Journal of Surgery and Surgical Research
Functional outcomes of ulnar nerve neurotization by anterior interosseous nerve in high level injury
HH Noaman*, Mohammed A Mohamed and Yasser Othman Sorour
Cite this as
: Noaman HH, Mohamed MA, Sorour YO (2021) Functional outcomes of ulnar nerve neurotization by anterior interosseous nerve in high level injury. J Surg Surgical Res 7(2): 070-074. DOI: 10.17352/2455-2968.000141Background: The ulnar nerve injury induce sever hand malfunction due to intrinsic muscle paralysis. The ulnar nerve repair in proximal area (high ulnar nerve injury) seldom leads to intrinsic muscle function because of long distance of nerve return. Therefore, the best techniques to restore intrinsic hand function in patient with high ulnar nerve injury is distal nerve transfer to minimize the regeneration time and distance.
Objective: The aim of this study is to describe the surgical results obtained with the transfer of the motor branch of the anterior interosseous nerve destined to the pronator quadrates muscle to the motor division of the ulnar nerve (the deep branch of ulnar nerve).
Methods: It is a retrospective study of thirty elderly patients with high ulnar nerve injury underwent a transfer of distal branch of anterior interosseous nerve to deep branch of ulnar nerve, and end to end suture of the ulnar nerve at the site of injury in Sohag microsurgery unit.
Results: The mean postoperative follow-up period was 22 months (range from 12 to 38 months). At the final follow-up, twenty-seven (90%) patients showed good results according to the Highet-Zachary scheme (M3 or M4, S3+, and negative Froment’s sign). The other three patient (10%) showed a poor result (M1, S2, positive Froment’s sign).
Conclusion: This technique of transfer of distal branch of anterior interosseous nerve to deep motor branch of ulnar nerve and primary repair of ulnar nerve at site of injury is effective for motor and sensory recovery of distal ulnar innervated side of the hand.
Introduction
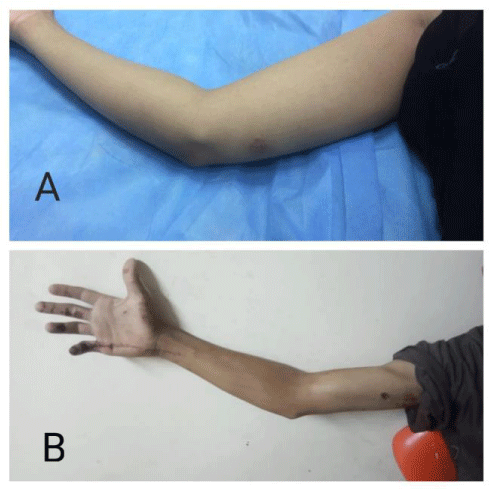
The ulnar nerve injury induce sever hand malfunction due to intrinsic muscle paralysis. The ulnar nerve repair in in proximal area (high ulnar nerve injury) seldom leads to intrinsic muscle function because of long distance of nerve recovery. Therefore, the best techniques to restore intrinsic hand function in patient with high ulnar nerve injury is distal nerve transfer to minimize the regeneration time and distance [1,2]. Injuries of the ulnar nerve can be classified as high or low. Low injuries take place distal to the origins of the motor branches of the flexor carpi ulnaris and ring and little finger flexor digitorum profundus muscles. Although the strength of the extrinsic hand muscles is not influenced, sensation is lost on the ulnar border of the hand and in the ring and little fingers, and the ulnar-innervated intrinsic muscles lose their function. Consequently, this shows through a weakened thumb pinch, claw deformity, loss of the normal pattern of finger flexion, and significant loss of hand dexterity and strength. High injuries occur above the aforementioned place (Figure 1). Here, loss of active ring finger flexion, little distal interphalangeal joint flexion, and wrist flexion compound the findings; paradoxically, however, the claw deformity has a tendency to be less severe [3].
Despite meticulous microsurgical repair, the prognosis of an injury of the ulnar nerve at a level above the elbow is usually considered poor in terms of potential for motor recovery of the distal muscle of the hand. A special nerve transfer technique was developed as a surgical alternative for these cases aiming to approximate the donor axons to the recipient muscles of the hand, the transfer of a terminal motor branch of the anterior interosseous nerve to the deep branch of ulnar nerve [3].
Material and methods
It is a retrospective study of thirty elderly patients with high ulnar nerve injury underwent a transfer of distal branch of anterior interosseous nerve to deep branch of ulnar nerve, and end to end suture of the ulnar nerve at the site of injury in Sohag microsurgery unit from September 2016 to October 2018 with 2 years follow up. Inclusion criteria include: any age & sex, complete isolated ulnar nerve injury, level of injury at or above elbow, and not more than 6 months before treatment. Exclusion criteria include partial nerve injury and neuropathy either hereditary or acquired. Before surgery, all patients had complete ulnar nerve palsy (M0, S0, and positive Froment’s sign). Preoperative electro diagnosis electromyography was performed for all patients and no contractile muscle fibers could be detected. The study was approved by our Institutional Review Board. An informed written consent was obtained for all patients for participation and publication of the both results and patients images.
Surgical technique
The procedure was performed under general anesthesia, with tourniquet inflation of the affected upper limb. In order to ascertain the absence of nerve function at the level of the wrist, electrical stimulation of the ulnar nerve was performed before any intraneural dissection, and thus avoiding that neuropraxia would provide negative results. Considering that the proximal border of the pronator quadratus muscle is usually positioned four fingertips proximally from the wrist. The incision incorporated the distal third of the forearm and the region of Guyon’s canal. Firstly, the deep and superficial divisions of the ulnar nerve was isolated and traced proximally to the level of the Guyon’s canal were identified. Then, the motor division of the ulnar nerve was isolated and traced proximally to the level or the pronator quadratus muscle, by means of an internal neurolysis of the ulnar nerve. The Anterior Interosseous Nerve (AIN) was approached by sweeping of all flexor tendons laterally, followed by the identification of the proximal border of the pronator quadratus muscle. The AIN runs over the interosseous membrane and enter the muscle centrally together with the vessels. The nerve was followed to the point where it began to branch out which usually occurred at the mid-portion of the muscle and mobilized proximally, to obtain a longer segment to be transported to the ulnar nerve. The motor fascicle of the ulnar nerve was divided as proximally as possible and the AIN was divided at its distal most segment into the muscle. A Tension free direct suture between both nerves was performed using two 10, 0 stitches. The ulnar nerve was sutured at the site of injury by direct repair to maintain sensory supply (Figure 2). The incision was sutured, and the wrist was immobilized for three weeks. Following this period, sensory and motor rehabilitation was initiated immediately. Motor rehabilitation included passively movements of the fingers and wrist, active exercise (Figure 3).
Postoperative follow up was done at 2, 8, 12, 24 and 48 weeks then every year. Evaluation of our patients using Highet-Zachary scheme was done at 6, 12, 18 and 24 months.
Results
The mean postoperative follow-up period was 22 months (range from 12 to 38 months). At the final follow-up, twenty-seven (90%) patients showed good results according to the Highet-Zachary scheme (M3 or M4, S3+, and negative Froment’s sign). The other three patients (10%) showed a poor result (M1, S2, positive Froment’s sign). Tables 1,2
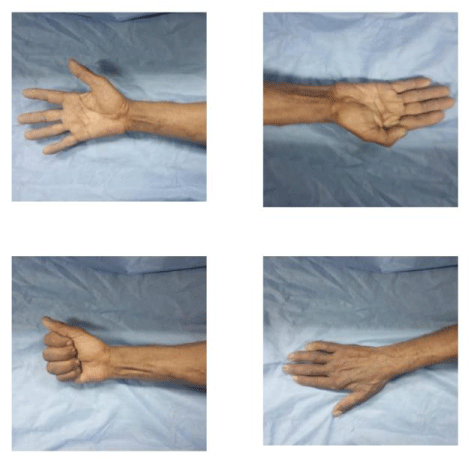
In patients with good results, the average static two- point discrimination was 7 mm (range from 6 to 8 mm) and the moving two-point discrimination was 6 mm (range from 5 to 6 mm). The grip and pinch strength in patients with good results was 80% of the normal side. The partial clawing was corrected in these patients. The muscle wasting was not fully restored (Figure 3).
The patients with a poor result had some touch sensibility and no two-point discrimination could be detected. The grip and pinch strength in this patient were only 40% of the normal side. The partial clawing was not corrected, and the patient needed tendon transfer using the flexor digitorum superficialis of the ring finger.
No functional deficit in pronation occurred in any patient. All patients had no complaints as in terms of the anesthetic area supplied by the palmar cutaneous branch of the median nerve. No painful neuroma was reported in the distal forearm, where the two terminal branches of the ulnar nerve were cut. This was concluded through both patient compliant and neurological examination of the patient by the operating g surgeon at the final follow up.
Discussion
There are many series reporting that high ulnar nerve lesions above the level of the elbow often have a poor prognosis. This is attributed to the fact that the ulnar nerve is a mixed nerve that carries both sensory and motor fibers and even with the most meticulous repair under the microscope, some cross innervations show poor sensory and motor recovery. Also, the long distance between the site of lesion and the innervated intrinsic muscles of the hand made it take long time to reach the motor end plate. During this long period, the denervated intrinsic muscles will undergo irreversible atrophic changes.
Gaul [4] reported that adults with high ulnar nerve lesions never recovered acceptable function. Vastamäki, et al. [5] concluded that a satisfactory result cannot be expected if the level of injury is more than 60 cm from the tip of the middle finger (i.e., high ulnar nerve lesions). Taha and Taha [6] reported that tendon transfer was needed in 72% of patients with high ulnar nerve lesions. Ruijs, et al. [7] reported the meta-analysis of 23 articles including the individual data for 623 median or ulnar nerve injuries. In ulnar nerve injuries, the chance of motor recovery was 71% lower than that in median nerve injuries. Secer, et al. [8] reviewed the results of repair of ulnar nerve lesion caused by gunshots in 455 patients over 40 years. Good results were noted in 15.06% of patients who had high-level lesions, 29.60% of patients with intermediate-level lesions, and 49.68% of patients with low-level lesions. Pfaeffle, et al. [9] observed that all patients with high- level ulnar nerve lesions required tendon transfer because the motor recovery is usually poor.
In this study, the terminal branch of the AIN supplying pronator quadrates muscle was transferred to the motor branch of the ulnar nerve. From the anatomical point of view, the width, and the number of myelinated fibers of both nerves are similar (the pronator quadratus branch of the median nerve was 1.5 ± 0.4 mm in diameter, with 866 ± 144 nerve fibers). The deep branch of ulnar nerve was 2.1 ± 0.4 mm in diameter, with 1318 ± 120 nerve fibers [6,9,10]. Direct coaptation is performed without the need for nerve grafting. The functional loss is minimal after denervation of pronator quadrates as the pronator teres can compensate. All these advantages make this procedure a good option to restore the motor function of irreparable high ulnar nerve lesions.
In this study, good motor recovery (M3 or M4) was observed in twenty seven (90%) out of thirty patients. This resulted in good postoperative lateral pinch and grip strength. The other three patients had poor motor recovery (M1) and tendon transfer was needed to restore the motor function. Haase and Chung [10] managed two cases with high ulnar nerve injuries by distal nerve transfer of the AIN to the deep motor branch of the ulnar nerve. They reported return of function to the ulnar-innervated intrinsic muscles of the hand in these two cases. Protective sensation was restored through the native pathway of the ulnar nerve after proximal repair of ulnar nerve injuries. Wang and Zhu [11] reported that transfer of the pronator quadratus branch of the AIN to the recurrent branch of the median nerve and the deep branch of the ulnar nerve to restore the intrinsic functions of the hand was performed on 20 patients. Fourteen patients were followed up for an average of 68 months. In the latest follow-up, normal muscle strength (M5) was regained in three patients, M4 strength in six patients, M3 strength in three patients, and M2 strength in two patients. No sensory nerve transfer was performed in these cases.
There are many options to restore the sensory function of high ulnar nerve injuries by distal nerve transfer from the median nerve or by end-to-side repair to the median nerve. In our report, primary repair of the ulnar nerve at the site of injury to restore sensory recovery.
Ozkan, et al. [12] described end-to-end transfer of the ulnar digital nerve of the index or long finger to the ulnar digital nerve of the small finger. They reported good sensory recovery in most cases. The disadvantage of this technique is that it decreased the sensory area in the same hand. Brown, et al. [13] described end-to-end transfer of the third common palmar digital nerve of median nerve to the volar sensory component of ulnar nerve and end-to-side re-innervation of the ulnar dorsal cutaneous branch to the remaining median sensory trunk. The sensory recovery was acceptable in their work. Many authors described end-to-side suture of the sensory ulnar nerve component to the third common palmar digital nerve of the median nerve in the palm or to the trunk of the median nerve in the distal forearm with variable results. The advantage of this technique is that no additional sensory loss occurred [14-16].
To our knowledge, only a few publications have used the same technique of distal neurotization of high ulnar nerve lesions using the AIN and the primary repair of the ulnar nerve at the level of injury to restore the motor and sensory function of the ulnar nerve. This report clarified the indications, the advantages, and disadvantages, and showed satisfactory results.
Conclusion
This technique of transfer of distal branch of anterior interosseous nerve to deep motor branch of ulnar nerve and primary repair of ulnar nerve at site of injury is effective for motor and sensory recovery of distal ulnar innervated side of the hand.
Author’s contributions
All authors contributed to this project and article equally. All authors read and approved the final manuscript.
- Post R, de Boer KS, Malessy MJ (2012) Outcome following nerve repair of high isolated clean sharp injuries of the ulnar nerve. PLoS One 7: e47928. Link: https://bit.ly/3AEx3QC
- (2013) Peripheral nerve injuries Campbell's Operative Orthopedics. Philadelphia: Mosby 3635-3706. Cannale ST BJ, eds, editor 2013.
- (1999) Nerve transfers. New options for reconstruction following nerve injury. Hand Clin 15: 643-666 ix. Link: https://bit.ly/2UxMqKl
- S (1982) Intrinsic motor recovery—a long-term study of ulnar nerve repair. J Hand Surg Am 7: 502-508. Link: https://bit.ly/3jYZF19
- (1993) The results of secondary microsurgical repair of ulnar nerve injury. J Hand Surg Br 18: 323-326. Link: https://bit.ly/3qSlVLJ
- (1998) Results of suture of the radial, median, and ulnar nerves after missile injury below the axilla. J Trauma 45: 335-339. Link: https://bit.ly/3qV4NEZ
- (2005) Median and ulnar nerve injuries: a meta-analysis of predictors of motor and sensory recovery after modern microsurgical nerve repair. Plast Reconstr Surg 116: 484-494. Link: https://bit.ly/3qSeZ1b
- (2007) Surgical repair of ulnar nerve lesions caused by gunshot and shrapnel: results in 407 lesions. J Neurosurg 107: 776-783. Link: https://bit.ly/3r6uqmB
- (2007) Ulnar nerve laceration and repair. Hand Clin 23: 291-299. Link: https://bit.ly/3hqflsC
- (2002) Anterior interosseous nerve transfer to the motor branch of the ulnar nerve for high ulnar nerve injuries. Ann Plast Surg 49: 285-290. Link: https://bit.ly/3dSFm1q
- (1997) Transfer of a branch of the anterior interosseus nerve to the motor branch of the median nerve and ulnar nerve. Chinese Med J 110: 216-219. Link: https://bit.ly/2TEn7pX
- (2001) Restoration of sensibility in irreparable ulnar and median nerve lesions with use of sensory nerve transfer: long-term follow-up of 20 cases. J Hand Surg Am 26: 44-51. Link: https://bit.ly/2UxlD0q
- (2009) Distal median to ulnar nerve transfers to restore ulnar motor and sensory function within the hand: technical nuances. Neurosurgery 65: 966-978. Link: https://bit.ly/3qSkNrr
- et al. (2007) End-to-side nerve neurorrhaphy: critical appraisal of experimental and clinical data. Acta Neurochir Suppl 100: 77-84. Link: https://bit.ly/3jPtSjg
- (2008) Nerve fiber transfer by end-to-side coaptation. Hand Clin 24: 461-483. Link: https://bit.ly/3hny7Ri
- (2005) End-to-side neurorrhaphy for defects of palmar sensory digital nerves. British Journal Plastic Surgery 58: 239-244. Link: https://bit.ly/3hqtmqs
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
