Journal of HIV for Clinical and Scientific Research
Prevalence and pattern of psychological disorders among key populations living with HIV/AIDS: findings from ECEWS supported global fund IMPACT project OSS centers in Southern Nigeria
Okezie Onyedinachi*, Raphael Aguanunu, Grace Jimbo, Esther Essien, Andy Eyo, Rebecca Badejo, Ngozi Okeke, George Odutuga and Olufemi Oke
Cite this as
Onyedinachi O, Aguanunu R, Jimbo G, Essien E, Eyo A, et al. (2022) Prevalence and pattern of psychological disorders among key populations living with HIV/AIDS: findings from ECEWS supported global fund IMPACT project OSS centers in Southern Nigeria. J HIV Clin Sci Res 9(1): 010-014. DOI: 10.17352/2455-3786.000034Copyright
© 2022 Onyedinachi O, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Introduction
Background
Nigeria ranks third among countries with the highest burden of Human Immuno-Deficiency Virus (HIV) infection in the world. The 2019 Nigeria National HIV/AIDS Indicator and Impact Survey showed that 1.9 million people were living with HIV and AIDS in Nigeria as of 2018 [1]. People Living with HIV/AIDS (PLHIV) are faced with daily interpersonal, social, physical, and psychological challenges as a result of their HIV status which also increases their vulnerabilities to various health conditions [2]. These conditions are worse for the key populations living with HIV because their activities are often criminalized in most parts of the world. As a result, they face intersecting socio-economic and structural inequalities that may increase their risk of mental health problems across their life course [3]. This includes but is not limited to psychosocial conditions such as discrimination, stigmatization, low self-esteem, and low self-efficacy that usually predispose them to mental health challenges.
Key populations are defined groups who, due to specific higher-risk behavior, are at increased risk of HIV infection irrespective of the epidemic type or local context [4]. They include men who have sex with men (MSM), Female Sex Workers (FSW), People Who Inject Drugs (PWID), transgender people and people in prisons. Aside from being vulnerable to HIV, members of the key populations face discrimination, stigmatization, and legal issues which are some of the stressors that are likely to predispose them to psychological disorders [4]. Such psychological issues are likely to be compounded among the key populations infected with HIV/AIDS in such a way that some of them may be deterred from adhering to their Anti-Retroviral Therapy (ART), thereby not achieving viral suppression.
By definition, psychological disorders are conditions characterized by abnormal thoughts, feelings, and behaviors [5]. Such disorders are also characterized by distress and impairment in personal functioning. They include but are not limited to depression, anxiety, psychosis and bipolar disorders [5]. Among the key populations on ART, adherence may be poor due to some psychological disorders [6]. For instance, members of the key populations who have substance use disorder may be finding it difficult to achieve viral load suppression faster than those without the disorder due to interference of substances on their ART adherence and efficacy. In addition, depression could deter a client living with HIV from medication compliance [7]. Based on this, there is a need to widen the horizon of our understanding by empirically establishing the prevalence of psychological disorders among members of the key populations living with HIV/AIDS. This will help the agencies and professionals involved in HIV prevention and treatment to see the need for the incorporation of mental health care while providing services to the members of the key populations living with HIV/AIDS to achieve the UNAIDS 95:95:95 goal among the key populations and by extension in the general population. The 95:95:95 goal implies that 95% of all people living with HIV know their HIV status; 95% of all people with diagnosed HIV infection receive sustained antiretroviral therapy; and 95% of all people receiving antiretroviral therapy have sustained viral suppression.
Statement of the problems
Globally, the key populations contributed a significant proportion of new HIV infections daily [8]. This indicates the importance of working with Key Populations (KP) sex workers, gay men and other men who have sex with men, transgender people, people who inject drugs, and people in prisons and other enclosed settings [8]. These Key populations are particularly vulnerable and disproportionately affected by HIV due to risk behaviors, marginalization, and social factors such as stigma, discrimination, violence, human rights violations, and criminalization, all of which contribute to a lack of access to health services. In 2020, key populations and their sexual partners accounted for 65% of new HIV infections worldwide and 39% of infections in sub-Saharan Africa (UNAIDS, 2021c). The high incidence and prevalence of HIV among key populations are well documented in the literature such as the study which shows that the key populations account for the majority of new infections in West and Central Africa, and an estimated 25% of new infections in East and Southern Africa, despite representing relatively small proportions of those populations [9,10]. Available data shows that HIV prevalence varied from 15.9% in The Gambia to 68% in Benin among female sex workers, whereas it ranged from 9.8% in The Gambia to 34.9% in Nigeria for MSM [11,12].
In Nigeria, the prevalence of HIV among FSWs was found to be 21.0% among brothel Based FSWs [13]. Likewise, even though Men who have sex with men (MSM) are conservatively estimated to be less than 1% of the Nigerian population, nationally account for about 20% of new HIV infections [9]. Also, the prevalence of HIV among people who inject drugs (PWIDs) is 9% in Nigeria [14].
According to the Nigeria Country Operational Plan 2020, Key populations and their partners, account for 32% of new HIV infections in Nigeria [15]. Key populations have higher vulnerability to HIV infection than the general population [16]. The prevalence of HIV among key populations and the challenging environment in which they operate often create psychological issues for the members of key populations which call for more integrated and holistic care for the members of the key populations.
Justification
Members of the key populations are major drivers of HIV/AIDS in sub-Saharan Africa, thus those involved in the prevention and treatment need to understand the context of key populations’ programming and the various pattern of the psychological disorders that affect them if we are to stem the tide of the transmission of HIV through this group of people. The understanding of the psychological disorders that affect members of the key populations is key to the quality of service provision for the key populations living with HIV/AIDS. In addition to that, most of the studies on key populations are foreign-based and as such may not be relied on or employed in policy-making or decision-making in Nigeria due to cross-cultural variations. To narrow this knowledge gap, this study is aimed at establishing the prevalence of psychological disorders among members of the key populations using data from four one-stop shops being manned by Excellence Community Education Welfare Scheme (ECEWS) as a sub-recipient to FHI360 under the Global Fund Optimizing HIV Investment for Impact Project. Such will help HIV service providers and donors to better understand and appreciate the relevance of psychological services among members of the key populations living with HIV/AIDS.
Objectives of the study
To determine the prevalence rate of psychological disorders among the various sub-types of Key Population members living with HIV.
Specifically, the study will determine the sub-type of key population members living with HIV with the highest prevalence of the psychological disorder. It will also determine the psychological disorder that is most prevalent among members of the key populations living with HIV.
Methodology
Study location
This study was conducted across the four One-Stop-Shops (OSS) located in Abia, Edo, Enugu and Imo State which are centers being manned by Excellence Community Education Welfare Scheme (ECEWS) as a sub-recipient to FHI360 under the Global Fund Optimizing HIV Investment for Impact Project.
Study population
The study population was among the three sub-types of Key population (Men who have Sex with Men [MSM]; Female Sex Workers [FSW]; People Who Inject Drug [PWID] whose age ranges from 17 to 58 years.
Inclusion criteria
I. All FSW, MSM, and PWID living with HIV who was enrolled in Enugu, Edo, Abia, and Imo States OSS.
II. All FSW, MSM, and PWID living with HIV enrolled in Enugu, Edo, Abia, and Imo States and have received psychological services from the OSS centers.
Exclusion criteria
I. All FSW, MSM, and PWID who are HIV negative
II. All FSW, MSM, and PWID were newly diagnosed with HIV and have not received any psychological support from the OSS.
Sampling technique
Purposive sampling was used in this study. It has to do with the selection of participants with the characteristics required to achieve the research objectives.
Data collection
A total of 1,095 members of the key populations (455 MSM, 571 FSW, 69 PWIDs) who were confirmed to be HIV positive on their visit to the OSS centers were selected and assessed for psychological disorders based on the Diagnostic and Statistical Manual (DSM-5) of mental disorders. The members of the key populations who were diagnosed with HIV infections at the OSS were assessed using different mental health screening tools, (intake form, Depression scale, Anxiety scale- Suicidal scale) after obtaining their consent. The face and content validity of the scales were evaluated and approved by four Psychologists who are versed in areas of psychometric properties and the ECEWS technical team. After that, the instruments were employed for psychological evaluation of the members of the Key Populations living with HIV. Their diagnoses of psychological disorders were based on the Diagnostic and Statistical Manual (DSM-5) of mental disorders. The data collection was done over nine months (January to September 2020). In all, valid data collected from 1,095 members of the key populations who were purposively selected for the study based on the inclusion criteria were utilized.
Data analysis
The data were analyzed using the statistical package for social sciences version 24, using descriptive statistics.
Ethical approval and informed consent: Ethical approval was obtained from the Ethic and Research Unit of the respective State Ministry of Health Ethical review board in the Research and Planning Unit. Informed consent was obtained from each participant. Other ethical issues considered were confidentiality and the study was devoid of any risk of dehumanization as the data collection procedure was done in such a manner that the process was devoid of physical and emotional harm. The study was fully explained and understood by the participants. Also, the participants could choose not to participate in the study at any time.
Results
The Table 1 indicated that thousand, ninety-five (1,095) members of the different KPs sub-types were assessed by the Psychologists across the four OSS centers (Abia, Edo, Enugu, and Imo State). Out of the 1,095 clients, 455 were MSM, 571 were FSW and 69 PWIDs (M -58; F-11) were different sub-types of KPs which account for 42% of the participants being MSM, 52% being FSW and 6% being PWID.
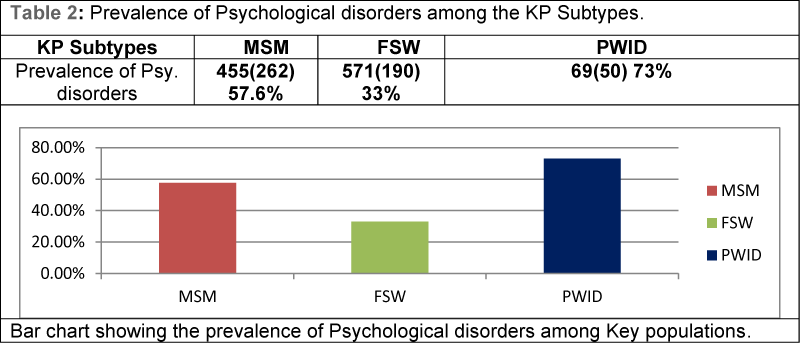
As indicated in Table 2, the prevalence of psychological disorders among the MSM is 262 out of 455 MSM assessed, accounting for a prevalence of 57.6%. Likewise, the prevalence of Psychological disorders among FSWs is 190 out of the 571 FSWs assessed accounting for a prevalence of 33%. Also, the prevalence of psychological disorders among PWID is 50 out of the 69 PWID assessed accounting for 73%. The study shows PWID has the highest prevalence of psychological disorders among all the KP subtypes followed by MSM and FSW has the least prevalence of psychological disorders among them. In all the prevalence of psychological disorders among the KP is 45.9% Figure 1.
Table 3 shows that 502 (262 MSM, 190 FSW, and 50 PWIDs) members of the KP were diagnosed with different psychological disorders using various screening tools. The prevalence of depression among the KPs was found to be 1095(183) 16.7%, Substance Use Disorder was 1095(145) 13.2% while Anxiety disorder has a prevalence of 1095(135) 12.3%. Likewise, Suicide Ideation 1095(23)2.1%, Sleep Disorders 1095(9) 0.8%, Psychosis 1095(6)0.6% and PTSD 1095(2)0.2%. Among the psychological disorders found, depression (16.7%) was the most prevalent psychological disorder among the KPs followed by substance use disorder (13.18%), anxiety (12.3%), suicidal ideation (2.1%), sleep disorder (0.8%), Psychosis (0.6%) and lastly by Posttraumatic stress disorder (0.2). Among the KPs, depression was highest among MSM (20.66%) followed by PWIDs (17.39%) and lastly by FSW (13.31%). Under substance use disorder, PWIDs (44.93%) was the highest followed by MSM (14.73%) and lastly by FSW (8.23%). Concerning anxiety disorder, MSM (16.48%) was the highest, followed by the FSW (9.46%) and lastly by PWIDs (8.70%). Under suicidal Ideation, MSM (3.08%) was the highest, followed by PWIDs (1.45%) and lastly by FSW (1.40%). Also, based on sleep disorder, MSM (1.32%) was the highest, followed by FSW (0.53%). No sleep disorder was recorded among the PWIDs. More so, FSW (0.18%) was highest under psychosis, followed by MSM (1.10%). No psychosis was reported among the PWIDs. Based on PTSD, MSM (0.22%) was the highest, followed by FSW (0.18%). No PTSD was reported among the PWIDs.
Discussion
The Findings in this study show that thousand, ninety-five (1,095) members of the different KPs’ sub-types were assessed by the Psychologists across the four OSS centers in Abia, Edo, Enugu, and Imo States. The 1,095 clients were made up of 455 (42%) MSM, 571 (52%) FSW, and 69 (6%) PWIDs. Out of the 1,095 members of the key populations, 502 (45.9%) had psychological disorders. Among MSM, the prevalence of psychological disorders was 57.6%, followed by FSW at 33% and 73% among PWIDs.
Among the psychological disorders found among the key populations living with HIV/AIDS, depression was the most prevalent disorder. This finding was similar to the study conducted by Bing, Burnam, Longshore, Fleishman, Sherbourne and London (2001) which also found depression as the most common neuropsychiatric disorder among people living with HIV/AIDS [17]. Based on the key populations’ typology, depression was more prevalent among the men who have sex with men, followed by people who inject drugs, and lastly by female sex workers. These findings aligned with the findings of the study conducted in Puerto Rico by Alegria, et al. which found high levels of depressive symptoms among people who inject drugs [18].
Aside from depression, substance use disorder was also of high prevalence among the key populations which was recorded highest among the PWIDs, followed by MSM and lastly by FSW. The result is similar to the outcome of the study carried out in Nigeria by Ochonye, et al. in 2019 in which one of their findings indicated that high prevalence of substance use among members of Key populations [16]. The findings in this study were also similar to another study conducted in Nigeria by Ogueji, Ifeanyichukwu, and Maia (2020), in which suicidal ideation is amongst the common early problems of newly diagnosed PLWHA as indicated in the study [19]. In line with the findings, Safren, et al. 2022 show that MSM with HIV infection is more vulnerable to experiencing mental health issues, particularly depression and anxiety, compared to the general population [20]. However, the findings from the study show PWID to have the highest prevalence of psychological disorders, this was however different from the findings of Kamen, et al. 2012 and De Moraes, et al. 2017 which shows that MSM was the group with the highest psychological disorder [21,22]. The findings in this study were also similar to the findings of Roxburgh, Degenhardt, and Copeland in 2006 which show that post-traumatic stress disorder and symptoms of depression, and injection of the drug were common among Female sex workers [23].
Conclusion
The finding in this study indicated that the prevalence of psychological disorders among the tions living with HIV/AIDS is high (45.64%). This underscores the need for quality mental health provision for the members of the key population. The inclusion of psychological services will help to attenuate the possible psychological disorders that could result in an interruption in treatment. People who inject drugs (PWID) KP sub-types have the highest prevalence of psychological disorders among all the KP subtypes living with HIV followed by MSM while FSW has the least prevalence of psychological disorders. Given this, the KP program in Nigeria should focus on the implementation of interventions geared towards supporting the mental health of the KP through a quality mental health program.
- National HIV/AIDS Indicator and Impact Survey. https://www.naiis.ng/resource/factsheet/NAIIS%20PA%20NATIONAL%20FACTSHEET%20FINAL.pdf
- Egbe CJ, Dakum PS, Ekong E, Kohrt BA, Minto JG, Ticao CJ. Depression, suicidality, and alcohol use disorder among people living with HIV/ AIDS in Nigeria. BMC Public Health. 17:542. https://d-nb.info/1136213287/34
- Beksinska A, Jama Z, Kabuti R, Kungu M, Babu H, Nyariki E, Shah P; Maisha Fiti Study Champions, Nyabuto C, Okumu M, Mahero A, Ngurukiri P, Irungu E, Adhiambo W, Muthoga P, Kaul R, Seeley J, Beattie TS, Weiss HA, Kimani J. Prevalence and correlates of common mental health problems and recent suicidal thoughts and behaviours among female sex workers in Nairobi, Kenya. BMC Psychiatry. 2021 Oct 14;21(1):503. doi: 10.1186/s12888-021-03515-5. PMID: 34649544; PMCID: PMC8518166.
- Afe AJ, Onyema M, Adewumi O, Ojoye AO, Iwuoha E. Analysis of HIV Treatment Cascade Among Key Affected Population in Lagos State, Nigeria. European Journal of Medical and Health Sciences. 2019; 1(3):57-69. https://www.ejmed.org/index.php/ejmed/article/view/57
- World Health Organization: Mental Disorders. https://www.who.int/news-room/fact-sheets/detail/mental-disorders
- Adejumo O, Oladeji B, Akpa O, Malee K, Baiyewu O, Ogunniyi A, Evans S, Berzins B, Taiwo B. Psychiatric disorders and adherence to antiretroviral therapy among a population of HIV-infected adults in Nigeria. Int J STD AIDS. 2016 Oct;27(11):938-49. doi: 10.1177/0956462415600582. Epub 2015 Sep 18. PMID: 26384949; PMCID: PMC4798907.
- Remien RH, Stirratt MJ, Nguyen N, Robbins RN, Pala AN, Mellins CA. Mental health and HIV/AIDS: the need for an integrated response. AIDS. 2019 Jul 15;33(9):1411-1420. doi: 10.1097/QAD.0000000000002227. PMID: 30950883; PMCID: PMC6635049.
- Key Population: Achieving Equitable Access to End AIDS. https://www.usaid.gov/global-health/health-areas/hiv-and-aids/technical-areas/key-population
- Eluwa GIE, Adebajo SB, Eluwa T, Ogbanufe O, Ilesanmi O, Nzelu C. Rising HIV prevalence among men who have sex with men in Nigeria: a trend analysis. BMC Public Health. 2019 Sep 2;19(1):1201. doi: 10.1186/s12889-019-7540-4. PMID: 31477073; PMCID: PMC6721282.
- Jin H, Restar A, Beyrer C. Overview of the epidemiological conditions of HIV among key populations in Africa. J Int AIDS Soc. 2021 Jul;24 Suppl 3(Suppl 3):e25716. doi: 10.1002/jia2.25716. PMID: 34190412; PMCID: PMC8242974.
- Djomand G, Quaye S, Sullivan PS. HIV epidemic among key populations in west Africa. Curr Opin HIV AIDS. 2014 Sep;9(5):506-13. doi: 10.1097/COH.0000000000000090. PMID: 25010898; PMCID: PMC4804351.
- UNAIDS: New HIV Infection Increasing Among Key Population: https://www.unaids.org/en/resources/presscentre/featurestories/2020/september/20200928_new-hiv-infections-increasingly-among-key-populations
- Okafor UO, Crutzen R, Ifeanyi O, Adebajo S, Van den Borne H. HIV prevalence and high-risk behaviour of young brothel and non-brothel based female sex workers in Nigeria. BMC Res Notes. 2017 Aug 10;10(1):380. doi: 10.1186/s13104-017-2712-8. PMID: 28797278; PMCID: PMC5553858.
- UNODC: HIV and AIDS. https://www.unodc.org/nigeria/en/hiv-and-aids.html
- Nigeria Country Operational Plan (COP) 2020. https://www.state.gov/wp-content/uploads/2020/07/COP-2020-Nigeria-SDS-Final-.pdf
- Ochonye B, Folayan MO, Fatusi AO, Bello BM, Ajidagba B, Emmanuel G, Umoh P, Yusuf A, Jaiyebo T. Sexual practices, sexual behavior and HIV risk profile of key populations in Nigeria. BMC Public Health. 2019 Sep 2;19(1):1210. doi: 10.1186/s12889-019-7553-z. PMID: 31477063; PMCID: PMC6721228.
- Bing EG, Burnam MA, Longshore D, Fleishman JA, Sherbourne CD, London AS, Turner BJ, Eggan F, Beckman R, Vitiello B, Morton SC, Orlando M, Bozzette SA, Ortiz-Barron L, Shapiro M. Psychiatric disorders and drug use among human immunodeficiency virus-infected adults in the United States. Arch Gen Psychiatry. 2001 Aug;58(8):721-8. doi: 10.1001/archpsyc.58.8.721. PMID: 11483137.
- Alegría M, Vera M, Freeman DH Jr, Robles R, Santos MC, Rivera CL. HIV infection, risk behaviors, and depressive symptoms among Puerto Rican sex workers. Am J Public Health. 1994 Dec;84(12):2000-2. doi: 10.2105/ajph.84.12.2000. PMID: 7998647; PMCID: PMC1615399.
- Ogueji A1, Okoloba MM. Compassion-Focused Therapy (Cft) As An Intervention Against Suicidal Ideation In Newly Diagnosed People Living With Hiv/Aids (Plwha) Attending A Nigerian Maternity Teaching Hospital. Global Psychiatry. 3 (1): 104-112.
- Safren SA, Blashill AJ, O’Cleirigh CM. Promoting the sexual health of MSM in the context of comorbid mental health problems. Aids Behav. 2011. doi: 10.1007/s10461-011-9898-x.
- Kamen C, Flores S, Taniguchi S, Khaylis A, Lee S, Koopman C, Gore-Felton C. Sexual minority status and trauma symptom severity in men living with HIV/AIDS. J Behav Med. 2012 Feb;35(1):38-46. doi: 10.1007/s10865-011-9329-5. Epub 2011 Feb 23. PMID: 21344319.
- Moraes RP, Casseb J. Depression and adherence to antiretroviral treatment in HIV-positive men in São Paulo, the largest city in South America: Social and psychological implications. Clinics (Sao Paulo). 2017 Dec;72(12):743-749. doi: 10.6061/clinics/2017(12)05. PMID: 29319720; PMCID: PMC5738567.
- Roxburgh A, Degenhardt L, Copeland J. Posttraumatic stress disorder among female street-based sex workers in the greater Sydney area, Australia. BMC Psychiatry. 2006 May 24;6:24. doi: 10.1186/1471-244X-6-24. PMID: 16719928; PMCID: PMC1481550.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.



 Save to Mendeley
Save to Mendeley
