Journal of Surgery and Surgical Research
Back to Basics – The best approach in reconstructive surgery to tide over the COVID pandemic crisis
Mainak Mallik, Sunil Kumar Rout* and Ranjit Kumar Sahu
Cite this as
Mallik M, Rout SK, Sahu RK (2021) Back to Basics – The best approach in reconstructive surgery to tide over the COVID pandemic crisis. J Surg Surgical Res 7(2): 083-087. DOI: 10.17352/2455-2968.000143Background- COVID-19 pandemic has wreaked havoc on Plastic Surgery practices globally. The superior forms of reconstruction or repair take long operative hours, more surgical team members and invasive post-operative monitoring which impose substantial risk of acquiring the infection. Having faced the numerous issues, we considered basic “old school” reconstructive strategies over the ideal ones during this pandemic and realized their importance.
Method- In this retrospective study period of one year, the patients whom we had earlier planned for a superior form of reconstruction, but ultimately had to be managed in a basic, safe, quick and “old school” ways, were included. The details of the changed plans of reconstruction or repair, the operative time, number of team members, post-operative stay and other data were retrieved and analysed.
Results- Among the 30 patients included, the mean age was 39.9 years, with male to female ratio of 3:2. The mean operative time was 64.7 minutes and the mean number of surgical team members was 2.5. The mean period of post-operative inpatient stay was 2.4 days. 16.7% of patients were infected by COVID-19 within the immediate 2 weeks of post-operative period but with no mortality. The mean period of OPD follow-up was 5.5 days after discharge with 20% overall complications.
Conclusion- In this difficult time of the COVID pandemic, the basic and fundamental surgical plans of repair and reconstruction still hold their significance and should be considered to achieve the reconstructive goals.
Introduction
The principle of reconstruction has taken a paradigm shift over the last two decades. Instead of reconstructive ladder, the approach at present is to use the reconstructive elevator, which essentially means to adopt technically demanding and superior modalities to start with rather than the basic, simple ones. This newer approach justifies itself by superior reconstruction in terms of form and function of the reconstructed site as well as the donor site morbidity. Microvascular free tissue transfer is relied upon more commonly than the pedicled loco-regional flaps for head and neck reconstruction, in particular. Hence, flaps like pectoralis major myocutaneous flap, Deltopectoral flap, and lateral forehead flaps have become the “endangered species”. These flaps, which have been basics for any plastic and reconstructive surgeon in the beginning of his/her career, has become difficult for teaching the trainees because of less opportunity for hands on.
Following the onset of COVID-19 pandemic, there have been tremendous impacts on all surgical practices globally [1-5]. In a recent study, there had been estimation of elective surgery cancellations using a beta-regression model to predict 12-week surgery cancellation rates for 190 countries which stated that there would be 72.3% overall cancellation rate (90.2% for benign diseases and 37.7% for cancer operations), also stating that if the normal surgical volume after the pandemic is increased by 20%, it would take a median of 45 weeks to clear the backlog [5].
There have been multiple studies focusing on issues associated with management of surgical cases in terms of COVID 19 transmission and suggestions to reduce it [6-9]. The problems pointed out are improper pre-operative screening for virus, aerosol generating procedures, performing multiple time consuming procedures in the same sitting of surgery, incompatibility of PPE with routine operative equipment, etc [1]. On a similar principle, we too modified our approach towards reconstruction of various post excisional and the post traumatic defects we came across during this pandemic, without compromising the goal of reconstruction and justify our decision.
Methodology
This was a retrospective observational study conducted over 1 year (April 2020 to March 2021) in the Burns & Plastic Surgery department of our institute (a tertiary level teaching hospital). The patients whom we had earlier planned for a superior form of reconstruction, but ultimately had to be managed in a basic, safe, quick and “old school” ways, were incorporated in this study. Also, the patients who attended the department for essential surgeries and their reconstructive plans modified to reduce the risk of COVID transmission were included in this study. The data of those patients were retrieved from the electronic database as well as the print records of our hospital and analyzed. The ideal operative plan, procedure performed (modified plan), time taken for induction of anaesthesia, type and method of endotracheal intubation, any additional procedure, number of OT staffs attended the case, post-operative hospital stay including stay in HDU/ICU were recorded in Microsoft Excel sheet. The clinical photographs of the patients were retrieved from the electronic archives of our department. The follow-up data were retrieved from the follow up clinic records to assess the short-term complications of those procedures.
Results
Within this period, 30 patients who received treatment and fulfilled the inclusion criteria were included in this study. The mean age of the patients was 39.9 years, with a male to female ratio 3:2. The mean duration of the procedures was 64.7 minutes. The mean number of surgeons involved in reconstruction was 2.5. The mean duration of HDU/ICU stay was 8.4 hours, and the mean duration of post-operative inpatient stay was 2.4 days. The mean period of first follow up at OPD was 5.5 days after discharge. There were 20% overall complications of any type. Five out of 30 patients (16.7%) were affected by COVID-19 within the first 30 days of surgery. Six out of 15 reconstruction team members (40%) were affected by COVID-19 during this period. Based on etiology, wound pathology and regions of body, majority of the patients presented with trauma to upper and the lower extremities (30% each) followed by oral malignancies which accounted for 20% of the total cases. The other subgroups of defects in scalp, maxillo-facial trauma and breast reconstruction constituted 6.7% each. There was no mortality observed among these patients. The other details of the subgroups are enumerated in table – 1. Details of the ideal / planned procedures and their modifications in this context are mentioned in Table 1.
Discussion
COVID 19 pandemic has affected the clinical practice of all the subspecialities of Plastic Surgery adversely [3, 4]. British Association of Plastic Surgery (BAPRAS) guidelines recommend to stop all elective surgeries and limit the emergency surgeries in the current scenario of COVID-19 and the emergency procedures to be managed in outpatient clinics with minor essential procedures [2]. An electronic survey questionnaire was distributed in April 2020 to 532 members of American Council of Academic Plastic Surgeons (ACAPS), with data on demographics, individual practices, preventive measures and procedures undertaken during this pandemic with a response rate of 30.2% [3]. Changes in hospital policies was the reason in 89% of the cases to determine the procedures offered. Less than 10% of the members offered aesthetic surgeries and no one performed gender reaffirming surgeries. Several studies reported significant association of COVID positivity in cases of head and neck cancer surgeries owing to high community incidence, intra-oral location of tumors, long induction time and tracheostomy [5].
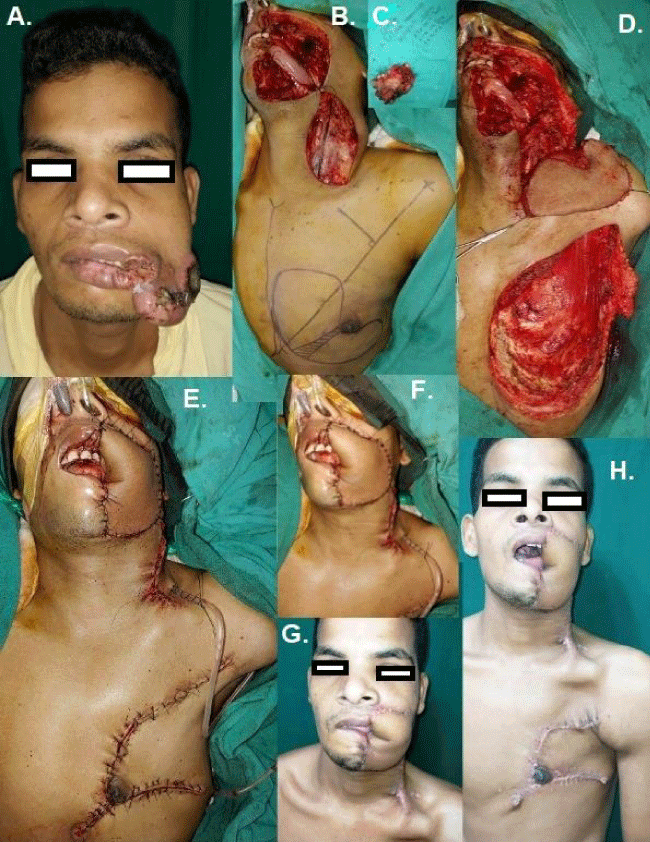
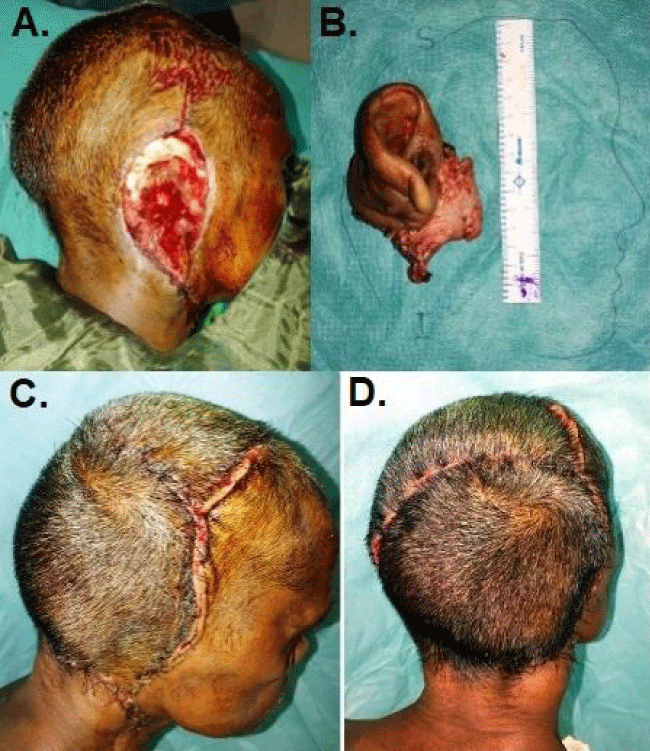
It is noted that there is: A trend to change the surgical plans has been observed towards the more basic and traditional ones, in order to avoid long duration procedures, which in turn increase the risk of viral transmission to the surgical team, prolongs the inpatient stay including the intensive phase and subject the patient to increased risk of acquiring COVID-19 infection [1-4,10]. Table 2 shows our modified plans for the reconstructive or reparative procedures which we adopted, considering all of these facts mentioned in literature. For head and neck reconstruction, we used pedicled locoregional flaps like the PMMC Figure 1, Deltopectoral and lateral forehead flap as opposed to the ideal free tissue transfers (Radial forearm, Anterolateral thigh and fibula osteocutaneous flaps). The advantages of these flaps are faster execution (mean operating time for reconstruction = 105 min), requirement of less number of surgical team members (mean = 3), no need for hourly monitoring of flaps and re-exploration, reduced ICU/HDU stay (mean duration = 26 hours) and quick discharge from hospital after surgery (mean period of stay in the ward = 4.2 days). As per literature, in this COVID-19 era, there has been no clear guidelines for general reconstruction following malignancy extirpation including head and neck malignancies, in which cases they were individualized in terms of pathology, operative planning and reconstruction [3]. However the pandemic has forced the British Association of Head and Neck Oncologists (BAHNO) to come up with the recommendations for day care surgeries wherever feasible, with reduction in length of surgery (local flaps versus free flaps) and HDU/ITU stay [4]. Head and neck cancer patients are generally high-risk candidates to acquire COVID-19 infection with severe outcomes, also imposing risks for virus transmission to health care workers and caregivers substantially [1]. In a cohort of 1137 consecutive patients undergoing primary head and neck surgery with curative intent, the commonest site involved was oral cavity (38%), the overall 30-day mortality 1.2%, 3% of the patients tested positive for COVID-19 within 30 days of operation and 3% members of the surgical team tested positive within 30 post-operative days [5]. In our study, the total number of patients (for all etiologies and sites) tested positive for COVID-19 within 14 days of surgery, was 5 out of 30 (16.67%), the number of surgical team members affected by COVID-19 within the study period of 1 year was 6 out of 15 (40%) and there was no mortality Figure 2.
All delayed breast reconstruction and planned procedures of revision reconstruction should be postponed as per the guidelines of American Society of Plastic Surgeons (ASPS) [2]. The Association of Breast Surgery (ABS) also advised, immediate breast reconstruction to be deferred and local flaps/oncoplastic techniques be considered [4]. The Society of Surgical Oncologists too recommend delaying immediate autologous breast reconstruction, in favor of tissue expanders and implants [3]. In our study, 2 patients who underwent mastectomy were addressed with pedicled transverse rectus abdominis myocutaneous (TRAM) flap and Latissimus Dorsi Myocutaneous (LDMC) flap instead of the free DIEP flaps Figures 3,4.
In cranio-facial surgeries, it is recommended to prioritize maxillofacial cases like injuries to facial nerve, eyelids, nose, trap-door fractures with entrapment of orbital contents, superior orbital fissure syndrome, septal haematoma, reduction of visual acuity necessitating orbital decompression and defer cases like closed maxillo-facial fractures, including mandibular and dento-alveolar ones [2]. Surgery for temporomandibular joint pathologies, craniofacial malformations, primary and secondary cleft lip and palate should also be deferred. AOCMF also recommends closed reduction of maxillo-facial fractures over open procedures, with preventive measures of full aerosol precautions during evaluation and operation, including usage of powered air purifying respirators and minimal irrigation and suctioning [3]. We have addressed 2 favorable and non-comminuted mandibular fractures with closed reduction and Intermaxillary Fixations (IMF) only.
As per British Orthopaedic Association (BOA) and British Society for Surgery of the Hand (BSSH), non-operative management of hand injuries are recommended, wherever possible with local anesthetic surgery and use of outpatient or procedure room facilities [4]. The BSSH has also recommended use of local anesthetic blocks or a “wide-awake, local anaesthetic, no tourniquet” protocol (WALANT), use of absorbable sutures and easily removable post-operative dressings and splints [2]. As per a recent case report, a 17-year-old male with osteosarcoma of the proximal humerus, initially planned for limb salvage surgery after neoadjuvant chemotherapy, had to undergo forequarter amputation, justifying low exposure risk in hospital setting and home convalescence monitored by video conferencing and multidisciplinary team telemedicine services [10]. We performed 9 hand surgery procedures (with modified plans) during this study period which were quick (mean operative time of 40 min) with an average involvement of 2.1 surgical team members and a mean post-operative stay of 1.3 days.
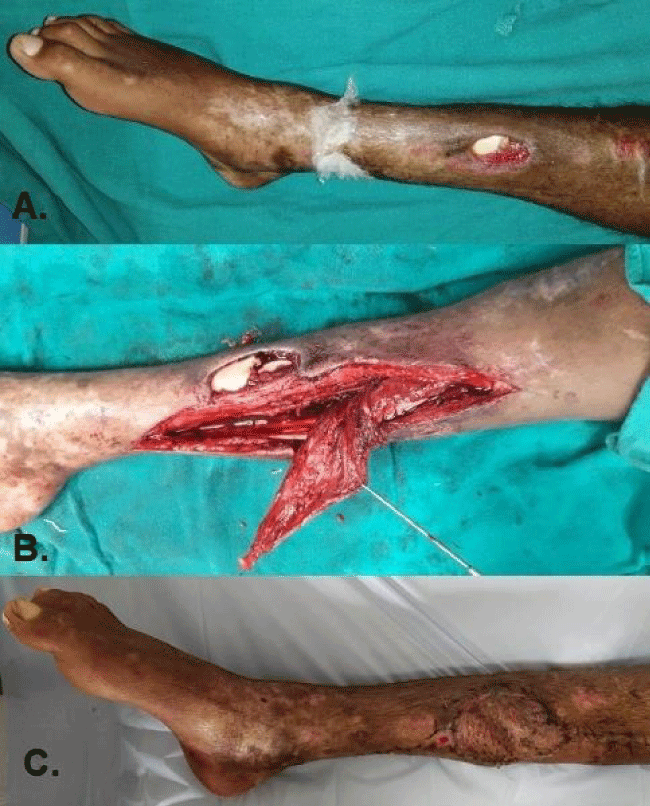
BOA, BSSH and Orthopaedic Trauma Society (OTS) has recommended alternative reconstruction plans to avoid multiple staged procedures and critical care requirement in lower limbs, also considering early amputation if limb salvage is uncertain and doubtful [4]. We had operated on 9 lower limb trauma patients with modified plans, with mean operative duration of 58.9 minutes and a mean post-operative stay of 2.1 days. Four amputations were performed with informed consents (2 each for upper and lower extremities at different levels) where the limbs were of doubtful vascularity requiring staged procedures and long post-operative stay.
These modified operative plans, by going “back to the basics”, which we executed during this period, substantially addressed the issues related to the clinical problems of the patients as well as COVID transmission risk to them and the health care workers. At the same time, these modifications also helped the trainees of plastic and reconstructive surgery to have an exposure to these traditional but fundamental reconstructive procedures. We believe, this approach would be appropriate even for the time to come, as long as the pandemic prevails.
Conclusion
As recommended by many international societies or professional bodies, the reconstructive problems can be addressed by suboptimal techniques in exclusive circumstances, with care being taken to achieve the reconstructive goals. The basic fundamental surgical plans of repair and reconstruction can still be considered as “the friend in need” during difficult times like COVID 19 pandemic.
- Day AT, Sher DJ, Lee RC, Truelson JM, Myers LL, et al. (2020) Head and neck oncology during the COVID-19 pandemic: Reconsidering traditional treatment paradigms in light of new surgical and other multilevel risks. Oral Oncol 105: 104684. Link: https://bit.ly/2UuJ7DR
- Al-Jabir A, Kerwan A, Nicola M, Alsafi A, Khan M, et al. (2020) Impact of the Coronavirus (COVID-19) pandemic on surgical practice - Part 2 (surgical prioritisation). Int J Surg 79: 233-248. Link: https://bit.ly/2UuJe2f
- Sarac BA, Schoenbrunner AR, Wilson SC, Chiu ES, Janis JE (2020) The Impact of COVID-19-based Suspension of Surgeries on Plastic Surgery Practices: A Survey of ACAPS Members. Plast Reconstr Surg Glob Open 8: e3119. Link: https://bit.ly/3xUWPxC
- Johal KS, Vinnicombe Z, Khan U, Mohanna PN (2021) COVID-19 and plastic surgery: lessons from a national specialty review in the United Kingdom: COVID-19 and plastic surgery. J Plast Reconstr Aesthet Surg. Link: https://bit.ly/3gg9NQo
- COVIDSurg Collaborative (2020) Head and neck cancer surgery during the COVID-19 pandemic: An international, multicenter, observational cohort study. Cancer 127: 2476-2488. Link: https://bit.ly/3AVCbiU
- Sharma D, Agrawal V, Agarwal P (2020) Roadmap for Restarting Elective Surgery During/After COVID-19 Pandemic. Indian J Surg 1-5. Link: https://bit.ly/3AVD6jm
- Guerci C, Maffioli A, Bondurri AA, Ferrario L, Lazzarin F, et al. (2020) COVID-19: How can a department of general surgery survive in a pandemic?. Surgery 167: 909-911. Link: https://bit.ly/3gfifzE
- Yeo D, Yeo C, Kaushal S, Tan G (2020) COVID-19 and the General Surgical Department - Measures to Reduce Spread of SARS-COV-2 Among Surgeons. Ann Surg 272: e3-e4. Link: https://bit.ly/3gfWoYI
- Di Marzo F, Sartelli M, Cennamo R, Toccafondi G, Coccolini F, et al. (2020) Recommendations for general surgery activities in a pandemic scenario (SARS-CoV-2). Br J Surg 107: 1104-1106. Link: https://bit.ly/3md0BQI
- Gaston CLL, Pag-Ong JP, Dacanay E, Quintos AJ (2020) Radical change in osteosarcoma surgical plan due to COVID-19 pandemic. BMJ Case Rep 13: e237197. Link: https://bit.ly/3kdKobw
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
