Journal of Surgery and Surgical Research
Death due to circumcision? Interest of circumcision campaigns in Africa
Thomas W Djeumi T1, Justin Kamga J2, Achille Mbassi3, Landry W Tchuenkam4*, Samuel Esembe4, Jules C Tagne1, Daniel Shu1 and Jean-Christian Youmba1
2Urology unit, Department of Surgery, Yaounde General Hospital, Cameroon
3Urology unit, Yaounde Central Hospital, Cameroon
4Faculty of Medicine and Biomedical Sciences, University of Yaounde I, Cameroon
Cite this as
Thomas W Djeumi T, Kamga JJ, Mbassi A, Tchuenkam LW, Esembe S, et al. (2020) Death due to circumcision? Interest of circumcision campaigns in Africa. J Surg Surgical Res 6(1): 008-011. DOI: 10.17352/2455-2968.000086Background: Male circumcision involves removing the foreskin that normally covers the glans of the penis. This surgery is one of the oldest and most common surgical procedures performed globally. However, in low income settings, circumcision is trivialized and sometimes done by an untrained traditional medical practitioner in the community.
Methodology: We organized a campaign in the city of Yaounde, Cameroon in 2019. The health campaign started with a theoretical and practical training of some heath providers in the hospitals. We started the preparative phase with sensitization, clinical evaluation and pre-operative workup of children.
Results: A number of 55 infants from 3 to 5years old were selected. The coagulation profile in 3 patients revealed abnormalities that were managed successfully. We circumcised all these children using a secure technique conducted by well-trained health providers according to the rules of surgery. Our technique was the Dorsal slits with 4 forceps. No complications were found during the surgeries. We had very little minor complications; a single case of bleeding and a case of infection because of poor hygiene at home which were successfully managed. Our team successfully repaired 3 unexpected cases of home circumcision accidents referred to us, initially done by untrained traditional practitioners.
Conclusion: Circumcision, though a common procedure, can be lethal. Bleeding remains the most frequently encountered complication which can be averted by a pre-operative medical evaluation, a mastery of surgical technique and post-operative care. Adequate training of all persons engaging in circumcision is fundamental in our setting to reduce the risk of these complications.
Introduction
WHO: World Health Organization; DHS: Demographic and Health Surveys; H: Hour
Background
Male circumcision involves removing the foreskin that normally covers the glans of the penis [1]. It is practised for social, cultural and medical reasons including HIV prevention. There is currently an increased interest in male circumcision services, since three randomized controlled trials have confirmed that circumcision reduces the risk of acquiring HIV infection in males [2].
This surgery is one of the oldest and most common surgical procedures performed globally. It is estimated that one in three males worldwide are circumcised, with almost universal coverage in some settings. However, in low income settings, circumcision is trivialized and sometimes done by an untrained traditional medical practitioner in the community.
Adequate training of all persons engaging in circumcision is fundamental. In order to raise awareness and reduce cases of circumcision made by untrained practitioners, health campaigns are one of the modalities. The general objective of the circumcision campaign was to provide quality care of circumcision to the population done by skilled and trained health personnel. We report a serial repair of three circumcision accident cases performed at home by a supposed health provider in a poor neighbourhood in Yaounde (Cameroon), encountered during a free circumcision campaign at Bethesda Full Gospel mission hospital in Yaounde (Cameroon).
Methodology
We conducted a descriptive study over a period of one month, the time of the campaign, in the surgical ward of Bethesda hospital. Infants above 2years were included; the exclusion criterion was refusal to sign the consent form. The study variables were: age, Prothrombin test, bleeding time, surgical technique, per operative and post-operative complications. Details of the procedure: There were 3 phases: a population awareness phase, training of hospital staff and patient registration, clinical evaluation, surgery.
Before the campaign
Sensitization: Awareness-raising was carried out within the hospital by the creation of banners in the French and English languages posted at the main crossroads of the hospital; it was also carried out via social networks and shared printed posters with religious bodies for dissemination in churches.
Staff training: Staff was trained during a 3-hours training session on the theoretical principles of safe circumcision, according to WHO recommendations and the guidelines on circumcision designed by the national urology society.
Patient registration: The patients were normally registered; each interested patient received a patient info sheet about circumcision, preparation for the intervention, the technique and its risks, potential complications as well as contact with additional questions. All patients received a reminder SMS and were called by telephone to recall their child's date and time of circumcision.
Coordination meetings: Coordination meetings were held the month before the campaign. All direct or indirect actors in the campaign could have the same level of information and take decisions in council. Participants during these meetings were: the campaign coordinator, medical doctors, nurses and the pharmacist.
During the campaign
Pre-procedure preparation & Clinical evaluation: We systematically carried out a medical consultation for each patient wishing to have a circumcision, supplemented by biological investigations in order to detect coagulation disorders. Coagulation assessment included the Prothrombin Time (PT) test and the bleeding time. Prior to performing circumcision, examination of the penis and scrotum aimed to make an operative plan and rule out contraindications to surgery which fall under exclusion criteria: Infants with serious medical conditions, Bleeding diathesis and congenital penile anomalies.
Procedure: A briefing in the presence of the entire team at the start of the campaign was carried out and debriefings at the end of the day to adjust our strategy day by day.
- After obtaining consent for all patients and guardians requesting circumcision, we premedicated with Paracetamol suppositories 15 to 30min before the intervention.
- The procedure is done under local anesthesia. We performed a penile nerve block for all patients (Dorsal penile block or ring block) using Lidocaine 1% or 2% with the maximum dose of 3mg/kg of body weight as recommended by WHO. We have provided resuscitation kit and trained personnel in resuscitation in the event of an incident.
- The surgical technique adopted was the "Dorsal slit method with 4 Forceps" for all patient.
The steps are: skin preparation (with povidone iodine) and draping; local anesthesia; marking the intended line of incision; degloving of the foreskin and adequate removal of any adhesions; applying forceps to the foreskin (4 small haemostats); cutting 02 lateral slits enabling a very minimal risk of injuring the glans as well as being easily reproducible; circumferential cutting at the foreskin; haemostasis with 3/0 absorbable sutures and reconstruction using the 4 cardinal points with absorbable 3/0 sutures and penile dressing.
There were no circumcision using devices.
Case considerations: For specific cases of slight anomalies in the Prothrombin (Tp) level, they were performed by the surgeon himself; we used a bloodless technique by carefully dissecting the fatty tissue between the mucosa and the prepucial skin, followed by good haemostasis. Exploration of these anomalies was planned later.
Post-circumcision care: Postoperative care consisted of antibiotic and sitz bath.
Results
The surgical health campaign indeed started with an awareness phase according to the methods described above. Awareness was raised in meetings, churches and other assembly points after agreement by administrative authorities. This awareness lasted almost a month before initiation of the hospital phase.
Concerning the training of practitioners, practice sessions were organized the week of August 5 to 9, 2019 during which the surgeon demonstrated and supervised the staff in the practices; a video was made and a montage was designed for the memory boost. Twenty-eight practitioners have been trained including doctors, nurses and nursing assistants from the emergency room, surgery, paediatrics and neonatology units.
The third and final phase of the campaign was the practical phase itself. We registered 80 children. Twenty-five (25) were excluded: 15 children were less than 2years old, 10 children presented with pulmonary, digestive and other medical pathologies as well as penile malformations following clinical evaluation. During our free circumcision health campaign, we performed 55 circumcisions. We had 3 out of 55 patients who had a prothrombin level below 70% and the lowest was 64%. All cases of 55 patients were operated under local anesthesia using the technique known as "Dorsal slits". No case of a major complication was identified. We had very little minor complications; a single case of bleeding and a case of wound infection diagnosed during post-operative care. These patients were successfully managed. Furthermore, we were particularly concerned about 3 patients. These were the children referred to the surgical team of our health campaign for circumcision accidents following surgery performed by a traditional healer at home.
Special cases presentation
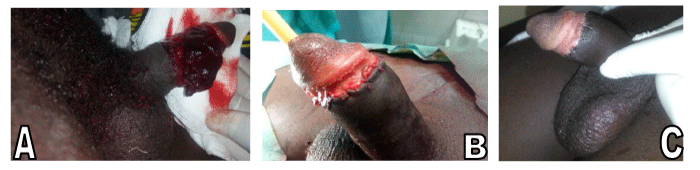
Case 1: This was the case of a 15years old brought in for consultation 6 hours after circumcision at home with excessive bleeding from the penis shaft. On admission, the patient was conscious and hemodynamically stable. Examination revealed a voluminous hematoma over the corporal bodies (Figure 1A). Pre-surgery workup notably the full blood count and the prothrombin time ruled out a coagulation disorder. Surgical exploration revealed a voluminous hematoma over the corporal bodies with complete loss of prepuce but no injury to the corpora carvenosa, corpus spongiosum or urethra. The repair consisted of copious irrigation, adequate haemostasis using electrocautery and reconstruction of the penile shaft with interrupted skin stitches (Figure 1B and 1C).
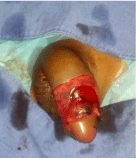
Case 2: This was the case of a 7years old younger sibling of our first index case with no relevant past history, who presented at the emergency unit for swelling of the penis after circumcision at home 24hours earlier. On examination, we noticed a mildly swollen penile shaft banded with hematoma in some places (Figure 2A). During surgical procedure, we found a large blood clot over the corporal bodies with a total loss of prepuce but no lesions of the corpora cavernosa and spongiosum or urethra. The repair consisted of copious irrigation, haemostasis with vicryl 3/o and reconstruction of the penile shaft with interrupted skin stitches (Figure 2B). Postoperative care consisted of antibiotic and sitz bath. The postoperative course was simple (Figure 2C).
Case 3: The last case was the case of an eleven years old kid with no relevant past history. He presented with a swollen penis following circumcision done under similar circumstances by the same inexperienced operator. Evaluation revealed a mildly swollen shaft banded with hematoma in some places (Figure 3). The surgical procedure was similar to that described in case 2, the post-operative was unremarkable.
Discussion
Circumcision is a very common surgical procedure in the world. In West Africa, circumcision is common among both non-Muslim and Muslim. Demographic and health surveys show a very high prevalence in numerous Sub-Saharan African countries [3]: 92.9% in Benin; 91.6% in Ghana and 88.3% in Burkina Faso. There are some variations in each country and territory. In Cameroon the prevalence is 94% [4].
The Incidence of complications is variable, depending on whether or not it has been systematically recorded in health facilities [2]. This incidence of associated adverse events is thus estimated at 2 to 6 per 1000 male circumcision in neonates [5]. This rate is multiplied by 10 if circumcision is done in children over 10 years old. They are most often due [6] to a lack of knowledge concerning the precise anatomy of the penis and associated variations; we also cite an incomplete pre-operative assessment aimed at looking for contraindications to surgery (genital abnomalities, coagulation disorders); poor surgical technique, lack of proper training and inexperienced operator as we have seen in our series of cases reported. Atikeler [7], showed that the frequency of the complications from inexperienced circumcision practitioners are more frequent and could result in severe early phase complications such as life-threatening bleeding or some late phase disorders with lifelong negative influences.
During our campaign for free circumcision, we carried out 55 circumcisions including the repair of the 3 cases earlier mentioned. We had no complication due to anaesthesia. Our surgical technique consisted of 4 steps: First was the degloving of the foreskin; penis foreskin removal using the Four Forceps guided technique based on the use of 4 small haemostats with 02 lateral slits enabling a very minimal risk of injuring the glans as well as being easily reproducible; haemostasis with 3/0 absorbable sutures; reconstruction using the 4 cardinal points with absorbable 3/0 sutures; For the cases with mild abnormalities in prothrombin time, we used a bloodless technique consisting of careful dissection of the connective tissue between the mucosa and skin of the prepuce, suture ligation and dressing with haemostatic gauze, followed by further investigation of the underlying abnormality later. During our health campaign, we had a single case of preoperative bleeding which was managed by suture ligation using an X stitch with 3/0 absorbable suture, a case presenting as mild purulent exsudation due to poor hygiene by the patient and it was managed by regular sitz baths. As found in the published literature [6], the most commonly reported complication of circumcision was excess bleeding, followed by local wound infection and urinary tract infection. Other commonly reported complications include insufficient and excessive skin removal, haematoma/abnormal swelling; abnormal scarring and anaesthetic complications. Major complications including urethral injuries, glans injury, penile amputation and urethra cutaneous fistulas were rare.
According to the WHO guidelines on circumcision [2,8], training of personnel is the key to safe circumcision practices in low income countries. Our campaign enabled us during the preliminary phases to organize a theoretical and practical training session of 28 health personnel including doctors, nurses, nursing aids working in the surgery unit and theatre, paediatrics and neonatology units and even those in the medical unit, the maternity and intensive care unit who were interested in the campaign.
Conclusion
Circumcision though a common practice can result in death. Bleeding remains the most frequently encountered complication that can be averted by preoperative medical evaluation including coagulation tests; proper intra-operative haemostasis and good postoperative wound care and follow up. Adequate training of all persons engaging in circumcision is fundamental in our setting to reduce the risks of these complications. In the event of complications, a specialist's referral may be necessary for evaluation and better management.
The authors would like to thank all the clinicians and staff of the Bethesda Missionary Hospital for the care of the patients.
Ethical considerations
Written informed consent was obtained from the guardians and parents for publication of this case report and any accompanying images.
A copy of the written consent is available for review by the Editor-in-Chief of this journal.
Any identifying material has been removed, including the patient's name, date of entry, face or any distinctive features on the pictures taken.
Authors 'contributions
TWD and JK, contributed in design of the study and writing of the manuscript.
AM and LWT, contributed in critical reading.
TWD, collected the pictures, and obtained the patient’s consent.
All authors have read and approved the final version of the manuscript.
- Circumcision (2019) Background, Pathophysiology, Epidemiology. Drugs & Diseases. Link: http://bit.ly/32tXKqz
- (2019) WHO. Neonatal and child male circumcision: A global review. Link: http://bit.ly/2SXDFWM
- Morris BJ, Wamai RG, Henebeng EB, Tobian AA, Klausner JD, et al. (2016) Estimation of country-specific and global prevalence of male circumcision. Popul Health Metr 14: 4. Link: http://bit.ly/2HTpGL9
- Kenu E, Sint TT, Kamenga C, Ekpini R (2016) Early Infant Male Circumcision in Cameroon and Senegal: Demand, Service Provision, and Cultural Context. Glob Health Sci Pract. 4: S18-28. Link: http://bit.ly/37VYgPs
- El Bcheraoui C, Zhang X, Cooper CS, Rose CE, Kilmarx PH, et al. (2014) Rates of adverse events associated with male circumcision in U.S. medical settings, 2001 to 2010. JAMA Pediatr 168: 625-634. Link: http://bit.ly/2v6pdTc
- Yiee JH, Baskin LS, Lockwood CJ (2018) Complications of circumcision. UpToDate. Link: http://bit.ly/3bZCPjw
- Atikeler MK, Geçit I, Yüzgeç V, Yalçin O (2005) Complications of circumcision performed within and outside the hospital. Int Urol Nephrol 37: 97-99. Link: http://bit.ly/3a4AWAs
- (2019) WHO. Manual for male circumcision under local anaesthesia. Link: http://bit.ly/2TbdEC9
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
