Journal of Neurology, Neurological Science and Disorders
Traumatic Brain Injury in the Elderly is common but is not as Bad as we Think! Exercise, not rest, can ensure faster recovery from post-concussion syndromes “Autobiographical case report”
Suresh Kishanrao*
Cite this as
K Suresh (2021) Traumatic Brain Injury in the Elderly is common but is not as Bad as we Think! (Exercise, not rest, can ensure faster recovery from post-concussion syndromes “Autobiographical case report”). J Neurol Neurol Sci Disord 7(1): 027-033. DOI: 10.17352/jnnsd.000045Copyright
© 2021 K Suresh. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Head injuries, medically known as Traumatic Brain Injuries (TBI) are a leading cause of seeking emergency medical care, hospitalization, long hospital stays, disabilities, rehabilitation services, case fatalities and socioeconomic losses in India. Head trauma is one of the common injuries in the old due to trivial falls, and its consequences need not be grievous always. As many of the elderly are on medication for hypertension, diabetes, and heart ailments and due to sudden rising from the bed, or even from the commode or Indian style of squatting plate develop giddiness and fall.
Incidence of head injuries is rising all over the world but fortunately more than half of them is either mild or moderate amenable to management with good outcomes. They can sometimes be serious and fatal when left untreated. The epidemiology of TBI is still an enigma in the medical world due to inconsistency in the definition and classification and discrepancies in data collection.
Glasgow Coma Scale (GCS) is a well-accepted tool to assess the seriousness at the first visit to stratify, monitor the prognosis, and recovery of brain functions in patients with traumatic brain injury. Seniors over the age of 60 years with head injury are generally considered to have a poor outcome. However, a recent large multicentric China epidemiologic study of minor head injury patients (GCS 13–15) reported over 90 % survival, few with minor consequences. Another large-scale retrospective study at a level II trauma centre in Florida from 2005 to 2008, too indicated that the outcome of elderly over 65 years old had a survival rate of over 80 %.
I report my own autobiographical case of a closed head injury, with good outcome due to timely care and early initiation of aerobic exercise (waking & tread meal) for recovery from concussion injury due to fall in washroom, with no major post-concussive symptoms.
Introduction
Incidence of head injuries (Traumatic Brain Injuries-TBI) are a leading cause of seeking emergency medical care, hospitalization, long hospital stays, disabilities, rehabilitation services, case fatalities and socioeconomic losses in India. Open or penetrating injuries form a small portion while most of the injuries are closed ones. The Closed head injury (blunt TBI) is caused by an external force strong enough to move the brain within the skull, that include falls, motor vehicle crashes, sports injuries like Cricket, hockey, getting struck by an object. While Road traffic injuries are the leading (60%) causes in general population, among elderly it was noted that trivial injuries due to domestic falls contributed most to the head injuries and their consequences [1]. The overall TBI information is not available in India due to lack of systematic collection efforts across the country [1].
The existing literature review on mTBI dysfunctions, based on its neuroimaging correlates, and on its relation to neuropsychological assessment, indicate that, despite substantial research on the relationship between brain structure, brain function and cognition, certain cognitive subdomains like planning, decision-making, inhibition response, visual perception, and receptive language have not been adequately studied, and the importance of social dysfunction after mTBI has been understated. Most of the study observations are made on combined group of mild (mTBI) and moderately severe TBIs (msTBI). Comparison of mTBI patients as a function of their subsequent cognitive and clinical outcome would be particularly beneficial, since not all mTBI individuals continue to exhibit Post-Concussion Syndromes (PCSs), and this effect may confound results if not considered. One of the recent published reports having systematically reviewed mTBI-related deficits and their cognitive assessment, has concluded that further knowledge synthesis in this research area requires future studies to focus on the rigorous and methodical assessment of cognitive subdomains and of their components, rather than on overarching cognitive domains, as still are being done for attention, Learning &Memory and Executive Functions [2].
This autobiographical care report is unique as the observations of a physician himself of self-progress seconded by a surgeon and neurosurgeon’s assessment. Most of other individual cases reported are assessed by physicians independently and the informed patient’s contribution was minimal.
Epidemiology of TBI
The epidemiology of TBI is still an enigma in the medical world due to inconsistency in the definition and classification and discrepancies in data collection. Many head injury patients dying at the scene of the accident or during transport to a hospital may not get reported at all. Similarly, some others getting discharged from the Emergency Department (ED) itself may not be documented fully. The differences in findings from diagnostic imaging CT scan at different time intervals and the human errors of the professional inferring the CT scan will also add to the complexity. For example, the CT scan may be normal immediately after injury, but a repeat scan is later may show evidence of pathology [3-6].
Globally 50 million persons get injured every year, resulting in 1.2 million deaths with an annual mortality 97/1,000,000 population. In India, 1 out of 6 trauma victims die, while in the United States this figure is 1 out of 200. In India one person died in every 6 to 10 minutes in 2002 and it is estimated that in 2020 one such death will be there every 3 minutes [5]. The incidence of Head injuries by categories in USA was reported as i) mild TBI - 131 cases, ii) the moderate TBI - about 15 cases iii) the severe TBI – 14 /100,000 people each. If prehospital deaths were included the number would rise to 21 per 100,000 people [4]. As per the annual report of NIMHANS for 2019-20 in the city of Bangalore alone, 10,000 individuals sustained brain injury and about 1,000 died [5]. Even the anecdotal data is 5 years old. NIMHANS in Bengaluru on every day basis registers 20 - 25 patients of a head injury. TBIs among elderly accounted for 5%, only. The male to female ratio was 4:1. Falls were the second-leading cause (25%), most of them occurring in children and elderly [1,5]. Accidental falls at home (26%), falls from stairs/steps (22%) and fall from building (14%) were the common pattern of fall injuries [5].
The common severe head injuries include
Concussion: Concussions, the most common head injuries occurs when the brain slams against the skull. A concussion is a type of TBI, caused by a bump, blow, or jolt to the head that can change the way your brain normally works. Concussions can also occur from a fall or a blow to the body that causes the head and brain to move quickly back and forth. They usually heal well, but repeated concussions can develop into some serious issues. Post-concussive symptoms are not associated with the severity of the initial injury and usually occur within the first seven to 10 days [5,6].
Hematoma: When a blood vessel in the brain ruptures, it can lead to collection and clotting of blood, and manifest as a bump that may not be noticed until a few days after your injury. There are 3 types namely, intracerebral, epidural, and subdural hematomas depending upon where the clot is located.
Skull fracture: When the cracks due to direct hit it can cut into the brain.
Oedema: Oedema or brain swelling can occur with any TBI, that can further damage to the brain [5].
Glasgow Coma Scale (GCS) is used as a tool to stratify risk, prognosis, and neurological recovery in patients with traumatic brain injury. In multiple traumas, other serious injuries may increase the risk, morbidity, and mortality.
I report an autobiographical case of a mild TBI after a fall in the bathroom. I had a fall in the washroom resulting in an external lacerated cut of about 4 inches in the left occipital region of the scalp, and I was in syncope for about 4 hours. Active bleeding had almost stopped due the pressure of the head on the pillow and clotting phenomenon with about 2 litres of blood lost when I got consciousness back around 0700 hrs.
Case
a) Patient description
I am an elderly male of 76 years, with an average built and known diabetic for 30 years and having undergone CABG in August 2005. After the day’s lunch I had food poisoning symptoms of diarrhoea since the 1900hrs of the evening of 17 August 2021.
b) Case history
Around midnight (0230 of 18 /08/21) after the fourth episode of purging and getting up from the commode, got rigors and collapsed head hitting the commode. Following the fall, I was unable to stand up but managed to crawl and reach the bed and went into syncope without even realizing the bleeding injury and lost consciousness till 0700 hrs.
It is only in the morning I noticed that entire pillow, bedsheet, and my shirt was drenched with blood. Touching the head, I noticed a cut, and clotted blood with little active oozing. I managed to clean the wound with warmwater and put up a tight bandage with a handkerchief on my head approximating the cut ends of the lacerated wound. Reached a private surgery around 0900hrs.
c) Physical examination
i. A lacerated half-moon shaped wound on the left occipital region.
ii. GCS score was 15.
iii. BP- 110/60 mm Hg
iv. SPO2- 92%
v. Pulse rate -75/minute
d) Results of pathological tests and other investigations
CT scan revealed:
a) small vessel ischaemic changes in bilateral periventricular regions
b) No evidence of intra/extra-cerebral Haematoma
c) No evidence of Fracture
Hemogram:
CT/BT & Hemogram- Normal
Hb-10G%.
Treatment plan followed
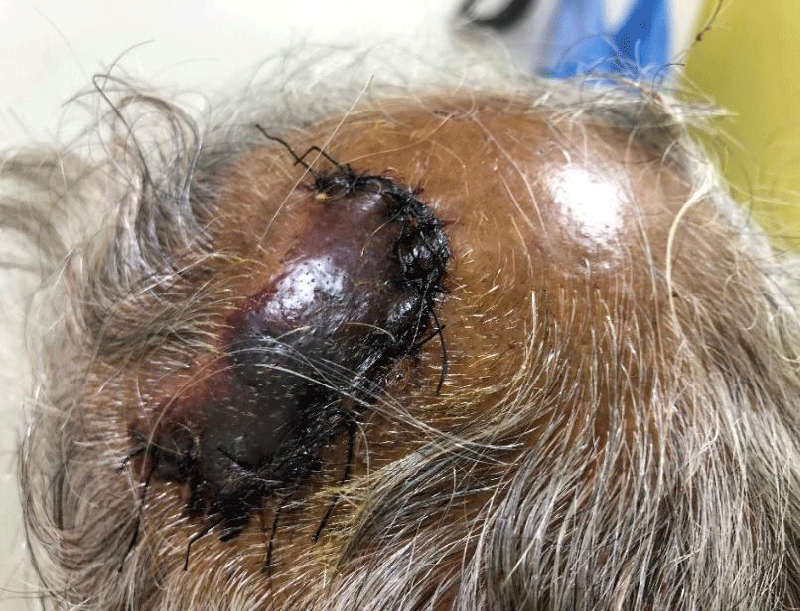
The wound was stitched (8 stiches), put on IV anti-biotics and kept for observation for 12 hours and discharged late in the evening. I was shifted by road to Bengaluru for further treatment, where in a private hospital wound dressings were done on every third day for 3 times and stiches removed on 10th day (Figure 1).
i. Inj. Hitan 40 mg IV BD on 18/8/21
ii. Carrom 1.5 G Inj. IV BD on 18/8/21
iii. Chymoral Plus Tablets 1 BD xc5 days
iv. KLOKMOX CL 625 mg BD x 8days
f) Actual outcome of the treatment plan
The wound has healed but a portion is covered with scab, that may take some more time peel off giving room for new skin. There are no neurological /psychological manifestations of head injury. I Started taking my routine morning walk on 5th day after injury increasing from 1 km to 4 km by end of second week. Also started Gym exercises including weight up to 10 Kg by end of third week Figures 2-4.
g) Expected outcome
Fortunately, none of the Immediate Symptoms of inability to remember the cause of the injury or events that occurred immediately before or up to gaining consciousness, confusion, and disorientation., headache. Dizziness, blurred vision, nausea or vomiting and ringing in the ears did not exhibit in my case.
Discussion
With the rise in life expectancy the population of elderly people is increasing, it has been noted that trivial injuries in this group are also contributing mortality and morbidity in developing countries including India. Head trauma is one of the common injuries in the old due to trivial falls, and its consequences can be innocuous and rarely grievous. The fall in washroom is common among ageing people across the world. Due to frequent getting up in the night the chances of fall, especially in the dark has increased. Many of these people are on medication for hypertension, diabetes, and heart ailments. Due to sudden rising from the bed, or even from the commode or Indian style of squatting plate some develop giddiness and fall. The giddiness may be due to other illnesses like gastroenteritis or food poisoning as it happened in my case being reported.
In a 3-year retrospective analysis of 73 consecutive patients age ≥65 years admitted to a university hospital with TBI, the Glasgow Outcome Scale (GOS) was used to assess outcome. The study indicated that injured persons were predominately male (82%). The mean patient age was 72.1 years (range, 65-97 years), and 20 were age ≥75 years. Head injuries were mild in 37 patients, moderate in 18, and severe in 18. Most injuries were contusions. Fifty-five patients (75%) were managed conservatively, and 18 (25%) underwent surgery. The conservative management of mild and moderate cases was associated with good outcome [7-10]. However, a univariate analysis showed that among aged ≥75 years, severe HI, acute SDH, and surgical management were significantly associated with poor outcome.
Another recent study published online of 154 mild TBI cases attending Emergency Department, 115 (74.7%) were males and 39 (25.3%) were females, with average age of 27 years. Of the patients with mild TBI, road traffic accidents (RTA) were the main cause (50.6%), followed by fall from height (42.9%), assault and sports-related injury (6.4%). Of the total, 96.1% underwent CT. Of these, 31.8% found abnormal CT results, 27.5% received wound treatment care, and 9.1% received emergency care. 75.3% patients were discharged [11].
An Indian autobiographical study [12] concluded that innovative and multi-pronged rehabilitation strategies involving everyday activities provide an answer as treatment challenges in such cases are increased due to patient’s actual deficits caused by neuronal/biochemical changes.
A Prospective study of consecutive trauma admissions to a level 1 trauma hospital of 90 patients with mTBI and 85 non-brain injured trauma controls using a PCS checklist, and neuropsychological and psychological measures. Multiple imputation of missing data in multivariable logistic regression and bivariate logistic regressions were used to predict acute PCS at a mean of 4.90 days after injury. The results indicated that the diagnosis of acute PCS was not specific to mTBI (mTBI 43.3%; controls 43.5%). Pain was associated with acute PCS in mTBI. The strongest effect for acute PCS was a previous affective or anxiety disorder (OR 5.76, 95% CI 2.19 to 15.0). Females were 3.33 times more likely than males to have acute PCS (95% CI 1.20 to 9.21). The effect of acute post-traumatic stress and neuropsychological function on acute PCS was relatively small. Higher IQ was associated with acute PCS [3].
An extensive systematic review in 2020 of Neuroimaging and Psychometric Assessment of Mild Cognitive Impairment After Mild Traumatic Brain Injury (mTBI) has concluded that common mTBI symptoms can be either somatic complaints like headaches, vertigo, sleep problems, nausea, light or sound sensitivity and affective symptoms like clinical depression, anxiety, irritability, and emotional instability [2].
The processing speed phenomenon is strongly associated with self-reported fatigue, as it happened in my case, that I attributed to blood loss (Johansson, et al. 2009; Ponsford, et al. 2013). Social cognition impairment has been reported up to ∼4 years post-mTBI. Impaired cognition is typically correlated with poor outcome, even when such impairment is subtle at all adult ages [2].
Individuals with a history of mTBI are at relatively high risk for post-concussive depressive symptoms (PCDSs), for anxiety and for irritability marked by lack of patience, aggression, and emotional instability. Emerging evidence suggests that disturbance of serotonin production in the gastrointestinal tract after TBI may be related to such symptoms. Some patients with a history of mTBI have been found to exaggerate their reports of injury severity. Impaired processing speed is perhaps the most frequently reported cognitive deficit after mTBI. The research evidence is mixed for increased anxiety, social and emotional cognition, self-awareness, complex attention, and sustained attention. Similarly, though overall Learning &Memory deficits have been recorded, increased challenges in Recognition Memory, Semantic and Episodic Memory, executive functions like planning, planning, decision-making, working memory, feedback response, inhibition, and flexibility either in acute stage or up to a year after TBI have mixed reports (Draper and Ponsford 2008; Konrad, et al. 2011; Rabinowitz and Levin 2014; McInnes, et al. 2017). Neuroimaging for example, a computed tomography (CT) lesion study found that frontal subdural lesions in mTBI are significantly associated with chronic PCDSs (Rao, et al. 2010). The current evidence does support the hypothesis that mTBI is not associated with a true dysfunction of memory storage & implicit learning (Autobiographical and episodic memory deficits in mild traumatic brain injury, Jeffrey D. Wammes et.al https://www.sciencedirect.com/science/article/abs/pii/S0278262616303384) Another study (Rohling et al., 2011) of only patients with uncomplicated mTBI; concluded that post-concussive cognitive deficits dissipate within 3 months [2].
This review summarizes recent literature on mTBI cognitive dysfunction, on its neuroimaging correlates, and on its relation to neuropsychological assessment. Neuroimaging studies indicates that, despite substantial research on the relationship between brain structure, brain function and cognition, certain cognitive subdomains have not been adequately studied, including planning, decision-making, inhibition response, visual perception, and receptive language [2].
This review quotes a few limitations, most important being lack of distinctions between (A) complicated and uncomplicated mTBI, between (B) neuroimaging-free vs. CT- and MRI-informed conclusions and between (C) single vs. multiple injuries being not explored due to the scarcity of psychometric studies which account for these distinctions [2].
Summary of the existing literature on the topic
According to the World Health Organization, traumatic brain injury will be the major cause of death and disability by the year 2020 with an estimated 10 million people getting affected annually by TBI [1]. If not attended elderly TBI patients will be increasing the burden on the society with the worldwide aging population. Increasing age is directly associated with odds of being admitted to the hospital after head injury and subsequent consequences. Seniors over the age of 60 years with head injury are generally considered to have a poor outcome. They will need long hospital stay for care and much more for inpatient rehabilitation or even end in death [5]. Elderly TBI patients also bear higher cost during hospital stay in cost-analysis models [9]. A Case Report reported that the main cause of TBI in elderly was fall, followed by motor vehicle accidents. Though elderly people in general did fare worse after traumatic brain injury, there are reports of 65–75 years aged, had as good outcomes as younger adults after minor to moderate head injury as was in my case [9]. The relationship with use of β-blockers as in my case the outcome in TBI patients is complex. β-blockade may result in attenuation of intracerebral post-traumatic catecholamine-induced vasospasm, decreasing potential for local ischemia. Preinjury statin use in elderly TBI patients is also associated with reduced risk of death and greater likelihood of achieving a good recovery at 12 months due to anti-inflammatory and immunomodulatory effects of statins. The fact that I was using Beta blockers and Statin after CABG might have also contributed to good recovery.
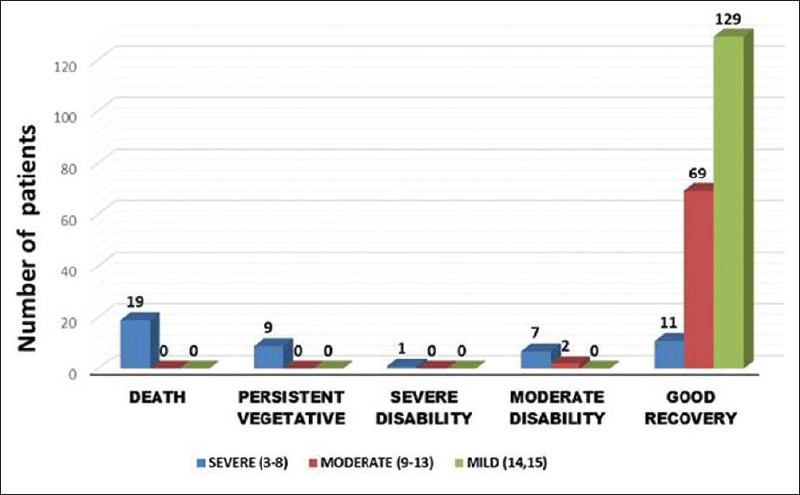
The overall outcome is affected mainly by GCS on admission, followed by age. In a large multicentre epidemiologic study of TBI in China, minor head injury patients (GCS 13–15) had over 90 % survival [10]. Another large-scale study suggested that the outcome of elderly TBI is encouraging, as over 65 years old had a survival rate of over 80 % at a retrospective cohort data at a level II trauma centre in Florida from 2005 to 2008 [13-18]. Increasing number of elderly individuals are surviving moderate to severe TBI over the past two decades as reported by Ramanathan, et al. [14]. Repetitive minor blunt head injuries can cause chronic traumatic encephalopathy at a later stage of life, characterized with memory disturbances, behavioural and personality changes, Parkinsonism, and speech and gait abnormalities [9]. A prospective study demographic profile, clinical features, imaging, and outcomes in patients with traumatic brain injury presenting to emergency room between March 2016 and July 2017 at Sri Venkateshwara Institute of Medical Sciences, Tirupati, Andhra Pradesh, India indicated a 100% recovery among 129 mild TBI cases (GCS 14 &15) [15] Figure 5.
GCS is the standard scoring system used globally to assess the neurological status of patients with traumatic brain injury. The Glasgow Outcome Score (GOS) is used to objectively assess and categorize patients recovering from head injury. In a study of 82 patients with isolated traumatic brain injury GCS was recorded at admission, 6 hours, and 12 hours. GOS was recorded at 7 days and 28 days. Statistical analysis done using Pearson’s Correlation co-efficient proved that there was statistically significant positive correlation between GCS recorded on admission with GOS recorded on day 7 and GOS recorded on day 28. Positive Correlation was also seen between GCS recorded at 6 hours with GOS recorded on day 7 and GOS recorded on day 28. Similar positive correlation was also seen between GCS recorded at 12 hours with GOS recorded on day 7 and GOS recorded on day 28. It now established that GCS can be used as a tool to stratify risk, prognosis, and neurological recovery in patients with traumatic brain injury [18].
Current literature on mTBI cognitive dysfunction, on its neuroimaging correlates, and on its relation to neuropsychological assessment indicates that, despite substantial research on the relationship between brain structure, brain function and cognition, certain cognitive subdomains have not been adequately studied, including planning, decision-making, inhibition response, visual perception, and receptive language [2].
Conclusion
My own case was one of mild TBI (GCS-15) with a fall due to collapsing after bouts of diarrhoea, head hitting the lid of the commode and its sharp edge causing a 4 inches moon shaped lacerated wound. Being in a small town the wound was approximated with unabsorbable sutures. The CT scan did not show any internal damages. Subsequent management in the state headquarter also did not involve any aggressive treatment and at the end of 3 months, I am fine and fit. The only immediate symptom observed feeling fatigue after starting my routine morning walk, which I attributed to blood loss and resulting anaemia, but it could also be due to processing phenomenon. The timely care and early initiation of aerobic exercise (waking & tread meal) would have helped early recovery from concussion injury with no significant post-concussive symptoms [19].
i. Elderly TBI was and will be an important burden to the society with increasing longer life expectancy and an aging population.
ii. Though the incidence of head injuries is rising all over the world, the good news is that fortunately more than half of them is either mild or moderate amenable to management with good outcomes.
iii. Available data in India suggest that fall in homes specially washrooms in the night are the commonest cause.
iv. The outcome of mild TBI cases among elderly in India and abroad is improving as more and more of the elderly individuals are surviving over the past two decades.
v. Increasing use of antiplatelet and anticoagulants is going to complicate the condition.
vi. Glasgow Coma Scale (GCS) is a well-accepted tool to assess the seriousness at the first visit, monitor the prognosis, and recovery of brain functions in patients with traumatic brain injury and is compatible with Glasgow outcome scores.
vii. Dedicated studies in our age group patients in India especially among mild TBIs are lacking.
viii. Available evidence lacks distinctions between complicated and uncomplicated mTBI
ix. Despite substantial research on the relationship between brain structure, brain function and cognition, certain cognitive subdomains have not been adequately studied
- Gururaj G (2002) Epidemiology of traumatic brain injuries: Indian scenario. Neurol Res 24: 24-28. Link: https://bit.ly/3HryB4a
- Calvillo M, Irimia A (2020) Neuroimaging and Psychometric Assessment of Mild Cognitive Impairment After Traumatic Brain Injury. Front Psychol 11: 1423. Link: https://bit.ly/30s975i
- Meares S, Shores EA, Taylor AJ, Batchelor J, Bryant RA, et al. (2008) Mild traumatic brain injury does not predict acute post-concussion syndrome. J Neurol Neurosurg Psychiatry 79: 300-306. Link: https://bit.ly/3oymOIz
- Gururaj G, Kolluri SVR, Chandramouli BA, Subbakrishna DK, Kraus JF (2005) Traumatic Brain Injury. Link: https://bit.ly/30lTr3F
- Annual Report 2019-20, NIMHANS Bengaluru. Link: https://bit.ly/3cgtipL
- Toyin S (2021) Traumatic Brain Injury (TBI) - Definition, Epidemiology, Pathophysiology.
- Dawodu ST, Kishner S (2021) Traumatic Brain Injury (TBI) - Definition, Epidemiology, Pathophysiology. Link: https://bit.ly/3FbVAOu
- Borkar SA, Sinha S, Agrawal D, Satyarthee GD, Gupta D, et al. (2011) Severe head injury in the elderly: risk factor assessment and outcome analysis in a series of 100 consecutive patients at a Level 1 trauma centre. Indian Journal of Neurotrauma 08: 77-82. Link: https://bit.ly/3DiiJOX
- Advanced Trauma Life Support (1993) Course for Physicians, American College of Surgeons.
- Prasad GL, Anmol N, Menon GR (2018) Outcome of Traumatic Brain Injury in the Elderly Population: A Tertiary Center Experience in a Developing Country. World Neurosurg 111: e228-e234. Link: https://bit.ly/3x0JLbj
- Ajay Choudhary, Ashok Kumar, Rajesh Kumar Sharma, Rahul Varshney, Satya Shiva Munja, et al. (2021) Emergency Department Management of Mild Traumatic Brain Injury in New Delhi. A Single Institute Cohort Management Data. Indian Journal of Neurosurgery. Link: https://bit.ly/3CfHEBd
- Banerjee M, Hegde S, Thippeswamy H, Kulkarni GB, Rao N (2021) Holistic rehabilitation in restoring cognition and recovering the 'self' following traumatic brain injury: A case report. Neurorehabilitation 48: 231-242. Link: https://bit.ly/3FlZdlb
- Mak CHK, Wong SKH, Wong GK, Ng S, Wang KKW, et al. (2012) Traumatic Brain Injury in the Elderly: Is it as Bad as we Think? Current Translational Geriatrics and Experimental Gerontology Reports 1: 171-178. Link: https://bit.ly/3neponC
- Jennett B, Teasdale G, Braakman R, Minderhoud J, Knill-Jones R, et al. (1976) Predicting outcome in individual patients after severe head-injury. Lancet 1: 1031-1034. Link: https://bit.ly/3os0FeV
- Kirankumar MR, Satri V, Satyanarayana V, Ramesh Chandra VV, Madhusudan M, et al. (2019) Demographic profile, clinical features, imaging, and outcomes in patients with traumatic brain injury presenting to emergency room. Link: https://bit.ly/3DhMak3
- Bhullar IS, Roberts EE, Brown L, Lipei H (2010) The effect of age on blunt traumatic brain-injured patients. Am Surg 76: 966–968. Link: https://bit.ly/3ceJYxK
- Ramanathan DM, McWilliams N, Schatz P, Hillary FG (2012) Epidemiological shifts in elderly traumatic brain injury: 18-year trends in Pennsylvania. J Neurotrauma 29: 1371-1378. Link: https://bit.ly/3wNdjsu
- Kodliwadmath HB, Koppad SN, Desai M, Badiger SP (2016) Correlation of Glasgow outcome score to Glasgow coma score assessed at admission. 3: 451-453. Link: https://bit.ly/30iCoiZ
- Leddy JJ, Master CL, Mannix R, Wiebe DJ, Grady MF, et al. (2021) Early targeted heart rate aerobic exercise versus placebo stretching for sport-related concussion in adolescents: a randomised controlled trial. Lancet Child & Adolescent Health 5: 792-799. Link: https://bit.ly/30u5eNC
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.




 Save to Mendeley
Save to Mendeley
