Open Journal of Biological Sciences
Does classical immunity acquired by the subcontinent population become advantageous to manage COVID-19 due to the low rate of mortality?
Partha Pratim Das1,2, Subhash Medhi1, Sangit Dutta2 and Pranab Jyoti Das3*
2Department of Medicine, Gauhati Medical College and Hospital, Guwahati, Assam 781032, India
3Indian Council of Agricultural Research-National Research Centre on Pig, Rani, Guwahati, Assam 790101, India
Cite this as
Das PP, Medhi S, Dutta S, Das PJ (2020) Does classical immunity acquired by the subcontinent population become advantageous to manage COVID-19 due to the low rate of mortality? Open J Biol Sci 5(1): 034-037. DOI: 10.17352/ojbs.000022The global pandemic due to the COVID-19 has severely affected the entire world risking human life and economy. Every possible attempt becomes inadequate in controlling the disease as the number rising each passing day. Indeed, a highly populated country like India has so far successful in mitigating the outbreak within the country. Meanwhile, the strategy based on a preliminary model of assumption with massive awareness program on social (physical) distancing, compulsory wearing of a mask and nationwide lockdown might have contributed immensely to controlling such an emergency. However, the influence of the immune-competent genetic architecture of the Indian racing population and comparatively a dominant young age group population cannot be ruled out completely. Moreover, a suitable environment for viral propagation and characteristics of viral strain are other such factors that simultaneously could add a real scientific justification. However, the current global scenario indicating the countries with higher median age are severely affected compared to the Indian and African subcontinent thereby survived an outbreak with a low mortality rate. At the same time, we never claimed for complete immunity for the COVID-19 depending on age or immunity. The increased incidence of positive cases might slowly also increase the death rate within India, but so far recorded low compared to other parts of the globe.
Introduction
Coronaviruses are a group of RNA virus usually causes respiratory disease in human [1]. The term ‘corona’ has been derived from the crown-like structural morphology observed on the surface of the virus [2]. This virus was identified in numerous hosts of avian and mammalian origin including humans. The possible animal reservoir of the viral strain of the beta-corona virus in recent times has transmitted to humans via intermediated host as a source of zoonotic infection. The novel coronavirus SARS-CoV-2 is highly infectious and found to be the seventh member of its family that infect humans [3]. The previously identified coronaviruses were 229E, NL63, OC43, HKU1, SARS-CoV and MERS-CoV. These identified coronaviruses are sub-grouped into two genera namely alpha-corona virus and beta-corona virus. Indeed, the novel coronavirus disease (COVID-19) ensured to be settled with a lower mortality rate than previous SARS and MERS coronavirus diseases [4]. The whole-genome sequence of SARS-CoV-2 is closely related (88% identity) to bat-SL-CoVVZC45 and bat-SL- CoVZXC21 than SARS-CoV and MERS-CoV which is about 79% and 50% respectively. Notably, the initial investigation also revealed 99.98% sequence similarity among the novel SARS-CoV-2 virus with the largest nucleotide difference of four mutations among a few initial samples tested, indicates the recent evolution of the virus in humans [5]. The evolutionary attributes of the viruses were strongly emphasized on the genetic exchange or prominence of recombination. A positive-strand RNA virus (like coronavirus) often demonstrate a copy-paste mechanism where a nascent RNA strand can dissociate from its original point and can continue synthesis elsewhere in the genome [6]. Thereby prompt to enhance the recombination possibility when attached to a similar sequence, which more often observed in coronavirus [7]. Due to the larger genome size of this virus, it is more likely to have recombination frequently and anonymously increases the chances of evolving new mutants [7]. As a result, this virus can escape host immunity and create an outbreak at a significant interval. Here, we briefly summarize a possible role of few dominant aspects in the Indian subcontinent, subsequently helps in the management of emergency outbreak due to COVID-19.
COVID-19 infection prospect in indian subcontinent
Recently, India ended up a phase-wise nationwide lockdown since March 25, 2020. Even, the incidence of positive cases of COVID-19 was eventually low initially; the rapid rise of positive cases after lockdown has put a tremendous burden on the healthcare system. However, a huge cluster of asymptomatic cases and low mortality rates compared to Europe and America open up diverse panoramas for the scientific community for intervention. The prediction about India’s infectivity scenario of COVID-19 has been robust. Initially, India too adopted the same policy regarding the outbreak based on a preliminary investigation of the epidemiological and mathematical model of assumption. While time to time scientists and epidemiologists from across the globe have put forward different hypotheses depicting India’s future of pandemic. The delayed sustainability towards community transmission and the low mortality rate of COVID-19 gained scientific attention. India also has not been witnessed any region-specific outbreak to date with a country with the second largest population in the world. Several classical factors might have hindered the fast propagation of the virus in the Indian environment. Any viral infectivity depends upon few factors i.e. virulence or harmfulness of the virus, host immune system status, a suitable environment to propagate the virus and lastly availability of the drug to mitigate the severity caused by the virus [8,9]. If all these factors favour the virus to infect, pandemic like emergency occurs. A lockdown like situation can minimize the severity of pandemic but cannot stop the viral infectivity.
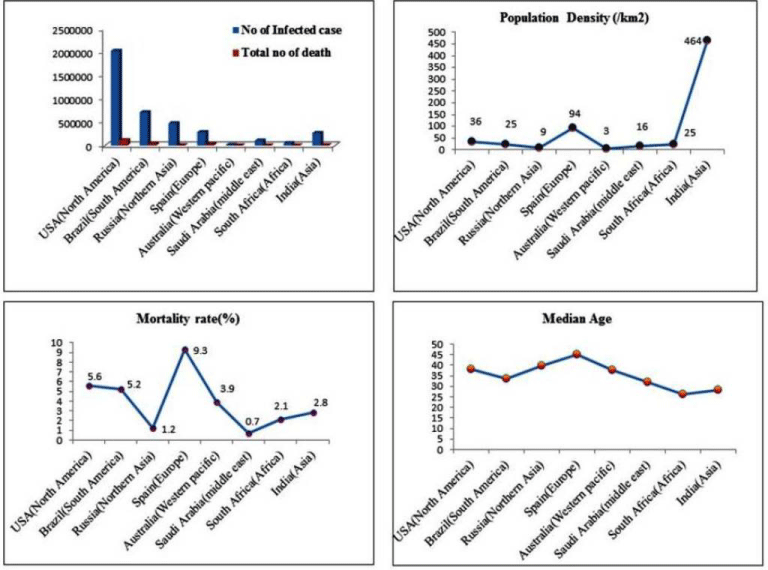
An unfavorable climatic condition of tropical temperature and high humidity might be advantageous to restrict the fast propagation of the virus in the Indian environment. Moreover, the role of a discrete immune profile acquired by the population in suppressing the exponential propagation of the virus cannot be diminished completely. Past research revealed that Indians acquired more and diverse KIR (killer cell immunoglobulin-like receptor) genes due to natural selection for survival [2], whereas another finding observed that Indian population possesses more number of NK (Natural killer) cells compared to Americans that can influence innate immunity [10]. Thereby, we can have a more proactive innate immune system. While the prediction of Chinese researcher Wang, Xu [11] about the low severity of COVID-19 for malaria-infected regions in the world somehow supporting the current global scenario. Moreover, a vivid social distinction of the Indian subcontinent and genomic admixture helps to inherit extensive MHC diversity within the population. Indeed, a variant of HLA has been found to associate with the various risk factor of autoimmune and infectious disease [12,13]. One of the most common HLA haplotypes, HLA-A2-B50-DR3 is predominant in the Indian population but not reported in the rest of the world [14]. Whereas, prevalent of subtype A*0211 of HLA-A2 allele in the distinct Indian population also reported in the past study [15]. The association of dominant HLA allele with the pathogen clearance has also been reported for HIV, HCV and HBV previously [16,17]. Such a finding supports the notion of mutation or selection of the genes acquired in response to environmental agents in due course of time within the region [18]. All these assumptions and clinical findings turned out to be a little advantageous blessing in the context of an outbreak and might be a cause of low mortality in India. Additionally, the demographic dividend of India seems to be eventually added further advantages in slowing pandemic like situation in India. It has also been seen that high median age countries are highly affected than low median age group countries. Italy, Spain has a population with a median age of 45 and 45 years respectively whereas the USA and China both have 38 years. However, India’s population median age is 28 years and interestingly that number for the African continent is 18 years correlating with the low mortality rate [19,20]. Figure 1 depicts some of the classical data of top nations from different continents. The mortality rate of COVID19 in India is so far recorded nearly 2.8% where 2,67,064 infection reported (till 8th June 2020). Although South Africa, Russia and Saudi Arabia recorded low rate of mortality but their population density is far below; which is 25, 9 and 16 respectively. Whereas, according to 2020 census data India’s population density is recorded 464 per square kilometer [20,21].
Thus, in regards to the current trend of pandemic across the world, India’s resilience in diminishing the effect has been outstanding. Though, it is hard to predict the future course of progression. But such heterogeneity ensures better management of this disease within the country. Effective and quick response from the government side also needs to acknowledge. However, we never the less advocate for any severity of infections in the future from COVID-19 in India. Precaution is the best policy to deal with such novel microbial entities and highly contagious diseases [22].
Conclusion
India almost witnessed having positive cases of COVID-19 from every corner of the county. From the public health standpoint, the only hint of optimism prevailing is due to the low rate of mortality. Despite the diversity in population in the country, the infectivity rate of SARS-CoV-2 may remain persistent. However, further work can elucidate the precise role of immunogenic profile in resisting viral pathogenicity for morbidity and mortality in various ways. The accumulation of knowledge with the unanswered question regarding the disease outbreak should be the top priority in the current time.
We thank Gauhati University, Department of Bioengineering & Technology and Department of Medicine, Gauhati Medical College & Hospital for infrastructure support.
- Weiss SR, Navas-Martin S (2005) Coronavirus pathogenesis and the emerging pathogen severe acute respiratory syndrome coronavirus. Microbiol Mol Biol Rev 69: 635-664. Link: https://bit.ly/2V7J2TQ
- Rajalingam R, Du Z, Meenagh A, Luo L, Kavitha VJ, et al. (2008) Distinct diversity of KIR genes in three southern Indian populations: comparison with world populations revealed a link between KIR gene content and pre-historic human migrations. Immunogenetics 60: 207-217. Link: https://bit.ly/314uKqP
- Cascella M, et al. (2020) Features, Evaluation and Treatment Coronavirus (COVID-19). StatPearls. Link: https://bit.ly/2Z1pgua
- Shi H, Han X, Jiang N, Cao Y, Alwalid O, et al. (2020) Radiological findings from 81 patients with COVID-19 pneumonia in Wuhan, China: a descriptive study. The Lancet Infectious Diseases 20: 425-333. Link: https://bit.ly/2BsSk5W
- Lu R, Zhao X, Li J, Niu P, Yang B, et al. (2020) Genomic characterisation and epidemiology of 2019 novel coronavirus: implications for virus origins and receptor binding. Lancet 395: 565-574. Link: https://bit.ly/3hNEYlj
- Kirkegaard K, Baltimore D (1986) The mechanism of RNA recombination in poliovirus. Cell 47: 433-443. Link: https://bit.ly/3eppu51
- Plyusnin A, Kukkonen SKJ, Plyusnina A, Vapalahti O, Vaheri A (2002) Transfection‐mediated generation of functionally competent Tula hantavirus with recombinant S RNA segment. EMBO J 21: 1497-1503. Link: https://bit.ly/2YmSm8p
- Manjarrez-Zavala ME, Rosete-Olvera DP, Gutiérrez-González LH, Ocadiz-Delgado R, Cabello-Gutiérrez C (2013) Pathogenesis of viral respiratory infection. Respiratory Disease and Infection: A New Insight 1. Link: https://bit.ly/2Z3Aej8
- Guomin C, Wu J (2019) Permanent Resident Virus in Human Beings Viral Microecology of Human Being. 3: 229-235. Link: https://bit.ly/2Cn2jKi
- Rathore DK, Holmes TH, Nadeau KC, Mittal P, Batra A, et al. (2018) Differences in multiple immune parameters between Indian and US infants. PloS One 13. Link: https://bit.ly/3dq5YUB
- Wang J, Xu C, Wong YK, He Y, Adegnika AA, et al. (2020) Preparedness is essential for malaria-endemic regions during the COVID-19 pandemic. Lancet 395: 1094-1096. Link: https://bit.ly/3enGAAj
- Matzaraki V, Kumar V, Wijmenga C, Zhernakova A (2017) The MHC locus and genetic susceptibility to autoimmune and infectious diseases. Genome biology 18: 76. Link: https://bit.ly/31haYIX
- Shiina T, Hosomichi K, Inoko H, Kulski JK (2009) The HLA genomic loci map: expression, interaction, diversity and disease. Journal of human genetics 54: 15-39. Link: https://go.nature.com/37Ng68O
- Mehra N (2010) Defining genetic architecture of the populations in the Indian subcontinent: impact of human leukocyte antigen diversity studies. Indian J Hum Genet 16: 105-107. Link: https://bit.ly/3doc6N1
- Mehra NK, Jaini R, Rajalingam R, Balamurugan A (2001) Molecular diversity of HLA‐A* 02 in Asian Indians: predominance of A* 0211. Tissue Antigens 57: 502-507. Link: https://bit.ly/2V1k3BB
- Singh R, Kaul R, Kaul A, Khan A (2007) A comparative review of HLA associations with hepatitis B and C viral infections across global populations. World J Gastroenterol 13: 1770-1787. Link: https://bit.ly/2NfNtYq
- Raghavan S, Selvaraj P, Swaminathan S, Alagarasu K, Narendran G, et al. (2009) Haplotype analysis of HLA‐A,‐B antigens and‐DRB1 alleles in south Indian HIV‐1‐infected patients with and without pulmonary tuberculosis. Int J Immunogenet 36: 129-133. Link: https://bit.ly/2YpUlZH
- Mehra NK (2000) The HLA genes and their diverse polymorphism. Indian J Clin Biochem 15: 65-77. Link: https://bit.ly/2NkYojG
- Organization WH (2020) Population median age (years) (Demographic and socioeconomic statistics). Link: https://bit.ly/3epDzPE
- WHO Link: https://www.who.int/
- Link: https://www.worldometers.info/
- Guan WJ, Chen RC, Zhong NS (2020) Strategies for the prevention and management of coronavirus disease 2019. Eur Respir J 55: 2000597. Link: https://bit.ly/3duNHWp
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
