Journal of Surgery and Surgical Research
Pathological lumbar hernia following recurrent retroperitoneal abscess
Tiffany J Cherry*, Ran Li and Rezvaneh Shakerian
Cite this as
Teoh B, Campbell N, Flanagan P, Campbell I (2019) Pathological lumbar hernia following recurrent retroperitoneal abscess . J Surg Surgical Res 5(1): 029-031. DOI: 10.17352/2455-2968.000065Lumbar hernias are a rare clinical presentation and are usually congenital, traumatic or spontaneous. We describe an unusual case of a pathological lumbar hernia due to recurrent retroperitoneal abscesses, likely precipitated by chronic tip appendicitis. A literature search of PubMed with the search terms “lumbar OR flank AND hernia” and “abscess” found only one similar published case.
Case History
A 69-year old female presented initially with a painful right flank mass with overlying erythema and systemic symptoms of fevers and fatigue. She had a past medical history of hypertension, asthma, and Hepatitis B infection which had been eradicated. A CT scan demonstrated a large right sided retroperitoneal abscess (12x10x12 cm) located immediately inferior to the right kidney, extending down into the pelvic inlet, effacing and compressing psoas major against the lumbar spine and extending laterally into the subcutaneous tissues of the abdominal wall. This required open drainage via a small flank incision, with 1.2 litres of purulent fluid drained. She required post-operative admission to the Intensive Care Unit for inotropic support in the setting of sepsis. The fluid grew Citrobacter koseri, Klebsiella pneumoniae, and Bacteroides fragilis which required prolonged antibiotic treatment. She was thoroughly investigated for the presence of atypical infections and malignancy. An outpatient colonoscopy showed no abnormalities to explain the development of this abscess.
Two years later she re-presented with pain over the right iliac crest, particularly with walking, and was found to have cellulitis on examination over the right gluteal area. CT demonstrated an abscess in the right retroperitoneum extending through the iliacus muscle into the subcutaneous tissues, which was drained percutaneously. The CT also demonstrated that the appendix tip was in continuity with the abscess and showed evidence of inflammatory changes, while the proximal retrocaecal appendix had normal radiological appearance. A follow-up scan two weeks later showed resolution of the collection and the drain tube was removed.
Over the proceeding seven months, the patient had three further presentations with similar local symptoms over the right flank and gluteal area consistent with recurrence of the retroperitoneal abscess. This was managed with percutaneous drainage. Each time, serial scans demonstrated resolution of the abscess cavity before the drain tubes were removed and antibiotics were targeted to the aspirated fluid culture. The patient did not have abdominal pain, altered bowel habits, anorexia or other symptoms or signs suggestive of appendicitis or an underlying colonic malignancy during any of her five presentations. A second colonoscopy, performed two years after the index presentation, did not identify any causative pathology.
Approximately three years after her initial presentation the patient underwent elective diagnostic laparoscopy and appendicectomy. This was performed due to the radiological finding of inflammation of the appendiceal tip and the multiple recurrent abscess episodes. The histopathology demonstrated distortion of the mucosa of the tip of the appendix, with fibrosis and chronic inflammatory infiltrates, consistent with previous tip appendicitis. The proximal appendix was normal.
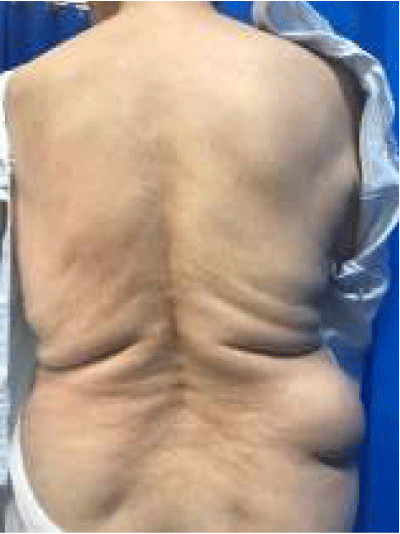
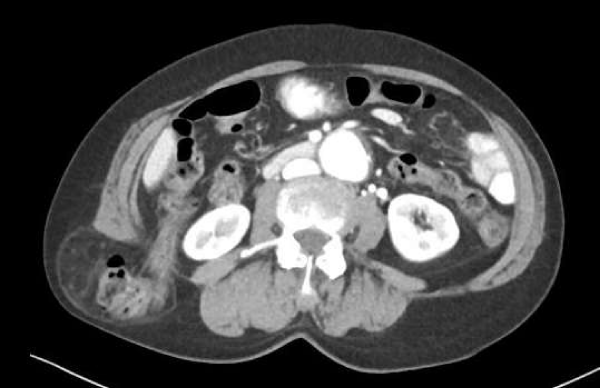
A year later she was referred for review in clinic with a large right-sided flank hernia. A CT demonstrated a 4.6 cm defect between the fascia of quadratus lumborum and the right external oblique and transversus abdominis. The hernia sac extended laterally to Latissimus dorsi, into subcutaneous tissue just above the iliac crest and contained distal ascending colon and hepatic flexure without evidence of obstruction. Her main presenting complaint was that of intermittent pain and dragging sensation. On examination there was a large, reducible right flank hernia without overlying skin changes (Figures 1,2).
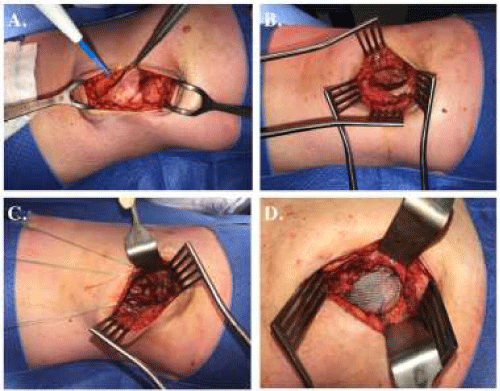
The patient underwent elective open repair of the right flank hernia. A transverse incision was made superior to the iliac crest, with a large hernial sac protruding lateral to quadratus lumborum, through a defect in the external oblique and emerging posterior to latissimus dorsi. This location confirmed the pathological nature of the hernia. After inspecting and reducing the contents of the hernia, the residual 6x4x5 cm defect was repaired using inlay prolene mesh. There was no viable fascia superior to the iliac crest and three Mitek bone anchoring screws were inserted into the iliac crest to support the mesh inferiorly (Figure 3). At the time of publication there has been no hernia recurrence.
Discussion
This case of a pathological lumbar hernia secondary to recurrent retroperitoneal abscess is very unusual and previously not described in the literature. A review of PubMed with the search terms “lumbar OR flank AND hernia” and “abscess” revealed only one similar case [1]. While the circumstances are unique, the principles of diagnosis and repair are the same. CT was useful in diagnosing and delineating the anatomy of the hernia. Lumbar hernias are usually divided into defects through the superior triangle (of Grynfeltt) or inferior triangle (of Petit). In this case, the hernia was more direct, and almost certainly due to inflammatory changes in the muscle after recurrent infections. It is possible that the previous open incision and multiple subsequent percutaneous drainages further damaged the muscle wall, contributing to hernia development. In planning for repair of this hernia, pre-operative imaging, clinical examination and pathology confirmed no major residual infection before laying the mesh. While there is ongoing contention over the use of laparoscopic versus open methods for lumbar hernia [2], in this case the need to use bone anchoring screws necessitated an open approach.
- Ali SM, Subramaniam S (2017) Appendicular abscess as an unprecedented cause of an inferior lumbar hernia. Ann R Coll Surg Engl 99: e85-e87. Link: https://goo.gl/P8Vyp2
- Moreno-Egea A, Baena EG, Calle MC, Martinez JA, Albasini JL (2007) Controversies in the current management of lumbar hernias. Arch Surg 142: 82-88. Link: https://goo.gl/Ynnywn
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
