Journal of Vaccines and Immunology
Ability of TLR agonists to upregulate Brucella abortus strain RB51 mediated protection in a murine respiratory model
M Walker1, N Sriranganathan2, I Kanevsky4, K Zimmerman2, N Tenpenny3, M Makris3, S Werre3 and S Witonsky1*
2Department of Biomedical Sciences and Pathobiology, USA
3Research and Graduate Studies, Virginia-Maryland Regional College of Veterinary Medicine, Virginia Tech, Blacksburg, VA, USA
4Department of Dairy Science, College of Agricultural and Life Sciences, Virginia Tech, Blacksburg, VA, USA
Cite this as
Walker M, Sriranganathan N, Kanevsky I, Zimmerman K, Witonsky S, et al. (2019) Ability of TLR agonists to upregulate Brucella abortus strain RB51 mediated protection in a murine respiratory model. J Vaccines Immunol 5(1): 001-010. DOI: 10.17352/jvi.000023Brucella abortus is a Gram-negative intracellular zoonotic bacterium that causes infertility and abortion in cattle, and undulant fever in humans. Its low dose of infectivity, ability to be aerosolized, and ease of genetic modification, makes it a bioterror concern. The overall goal is to generate a safe and effective vaccine for humans. One candidate vaccine is Brucella abortus strain RB51, which was approved for use in cattle, and provides protection by initiating a strong T-helper 1 (CD4 Th1) response. Based on a model for aerosol exposure, mice were vaccinated intranasally (IN) with strain RB51 and challenged IN with B. abortus strain 2308. However, strain RB51 did not protect. Protection against Brucella is mediated through Toll Like Receptors (TLRs) 2, 4 and 9. The addition of TLR 2 or TLR 4, and a trend with TLR9 agonists, when combined with IN strain RB51 vaccination, significantly increased bacterial clearance in the lung after strain 2308 challenge. Therefore, for this study, we hypothesized that combining TLR agonists 2, 4, and 9 with strain RB51 IN would enhance protection and clearance in the lung against strain 2308 challenge (IN), by activating the DC1 and CD4 Th1 and CD8 immune response. This study showed that protection was not enhanced by combining all TLR agonists. The group with non-significantly greater clearance was strain RB51 and TLR 2 and 4 agonists. Additional studies are warranted to further define the differential mechanisms and endpoints of protection and chronic infection.
Introduction
Brucella is one of the top 5 zoonotic diseases worldwide [1]. It is easily transmitted to humans from infected animals, through contact with aborted fetal material, consumption of unpasteurized dairy products, and/or ingestion and inhalation of infected materials. The ability of Brucella to be easily aerosolized, combined with its virulence, and potential to be genetically modified, make this pathogen a candidate for use as a biological weapon [1]. At this time, there is no efficacious vaccine for humans.
As a model for disease in humans and cattle, mouse models initially focused on intraperitoneal (IP), intramuscular (IM), or intravenous (IV) routes of vaccination and challenge [2-4]. None of these models were used to assess protection against respiratory infection. When laboratories began using these established mouse models to investigate respiratory infection and protection, there were differences in the ability of vaccination to provide protection against respiratory challenge irrespective of vaccine and challenge strains. Initially, Olsen et al. had shown that vaccination of mice IP with B. abortus strain RB51 provided protection against B. abortus strain 2308 IP but not aerosol challenge [2]. In an attempt to establish mucosal protection, Surendran et al. [5] vaccinated mice IN using strain RB51, but they were not protected against IN challenge with strain 2308 [5]. Furthermore, systemic IP vaccination and IN boost did not enhance clearance in the lung or mediastinal lymph node when challenged with strain 2308, nor did priming with intramuscular (IM) or intradermal (ID) vaccination followed by IN boost [5]. However, IP primary vaccination followed by secondary IN boost using B. abortus strain RB51SOD, a strain over expressing superoxide dismutase, showed significant clearance in the spleen, but not in the lung [5]. By contrast, using a B. melitensis vaccine strain administered IP, Kahl-McDongah et al., demonstrated protection in the lung against aerosolized challenge with either B. melitensis or B. abortus [6]. These studies support that the ability to protect the host against Brucella is dependent upon which strain, route, and dosage of vaccine and challenge strain is used. A vaccine that can stimulate the innate and adaptive immune response, including creating long term memory, is needed to provide protection against infection.
To develop an efficacious vaccine, knowledge is needed regarding the protective immune response against Brucella. Protection is mediated by TLRs 2, 4, 6, and 9, which can initiate a strong DC1 response and subsequently protective CD4 Th1 CD8 adaptive response. Brucella interferes with DC function, and therefore does not sufficiently activate T-cells, compared to uninfected cells [7-9]. Previous studies have demonstrated a role for TLR 2, 4, 6, and 9 in vitro and in vivo for Brucella mediated DC function [10-14]. As a first step, we demonstrated protection in the lung could be improved by using TLR 2 and 4, and a trend for TLR9, agonists individually, when combined with strain RB51 [11]. Therefore, the objective of this study was to determine if the addition of TLR agonists 2, 4, and 9 to intranasal (IN) strain RB51 vaccination, will enhance protection and clearance against strain 2308 IN challenge. We hypothesized that the addition of TLR agonists 2, 4, and 9 with IN B. abortus strain RB51 vaccination would upregulate the protective immune response against IN challenge with B. abortus strain 2308. Protection was assessed based on clearance and development of a DC1 CD4 Th1 CD8 response.
Materials and methods
Mice. Female BALB/c mice, 5-8 weeks old, from Charles River Laboratories Inc., Wilmington, MA were used in accordance to our approved protocol (10-009-CVM) by Institutional Animal Care and Use Committee at Virginia Tech.
Bacterial strains. Live B. abortus strain 2308 and strain RB51 were obtained from our stock culture collection. Experiments were performed in our Biosafety level (BSL)-3, Centers for Disease Control approved (C2003 1120-016) facility [3,5].
Experimental design. BALB/c mice (n=5/group) were anesthetized with 0.4 mL of xylazine-ketamine (0.2 mg/mL and 0.9 mg/mL) mixture; serum was collected by retro-orbital bleeding. Mice were vaccinated with 20 µL phosphate buffered saline (PBS control) or B. abortus strain RB51 (4x108 CFU/mouse) alone, or in combination with TLR agonists 2 and 4, or TLR agonists 2, 4, and 9 (all TLR agonists: Invivogen San Diego, CA). Concentrations were TLR2 agonist PAMCSKK4 (5 ug/mouse), TLR4 agonist ultrapure E. coli 0111:B4 LPS (10 ug/mouse), and TLR9 agonist CpG (30 ug/mouse) These doses were chosen based on previous studies which demonstrate protection at this dose for TLR2 and TLR4 with a trend for TLR9 in the lung (8, 9). The four groups are: PBS control, experimental RB51: RB51; strain RB51 with TLR 2 4 agonists: RB51TLR24; and RB51 with the TLR 2 4 9 agonists: RB51TLR249 groups. Six weeks post vaccination, mice were anesthetized and challenged IN with strain 2308 (2x104 CFUs/mouse). Mice were euthanized two weeks post challenge using 1.4 mL of xylazine-ketamine mixture. Bronchoalveolar lavage (BAL), serum, lung, spleen, mediastinal lymph node (MLN) were collected. Organs were homogenized using a tissue homogenizer, and then serially diluted and plated on Tryptic soy agar (TSA) plates. Plates were incubated for 5 days at 37°C and 5% CO2(8). Minimum level of detection of CFU’s was 20. Samples with no colonies present were recorded as 19 CFUs. Organ homogenates were frozen for cytokine analysis [3,5,10].
Antibody titers. BAL and serum were stored at -80°C until analyzed. Plates were coated with either heat killed strain 2308 or heat killed strain RB51 at 1 µg/well. Plates were washed with Tris buffered saline TBS (Fisher Scientific, Fairlawn, NJ) and 0.05% Tween 20 (Fisher Scientific). Plates were blocked with 200 µL 2% BSA (Sigma, St. Louis, MO) in TBS at 37°C for 1 hour, and then plates were washed. The bronchoalveolar lavage (BAL) samples were not diluted. Serum samples were diluted 1:100 for identification of IgA and IgG1, and a dilution of 1:100 and 1:200 were used for IgG2a in 2% BSA (Fisher Scientific). Fifty µL per well was added to each well, and duplicate samples were incubated for 4 hours at room temperature (RT). Plates were washed, and isotype specific anti-mouse horseradish peroxidase conjugates antibodies (IgG1, IgG2a, IgA) (Southern biotechnology associates Inc., Birmingham, Alabama) were added at 1:4000 dilution. Plates were incubated, and then plates were washed. TMB was added at 100 µL per well (Microwell peroxidase substrate, Kirkgaard & Perry Laboratories, Gaithersburg, MD). The reaction was stopped using 100 µL per well of 0.185 M sulfuric acid (Fisher Scientific) to stop the reaction. Antibody levels in serum of pre-vaccinated, and serum and BAL of post-challenged mice were measured by ELISA using OD values [3].
Splenocyte isolation. Splenocytes were isolated as previously described. Briefly, red blood cells were lysed with 2 mL ACK lysis buffer (Lonza, Walkersville, MD) (150 mM NH4Cl, 1 mM KHCO3 0.1 mM Na2EDTA) for 2 minutes [15]. Samples were washed and resuspended in RPMI 1640 (Cellgro, Manassas, VA) complete media at 5 x 106 cells/ml. Splenocytes (5 x 105 cells/well) were cultured in 96 well plates and stimulated for 5 days with media, ConA (0.5µg/ well) (Sigma), irradiated (IR) or heat killed (HK) strain 2308 or RB51 at 106 CFU/ well. RPMI 1640 media (Cellgro) was supplemented with 2mM L-glutamine (Cellgro), 10% heat-inactivated fetal calf serum (Atlanta biological, Lawrenceville, GA), penicillin/streptomycin (Cellgro), and 50 µM 2-mercaptoethanol (Sigma). After 5 days, supernatants were harvested as previously described by Vemulapalli et al., and stored at -80°C until cytokine ELISAs could be performed [15].
Processing of Bronchoalvelor Lavages (BALs). BALs were spun at 250 x g for 5 minutes to isolate cells; BALs from mice were combined from either 2 mice (mice #4-5 per group) or 3 mice (mice #1-3 per group) to ensure enough cells for flow cytometry [11]. BAL supernatants were frozen at -80°C for cytokine and immunoglobulin analysis [11].
Flow cytometry. BAL and splenocyte samples were aliquoted for flow cytometry and proliferation assays [16]. As performed previously, because cell numbers were limited on some samples, 5 x 105 cells/sample were stained for flow cytometry [5,7,10,16]. Stain combinations were: DC1: APC conjugated anti-CD11c (BioLegend, San Diego, CA), PE conjugated anti -I-A/I-E (BD Pharmingen, Franklin Lakes, NJ), Biotin conjugated anti-CD40 (BioLegend), Pacific Blue conjugated anti-CD86 (BioLegend), PE-Cy7 conjugated anti-CD11b (BioLegend), PerCP conjugated Streptavidin (BioLegend); DC2: APC conjugated anti-CD11c (BioLegend), PE conjugated anti-I-A/I-E (BioLegend), Pacific Blue conjugated anti-CD8α (BioLegend), Biotin conjugated anti-CD103 (BD Pharmingen), PE-Cy7 conjugated anti-CD11b (BioLegend), PerCP conjugated Streptavidin (BioLegend); T1: APC conjugated anti-CD25 (BioLegend), PE-Cy7 conjugated anti-CD69 (BD Pharmingen) or FITC (BioLegend) conjugated anti-CD69, Texas Red conjugated anti-CD4 (Caltag Laboratories, Invitrogen Camarillo, CA), Pacific Blue conjugated anti-CD8α (BioLegend), PE conjugated ant--CD45RB (Caltag Laboratories); T2: PE conjugated anti-CD44 (BD Pharmingen), Texas Red conjugated anti-CD4 (Caltag Laboratories, Invitrogen), FITC conjugated anti-CD62L (BD Pharmingen), Pacific Blue conjugated anti-CD8α (BioLegend); T3: PE conjugated anti-B220 (BD BPharmingen), FITC conjugated anti-CD69 (BioLegend) [5,8,10].
Cytokines as determined by ELISAs. BALs, splenocyte supernatants, organ homogenates (lung, liver, spleen, MLN) were stored at -80°C. TNF-alpha (α), IL-12p70, IFN-γ, IL-10, IL-4, IL-17 were measured using indirect sandwich ELISAs (BD Pharmingen) [3,8,9]. Plates (Nunc, Roskilde, Denmark) were coated overnight with the respective capture antibodies for each cytokine at specified concentrations in their respective coating buffers. Plates were then blocked with 2% BSA in PBS for 30 minutes at 37°C, and then plates were washed 4 times with 0.5% Tween PBS wash buffer. Samples and recombinant cytokines for a standard curve were added at 50 µL per well. All samples and standards were run in duplicate. Plates were incubated for 3 hours at RT. Samples were then removed, and plates were washed 4 times with wash buffer. The primary antibody was added at the specified concentration, and incubated for 45 minutes at RT. The plates were washed again (4 times), and the horse radish peroxidase conjugated secondary antibody was applied for 30 minutes at room temperature. The plates were then washed again (8 times) before the TMB substrate solution (Dako, Carpinteria, CA) was added. The reaction was stopped with 0.185 M sulfuric acid (Fisher). The plates were then read at 450 nm. Averages from duplicate wells were calculated.
Statistical analysis. Organ CFUs were analyzed using Wilcoxon/Kruskal-Wallis Tests followed by Dunn procedure for multiple comparisons with JMP software. Significant differences were determined at p<0.05; and standard deviations were reported. For flow cytometry results from BAL and splenocytes, samples were analyzed using one way ANOVA followed by Tukey-Kramer procedure performed using GLIMMIX procedure for SAS (NC, USA).
Results
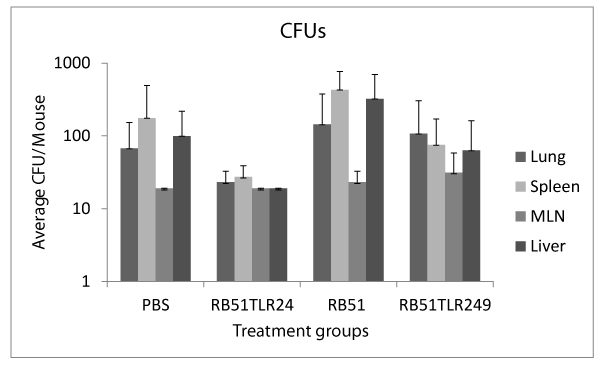
Protection based on colony forming units (CFU): There were no significant differences between treatment groups based on CFUs of any of the organs (Figure 1).
Increased total cell numbers in BAL and spleen by non-protected groups: In the BAL, the RB51 group (1.97 x 105 cells ± 4.35 x 104) had significantly higher total cells versus the PBS (1.94 x 104 cells ± 1.38 x 104) and RB51TLR24 (3.77 x 104 cells ± 3.24 x 103) groups. The RB51TLR249 group (9.52 x 104 cells ± 3.18 x 104) had significantly more cells vs. the PBS treatment. Comparatively, the RB51 (1.52 x 107 cells ± 4.35 x104) and RB51TLR249 (1.42 x107 cells ± 3.18x104) had significantly more splenocytes than the PBS group (8.64 x106 cells ± 1.38x104).
Vaccination induces higher antibody titers in BAL and serum: In both the BAL and serum, post 2308 challenge samples had a mixed IgG2a and IgG1 response, with lower amounts of IgA, suggesting a mixed Th1 and Th2 response against strain RB51 (Figure 2A-E). Antibody production against strain 2308 was lower than against strain RB51. It followed the same pattern, but had lower OD values vs. strain RB51 induced response (data not shown).
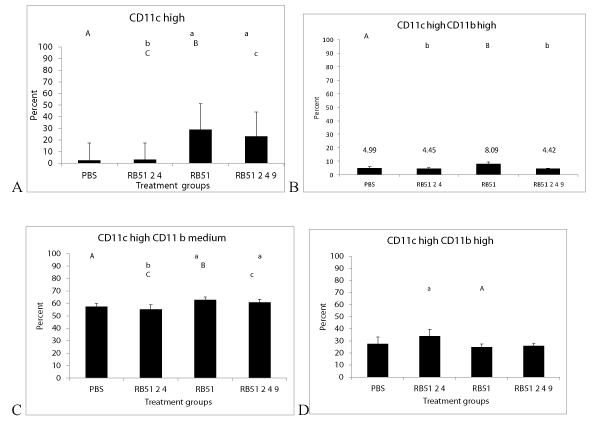
DC recruitment: RB51TLR24 and RB51 had higher levels of CD11b DC whereas RB51TLR249 had increased CD103 DC. In the BAL and spleen, DC subtype (CD103 DC, CD11b, and CD8α resident DC), as well as up regulation of activation markers (MHC class II, CD40 and CD86) were assessed to determine if there were immune correlates of protection and/or differences in vaccine induced responses. DC were identified based on CD11c+ staining. In the BAL, (Figure 3) RB51 and RB51TLR249 had significantly increased CD11c high than PBS and RB51TLR2. RB51 had significantly increased CD11c high CD11b high in BAL compared to RB51 and RB51TLR249. Similarly, in the spleen, RB51 and RB51 TLR249 had increased CD11c high CD11c medium compared to PBS and RB51TLR24. Additionally, RB51TLR24 had increased CD11c high CD11b high vs. RB51.. In the spleen, only RB51TLR24 upregulated CD11c high CD11b cells vs. RB51 and RB51TLR249 group (Figure 3C-D).
In assessing the remaining DC subsets (CD103, CD8 alpha (α)), the RB51TLR249 group had overall significantly greater CD11c low MHC class II high CD103 DC than most other treatment groups in the BAL (Figure 4A-B ). By comparison, in the spleen, the RB51TLR24 and RB51TLR249 groups had greater CD11c high CD8α high than the RB51 group (data not shown). The RB51 and RB51TLR249 groups had increased CD11c low MHC class II high CD8α cells compared to PBS and RBTLR24 groups (Figure 4C), suggesting differences in TLR mediated activation and protection and response to infection.
RB51TLR2 upregulated CD11c high CD86 in BAL (Figure 5A-C) vs. RB51 and RB51TLR249 had increased CD11c low CD40 and CD11c low CD86 CD40. RB51TLR249 and RB51 had increased CD11c high MHC class II low CD40 and CD11c low MHC class II high vs. the PBS and RB51TLR2 groups (Figure 5D-F, data not shown). Additionally, the RB51 group in the spleen had higher CD11c low CD86+ CD40- cells than the RB51 TLR249 group (data not shown). RB51 and RB51TLR249 did not upregulate CD11c compared to RB51TLR24. Additionally, the RB51TLR249 and RB51 groups induced more activation of cells via CD40 expression, while the RB51TLR24 group more consistently upregulated through CD86 expression, potentially due to differences in TLR mediated activation and/or levels of infection.
Infection associated with increased activated T cells: To assess the immune response associated with clearance/chronic infection, identify possible correlates of protection, and determine how the vaccine groups differentially stimulated immunity, lymphocytes were assessed for subsets and activation by flow cytometry. Lymphocyte subsets (CD4, CD8, B cells (B220), and activation/phenotype (CD69 early activation, CD45RB effector, CD62L naïve, CD44 memory, CD25 T-reg or activation) were determined for BAL and spleen samples (Figure 6A-E).
Overall, there was a pattern that the RB51TLR249 had increased CD4 effector and CD8 high activation in the BAL. Correspondingly, there was a decrease in CD4 effector cells in the spleen of RB1TLR249 (Fig 6B-E). Neither PBS nor RB51 groups upregulated CD8 high CD45RB high (data not shown). RB51TLR2 had increased CD4 low CD25 (Figure 6D) and increased CD4 low (data not shown) compared to RB1TLR249, suggesting differences in TLR inducted immune responses as well as levels of infection. Overall, RB51TLR249 groups tended to induce increased CD4 and CD8 CD69 and CD45RB expression, while the RB51TLR24 group induced higher CD25 expression but also CD69 expression in CD4 low and CD8 low T cells. The PBS and RB51 groups did not upregulate CD8 high.
Changes in naïve and memory responses in the spleen: Naïve and memory T-cell status was based on CD62L (naïve) and CD44 (memory) expression in the spleen. For this study, we used CD44 to identify memory cells and CD62L to stain naïve cells as the cell populations were assessed in the spleen. We recognize the central memory cells are CD62L, and are located predominantly in the lymph nodes, not in the spleen. Therefore, for the purpose of this study, we refer to CD62L+ cells as naïve. We recognize that there is the unlikely potential that the CD62 cells in the spleen could be central memory cells. Overall, the PBS and RB51TLR24 groups had higher naïve cells than the RB51 and RB51TLR249 groups in comparison, potentially indicating a naïve response, reflective of lack of induction and declining infection, respectively (Fig 7A-B, data not shown). Besides significant changes noted, the RB51 group was significantly higher than the RB51TLR24 group in CD8 low CD44 high (data not shown). Collectively, there was a tendency for the CD4 and CD8 cells in the PBS and RB51TLR24 groups to have increased CD62 naïve cells (data not shown), and the RB51 and RB51TLR249 groups had increased CD44 memory cells (Figure 7). The functional significance of the CD4 and CD8 high and low subsets needs to be determined.
T and B-cell activation: PBS and RB51TLR24 groups had significantly higher percentages of both B cells (data not shown) and activated (CD69) B cells compared to the RB51 and RB51TLR249 groups (Figure 7C).These data were not associated with differences in antibody production in the serum or IL-4 levels in any organ.
RB51TLR2 induces DC1 CD4 Th1 CD8 cytokine profile in BAL and lung: The specific cytokine profile reflects the nature of the immune response. TNF-α and IL-12, are consistent with a Th1 response, and have been shown to provide protection against Brucella infection [8,17]. Production of IFN-γ, a Th1 cytokine by immune cells, has been shown to be essential in control and clearance of Brucella [18]. Production of IL-4 supports a Th2 response, and IL-10 can be consistent with a Th2 or T-regulatory (T-reg) response. IL-17 is associated with a Th17 response; it has shown to have a role in protection or exacerbation of different infectious diseases, as well as having a role in some non-infectious chronic diseases [19,20].
In the BAL, RB51TL2 induces TNF-α and IL-17 in the BAL, and IL-12 consistent with a DC1 CD4 Th1 CD8 and IL-17 response. RB51TLR9 has increased IL-12 in the BAL (Figure 8-11). In the BAL and lung, IFN-γ and IL-4 were not detected (Figure 9A-D, data not shown). In the spleen, no IL-4 production was detected in any groups (Figure 10A-E, data not shown). In the MLN, significant changes are demonstrated. PBS had significantly increased TNF-alpha and IL-17 in te MLN compared to RB51TLR249 (Figure 11A- F).
Cytokine production from stimulated splenocytes: Insufficient samples were present for TNF-α and IL-17 determination. For IL-12 production, there was a pattern that for media, ConA, and IR2308 stimulated samples, that the RB51 and RB51TLR24 samples were greater than the PBS stimulated splenocytes (Figure 12A). There was a pattern that RB51TLR249 stimulated increased IL-10 in RB51TLR249 vs. RB51 and RB51TLR24 suggesting possible T-regulatory involvement.
For IFN-γ production, there was a pattern for the RB51TLR24, RB51 and RB51TLR249 stimulated splenocytes induced higher IFN-γ than PBS stimulated splenocytes (Fig 12B). Overall, the RB51TLR24 group, and in many cases the RB51 group, induced higher production of Th1 type cytokines (IL-12 and IFN-γ), similar to the pattern of the organ homogenates. The addition of TLR 9 (TLR 2 4 9) did not induce as strong of a Th1 response.
Splenocyte stimulated IL-4 production was present but low (data not shown). There was a pattern with Con A, that the RB51 group was significantly greater than the RB51TLR249 group. With IR2308 stimulation, the PBS and RB51 groups were significantly greater than the RB51TLR249 group. With IRRB51 stimulation, there was a pattern for the PBS group to be greater than the RB51 groups to be significantly greater than the RB51TLR249 groups (data not shown). This suggests a partial Th2 response by the PBS and RB51 groups following infection/challenge.
In assessing the IL-10 response, there was a pattern that RB51TLR24 induced more IL-10 than PBS or RB51TLR249 groups, suggesting possible differences in induction of immunity associated with TLR9 and/or response to infection (Figure 12C).
The total amount of splenocyte supernatants was limited; therefore, some samples (i.e., PBS) could not be tested for IL-17 production. When stimulated with IR2308 and IRRB51, the amount of IL-17 increased dramatically for both the RB51 and RB51TLR249 groups. However, these were the only two groups with samples to test. The production of IL-17 was not significantly different between groups (data not shown). The RB51TLR249 group also induced high IL-17 production when stimulated by HK2308 and HKRB51 (data not shown), however this was the only group tested. The RB51 and RB51TLR249 groups induced IL-17, suggesting a potential role in the immune response associated with vaccination and/or infection.
Discussion
In analyzing our results, and the lack of efficacy of the RB51TLR agonists against strain 2308 challenge, it is apparent that the level of infection in the control mice is lower than our previously published studies [11]. We did back calculate our challenge dose, and it was accurate. Possible explanations for the decreased titer in control, and potentially other mice, would be unknowingly administering a lower dose to all mice through a pipetting error. After examining our records, we did not identify an error in dosing, administration, etc., and despite that the dose in the BALB/c mice is lower than expected, the reported results are statistically significant. We may have seen more differences both in protection and correlates of protection/chronic infection, if the mice had maintained a higher dose of strain 2308. In addition, while the numbers of mice for the study were not extensive, this is the same or similar to other similar publications, and our results are statistically significant [11,21,22].
While not statistically significant, based on clearance, strain RB51 with TLR2 and 4 agonists (RB51TR24 group) appeared to be the most promising. There were significant differences in the immune responses in both treatment groups (RB51TLR24, RB51TLR249), as well as strain RB51 alone, supporting important differences in the pathways, mechanisms of the TLR vaccine induced pathways, and the immune response associated with subsequent infection/challenge.
In assessing the mechanisms of how the different vaccines with TLR agonists induced immune responses, we propose that there appears to be a pattern for both DC subsets and activation, lymphocyte responses as well as cytokine production. Based on our previous study by Surendran et al. [10], we proposed that the addition of the TLR2 or TLR4 agonist with strain RB51 induced immunity against respiratory challenge with strain 2308 was associated with a CD103 DC mediated response. We proposed that the CD103 DC was present in the initial response, and stimulated a protective immune response based on cytokine production in the lung/organs. As infection declined, the CD103 DC and cytokine production decreased, whereas persistently infected mice still had increased CD103 DC and cytokine levels. We proposed that the CD103 DC were most critical for protection in the initial response. In this study, at 2 weeks post-challenge, there appeared to be a role for CD103 as well as possibly CD11b. In this study, we propose but cannot prove that the RB51TLR24 vaccine group had already induced a CD103 response and transitioned to a CD11b response, whereas the RB51TLR249 group still had an increased CD103 response, but had not transitioned. By contrast, the RB51 group, which appeared to overall poorly stimulate a protective response, induces a CD11b response. The exact mechanism for the RB51 response is not clear, but our data suggest that the RB51 induced response may be different than those induced by RB51 with various TLR agonists.
In our model, RB51 and RB51TLR249, had significantly increased CD11c low, CDlow, MHC class II low, CDllc lo MHC class II high, CD11c low CD40 vs. the PBS and RB51TLR24 groups. By comparison, RB51TLR2 had increased CD11c high, (CD11c I cd86 high, CD49) in the BAL and increased CD11c CD86+ cells. We proposed that because of differences in TLR mediated activation and infection, that RB51TLR249 and RB51 activate cells in response to infection differently than RB51TLR24. In other models, a role has been shown for the CD11c high cells to be more functional with respect to activating T-cells [23-27]. Additional studies are needed to identify the differences in these DC subsets in protection.
Some of the differences in DC activation and cytokine production within different organs may reflect the differential pathways by which the vaccines +/- TLR agonists induced immune responses and response to challenge/infection. For instance, in the BAL, the RB51TLR24 group induced higher levels of TNF-α and IL-17, but non-significantly lower levels of IL-12 vs. the RB51TLR249 group at this time point. Additionally, splenocytes from the RB51TLR24 vaccinated mice consistently had increased IFN-ɣ production vs. the RB51TLR249 stimulated splenocytes. This supports the overall higher CD4 Th1 CD8 Tc1 response by the RB51TLR24 vs. other groups. The question still remains as to why overall clearance by the RB51TLR24 group was not higher. Possible explanations include that the RB51TLR24 group induced response may not be great enough (i.e. it is a DC1 CD4 Th1 CD8 Tc1 response, but it is not high enough, or that some aspect of combining the TLR2 and 4 agonists stimulated different types of responses, which limited the overall response). It is possible that our combined dose of TLR agonists was not optimal despite our and other previous studies (REF).
In examining more closely the differences between the RB51, RB51TLR24, RB51TR249 groups for mechanisms associated with the differential TLR activation, Chandran et al. [28], demonstrated that TLR2 agonists combined with influenza HA peptide stimulated IL-2 and Il-17 dependent activation, whereas the TLR4 agonist with HA peptide stimulated decreased numbers of CD4 cells, but higher percentages of IFN-gamma producing cells. Other studies have demonstrated a role for TLR2 in Th1, Th2, Th17 or T-reg responses [10,12,20,28,29]. Additionally, Mori et al., have also demonstrated a role for TLR9 and IL-17 [30].
Our previous studies in TLR KO mice demonstrated that the TNF-α production was TLR2 and TLR9 dependent, whereas IL-12 was TLR2 and TLR4 dependent [10,11]. Based on our data in this study, in the BAL, we see that the RB51TLR24 pathway induces significantly increased TNF-α production vs. the RB51TLR249 pathway, and also the former has increased IL-17 vs. RB51 without TLR agonists. These data support the ability of the RB51TLR24 group to promote a stronger DC1 response vs. the RB51TLR249 group.
In regards to the subsequent T-cell response, strain RB51 has previously demonstrated to show a role for CD25 cells in response to infection. It is not clear if the CD25 response is a primary response associated with infection, which could potentially limit the protective immune response vs. a mechanism for resolving the immune response. Several investigators (Pasquali et al. [31]., Xavier et al., [32], Corsetti et al [33], have demonstrated a role for some combination of CD4, CD25 and IL-10 in limiting the protective immune response. Collectively, these studies support that the RB51TLR24 group with the increased CD4 CD25 population in our model, could be limiting the protective immune response.
If Xavier/Tsolis and Corsetti et al’s theories are accurate for our models, we would expect differences in IL-10 responses and clearance. Our time point was 2 wks post challenge, and ideal time points would be earlier. Thus, an alternative explanation, based on Martirosya et al.’s study [34], in which they determined that there is a CD4 CD25 CD62 CD44 CD43 IFN-gamma producing cytotoxic cells in infection. The functionality of the cells must be assessed in order to define their role in regulating (promoting/inhibiting) the immune response to Brucella [35,36].
Based on these data, we propose that the differences in DC function are also associated with increased DC activation and ultimately T-cell activation and function and protection. Although additional studies are needed to further define the mechanisms of the TLR mediated immune responses, potential protection and also lack of protection, these data do support that the RB51TLR24 responses can upregulate immunity. Enhancement of immunity is needed to upregulate protection. Additional studies are warranted on the mechanisms by which the TLRs activate immunity and protection, as well as the roles of IL-10, CD4 CD25 and Th17 cells in immunity.
This project was funded through internal grant proposals to the Virginia Maryland College of Veterinary Medicine, Blacksburg, VA.
- Pappas G, Papadimitriou P, Akritidis N, Christou L, Tsianos EV (2006) The new global map of human brucellosis. Lancet Infect Dis 6: 91-99. Link: https://tinyurl.com/y5momp3c
- Olsen SC, Waters WR, Stoffregen WS (2007) An Aerosolized Brucella spp. Challenge Model for Laboratory Animals. Zoonoses and Public Health 54: 281-285. Link: https://tinyurl.com/yyvryaxb
- Vemulapalli R, He Y, Cravero S, Sriranganathan N, Boyle SM, et al. (2000) Overexpression of Protective Antigen as a Novel Approach To Enhance Vaccine Efficacy of Brucella abortusStrain RB51. Infection and Immunity 68: 3286-3289. Link: https://tinyurl.com/yxzevfmd
- Pasquali P, Rosanna A, Pistoia C, Petrucci P, Ciuchini F (2003) Brucella abortus RB51 induces protection in mice orally infected with the virulent strain B. abortus 2308. Infect Immun 71: 2326-2330. Link: https://tinyurl.com/y34ugrv2
- Surendran N, Sriranganathan N, Lawler H, Boyle SM, Hiltbold EM, et al. (2011) Efficacy of vaccination strategies against intranasal challenge with Brucella abortus in BALB/c mice. Vaccine 29: 2749-2755. Link: https://tinyurl.com/y694d5zq
- Kahl-McDonagh M, Arenas-Gamboa A, Ficht T (2007) Aerosol infection of BALB/c mice with Brucella melitensis and Brucella abortus and protective efficacy against aerosol challenge. Infection and Immunity 10: 4923-4932. Link: https://tinyurl.com/yyx47tv9
- Billard E, Dornand J, Gross A (2007) Interaction of Brucella suis and Brucella abortus Rough Strains with Human Dendritic Cells. Infection and Immunity 75: 5916-5923. Link: https://tinyurl.com/yy748kbu
- Billard E, Dornand J, Gross A (2007) Brucella suis Prevents Human Dendritic Cell Maturation and Antigen Presentation through Regulation of Tumor Necrosis Factor Alpha Secretion. Infection and Immunity 75: 4980-4989. Link: https://tinyurl.com/yxs9b75l
- Surendran N, Hiltbold EM, Heid B, Sriranganathan N, Boyle SM, et al. (2011) Live Brucella abortus rough vaccine strain RB51 stimulates enhanced innate immune response in vitro compared to rough vaccine strain RB51SOD and virulent smooth strain 2308 in murine bone marrow-derived dendritic cells. Vet Microbiol 147: 75-82. Link: https://tinyurl.com/yxntawtm
- Surendran N, Hiltbold EM, Heid B, Akira S, Standiford TJ, et al. (2012) Role of TLRs in Brucella mediated murine DC activation in vitro and clearance of pulmonary infection in vivo. Vaccine 30: 1502-1512. Link: https://tinyurl.com/y5xmzhlu
- Surendran N, Sriranganathan N, Boyle SM, Hiltbold EM, Tenpenny N, et al. (2013) Protection to respiratory challenge of Brucella abortus strain 2308 in the lung. Vaccine 31: 4103-4110. Link: https://tinyurl.com/y6gf3oqn
- Campos MA, Rosinha GMS, Almeida IC, Salgueiro XS, Jarvis BW, et al. (2004) Role of Toll-Like Receptor 4 in Induction of Cell-Mediated Immunity and Resistance to Brucella abortus Infection in Mice. Infection and Immunity 72: 176-186. Link: https://tinyurl.com/y5mdomfc
- Weiss D, Takeda K, Akira S, Zychlinsky A, Moreno E (2005) MyD88, but not toll like receptors 4 and 2, is required for efficient clearance of Brucella abortus. Infection and Immunity 73: 5137-5143. Link: https://tinyurl.com/y3z9xvlv
- Huang L-Y, Aliberti J, Leifer CA, Segal DM, Sher A, et al. (2003) Heat-Killed Brucella abortus Induces TNF and IL-12p40 by Distinct MyD88-Dependent Pathways: TNF, Unlike IL-12p40 Secretion, Is Toll-Like Receptor 2 Dependent. The Journal of Immunology 171: 1441-1446. Link: https://tinyurl.com/y4yda786
- Vemulapalli R, Contreras A, Sanakkayala N, Sriranganathan N, Boyle SM, et al. (2004) Enhanced efficacy of recombinant Brucella abortus RB51 vaccines against B. melitensis infection in mice. Vet Microbiol 102: 237-245. Link: https://tinyurl.com/y4twstbc
- Surendran N, Zimmerman K, Seleem MN, Sriranganathan N, Boyle SM, et al. (2010) Ability of Brucella abortus rough vaccine strains to elicit DC and innate immunity in lung using a murine respiratory model. Vaccine 28: 7009-7015. Link: https://tinyurl.com/y5zks8nb
- Grillo MJ, Blasco JM, Gorvel JP, Moriyon I, Moreno E (2012) What have we learned from brucellosis in the mouse model? Vet Res 43: 29. Link: https://tinyurl.com/y4nfbndo
- Fernandes DM, Jiang X, Jung JH, Baldwin CL (1996) Comparison of T cell cytokines in resistant and susceptible mice infected with virulent Brucella abortus strain 2308. FEMS Immunol Med Microbiol 16: 193-203. Link: https://tinyurl.com/y2zg4o2f
- Clapp B, Skyberg JA, Yang X, Thornburg T, Walters N, et al. (2011) Protective live oral brucellosis vaccines stimulate Th1 and th17 cell responses. Infect Immun 79: 4165-4174. Link: https://tinyurl.com/y4dvff3w
- Kolls JK, Khader SA (2010) The role of Th17 cytokines in primary mucosal immunity. Cytokine & growth factor reviews 21: 443-448. Link: https://tinyurl.com/yyubvoe2
- Jain-Gupta N, Contreras-Rodriguez A, Smith G, Garg V, Witonsky S, et al. (2014) Immunotherapeutics to prevent replication of Brucella in a treatment failure mouse model. Vaccine 32: 918-923. Link: https://tinyurl.com/yyrw8t4c
- Sanakkayala N, Sokolovska A, Gulani J, HogenEsch H, Sriranganathan N, et al. (2005) Induction of antigen specific Th1 type immune responses by gamma-irradiated recombinant Brucella abortus RB51. Clin Diagn Lab Immunol 12: 1429-1436. Link: https://tinyurl.com/y5ppbmn2
- Periasamy P, Petvises S, O’Neill H (2013) Development of two distinct dendritic like APCs in the context of splenic stroma. Frontiers in Immunology 4: 1-11. Link: https://tinyurl.com/y6olw9wl
- Furuhashi K, Suda T, Hasegawa H, Suzuki Y, Hashimoto D, et al. (2012) Mouse Lung CD103+ and CD11bhigh Dendritic Cells Preferentially Induce Distinct CD4+ T-Cell Responses. Am J Respir Cell Mol Biol 46: 165-172. Link: https://tinyurl.com/y2dt4ry5
- Suzuki Y, Suda T, Furuhashi K, Shibata K, Hashimoto D, et al. (2012) Mouse CD11bhigh lung dendritic cells have more potent capability to induce IgA than CD103+ lung dendritic cells in vitro. Am J Respir Cell Mol Biol 46: 773-780. Link: https://tinyurl.com/y6dzybu2
- Shao Z, Bharadwaj AS, McGee HS, Makinde TO, Agrawal DK (2009) Fms-like tyrosine kinase 3 ligand increases a lung DC subset with regulatory properties in allergic airway inflammation. J Allergy Clin Immunol 123: 917-924.e2. Link: https://tinyurl.com/y3hd2cbn
- Ganesh BB, Cheatem DM, Sheng JR, Vasu C, Prabhakar BS (2009) GM-CSF-induced CD11c+CD8a--dendritic cells facilitate Foxp3+ and IL-10+ regulatory T cell expansion resulting in suppression of autoimmune thyroiditis. Int Immunol 21: 269-282. Link: https://tinyurl.com/y4dqux8w
- Chandran SS, Verhoeven D, Teijaro JR, Fenton MJ, Farber DL (2009) TLR2 engagement on dendritic cells promotes high frequency effector and memory CD4 T cell responses. Journal of immunology 183: 7832-7841. Link: https://tinyurl.com/y5g4rwk9
- Sheng KC, Day S, Wright MD, Stojanovska L, Apostolopoulos V (2013) Enhanced Dendritic Cell-Mediated Antigen-Specific CD4+ T Cell Responses: IFN-Gamma Aids TLR Stimulation. Journal of drug delivery 2013: 516749. Link: https://tinyurl.com/y679gh7j
- Mori A, Oleszycka E, Sharp F, Coleman M, Ozasa Y, et al. (2012) The vaccine adjuvant alum inhibits IL-12 by promoting PI3 kinase signaling while chitosan does not inhibit IL-12 and enhances Th1 and Th17 responses. Eur J Immunol 42: 2709-2719. Link: https://tinyurl.com/yxzu5t8n
- Pasquali P, Thorton A, Vendetti S, Pistoia C, Petrucci P, et al. (2010) CD4+CD25+ T regulatory cells limit effector T cells and favor the progression of brucellosis in BALB/c mice. Microbes Infection 12: 3-10. Link: https://tinyurl.com/y2zsvqrd
- Xavier MN, Winter MG, Spees AM, Nguyen K, Atluri VL, et al. (2013) CD4+ T cell-derived IL-10 promotes Brucella abortus persistence via modulation of macrophage function. PLoS pathogens 9: e1003454. Link: https://tinyurl.com/yxm2sp7t
- Corsetti PP, de Almeida LA, Carvalho NB, Azevedo V, Silva TM, et al. (2013) Lack of endogenous IL-10 enhances production of proinflammatory cytokines and leads to Brucella abortus clearance in mice. PLoS One 8: e74729. Link: https://tinyurl.com/y6ouobhy
- Martirosyan A, Von Bargen K, Gorvel A, Zhao W, Hanniffy S, et al. (2013) In vivo identification and characterization of CD4+ cytotoxic T-cells induced by virulent Brucella abortus infection. PLoS One 8: e8508. Link: https://tinyurl.com/yxrzwo48
- Arenas-Gamboa AM, Rice-Ficht AC, Kahl-McDonagh MM, Ficht TA (2011) Protective Efficacy and Safety of Brucella melitensis 16MΔmucR against Intraperitoneal and Aerosol Challenge in BALB/c Mice. Infection and Immunity 79: 3653-3658. Link: https://tinyurl.com/y2jy57on
- deAlmeida L, Macedo G, Marinho F, Gomes M, Corsetti P, et al. (2013) Toll like receptor 6 plays an important role in host innate resistance to Brucella abortus infection in mice. Infection and Immunity 81: 1654-1662. Link: https://tinyurl.com/yyhnncfm
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.




 Save to Mendeley
Save to Mendeley
