Journal of Surgery and Surgical Research
Rehabilitation of a patient with palatal defect- A case report
Sadeq Mohammed Taqi Fadhil1* and Emre Mumcu2
2Associate Professor, Head of Department of Prosthodontic, Faculty of Dentistry, Eskişehir Osmangazi University, Turkey
Cite this as
Taqi Fadhil SM, Mumcu E (2019) Rehabilitation of a patient with palatal defect- A case report. J Surg Surgical Res 5(2): 093-096. DOI: 10.17352/2455-2968.000081Defects in the jaw and face area are caused by congenital anomalies and some infections. In this study, we present a case of palatal insufficiency after maxillectomy, treated with shutter which was applied to ensure the aesthetics, phonation and functional deficiency of the patient. After epithelialization of the defect of maxillectomy, the patient was informed about the technique. Problems of prosthesis for the patient, retention, stability and insufficiency of tissue support are detailed. Further, we present the successful rehabilitation with the hollow bulb obturator.
Introduction
Defects of maxilla are usually produced by surgical removal of benign and malignant tumors, due to trauma or infectious causes. Deficiencies and disorders of stomatognathic structures or related facial components are called jaw facial defects. The speciality of dentistry, which deals with restoration and rehabilitation of maxillofacial defects with fixed or removable prostheses, is called maxillofacial prostodontics [1,2]. Total or partial surgical treatment of tumors in the maxillary region can cause chewing, phonation, aesthetic and functional disorders. If the defect occurs after removal of the upper jaw tissues, it is closed by a surgical operation. Cases without surgical reconstruction are closed with prosthetic treatment. Prosthetic treatment has an important role in the elimination of these problems. Prostheses used in the removal of maxillary defects are generally referred to as "obturator" [3].
Prosthetic treatment of maxillofacial defects has been performed for many years. In the 1500s, Ambrose used the term obturator to fix a defect in Pre maxilla by attaching a sponge piece on a palatinal plate. After that date, obturator construction concepts and methods have been developed. In general, obturator is divided into three types: surgical obturator, temporary obturator and permanent obturator [4-7].
Surgical obturators; these types of obturators on the models obtained before the operation are removed 7-10 days after the operation. Temporary obturators; It is usually converted into a treatment obturator by applying temporary treatment primers to an immediate surgical obturator. Therapy obturator is used for 3-4 months by varying the primer material frequently. Permanent obturator; Following resection, epithelization and healing of the remaining tissues can be completed and resumed after permanent resection. This period lasts for approximately 3-4 months. However, the patient's age, general condition, resection limits and size affect this duration. Radiotherapy may be delayed for up to 12 months according to the dose given.
Case Report
In this study, the patient who underwent hemimaxillectomy due to neoplasia (Adenoid cystic carcinoma), was explained about the obturation process from the first day of the surgery to the delivery of prosthesis.
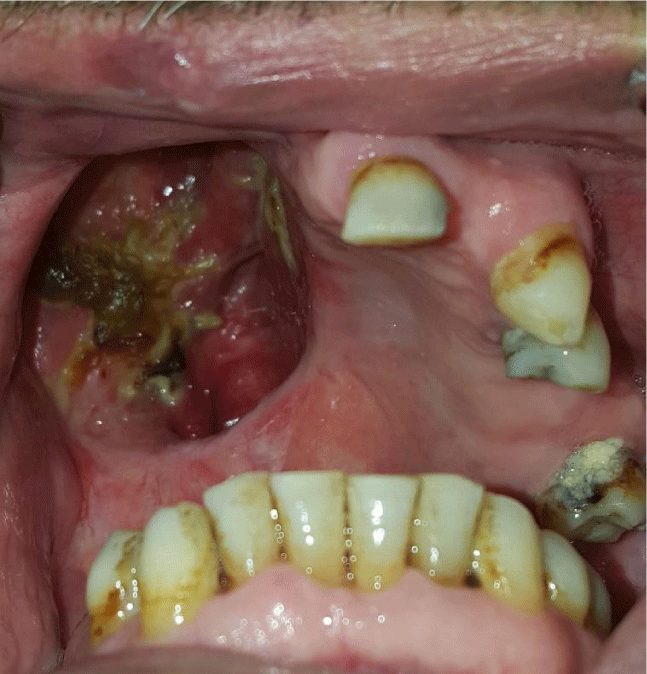
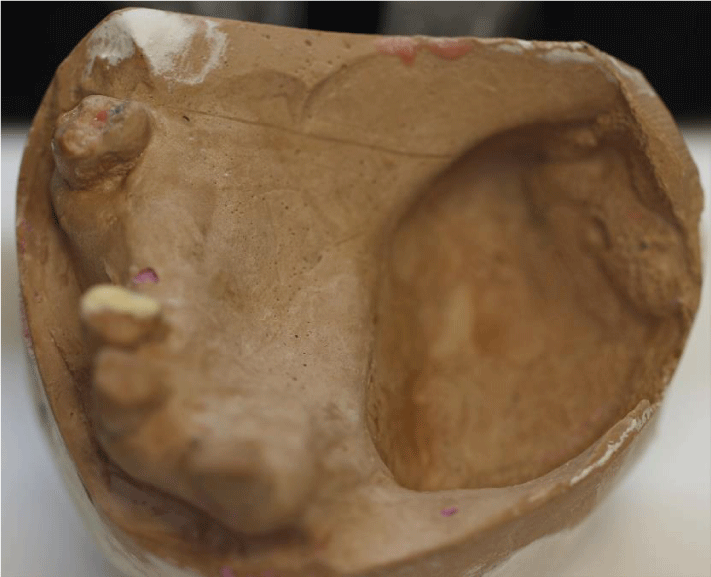
A 57-year-old patient was referred to the prosthetic dentistry clinic of Eskişehir Osmangazi University Faculty of Dentistry after maxillofacial resection and the prosthetic approach was evaluated (Figures 1,2). Preoperative measurements were taken from the patient and a plaster model was obtained. Transparent acrylic plate was printed on the obtained model. The operation limits determined by imaging techniques were plotted on the gypsum model under the guidance of the surgeon. In order to prevent a possible error, the resected area of the patient was observed during the operation and necessary modifications were made in the drawing on the model.
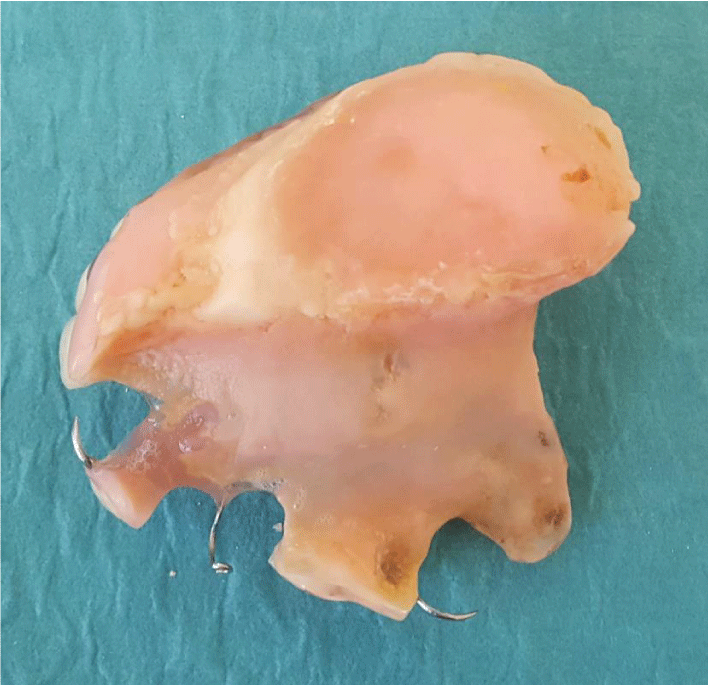
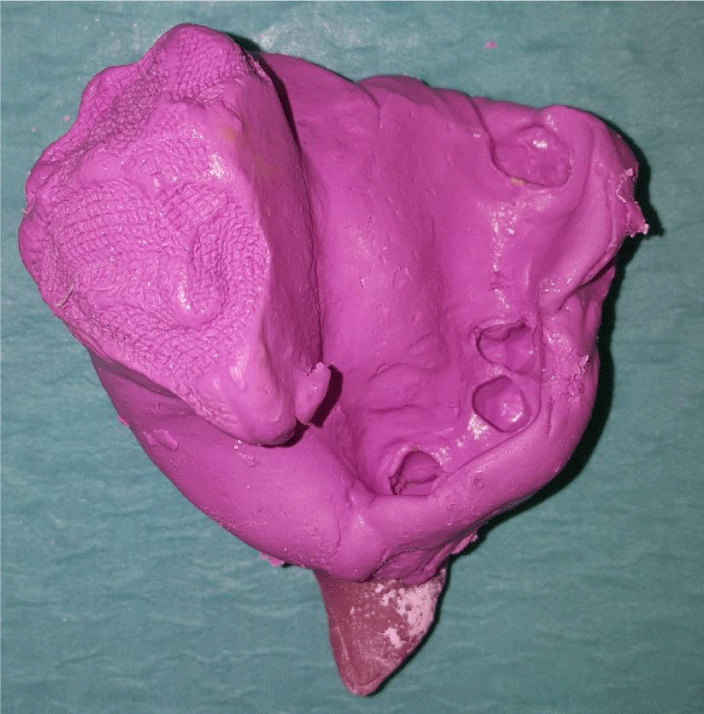
After obtaining a clear acrylic plaque, the plate was modified to make the surgical obturator on the model. To increase the retention of the plaque to the hot acrylic (Meliodent, Heraeus Kulzer GmbH, Hanau, Germany), which is equal to the thickness of a layer including the defect zone, the hooks were added. The surgical obturator was placed in the patient's mouth on the day after the operation and adaptations were made. In addition, tissue regulator (Trusoft, Bosworth Company, Skokie, IL, USA) was applied to the tissue surface of the obturator and the patient was able to use the obturator more easily. During this period, the patient was offered and monitored with exercises. At the end of 1 week, the surgical obturator was removed and a treatment obturator was prepared using tissue healing materials (Softone, Bosworth Company, Skokie, IL, USA) on the surgical obturator. (Figures 3,4). This obturator was used for approximately 12-13 weeks and was controlled for two weeks and the tissue healing material (Softone, Bosworth Company, Skokie, IL, USA) was renewed. Wound status was considered for deciding whether or not to take control and measure the patient's irreversible hydrocolloid (Blueprint, Dentsply, Konstanz, Germany) with a clear measure taken and made of a personal spoon. A personal spoon was used to obtain a functional measure of the defect region (Figures 5,6).
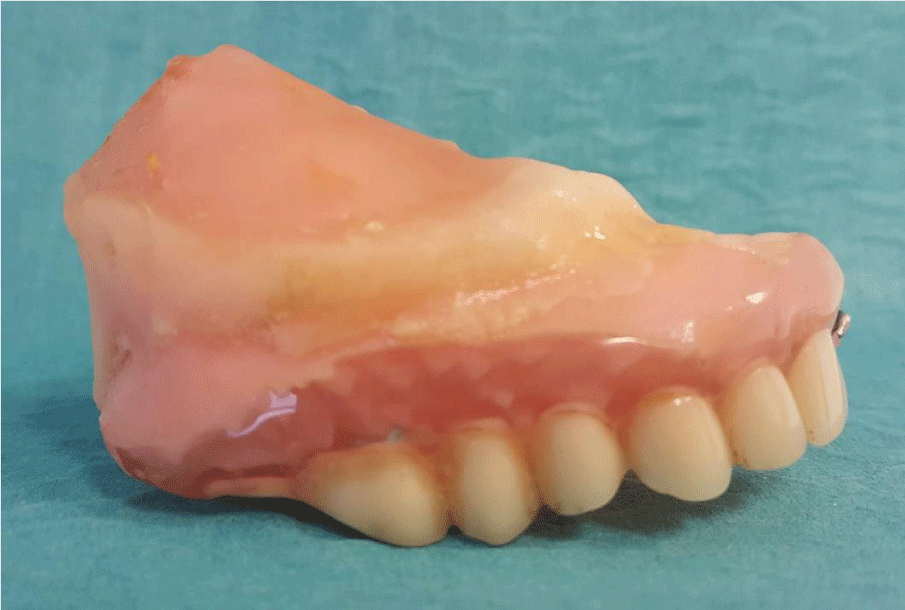
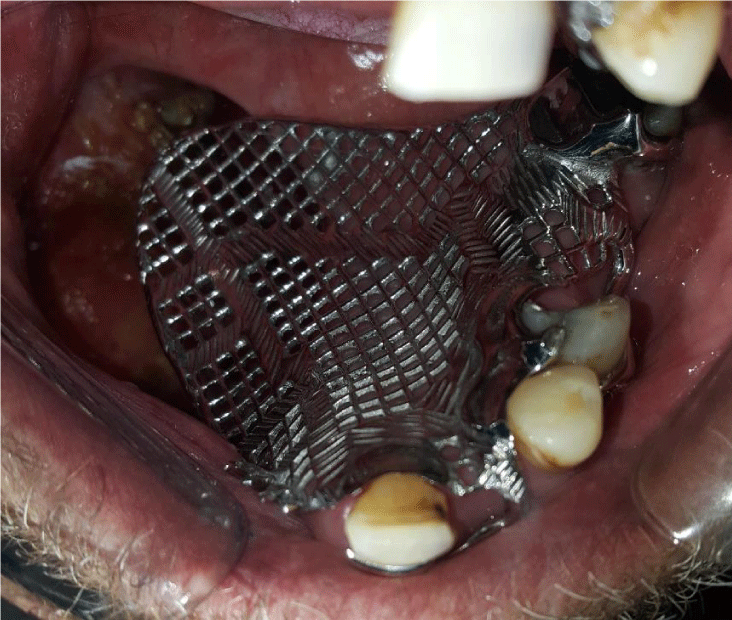
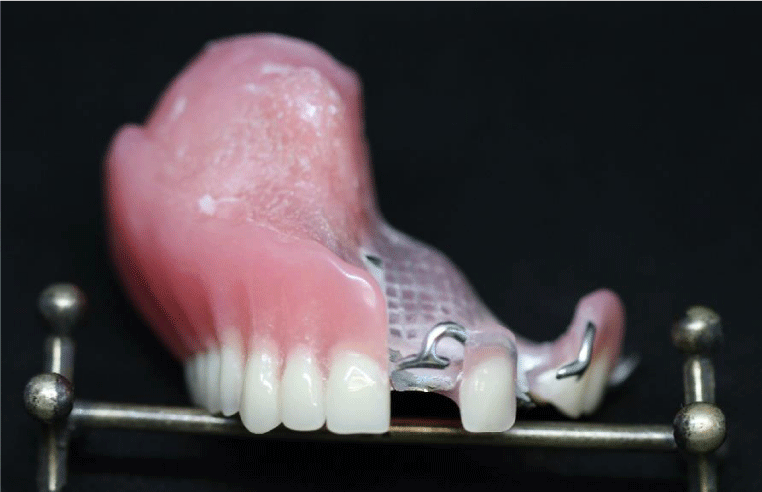
Although the resection area was large, it was determined that the existing teeth and residual alveolar crest may provide adequate support to the obturator and the patient was planned to have a shutter. The lower jaw teeth of the patient were rehabilitated with a conventional lower full denture. After, taking support from the remaining solid teeth in the mouth to increase the retention of the shutter, all soft palate, defect region and a skeletal substructure compatible with teeth were obtained(Figures 7,8). Acrylic plaque was made on the grill section on the defect region of the skeleton infrastructure and the plate was extended to 3-4 mm in the defect area. Approximately 1 cm depth of defect was obtained by functional measurement. The obtained measurement was taken into muffle. After the wax discharge process, hollow bulb obturator type superstructure has been completed by using pumice core method. Then, the wax pattern was made to the obturator which was close to the perfectness of the tissue. After determining a correct vertical closure, the closing record is fixed (Figures 9,10).
In this way, the patient's aesthetic and functional expectations were considered. After the laboratory procedures were completed, the prosthesis was delivered to the patient and necessary controls were made in the mouth. The patient was referred to the controls at 15 days, 1 month and 3 months period (Figures 11).
Discussion
Closure of the defect after maxillary resections is of great importance in terms of patient rehabilitation. This closure process was done in the form of the introduction of thermoplastics such as Güta-percha and Stenç [4,8]. However, this type of closure is not suitable for hygiene and patient rehabilitation. In order to overcome the problems after the surgery, it is necessary to motivate the patient about oral hygiene. Although it is possible to provide this in mature patients, it is not very successful in providing this motivation for children.
The greatest problems of obturators after maxillectomy include retention, stability and insufficiency of tissue support. The frame design of conventional skeletal substructure-supported obturators is used in various retention components to increase the retention [9-11]. The rehabilitation of patients with partial maxillectomy compared to patients with conventional partial prosthesis requires more knowledge, experience, teamwork, and expertise. Skeleton design for obturator; The basic principles of the prosthetic design of the movable part should be reviewed. The major binder must be rigid, occlusal nails must be able to transmit the forces coming to the teeth parallel to the long axis of the teeth and retention should be within the physiological limits of the periodontal tissues [12]. Aramany reported that in Class II, where the contralateral side and the anterior teeth were protected, the possibility of displacement of the prosthesis would be minimized by suitable retaining designs. The tooth-assisted case presented in this paper was prepared as a retentative mesh of the main binder to increase the retention of the obturator prosthesis and to be slightly resistant to the prosthesis [13].
When deciding on the design of the body for the obturation process after maxilla resection, the characteristics such as oral hygiene, the size of the defect and the need for conservatism should be evaluated [10]. Before the obturator is made, the size of the defect, the weight of the obturator, the comfort of the patient and the force of the obturator on the teeth should be considered [14]. In a study, balloon obturators were reported to attenuate the obturator weight in values ranging from 6.5 to 33.06% [15]. However, these values were compared with monobloc filled prostheses. If the core method is correctly applied during the obturator construction, hollow bulb obturators will have no disadvantage in terms of weight [15,16]. Because the cavity walls in the obturator superstructure will be homogenous thickness. For these reasons, open-space obturator was preferred in the case presented in our study. The biggest problem of open-space obturators is that the polishing process on the inner surfaces of the acrylic part, which is located in the defect zone and which is considered as a pool, cannot be performed completely [17].
Prosthetic approaches to be used in cases of maxillectomy have a very important role in improving the quality of life of the patient. The superstructure of the obturators entering certain proportions within the nasal defect contributes to the realization of the ironical separation, stability, and retention, thus, the patient's aesthetic and phonation expectations were provided. The form and height of the superstructure are important, but it should be noted that the weight of the obturator will lead to the loss of restraint and also to the propelling forces in the supporting teeth [18,19].
In many studies, it was investigated how different obturator designs affect the chirping properties of the obturators and the speech. Open-ended and closed-space obturators with different medial and lateral wall heights were used in the study. As a result, open space obturators with low medial wall height have been reported to be more successful. In the present case, it was observed by the researchers that phonation was positively affected in the controls after prosthesis delivery [10,20].
Conclusion
Obturators contribute function, aesthetics, phonation and psychological to the patient. The well-established multidisciplinary relationship between surgical and prosthetic physicians plays a major role in achieving these goals. Open macular obturators may be preferred in maxillectomy cases without skin graft application.
- Adisman IK (1990) Prosthesis serviceability for acquired jaw defects. Dent Clin North Am 34: 265-284. Link: http://bit.ly/2QH9ylm
- Martin JW, Lemon JC, King GE (1994) Maxillofacial restoration after tumor ablation. Clin Plast Surg 21: 87-96. Link: http://bit.ly/2QEwh1t
- Sun J, Shen Y, Li J, Zhang ZY (2011) Reconstruction of high maxillectomy defects with the fibula osteomyocutaneous flap in combination with titanium mesh or a zygomatic implant. Plast Reconstr Surg 127: 150-160. Link: http://bit.ly/35oxQon
- Beumer J, Curtis TA, Firtell AD (1979) Maxillofacial rehabilitation. 90-169.
- Keskin H, Özdemir J (1995) Çene yüz protezleri. 145-74.
- Lang BR, Bruce RA (1967) Presurgical maxillectomy prosthesis. J Prosthet Dent 17: 613-619. Link: http://bit.ly/2OFOcT8
- Kipfmueller LJ, Lang BR (1972) Presurgical maxillary prosthesis: an analysis of speech intelligibility. J Prosthet Dent 28: 620-625. Link: http://bit.ly/33dKgOl
- Curtis TA (1967) Treatment planning for intraoral maxillofacial prosthetics for cancer patients. J Prosthet Dent 18: 70-76. Link: http://bit.ly/34bMqj5
- Alfonso C, Toothaker RW, Wright RF, White GS (1999) A technique to create appropriate abutment tooth contours for removable partial dentures. J Prosthodont 8: 273-275. Link: http://bit.ly/2Oc5p7i
- Dos Santos DM, de Caxias FP, Bitencourt SB, Turcio KH, Pesqueira AA, et al. (2018) Oral rehabilitation of patients after maxillectomy. Br J Oral Maxillofac Surg 56: 256-266. Link: http://bit.ly/2OapDPa
- Aramany MA (1978) Basic principles of obturator design for partially edentulous patients. Part I: classification. J Prosthet Dent 40: 554-557. Link: http://bit.ly/2OxLEq4
- Keyf F (2001) Obturator prostheses for hemimaxillectomy patients. J Oral Rehabil 28: 821-829. Link: http://bit.ly/37t1mva
- Aramany MA (1978) Basic principles of obturator design for partially edentulous patients. Part II: design principles. J Prosthet Dent 40: 656-662. Link: http://bit.ly/2XHBAyL
- Parr GR, Gardner LK (2003) The evolution of the obturator framework design. J Prosthet Dent 89: 608-610. Link: http://bit.ly/2qABgFY
- Devlin H, Barker GR (1992) Prosthetic rehabilitation of the edentulous patient requiring a partial maxillectomy. J Prosthet Dent 67: 223-227. Link: http://bit.ly/2QIdEK6
- Rilo B, Dasilva JL, Ferros I, Mora MJ, Santana U (2005) A hollow‐bulb interim obturator for maxillary resection. A case report. J Oral Rehabil 32: 234-236. Link: http://bit.ly/37uinoE
- Sharaf MY, Ibrahim SI, Eskander AE, Shaker AF (2018) Prosthetic versus surgical rehabilitation in patients with maxillary defect regarding the quality of life: systematic review. 22: 1-11. Oral Maxillofac Surg Link: http://bit.ly/2Xz4pNS
- Breeze J, Rennie A, Morrison A, Dawson D, Tipper J (2016) Health-related quality of life after maxillectomy: obturator rehabilitation compared with flap reconstruction. Br J Oral Maxillofac Surg 54: 857-862. Link: http://bit.ly/2s2tZis
- Wang F, Huang W, Zhang C, Sun J, Qu X (2017) Functional outcome and quality of life after a maxillectomy: a comparison between an implant supported obturator and implant supported fixed prostheses in a free vascularized flap. Clin Oral Implants Res 28: 137-143. Link: http://bit.ly/2s7yhoV
- Kwon HB, Chang SW, Lee SH (2011) The effect of obturator bulb height on speech in maxillectomy patients. J Oral Rehabil 38: 185-195. Link: http://bit.ly/2QHNEPc
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.





 Save to Mendeley
Save to Mendeley
