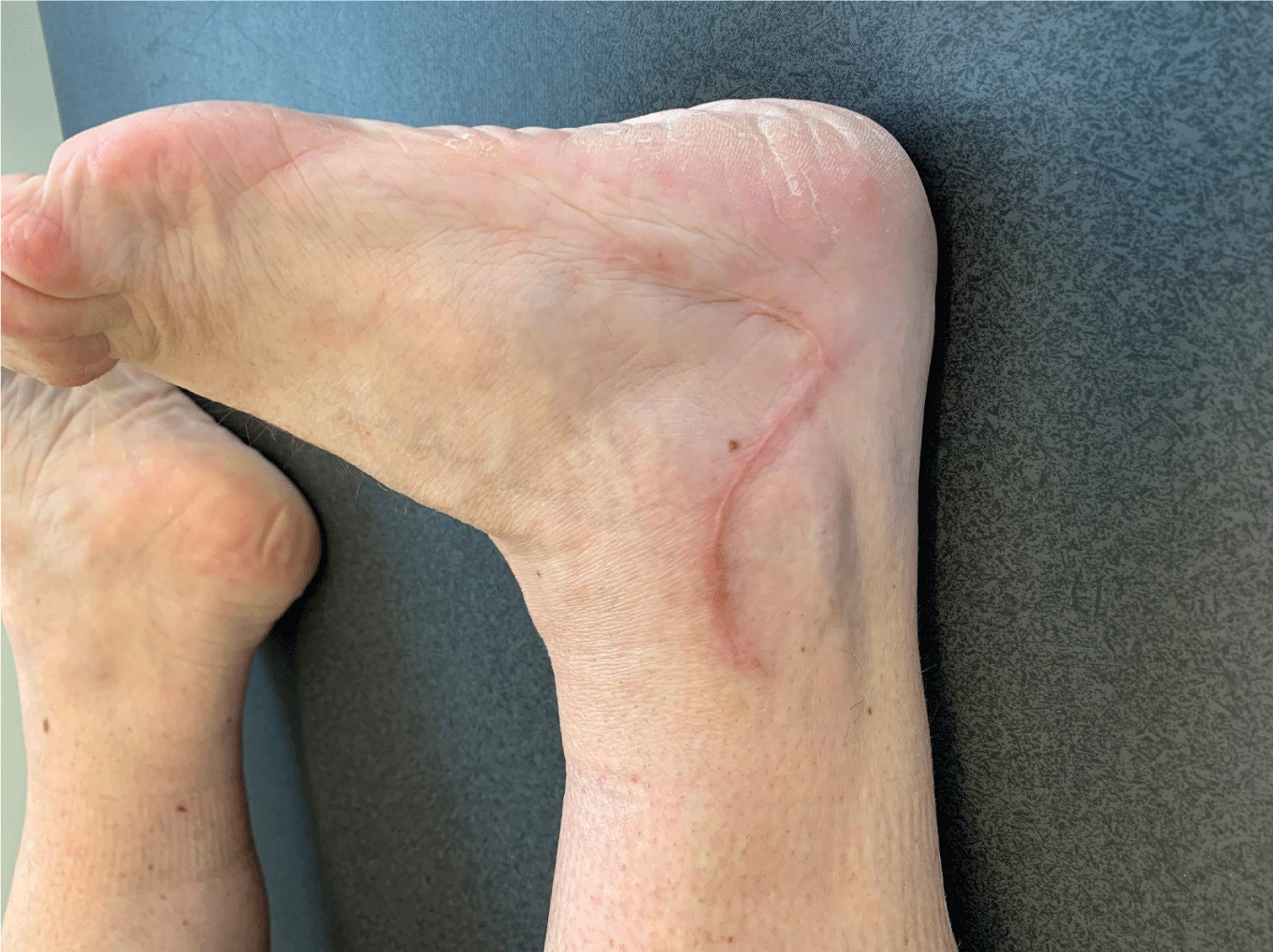
Good wound healing is seen at 6 weeks postoperative consult (Figure 6).
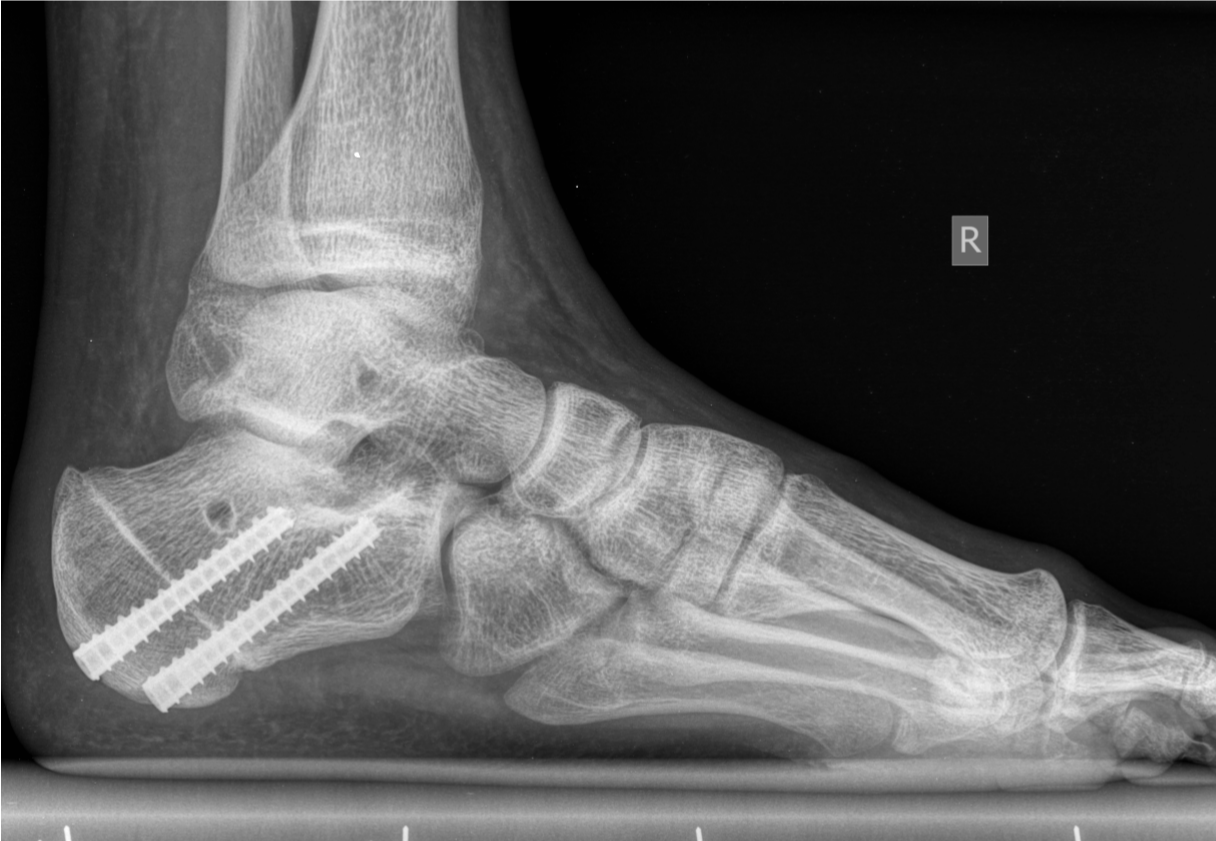
Postoperative X-ray at 6 weeks with consolidation of the osteotomy and remnants of the tunnels of the lateral ligament reconstruction (Figure 7).
Discussion
We propose a universal S-shaped lateral approach of the hindfoot. Our purpose was to create an incision with maximal visualization and good wound healing potential. We performed this incision at our institution in 11 cavovarus cases. With this approach we had maximal visualization of the calcaneus, the lateral malleolus, the lateral ankle ligaments, talar neck and peroneal tendons. We had minimal wound traction and consequently had no wound healing problems, no tender scars and no keloid formation. With this singular approach we avoid multiple incisions in the lateral hindfoot, where wound healing complications are common. In previous studies it is shown that wound complication rate up to 30% is described for intra-articular calcaneal fractures treated with open reduction and have the advantage that a large area can be accessed due to the creation of two flaps that can be retracted. A maximal visualization is obtained and all relevant anatomical structures can be reached to correct hindfoot varus and lateral ankle instability. The described S-shaped incision is particulary suited for the combination of lateral ankle ligament reconstruction and calcaneal osteotomy as is described in the operative technique. However this approach can potentially be used for other procedures of the calcaneus, the lateral malleolus, the lateral ankle ligaments, talar neck and peroneal tendons.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
- Kaplan JRM, Aiyer A, Cerrato RA, JengCL, Campbell JT (2018) Operative Treatment of the Cavovarus Foot. Foot Ankle Int 39: 1370-1382. Link: https://bit.ly/2AXTBBv
- Bosman HA, Robinson AH (2013) Treatment of ankle instability with an associated cavus deformity. Foot Ankle Clin 8: 643-57. Link: https://bit.y/3c4px3W
- Kuhn MA, Lippert FG (2006) Revision Lateral Ankle Reconstruction. Foot Ankle Int 27: 77-81. Link: https://bit.ly/2AXbJLS
- Fortin PT, GuettlerJ, Manoli A (2002) Idiopathic cavovarus and lateral ankle instability: Recognition and treatment implications relating to ankle arthritis. Foot Ankle Int 23: 1031-1037. Link: https://bit.ly/2Xz0bGr
- Tourné Y, Mabit C (2017) Lateral ligament reconstruction procedures for the ankle. Orthop Traumatol Surg Res 103: S171–S181. Link: https://bit.ly/3d76abS
- Bernirschke SK, Kramer PA (2004) Wound healing complications in closed and open calcaneal fractures. J Orthop Trauma 18: 1-6. Link: https://bit.ly/2LWqIbl
- Folk JW, Starr AJ, Early JS (1999) Early Wound Complications of Operative Treatment of Calcaneus Fractures: Analysis of 190 Fractures. J Orthop Trauma 13: 369-372. Link: https://bit.ly/3elCWq5
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.



 Save to Mendeley
Save to Mendeley
