Journal of Surgery and Surgical Research
Intestinal Perforation Secondary to Peritoneal Dialysis Catheter; An Uncommon Complication
Uraik Fernando Hernández-Bustos, Jonathan Salgado-Vives*, Dante Alejandro Saldivar-Vera, Pedro Antonio Alvarado-Bahena and Enrique Chávez-Serna*
Enrique Chávez-Serna, General Surgery Department, Regional General Hospital No.1, Mexican Institute of Social Security IMSS, Postgraduate Studies Division, Autonomous University of Querétaro, México, Tel: 52223231287; Fax: 2223991635; E-mail: Enrique.chavez.serna@gmail.com
Cite this as
Hernández-Bustos UF, Vives JS, Saldivar-Vera DA, Alvarado-Bahena PA, Serna EC (2020) Intestinal Perforation Secondary to Peritoneal Dialysis Catheter; An Uncommon Complication. J Surg Surgical Res 6(2): 168-170. DOI: 10.17352/2455-2968.000124Introduction: One of the rare complications of peritoneal dialysis catheter placement is intestinal perforation, often with a late presentation.
Clinical case: The case of a 28-year-old female with a history of placement of a Tenckhoff catheter in March 2019 is presented. She came to the emergency service in June 2020 for referring a catheter discharge by anal region.
Conclusions: Due to the low incidence of this complication, there is no standard management. In general, removal of the catheter with primary closure of the defect appears to be the best alternative.
Introduction
In Mexico, chronic kidney disease has a high prevalence, and in terminal phases it will require individualized dialysis treatment; peritoneal dialysis is one of the most widely used renal replacement therapies [1]. The most recent data from the Mexican Institute of Social Security (IMSS) report a total of 59,754 patients on dialysis; of them 35 299 (59%) are on Peritoneal Dialysis (PD) and the rest, 24 455 (41%), on hemodialysis [2]. The Tenckhoff catheter was developed by Henry Tenckhoff i1n 1968 to take advantage of the capacity of the peritoneum as dialyzing membrane; It consists of a 35 cm long silicone tube with two bearings, which has three segments: an intraperitoneal portion with multiple perforations and a radiopaque strip; an intraparietal portion with one or two dacron pads; and finally the external potion that binds to its connector. Its placement can be performed by open, percutaneous or laparoscopic surgery [3]. Although the insertion of the dialysis catheter by open technique is practically a routine surgical procedure, it is not exempt from complications, those with early appearance include infection, hematoma, leakage and peritonitis; which are found in relation to the patient's comorbidities, such as uncontrolled diabetes mellitus, poor nutritional status and concomitant sepsis. The most frequent late complication is peritonitis associated with peritoneal dialysis. One of the complications inherent to the surgical procedure is intestinal perforation, however, there are few cases reported with a low incidence of 0.4. However, larger studies are needed to ensure the risk of intestinal perforation associated with peritoneal dialysis catheter [1,3,4]. Despite the fact that the intestinal perforation is rare, it is important to recognize this clinical entity, establish a timely diagnosis and treatment.
Clinical case
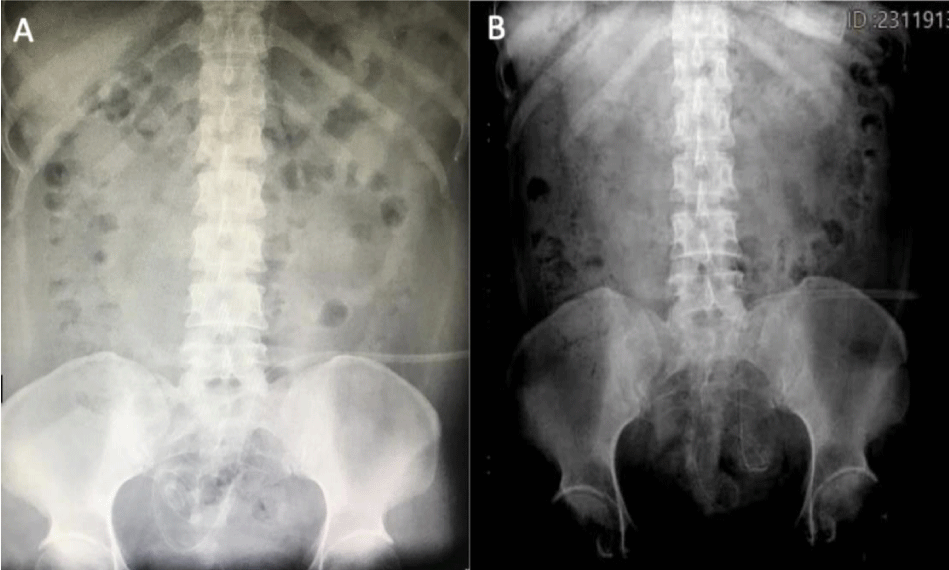
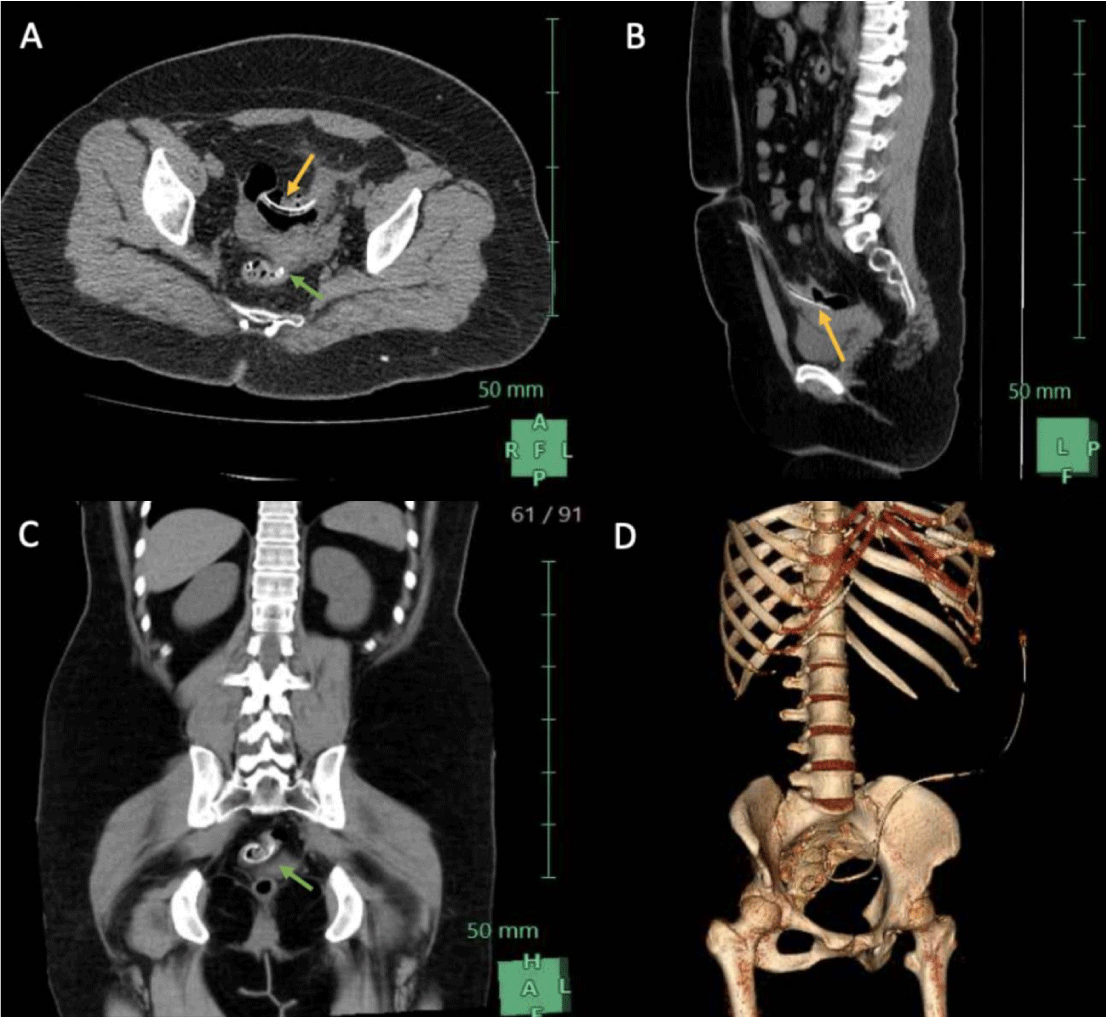
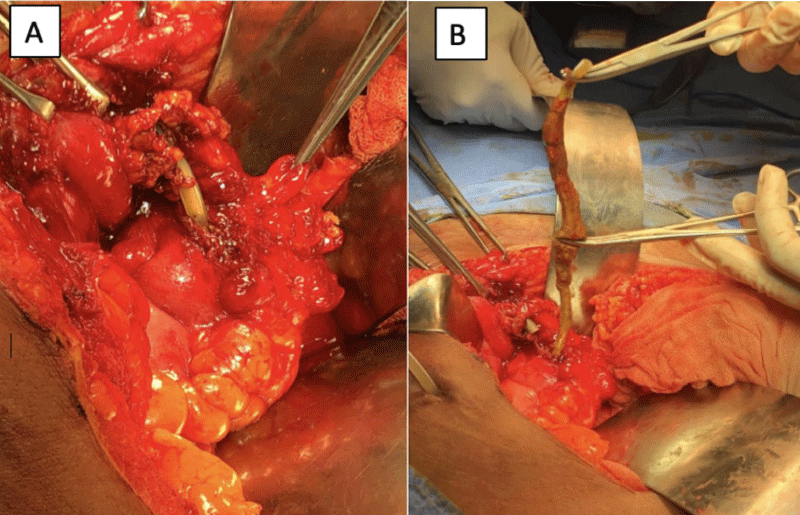
The case of a 28-year-old female is presented, with a history of 4-year diagnosis of systemic arterial hypertension on treatment with Losartan, end-stage chronic kidney disease (stage V) secondary to nephrocalcinosis on continuous ambulatory peritoneal dialysis with replacements every 10 days, during this period the patient had a course without metabolic alterations but with a delay in the entry and exit times of the dialysis solution since May 2020, the last replacement in the first days of June 2020. Surgical history: appendectomy, cholecystectomy, placement of a Tenckhoff catheter in March 2019. He came on May 2020 for evaluation to the emergency department for referring discharge of the peritoneal dialysis catheter through the anal region, with manual reintroduction of this, in addition to the presence of fecal matter in dialysis fluid exchanges receiving treatment for probable peritonitis associated with peritoneal dialysis with broad-spectrum antibiotics without improvement. On physical examination, there was no evidence of an acute abdomen, with the presence of a dialysis line with cloudy fluid inside without having fecaloid features. A plain abdominal X-ray was performed standing and in decubitus, without the presence of free subdiaphragmatic air and kinking of the Tenckhoff catheter in the pelvic hollow (Figure 1). A computerized axial tomography was performed with a third-dimensional reconstruction of the abdomen and pelvis, showing the presence of the intraluminal peritoneal dialysis catheter in the sigmoid, with its distal end in the rectum (Figure 2) admission laboratories without leukocytosis or neutrophilia. It was decided to perform an exploratory laparotomy where the following findings were described: multiple omentum-wall adhesions, which were released; A search for the catheter was carried out and the peritonized path of the catheter was found to the emblazoned sigmoid colon, the plastron was removed, finding a 1.5-cm perforation of necrotic edges in the sigmoid (Figure 3), the catheter was removed, edge debridement and primary closure of perforation in 2 planes. Subsequently, she had an adequate postoperative evolution and was discharged without complications. The patient then continued her treatment with hemodialysis every 3 days and follow-up with the nephrology service.
Discussion
Bowel perforation has been reported in 4 to 8% of patients on peritoneal dialysis, predominantly in males, associated with the use of rigid or straight catheters, especially in patients requiring acute dialysis, with a history of previous surgeries or with intra-abdominal adhesions at the time of catheter placement [3]. Obesity and hypoalbuminemia, as well as the presence of diabetes and hypertension are also associated with this complication [3]. The most common site of intestinal perforation is the sigmoid colon, as happened in our case [5]. The presence of pathology at the colonic level also represents an increased risk of perforation, with diverticulitis and colonic amyloidosis being the most related pathologies [5]. Another risk factor for perforation is the lack of use of the peritoneal dialysis catheter, since that the peritoneal fluid acts as a barrier that prevents adhesion of the catheter with the intestine, with the consequent development of is local burning, which eventually leads to erosion, laceration, and perforation [5,6]. The literature reports that perforation occurs after a period of cessation of dialysis between 1.6 and 48 months, however, in the present case the patient refers to performing only one replacement every 10 days, which may indicate that not only the cessation of dialysis, but also prolonged exchanges contribute to the appearance of this complication [4,6]. Wang, et al. conducted a review of the literature from 1980 to 2014, of cases of intestinal perforation secondary to the placement of a peritoneal dialysis catheter, finding only 28 cases with this complication. According to this study, the clinical presentation is heterogeneous, making the diagnosis complex, and includes pictures of peritonitis, watery diarrhea and protrusion of the catheter through the anus, the latter being the least frequent, appearing only in 4 patients (14%), however, its appearance and direct visualization practically establishes the diagnosis [6]. There is a report of cases of patients who remain asymptomatic, which may be due to the closure of the intestinal perforation due to the inflammatory process, the formation of adhesions and fibrosis; This is consistent with the intraoperative findings and the absence of clinical or radiological data of intestinal perforation in our patient [4,5]. In some cases, when the clinical presentation suggests a picture of peritonitis, it is difficult to determine whether it is secondary to peritoneal dialysis or a problem secondary to intestinal perforation, in these cases of doubt, imaging studies such as computed tomography and catheterization can help to establish the diagnosis, and its performance is suggested if after 3 days of conservative treatment there is no resolution of the symptoms [6-8]. Once the diagnosis is made, early surgical management with catheter removal and primary closure of the perforation generally offers a good prognosis for patients. Although there are other treatment options described, such as conservative management only with removal of the catheter without primary closure of the defect in patients without signs of sepsis or peritonitis, and even radical management with colonic resection and anastomosis. Currently, there is no consensus on the management of this type of case, so the management will be determined by the surgeon's experience and the intraoperative findings [3,4]. In our case, we opted for the removal of the catheter with primary closure of the defect, with a favorable result.
Ethical considerations
The patient authorized the use of the clinical record for the publication of this article.
Conclusion
Peritoneal dialysis catheters are intended to remain long-term in the peritoneal cavity, however, they are not entirely safe, and their presence represents a latent risk for the damage of intra-abdominal structures. Intestinal perforation secondary to a Tenckhoff catheter is one of the complications of which there is hardly any record. Due to the low incidence of this complication, there is no established management. In general, removal of the catheter with primary closure of the defect appears to be the best alternative.
- Méndez A, Chavira P, Martínez C, Orozco P, Godoy A (2007) Percutaneous placement of a Tenckhoff catheter, an ideal technique for the initiation of peritoneal dialysis. Journal of the UNAM Faculty of Medicine 50: 204-207.
- Tamayo-y Orozco JA, Lastiri-Quirós HS (2016) Chronic kidney disease in Mexico. Towards a national policy to confront it. Mexico: National Academy of Medicine of Mexico. Link: https://bit.ly/2VDfE7P
- Vargas-De la Llata RG, De Luna-hernandez P, Marquez-Rodriguez G (2015) Involuntary foreign body in the rectum. Rev Mex de Surgery of the Digestive System 4: 118-121. Link: https://bit.ly/2VxZEUw
- Quinto Ruiz J, Durón Gutiérrez CE, Romero Moreno AH, González Rosas S, Castañeda Gutiérrez AD (2017) Erosion of a Tenckhoff catheter to the sigmoid colon: an uncommon delayed complication. CEN Case Rep 6: 129-131. Link:
- Chu PY, Siu KL (2016) A rare but serious complication of continuous ambulatory peritoneal dialysis: delayed perforation of the colon by the Tenckhoff catheter. Hong Kong Med J 22: 286-288. Link: https://bit.ly/3gg7cVC
- Wang R, Chen Z, Wang J, Zhang X, Shou Z, et al. (2014) Delayed bowel perforation in a peritoneal dialysis patient: a case report and literature review. Perit Dial Int 34: 460-466. Link: https://bit.ly/2JxDyyY
- Yao J, Witherspoon L, McCormick BB, Belanger E, Warren JE (2018) Abdominal visceral perforation by buried peritoneal dialysis catheters: cause or coincidence?. Seminars in Dialysis 31: 305–308. Link: https://bit.ly/2VxGgHc
- Shima H, Mizoguchi S, Morine Y, Tashiro T, Okada K, et al. (2018) Intestinal perforation by a peritoneal dialysis catheter in which fungal peritonitis led to diagnosis: a rare case report. CEN Case Rep 7: 208-210. Link: https://bit.ly/36D7Jxn
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
