Journal of Surgery and Surgical Research
Staged feminizing genitoplasty with total urogenital sinus mobilization
Fatih Akbiyik*
Cite this as
Akbiyik F (2022) Staged feminizing genitoplasty with total urogenital sinus mobilization. J Surg Surgical Res 8(3): 036-040. DOI: 10.17352/2455-2968.000151Copyright
© 2022 Akbiyik F. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Background : The diagnosis and treatment of individuals with Disorders of Sexual Development is a complex process and requires a multidisciplinary approach. Each individual should be evaluated objectively and the treatment process of each individual has its own unique differences. The aim of this study is to discuss the effectiveness of staged feminizing genitoplasty operations using the total urogenital mobilization technique.
Material and methods : Hospital records of patients who underwent vaginoplasty using the TUM technique between 2014 and 2019 by a single surgeon in a pediatric surgery center of a tertiary pediatric hospital were retrospectively reviewed.
Results : All ten patients who underwent TUM had 46 XX chromosomes. The TUM procedure for vaginoplasty was performed in all patients by the author. A clitorolabioplasty had been previously performed in six patients with congenital adrenal hyperplasia. The follow-up period of the patients was 1-6 years. No serious complications developed in any of the patients. Neither infection nor tissue necrosis occurred. A second surgical procedure was not required for urinary fistula, vaginal stenosis, urinary incontinence, or early suture dehiscence.
Conclusion : This study shows that vaginoplasty can be performed in a single session in infancy for patients with low confluence and a short Urogenital Sinus (UGS). Apart from this, postponing vaginoplasty surgeries to the adolescence period and performing UGS mobilization surgery seem to carry successful results.
Introduction
The diagnosis and treatment of individuals with Disorders of Sexual Development (DSD) is a complex process and requires a multidisciplinary approach. In this complex situation, medical, psycho-social and ethical situations should be considered. Each individual should be evaluated objectively. Therefore, the treatment process of each individual has its own unique differences.
There have been intense debates on this subject, from nomenclature to the time of surgery and the surgical technique; however, there remains no consensus [1,2]. While there are those who recommend an early and single-session surgery [3,4] and those who recommend that the surgery be performed gradually [5,6], studies have advocated for postponing all surgeries until the patients reach an age where they can decide on their own [7]. In terms of surgical technique, different techniques have been suggested, from flap vaginoplasty to total urogenital sinus mobilization (TUM) [8].
In this study, staged feminizing genitoplasty operations with the TUM technique are presented and their results are discussed in the light of previous studies.
Materials and methods
Hospital records were retrospectively reviewed for patients who underwent vaginoplasty with a perineal approach using the TUM technique by the author between 2014 and 2019 in the Pediatric Surgery Clinic of Ankara Children’s Hematology and Oncology Training Hospital (later on moved to Ankara City Hospital Children’s Hospital). The information collected from the patient's records was including demographics, radiological imaging, the type of operation, and the follow-up period.
The patients were questioned regarding the age of menarche of the mother and any sisters. The patients also received a physical examination to determine their Tanner classification and to perform measurements of ovarian volume, uterine volume and endometrial thickness by ultrasound imaging, which were performed to estimate the age of menarche. A time for the operation was planned for individuals just before the predicted menarche or menstruation.
Technique
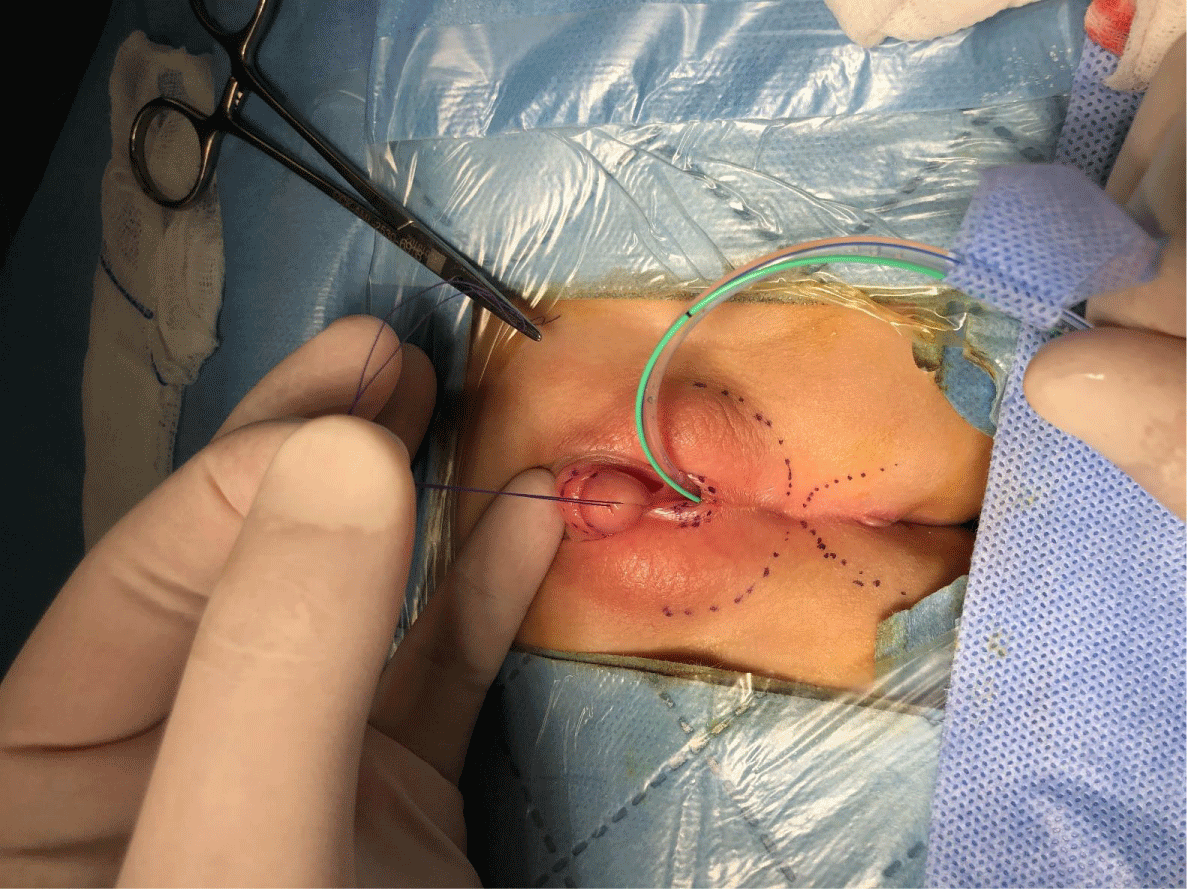
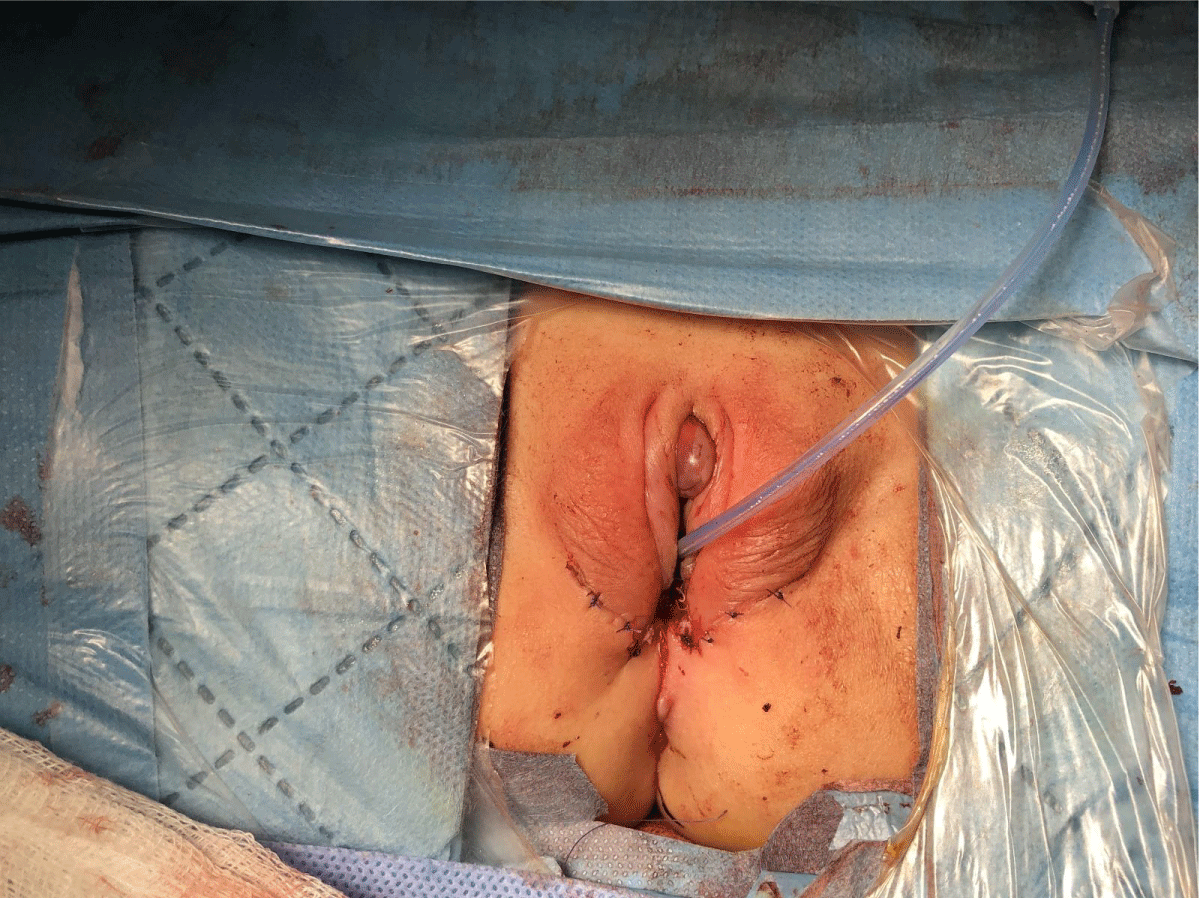
Before the operation, all patients underwent a cystoscopy in the form of Urogenital Sinus (UGS) endoscopy under general anesthesia. At the cystoscopy, a urinary catheter to the bladder and a Fogarty catheter to the vagina was placed. Vaginoplasties were performed with the TUM technique that was previously described by Ludwikowski, et al. and UGS was preserved as vaginal flep [9] (Figures 1-3). A small gauze dressing was placed on the genitalia and removed the next day.
The urinary catheter was retained for 10 days and taken off just before hospital discharge. Pain was controlled with analgesics. Patients were called for examinations at the clinic in the 2nd, 4th and 12th weeks and 6th and 12th months postoperative period. In the 12th week, all patients were examined and vaginal calibration was performed with Hegar dilatator under sedation.
Median age, median UGS length, and median follow-up duration were used for the statistical method.
Ethical approval was obtained from the Ankara City Hospital Ethical Committee (Number: E221-519).
Results
Ten patients who underwent TUM were included in the study, other patients who were operated with different techniques are excluded. Ages of patients were between 6-16 years (median: 12 years). TUM surgery was performed on nine patients with a diagnosis of CAH, while in one patient with a diagnosis of Mc Kusick-Kaufmann syndrome, who had numerous previous operations in another center.
Six patients were previously operated by the author for clitorolabioplasty in their early childhood as the two-stage vaginoplasty plan, since the UGS was long and they were waiting for vaginoplasty surgery. Due to faled vaginoplasty on two patients with CAH, the TUM was performed.
Cystoscopic evaluation showed that the shortest UGS length was 2.5 cm, while the longest was 4.5 cm (median: 3.5 cm). The data of the patients is shown in Table 1.
Of the five patients without preoperative menarche; score of Tanner Breast were 3-4, volume of uterus was 11-18 cm3 (median: 16.1 cm3), endometrial thickness 4-9 mm (median: 5 mm) and ovarian volumes were 3-6 cm3 (median: 4 cm3). These patients began to menstruate within 1–5 months (median: 3.6 months).
Only one complication, mild vaginal-entrance stenosis developed in one patient. She was diagnosed by Mc Kusick Kaufmann Syndrome and had multiple surgeries before. Her stenosis was solved by minor cut-back surgery. Infection and tissue necrosis did not occur. A second surgical procedure was not required for urinary fistula, urinary incontinence or early suture dehiscence.
There was no vaginal stenosis at the postoperative 3rd month exanimation and vaginal calibration under sedation. The follow-up period of the patients was 1-6 years (median: 4 years). No urinary infections and no urinary incontinence occurred in any of the patients. None of the patients required a vaginal dilatation.
Discussion
In a feminizing genitoplasty, there are several aims, including creating a genital appearance compatible with the patient’s gender, providing an anatomical and urinary tract that will not cause incontinence and ensuring a genital structure that will fulfil sexual and reproductive functions during adult life [10].
There is no consensus on the timing and the surgical technique to perform these operations [2]. For example, at the time of diagnosis, a single-session operation can be performed during infancy.
However, if the operation involves the genital appearance, a genitoplasty can either be performed or the operation can be completely postponed.
The most important anatomical factor that will affect vaginoplasty is the confluence of the urethra and vagina, which may be low or high, and the length of the UGS [11]. This will also affect the surgical technique and results.
Many reports have been published advocating early surgery. These have argued that this will eliminate parental stress and the procedure can be finalized with a single surgery [3,4]. It is an important advantage that the surgery is completed before the patient suffers psychological trauma, as with in hypospadias surgery. Moreover, surgery is easier with the benefit of maternal estrogen during the infantile period [12].
The biggest argument of those who advocate a vaginoplasty in late childhood is that vaginoplasties performed at an early age mostly require revisions later. There are studies that have reported a high rate of complications and revisions after early operations [5,6]. Considering these reports, it has been recommended that a clitorolabioplasty be performed, and if necessary for cosmetic reasons, this should be performed at an early age in a virialized patient and then a prepubertal-pubertal vaginoplasty operation can be performed at a later date.
It has been suggested that pubertal estrogen will facilitate the operation. Moreover, it has been claimed that postponing a vaginoplasty to a later period, and allowing hydrometrocolpos, will ensure sufficient dilatation that facilitates the vaginoplasty operation [13]. In the present study, the general approach was a staged feminizing genitoplasty.
Estrogen is known to play an important role in coagulation, homeostasis and the overall inflammatory process [14]. Various animal experiments have shown that estrogen increases the blood supply and elasticity of vaginal tissues and accelerates wound healing [15,16]. Alternatively, it has been reported that preoperative vaginal estrogen administration in the postmenopausal period increases the synthesis of mature collagen and decreases the degrading enzyme activity. It also strengthens the vaginal tissue by increasing both the integrity of the connective tissue and the chances of surgical success [17]. In this study, patients were followed up and waited for vaginoplasty until adolescence since the facilitating effect of estrogen was expected at a later time. During this period, some parameters were recorded, such as questioning the menarche age of the mother and other sisters. Also, during this period, patients received a physical examination to determine their Tanner classification and measurements of ovarian size, uterine volume and endometrial thickness were determined using ultrasound imaging [18,19].
Many techniques have been described for vaginoplasty. A U-flap vaginoplasty, described by Fortunoff, et al. can be considered an important step in these surgeries [20]. Hendren, et al. later described a pull-through vaginoplasty [18]. Passerini’ technique and anterior sagittal transanorectal approach (ASTRA), are among the techniques described [21,22]. TUM operations were described by Pena to correct the cloacal anomaly, while Ludwikowski et al. suggested using these for vaginoplasty [9,23]. Rink, et al. also suggested a partial urogenital sinus mobilization and showed that the sinus mucosa excised by Pena could be used for repair [24]. Intestinal substitutions can also be used for vaginoplasty. Undoubtedly, a combination of these techniques can also be applied.
Bailez, et al. reported that TUM achieves good results with a combination of different techniques in a study involving 55 patients [11]. Ludwikowski, et al. reported adapting TUM for DSD and stated that it would be suitable for cases where the UGS is ≥ 3 cm and that it would reduce potential urethral innervation damage and surgical times since a urethral and vaginal separation is not needed [9]. It can be considered that a non-intensive dissection and U flap vaginoplasty would be sufficient with a UGS ≤ 2–2.5 cm.
Although Palmer et al. have reported that a TUM or partial urogenital mobilization [PUM] did not increase urinary incontinence in patients [25]. Stites, et al. have reported they prefer a PUM instead of a TUM because of severe urinary incontinence after a TUM. There were no incontinence complaints in any of presented patients. Although there are some concerns about continence, it is clear that urogenital sinus mobilization is a positive step in feminizing genitoplasty.
TUM looks promising with its early results and has become increasingly popular in recent years. Ludwikowski and Gonzales also advocate the feminizing genitoplasty, which can be performed in a single session with TUM [26]. In the same article, they drew attention to the word “total” in TUM and emphasized the integrity concept by saying “‘total’ refers to an en bloc dissection and not to the extent of the proximal dissection”. The survey conducted by Yankovic et al. found a significant portion of the participating surgeons declared that a PUM or TUM gave better results in their personal experience [27-30].
Although knowledge concerning the surgical technique has increased, there is no consensus on performing surgery in a single session or in stages. In this study, six patients underwent clitorolabioplasty in infancy and vaginoplasty with the TUM technique during adolescence. The patients were followed up without any problems. On the other hand, a re-vaginoplasty was performed with the TUM technique in two patients who underwent a single-session clitorolabiovaginoplasty in childhood and whose vaginoplasty was unsuccessful. These results support the view that a staged vaginoplasty and TUM technique give good results.
Carrying out in a single center by a single surgeon with a single surgical technique is the strength of this study. On the other hand, not being a comparative study with other techniques is the limitation of this study.
Conclusion
This study shows that vaginoplasty can be performed in a single session at an early age in patients with low confluence and short UGS, but in patients with long UGS, postponing vaginoplasty operations until puberty and performing TUM technique will yield successful results.
The author would like to thank to Prof. Dr. Hakan Çavuşoğlu, MD and Ulfet Irdem Köse, MD for their kind support in this research.
Ethical consideration
Ethical approval was obtained from the Ankara City Hospital Ethical Committee (Number: E221-519).
- Viau-Colindres J, Axelrad M, Karaviti LP; Texas Children’s Hospital Gender Medicine Clinic. Bringing Back the Term "Intersex". Pediatrics. 2017 Nov;140(5):e20170505. doi: 10.1542/peds.2017-0505. PMID: 29070532.
- Lee PA, Nordenström A, Houk CP, Ahmed SF, Auchus R, Baratz A, Baratz Dalke K, Liao LM, Lin-Su K, Looijenga LH 3rd, Mazur T, Meyer-Bahlburg HF, Mouriquand P, Quigley CA, Sandberg DE, Vilain E, Witchel S; Global DSD Update Consortium. Global Disorders of Sex Development Update since 2006: Perceptions, Approach and Care. Horm Res Paediatr. 2016;85(3):158-80. doi: 10.1159/000442975. Epub 2016 Jan 28. Erratum in: Horm Res Paediatr. 2016;85(3):180. Koopman, Peter [added]. Erratum in: Horm Res Paediatr. 2016;86(1):70. PMID: 26820577.
- Braga LH, Pippi Salle JL. Congenital adrenal hyperplasia: a critical appraisal of the evolution of feminizing genitoplasty and the controversies surrounding gender reassignment. Eur J Pediatr Surg. 2009 Aug;19(4):203-10. doi: 10.1055/s-0029-1233490. Epub 2009 Aug 19. PMID: 19693746.
- Vidal I, Gorduza DB, Haraux E, Gay CL, Chatelain P, Nicolino M, Mure PY, Mouriquand P. Surgical options in disorders of sex development (dsd) with ambiguous genitalia. Best Pract Res Clin Endocrinol Metab. 2010 Apr;24(2):311-24. doi: 10.1016/j.beem.2009.10.004. PMID: 20541154.
- Alizai NK, Thomas DF, Lilford RJ, Batchelor AG, Johnson N. Feminizing genitoplasty for congenital adrenal hyperplasia: what happens at puberty? J Urol. 1999 May;161(5):1588-91. PMID: 10210421.
- Creighton SM, Minto CL, Steele SJ. Objective cosmetic and anatomical outcomes at adolescence of feminising surgery for ambiguous genitalia done in childhood. Lancet. 2001 Jul 14;358(9276):124-5. doi: 10.1016/S0140-6736(01)05343-0. PMID: 11463417.
- Gardner M, Sandberg DE. Navigating Surgical Decision Making in Disorders of Sex Development (DSD). Front Pediatr. 2018 Nov 19;6:339. doi: 10.3389/fped.2018.00339. PMID: 30510925; PMCID: PMC6252317.
- Piaggio LA. Congenital Adrenal Hyperplasia: Review from a Surgeon's Perspective in the Beginning of the Twenty-First Century. Front Pediatr. 2014 Jan 2;1:50. doi: 10.3389/fped.2013.00050. PMID: 24400298; PMCID: PMC3877834.
- Ludwikowski B, Oesch Hayward I, González R. Total urogenital sinus mobilization: expanded applications. BJU Int. 1999 May;83(7):820-2. doi: 10.1046/j.1464-410x.1999.00995.x. PMID: 10368205.
- Joint ESPE/LWPESCAH workinggroup. Consensus statementon21- hydroxylase deficiency from the European society for paediatric endocrinology and the Lawson Wilkins Pediatric Endocrine Society. Horm Res 2002; 58:188–95. https://doi.org/10.1159/000065490 5.
- Bailez MM, Cuenca ES, Dibenedetto V. Urinary continence following repair of intermediate and high urogenital sinus [UGS] in CAH. Experience with 55 cases Front Pediatr 2014; 2: 67. https://doi.org/10.3389/fped.2014.00067.
- Hemesath TP, de Paula LCP, Carvalho CG, Leite JCL, Guaragna-Filho G, Costa EC. Controversies on Timing of Sex Assignment and Surgery in Individuals With Disorders of Sex Development: A Perspective. Front Pediatr. 2019 Jan 10;6:419. doi: 10.3389/fped.2018.00419. PMID: 30687685; PMCID: PMC6335325.
- Guarino N, Scommegna S, Majore S, Rapone AM, Ungaro L, Morrone A, Grammatico P, Marrocco GA. Vaginoplasty for disorders of sex development. Front Endocrinol (Lausanne). 2013 Mar 11;4:29. doi: 10.3389/fendo.2013.00029. PMID: 23483838; PMCID: PMC3593621.
- Horng HC, Chang WH, Yeh CC, Huang BS, Chang CP, Chen YJ, Tsui KH, Wang PH. Estrogen Effects on Wound Healing. Int J Mol Sci. 2017 Nov 3;18(11):2325. doi: 10.3390/ijms18112325. PMID: 29099810; PMCID: PMC5713294.
- Ripperda CM, Maldonado PA, Acevedo JF, Keller PW, Akgul Y, Shelton JM, Word RA. Vaginal estrogen: a dual-edged sword in postoperative healing of the vaginal wall. Menopause. 2017 Jul;24(7):838-849. doi: 10.1097/GME.0000000000000840. PMID: 28169915; PMCID: PMC5484719.
- Akbiyik F, Mesci ÇG, Çavuşoğlu YH. Estrogen as primary factor in vaginal healing in rats. Eur Rev Med Pharmacol Sci. 2022 Mar;26(5):1508-1512. doi: 10.26355/eurrev_202203_28215. PMID: 35302195.
- Rahn DD, Good MM, Roshanravan SM, Shi H, Schaffer JI, Singh RJ, Word RA. Effects of preoperative local estrogen in postmenopausal women with prolapse: a randomized trial. J Clin Endocrinol Metab. 2014 Oct;99(10):3728-36. doi: 10.1210/jc.2014-1216. Epub 2014 Jun 20. PMID: 24947034; PMCID: PMC4184065.
- Ersen A, Onal H, Yildirim D, Adal E. Ovarian and uterine ultrasonography and relation to puberty in healthy girls between 6 and 16 years in the Turkish population: a cross-sectional study. J Pediatr Endocrinol Metab. 2012;25(5-6):447-51. doi: 10.1515/jpem-2012-0014. PMID: 22876537.
- Hagen CP, Mouritsen A, Mieritz MG, Tinggaard J, Wohlfahrt-Veje C, Fallentin E, Brocks V, Sundberg K, Jensen LN, Juul A, Main KM. Uterine volume and endometrial thickness in healthy girls evaluated by ultrasound (3-dimensional) and magnetic resonance imaging. Fertil Steril. 2015 Aug;104(2):452-9.e2. doi: 10.1016/j.fertnstert.2015.04.042. Epub 2015 Jun 6. PMID: 26051091.
- Fortunoff S, Lattimer JK, Edson M. Vaginoplasty technique for female pseudohermaphrodites. Surg Gynecol Obstet. 1964 Mar;118:545-8. PMID: 14133087.
- Dòmini R, Rossi F, Ceccarelli PL, De Castro R. Anterior sagittal transanorectal approach to the urogenital sinus in adrenogenital syndrome: preliminary report. J Pediatr Surg. 1997 May;32(5):714-6. doi: 10.1016/s0022-3468(97)90012-9. PMID: 9165458.
- Passerini-Glazel G. Feminizing genitoplasty. J Urol 1996; 161:1592-3. https://doi.org/10.1016/ s0022-5347[05]68987-2.
- Peña A. Total urogenital mobilization--an easier way to repair cloacas. J Pediatr Surg. 1997 Feb;32(2):263-7; discussion 267-8. doi: 10.1016/s0022-3468(97)90191-3. PMID: 9044134.
- Hendren H,Crawford J. Adreno genital syndrome: the anatomy of the anomaly and its repair. Some new concepts. J Pediatr Surg 1969;4:49–58 https://doi.org/10.1016/0022-3468[69]90183-3
- Palmer BW, Trojan B, Griffin K, Reiner W, Wisniewski A, Frimberger D, Kropp BP. Total and partial urogenital mobilization: focus on urinary continence. J Urol. 2012 Apr;187(4):1422-6. doi: 10.1016/j.juro.2011.12.012. Epub 2012 Feb 16. PMID: 22341265.
- Ludwikowski BM, González R. The Surgical Correction of Urogenital Sinus in Patients with DSD: 15 Years after Description of Total Urogenital Mobilization in Children. Front Pediatr. 2013 Nov 21;1:41. doi: 10.3389/fped.2013.00041. PMID: 24400287; PMCID: PMC3864266.
- Yankovic F, Cherian A, Steven L, Mathur A, Cuckow P. Current practice in feminizing surgery for congenital adrenal hyperplasia; a specialist survey. J Pediatr Urol. 2013 Dec;9(6 Pt B):1103-7. doi: 10.1016/j.jpurol.2013.03.013. Epub 2013 May 18. PMID: 23693144.
- Akbiyik F, Tiryaki T, Şenel, E Mambet, Livanelioğlu Z, Atayurt H. Feminizing genitoplasty: an evaluation of 41 patients in 8 years. Turk J Med Sci 2010; 40 (5): 813-818. https://doi.org/10.3906/ sag-1002-653.
- Rink RC, Metcalfe PD, Kaefer MA, Casale AJ, Meldrum KK, Cain MP. Partial urogenital mobilization: a limited proximal dissection. J Pediatr Urol. 2006 Aug;2(4):351-6. doi: 10.1016/j.jpurol.2006.04.002. Epub 2006 Jul 10. PMID: 18947635.
- Stites J, Bernabé KJ, Galan D, Felsen D, Poppas DP. Urinary continence outcomes following vaginoplasty in patients with congenital adrenal hyperplasia. J Pediatr Urol. 2017 Feb;13(1):38.e1-38.e7. doi: 10.1016/j.jpurol.2016.10.012. Epub 2016 Nov 22. PMID: 27932079.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.



 Save to Mendeley
Save to Mendeley
