Journal of Surgery and Surgical Research
Seroma after sternal wound debridement: Case report
Julia Glizevskaja*, Mohammed Abbas and Nnamdi Nwaejike
Cite this as
Glizevskaja J, Abbas M, Nwaejike N (2021) Seroma after sternal wound debridement: Case report. J Surg Surgical Res 7(1): 047-048. DOI: 10.17352/2455-2968.000135Seroma formation is a common complication of any surgery producing a significant dead space or causing disruption of the lymphatic drainage. Although this is uncommonly reported in cardiac surgery. Such collections can cause localized pain, wound dehiscence, infection and can reoccur frequently, requiring multiple interventions. We present case of large sternal wound seroma after wound debridement with Computed tomography imaging for the patient, that initially underwent Coronary artery bypass grafting.
Abbreviations
CABG: Coronary Artery Bypass Grafting; CT: Computed Tomography
Introduction
Operations involving extensive soft tissue surgery and disrupting lymphatic drainage may result in a postoperative seroma. Although this is uncommonly reported in sternal wounds after cardiac surgery. Such collections can cause localized pain, wound dehiscence, infection and can reoccur frequently, requiring multiple interventions. We present case of sternal wound seroma after wound debridement.
Case presentation
57 years old male developed chronic sternal wound sinus following CABG and required multiple courses of antibiotics. His risk factors of wound infection included bilateral mammary arteries harvest, long term smoker, use of systemic immunosuppressant and topical steroid creams for severe dermatitis. He firstly underwent one culpable sternal wire removal 6 months following CABG. Limited strategy was used to minimise wound infection risk in patient with severe skin conditions. Following another 6 months he developed further sinus lower to the previous one, therefore decision made to proceed with all sternal wires removal. He underwent elective sternal wound debridement, excising previous sternotomy scar and removing all remaining sternal wires. Intraoperatively he was found to have bone involving, and precise wound debridement was performed including debridement of unhealthy bone segment, living around 3x1x0.5cm sternal defect without penetration to mediastinum or disturbing sternal stability. To approximate wound edges, bilateral skin flaps with underlying subcutaneous tissues were prepared. Wound closed layered, living Redon Redivac drain (PFM Redon system, Mepro, Koln Germany) in both pockets. Postoperatively patient made good recovery, he remained in hospital while drains were in situ, draining 300 ml of hemo-serous fluids over first 24 hours. After drainage gradually reduced, drains were removed on day 5 and patient was discharged home. Intra-operative wound swab came back negative.
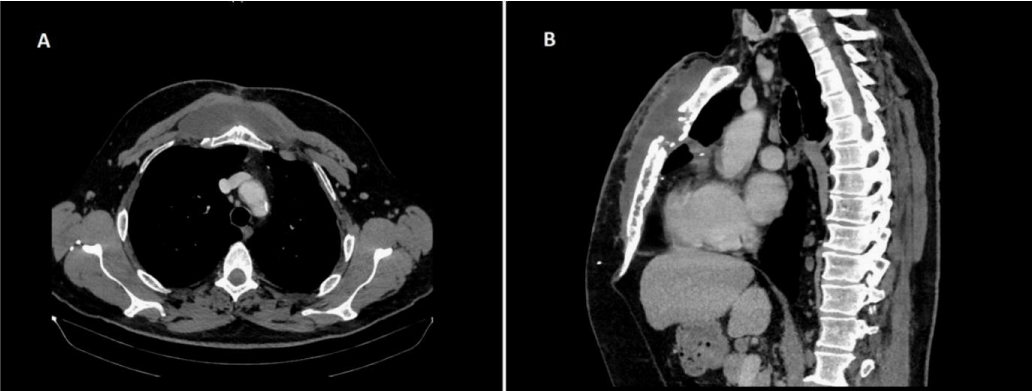
He presented to our department 2 weeks later with large fluctuating non painful swelling over sternotomy wound. There were no signs of infection, sternal wound has healed well, his inflammatory markers were within normal limits. At admission he underwent a CT scan, which demonstrated large 3.4x10.8x 18.8cm collection subcutaneously anterior to the sternum; the fluid collection did not contain locules of gas (Figure 1). There was no connection of seroma with mediastinum and there was no pericardial effusion. We proceed with drainage of collection under local anaesthesia using vacuum-assisted drainage, as described by Fitzgerald and Charles [1,2] and evacuated 150ml of serous fluids with immediate improvement. Patient was discharged home same day. He was seen in our follow-up clinic in 2 weeks time, unfortunately at that point seroma has re-accumulated. After discussion with the patient, conservative “watch-and-wait” approach was selected. By the mean time we referred him to his dermatologist for relapse of dermatitis. At the further follow-up in 3 months time seroma has completely resolved, at the same time following adjustment in dermatological treatment his skin condition has significantly improved.
Discussion
A seroma is a serum collection that develops as a response to trauma/injury such as surgery. Seroma formation is a known complication of various types of surgeries. So far described published cases of seroma in cardiac surgery were cases of groin seromas as complication of peripheral cannulations.
The presence of seroma in a wound might delay the wound healing and becomes medium for bacterial growth. Factors predisposing to sternal wound complications (including seroma) are diabetes, obesity, long operation duration, redo sternotomy, mechanical ventilation longer than 72 hours and smoking [3,4].
Few studies reported superficial sternal wound infection rate between 0.5-6.4%, while deep sternal wound infection between 0.22-1.6% [5,6]. Trans-sternal seromas post thymectomies are uncommon complications as incidence rate described by Kas et al. about 0.9% [7]. On the other hand, up to 35% of patients who undergo mastectomy develop seroma [8]. During our literature review (through PubMed), we could not find specific incident rate or risk factors for seroma in cardiac surgery.
Conclusion
We presented a rare case of large sternal seroma after sternal wound debridement with instructive images from CT scan. Multiple management strategies of seromas are known, including conservative management and observation, multiple drainages and aspirations, wound re-exploration, sclerotherapy. We have chosen initially percutaneously aspirate seroma, however following re-accumulation it was left for watch-and-wait tactic, which eventually lead to complete resolving of seroma at 3 months follow-up.
In this man’s case we have observed, that addressing severe skin pre-condition has facilitated clearance of large seroma with conservative approach. We believe that combination of exacerbation of dermatitis and extensive exfoliation of the subcutaneous tissues were main factors of seroma formation in our case.
The authors received no financial support for the authorship or publication of this article.
- Fitzgerald JEF, Hayes AJ, Strauss DC (2011). Vacuum-assisted sterile drainage of large post-operative seromas: the Royal Marsden technique. Ann R Coll Surg Engl 93: 646–647. Link: https://bit.ly/3uBQDcn
- Charles JB, Samer S, Pari-Naz M (2010). A closed vacuum drainage system for the management of postoperative seromas. Ann R Coll Surg Engl 92: 354–355. Link: https://bit.ly/3mu3tqs
- Wouters R, Wellens F, Vanermen H, De Geest R, Degrieck I, et al. (1994). Sternitis and mediastinitis after coronary artery bypass grafting. Analysis of risk factors. Tex Heart Inst J 21: 183-188. Link: https://bit.ly/3mFJeX7
- Milano CA, Kesler K, Archibald N, Sexton DJ, Jones RH (1995) Mediastinitis after coronary artery bypass graft surgery. Risk factors and long-term survival. Circulation 92: 2245-2251. Link: https://bit.ly/3dDlwq0
- Ridderstolpe L, Gill H, Granfeldt H, Ahlfeldt H, Rutberg H (2001) Superficial and deep sternal wound complications: incidence, risk factors and mortality. Eur J Cardiothorac Surg 20: 1168-1175. Link: https://bit.ly/3dOmvUq
- Salehi Omran A, Karimi A, Ahmadi SH, Davoodi S, Marzban M, et al. (2007) Superficial and deep sternal wound infection after more than 9000 coronary artery bypass graft (CABG): incidence, risk factors and mortality. BMC Infect Dis 7: 112. Link: https://bit.ly/3cYwiYN
- Kas J, Kiss D, Simon V, Svastics E, Major L, et al. (2001) Decade-long experience with surgical therapy of myasthenia gravis: early complications of 324 transsternal thymectomies. Ann Thorac Surg 72: 1691-1697. Link: https://bit.ly/3s1rxSw
- Hashemi E, Kaviani A, Najafi M, Ebrahimi M, Hooshmand H, et al. (2004). Seroma formation after surgery for breast cancer. World J Surg Onc 2: 44. Link: https://bit.ly/39OtMTd
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
