Journal of Surgery and Surgical Research
Vacuum-assisted foetal delivery device to remove a rectal foreign body – A novel application of the Ventouse method
Basilie Teoh*, Raaj Chandra, Jacob McCormick and Ran Li
Cite this as
Teoh B, Chandra R, McCormick J, Li R (2019) Vacuum-assisted foetal delivery device to remove a rectal foreign body – A novel application of the Ventouse method. J Surg Surgical Res 5(1): 034-035. DOI: 10.17352/2455-2968.000066Rectal foreign bodies (RFBs) are an unusual emergency presentation readily confirmed via clinical examination and imaging, which must be quickly removed due to the risk of rectal wall tissue damage leading to perforation and subsequent peritonitis. Several non-operative methods are described in the literature to retrieve RFBs, however removal can be especially difficult if they not easily graspable, for example a ball-like object. We present the case of a spherical RFB successfully extracted using a vacuum-assisted delivery device.
Introduction
Rectal foreign bodies (RFBs) are a common surgical emergency that can pose a challenge for clinicians to manage. Timely removal is a priority as there is a risk of rectal perforation causing peritonitis. To date, there has been scarce literature describing the use of Ventouse (vacuum-assisted) extraction to facilitate this, with only one other known report of a spherical object in the rectum being removed using vacuum extraction [1]. We report the case of a male patient who presented with a spherical rectal foreign body, which was safely removed using the Ventouse method.
Case Report
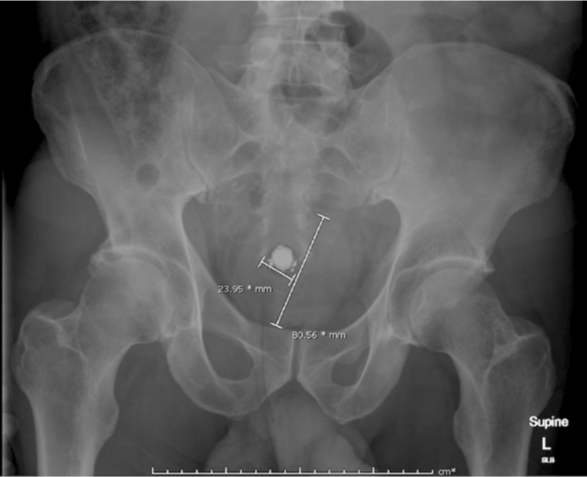
A 58-year-old man presented to our emergency department with mild lower abdominal discomfort, several hours after insertion of a rubber ball per anus by his partner and multiple unsuccessful attempts at self-removal. His medical history included hypertension and hypercholesterolaemia. On examination, he was haemodynamically stable with a soft and non-tender abdomen, and digital rectal examination identified no external trauma, with a palpable firm, round object approximately 4cm from the anal verge, unable to be removed in the emergency department. A plain abdominal X-ray revealed a radio-opaque circular foreign body 80mm in diameter, with no evidence of bowel obstruction or free intra-abdominal gas to indicate colonic perforation (Figure 1).
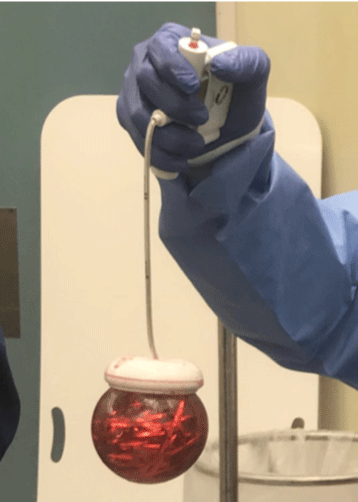
He subsequently underwent an examination under general anaesthetic in theatre the same day. A digital rectal examination was repeated in the lithotomy position, and again the round RFB was unable to be removed by hand or graspers. A vacuum-assisted foetal delivery device, the Kiwi OmniCup® with PalmPump™ (Clinical Innovations, Utah, USA) was employed to apply suction to the ball followed by successful removal with traction (Figure 2). Multiple initial attempts with the vacuum-assisted device were unsuccessful due to insufficient suction; the ball would become dislodged at the pelvic outlet due to the tightness of the pelvic floor musculature and adjacent bony structures. The technique was improved by applying a water-based lubricant to the suction cup to create a superior seal, and this increased suction allowed for easy removal of the RFB. A rigid sigmoidoscopy was then performed to inspect the rectal mucosa, which showed no signs of bleeding or injury. The patient had an uneventful recovery and was discharged home the same day after observation.
Discussion
Patients with RFBs usually have delayed presentations to the emergency department seeking help with removal after unsuccessful self-attempts, or may present with vague lower abdominal pain or rectal bleeding – rarely do they present with an acute abdomen [2,3]. The most common reason for object insertion is sexual gratification, however due to the sensitive nature of the presentation patients may not be forthcoming with details, with many citing accidental insertion [2,4]. Other circumstances include assault and “body packing” for concealing objects [4]. As such, the true incidence of this phenomenon is unknown, though most patients are male with a male: female ratio reported to be as high as 28:1 [5], and the majority of patients are between 30 to 40 years old [6].
Clinical examination of the abdomen is generally unremarkable unless peritonism has resulted from colonic perforation, with digital rectal examination being the key to assessment for identifying a RFB – however, it may not be palpable if high lying (above the rectosigmoid junction) [5]. A plain abdominal X-ray is usually sufficient to confirm the presence of a radiopaque RFB, along with size, number, shape and location, as well as the presence of free intra-abdominal gas, and computerized tomography of the abdomen and pelvis can aid in identifying radiolucent items or bowel obstruction, abscess or perforation [4,7].
Management of RFBs should be systematic, and aim for extraction without causing further bowel wall or anal sphincter complex injury [8]. Non-operative transanal removal should be trialled first – this can be performed with or without sedation, though poor patient tolerance may require examination under anesthesia. Instruments such as grasping forceps, obstetric forceps or bone cutters can be utilized to help grasp or break the object into more easily retrievable pieces, although these devices can also cause significant injury to the rectum and surrounding structures including perforation [5]. Endoscopic removal by flexible sigmoidoscopy may aid in removing smaller objects, though care must be taken not to push the RFB proximally [5]. Peritonitis and failure to retrieve the object transanally or endoscopically are indications for laparotomy [8]. After successful extraction, the rectosigmoid mucosa and anal sphincter must be thoroughly examined to rule out injury that may require repair.
In our case, use of the obstetric vacuum-assisted delivery device prevented the need for laparotomy to remove the RFB. There were three key learning points from our experience: the RFB must be round with a smooth surface to fit the shape of the suction cup, lubricant must be applied to form a seal for adequate suction, and maximum suction as shown on the vacuum indicator must be applied (beyond the advised safe limit for use in obstetrics). Similar to foetal delivery, the operator must use a finger to check that no rectal tissue is trapped between the cup rim and RFB. Once tissue clearance is confirmed, the cup seal should be increased to over 600mmHg (red zone on the vacuum indicator). Constant traction force is then applied in conjunction with gentle pendulum movements and the RFB can be gradually extracted.
The removal of RFBs can be challenging for clinicians, with large, hard round objects being especially difficult to retrieve due to their inability to be easily grasped. Although vacuum-assisted delivery devices are designed for foetal delivery, their use can be considered as a safe option for spherical RFB removal, and may prevent the need for laparotomy.
- Feigelson S, Maun D, Silverberg D, Menes T (2007) Removal of a large spherical foreign object from the rectum using an obstetric vacuum device: a case report. Am Surg 73: 304-306. Link: https://goo.gl/S2WDzE
- Cawich SO1, Thomas DA1, Mohammed F1, Bobb NJ1, Williams D, et al. (2017) A management algorithm for retained rectal foreign bodies. Am J Mens Health 11: 684-692. Link: https://goo.gl/1YnqTk
- Gajjar RA, Gupta PB (2016) Foreign body in the rectum: a challenge for the emergency physician. J Family Med Prim Care 5: 495-497. Link: https://goo.gl/e3tPpt
- Ayantunde AA (2013) Approach to the diagnosis and management of retained rectal foreign bodies: clinical update. Tech Coloproctol 17: 13-20. Link: https://goo.gl/dUCgU3
- Clarke DL1, Buccimazza I, Anderson FA, Thomson SR (2005) Colorectal foreign bodies. Colorectal Dis 7: 98-103. Link: https://goo.gl/j2JaHk
- Kasotakis G, Roediger L, Mittal S (2012) Rectal foreign bodies – a case report and review of the literature. Int J Surg Case Rep 3: 111-115. Link: https://goo.gl/tcjiqD
- Rodríguez-Hermosa JI1, Codina-Cazador A, Ruiz B, Sirvent JM, Roig J, et al. (2007) Management of foreign bodies in the rectum. Colorectal Dis 9: 543-548. Link: https://goo.gl/ua68oR
- Lohsiriwat V (2016) Anorectal emergencies. World J Gastroenterol 22: 5867-5878. Link: https://goo.gl/7pMHhK
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
