Journal of Dental Problems and Solutions
External root resorption of a permanent tooth. Case study
Jacel Kotuła1*, Anna Kuc2, Jakub Nawrocki2, Alicja Babczyńska1, Michał Sarul1 and Joanna Lis1
2Dental Star Specialist Aesthetic Dentistry Center, 15-215 Białystok. M. Konopnickiej 1c lok U3, Poland
Cite this as
Kotuła J, Kuc A, Nawrocki J, Babczyńska A, Sarul M, et al. (2022) External root resorption of a permanent tooth. Case study. J Dent Probl Solut 9(2): 020-024. DOI: 10.17352/2394-8418.000112Copyright License
© 2022 Kotuła J, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Introduction: External resorptions often occur as a lesion of inflammatory origin. The origin of the process begins on the side of the root cementum and goes towards the pulp of the tooth. The changes consist of the pathological loss of root cement, dentin, and bone surrounding the tooth. The dynamics of the process are enhanced by inflammatory or necrotic pulp changes.
Aims: This study aimed to present contemporary views on the resorption of external tooth roots and the possibility of their treatment.
Material and methods: The technique of observation and clinical and radiological diagnostics were used by the case-by-case method
Result: Endodontic treatment was undertaken, consisting of chemo-mechanical preparation of the canal system and simultaneous obturation of the gutta percha canals with the AH + sealant and the BL thermal system.
Conclusions: The applied treatment inhibited the progression of the resorption and led to the healing of periapical periodontitis.
External root resorption of a permanent tooth is a pathological process that, in the absence of endodontic treatment, inevitably leads to tooth loss [1,2]. There are external surface resorption and replacement resorption [1-3]. Cement-originated external inflammatory resorption may also involve dentin, which leads to shortening or even complete destruction of the root [3]. It is most often a complication of tooth caries, caused by inflammatory factors, an infection caused by irreversible pulpitis, local blood flow disorders [1,3], vitamin A and D deficiencies, hormonal disorders, genetic factors, pressure or trauma [1-4], orthodontic treatment [5], pressure from impacted teeth, cysts, tumors, trauma-related chronic inflammation of the periapical tissues of the teeth [4,6-10]. In 2003. The classification due to the pathomechanism of change was proposed by Z. Fuchs [8]. The author distinguishes 5 groups of changes [8,11]. These include resorptions related to:
- pulp inflammation,
- periodontitis,
- pressure caused by orthodontic treatment,
- pressure caused by impacted teeth and tumors
- ankylotic resorptions.
The etiology of different types of root resorption requires two phases: mechanical or chemical injury to the protective tissues and stimulation by infection or pressure. Injury can be similar in various types of root resorption. The selection of proper treatment is related to the stimulation factors. Intrapulpal infection is the stimulation factor in internal root resorption and external periradicular inflammatory root resorption. Adequate root canal treatment controls intrapulpal bacteria and arrests the resorption process [11].
Inflammatory resorption is a response to the presence of infected pulp contacting with damaged periodontium and root cementum [8,9]. It is characterized by a loss of tooth tissue: dentin, root cementum [9] and the surrounding alveolar bone. External resorption [9,12,13] begins in the tissue of the root cement and proceeds towards the tooth pulp. The cause of resorption is the loss of the protective layer of cementoblasts and the remains of Mallassez epithelial islands [3]. Damage to the protective layer makes it easier for macrophages and osteoclasts to remove damaged ones and periodontal fibers and root cement on its surface [1,12]. During the process, the periodontium is transformed into richly vascularized granulation tissue with increased activity of cementoblasts. Their activity is indicated on the tooth root wall, leading to a wide connection of the periapical tissues with the tooth pulp. Injuries [3,5,8,9,14-16] and other irritants mobilize osteoclast-initiating factors. Activating factors include: osteoclast activating factor, macrophage chemotactic factor (MCF), prostaglandins, heparin, and bacterial products [3,9,10,12,13,16,17]. The external resorption process is usually asymptomatic. In superficial changes, resorptive lacunae are formed through the active metabolism of macrophages and osteoclasts. Inflammatory changes are rapid and often lead to the destruction of the entire root in a short period of time. In this type of lesion, microorganisms and their toxins migrate through the dentinal tubules to the outer surface of the cement, leading to the atrophy of the periodontium and surrounding bone, which accelerates the resorption of the tooth root [3,14,18]. Ankylotic resorptions initially lead to the formation of resorptive lacunae. They are eventually filled with new bone tissue with the participation of bone marrow cells and productive healing of root cement and Sharpey fibers from the periodontium [3].
The classification of external resorption [19] proposed by Lewander and Malmgren [18,19] includes 5 degrees of decay:
- Absence of root resorption
- Blur the outline of the root
- Root length shortened to 2 mm.
- Resorption over a distance longer than 2 mm, but not exceeding 1/3 of the root length
- Resorption of more than 1/3 of the root length.
Detection of the resorption occurs accidentally on the basis of radiographic diagnostic images [4]. As a chronic process, resorption does not produce pain symptoms. They appear only in connection with the exacerbation of the chronic process and extrinsic superinfection caused by the migration of microorganisms to the area of the root apex of the resorbed tooth from the area of the gingival pocket or through the bloodstream. Resorptive changes may concern single-rooted and multi-rooted teeth. In multi-rooted teeth, the changes may concern a single root, and less frequently both roots simultaneously. With single-root external resorption, the pulp of the tooth is often in a state of necrosis or irreversible inflammation. Therefore, the tooth may react to thermal stimuli and could not react to percussion.
Among the numerous types of root resorption, there is also idiopathic resorption. The prognosis of preserving the dentition is for the most part unfavorable. No standard treatment protocol is available for this condition. A dental treatment plan should be flexible and individually adjusted to the patient's wishes [20].
Treatment of resorption makes high therapeutic demands. Both the chemo-mechanical preparation and the tight filling of the canal system are significantly difficult due to the resorbed surface of the root tip and the missing root cement [19]. The prognosis for significantly advanced root resorptions is uncertain [19]. Resorption most often stops after the removal of infected or necrotic pulp tissue [3,20,21]. The best treatment is endodontic root canal preparation combined with apical closure as the protection against the recurrence of infection and resorption [3]. The therapeutic activities consist of the chemomechanical preparation of the root canal system. Two alternative procedures can be used. The first need is temporarily to fill the root canals with calcium hydroxide-based material for a period of at least 1-2 weeks. Then, tightly fill the root canals up to the border of the resorption with the gutta-percha with a sealant based on epoxy resins [3]. It is also possible to omit the temporary filling of the root canals with temporary material, and immediately after the chemo-mechanical preparation of the root canal system, the final filling of the gutta perch with a sealant based on epoxy resins. Then, tightly fill the root canals up to the border of the remaining tooth root with the gutta perch resorption gap with a sealant based on epoxy resins [3]. It is also possible to skip the temporary filling of the root canals, and immediately perform the final filling of the gutta perch with a sealant based on epoxy resins after the chemo-mechanical preparation of the root canal system.
A case report
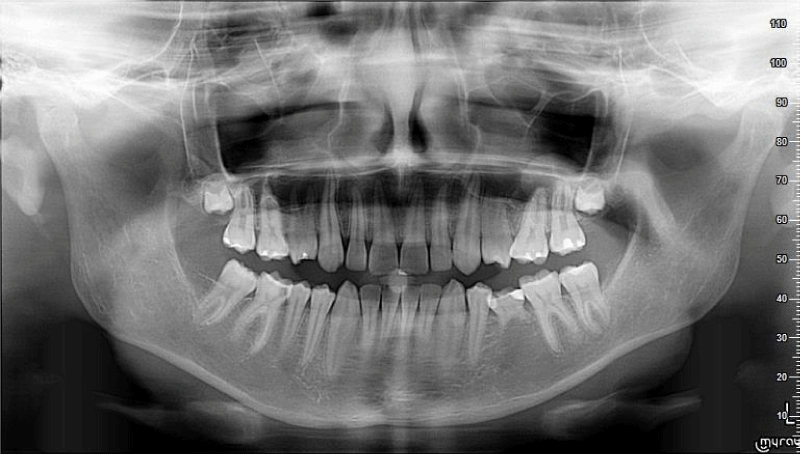
A 17-year-old patient came to the dentist's office for a routine dental examination. The interview showed that the patient did not feel any pain in the area of tooth 46. The clinical examination revealed, i.a. carious defect in tooth 46, confirmed by radiography (Figure 1). Conservative treatment was undertaken at the clinical diagnosis of caries profunda simplex by filling the defect with compound material. After the conservative treatment was completed, the patient did not feel any discomfort from the tooth in question.
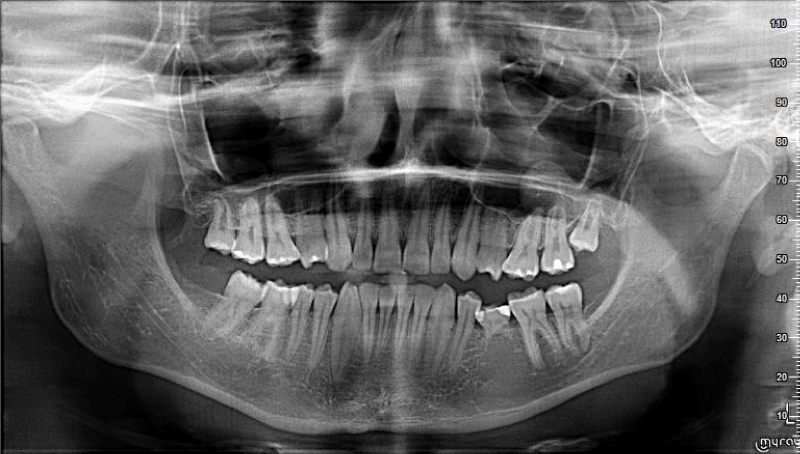
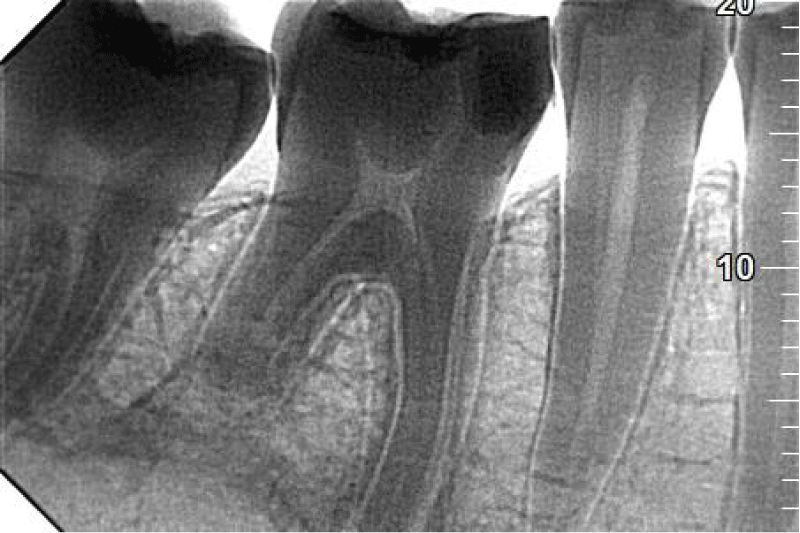
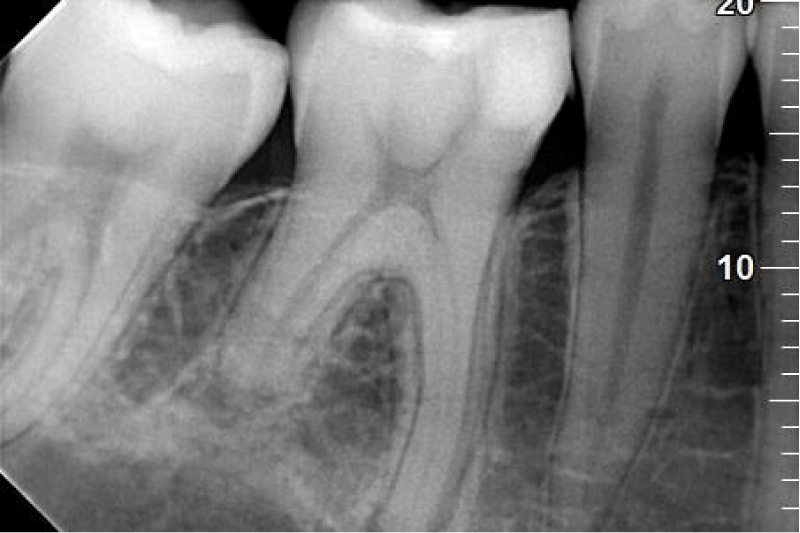
After six months patient complained of the pain that had appeared 2 days earlier. It was a spontaneous pain with long intermissions without increased sensitivity to pressure or biting. After taking the painkiller Ibuprom 200 mg the pain subsided and did not return. On the day of coming to the office, the patient felt no pain. In a clinical examination, filling on the occlusal surface was found. The tooth was insensitive to vertical and horizontal percussion. At the same time, increased sensitivity to thermal stimuli was diagnosed. In the literature, the relative decrease in electric pulp test level could be a diagnostic sign of root resorption [5]. In the auxiliary study, no decrease in the level of pulp excitability to thermal stimuli was found, which could suggest tooth root resorption. It was decided to take a control x-ray image. In the orthopantomographic X-ray analysis, the 2 mm radiolucency in the area of tooth 46 and the disappearance of 1/3 of the apical part of the length of the distal root of that tooth were found. On the other hand, in the crown part of the tooth, a filling was found within the tooth crown (Figure 2). After the panoramic X-ray analysis, a decision was made to take an intraoral image (Figures 3,4).
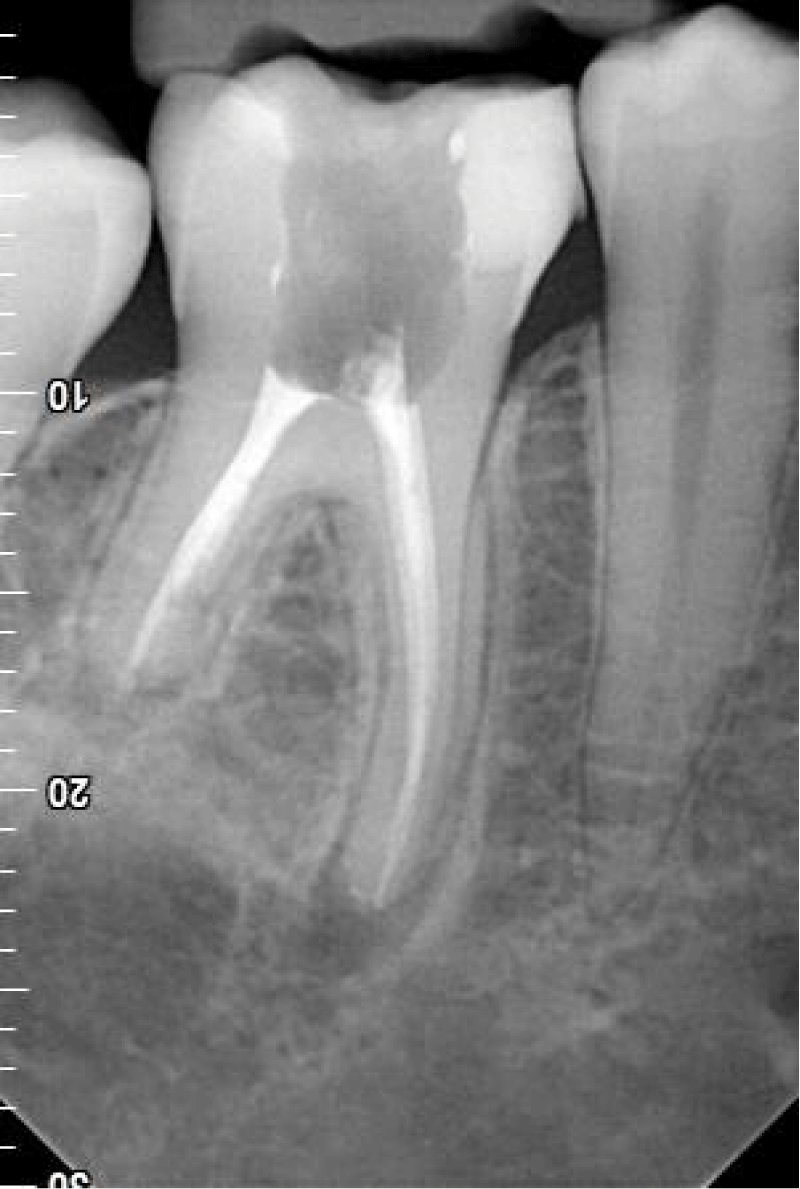
X-ray analysis of tooth 46 revealed external resorption of the root of the distal tooth 46 reaching 1/3 of the apical part of the tooth root and widening the periodontal gap around the apex of the mesial root.
Higher spatial resolutions have improved the radiographic diagnosis of simulated ERR in multi-rooted teeth and this should be considered when performing digital radiographs [22].
Based on the information obtained from the patient about the pain incident for 2 days, inconclusive results of the clinical examination, and the unequivocal result of the radiological examination, a clinical diagnosis was made; periodontitis periapical Chronica exacerbate cum resorption external radicis distalis dentist 46. Endodontic treatment of the tooth has been attempted. After trepanation of the tooth chamber, the presence of bright, vividly bleeding pulp was found both in the area of the crown and the tooth roots. A full protocol for the chemomechanical preparation of the canal system was implemented. A canal system was chemomechanical prepared using method 642 for 02/35 apical enlargement. A 5.2% NaOCl, 3% H2O2, 0.9% NaCl, citric acid, isopropanol rinse was used. The obturation was made with a gutta percha and AH + sealant using the BL system. An x-ray was taken as a control (Figure 5). The canal filling was complete, and completely tight reaching the tops of the mesial root and the height of the distal root resorption position. After X-ray analysis, the final carious cavity was filled with composite material.
Control visit after 4 months. From the interview, the patient did not report any complaints about the treated tooth. No disturbing symptoms were found in the clinical examination: vertical percussion and negative horizontal percussion, no local changes in the projection of the apexes of the tooth roots 46, no local changes indicative of the presence of a fistula, and negative ICA. The follow-up X-ray showed condition after endodontic treatment (Figure 6). At the top of the mesial root, there is a slight widening of the periodontal fissure indicating the regeneration of periapical tissues - a clear healing condition compared to the photo taken immediately after filling the root canals, resorbed distal root. The visible outline of the periodontal gap being formed proves the process of regeneration of periapical periodontal tissues was going. The radiological status indicates a clinical stoppage of the distal root resorption process. Further monitoring of the condition of the periapical tissues and the distal root is recommended at 6-month intervals. The further prognosis for the tooth is favorable.
Discussion
External resorptions of tooth roots caused by inflammation occur relatively rarely, but their diagnosis requires firm decisions and prompt treatment initiation. The resorption processes often take place without tangible clinical symptoms and the teeth may respond properly to thermal and electrical stimuli. Modern diagnostic methods allow extending the direction of diagnostics only from a clinical examination, tests of the level of reaction to thermal and radiological stimuli to the examination of ERR markers from the gingival fluid and saliva [23-25]. Treatment of external resorptions can be a challenge for dentists in everyday clinical practice and the prognosis is uncertain. An improved prognosis can be achieved with a quick diagnosis and introduction of endodontic treatment with the use of chemo-mechanical preparation of the root canal system as soon as possible. Pain ailments often appear with a delay and testify to the advancement of the disease process. They occur when the disease covers the area of the tooth pulp and indicates advanced root resorption [3]. The literature mentions the possibility of treatment with a one-step filling of the gutta perch canal system with a sealant based on epoxy resins, with the postponement of the final filling with the use of hydroxide-calcium preparations, using the closure of the root apex resorbed with MTA preparations and cleaning the lesions from the root surface with the use of lasers. Although numerous studies show an uncertain prognosis [5,13,23-26], in the presented case the effect was favorable. In the presented case, immediately after confirming the external resorption of the root, a classic chemo-mechanical treatment of the root system of the tooth with gutta-percha obturation and sealing with AH + resin was performed. A favorable treatment result was obtained.
Conclusion
The process of external resorption very often takes place in a latent manner with asymptomatic teeth, often with vital pulp.
Symptoms often appear only when the chronic process is exacerbated.
The implemented endodontic treatment should be undertaken without undue delay.
ERR biomarkers from gingival fluid and saliva should be included in the diagnosis of ERR
High-resolution projections should be used in radiological diagnostics.
A favorable prognosis is influenced by quick diagnosis, general health, and the young age of the patient.
Selection of the treatment method: filling the root canal system directly after thorough chemo-mechanical preparation, indirect filling of the root canal system with calcium hydroxide-based materials, preparation and closure of the tooth root at the level of the resorption gap with MTA, and subsequent filling of the canal with gutta-percha and sealant based on epoxy resins, laser treatment of the resorptive cavity with Er - YAG lasers after classic endodontic treatment. The method of single-stage chemo-mechanical endodontic treatment presented in the discussed case, filling root canals with gutta-percha and AH + sealant gives favorable treatment results.
In the therapeutic process, it is possible to use regenerative treatments with the use of plasma fibrin, which stops resorption. However, the presented case report showed good long-term results using the classic simultaneous method of chemo-mechanical root canal preparation and obstruction.
Teeth with resorption after endodontic treatment require long monitoring of the condition of the root and periapical tissues.
- Andreasen JO. External root resorption: its implication in dental traumatology, paedodontics, periodontics, orthodontics and endodontics. Int Endod J. 1985 Apr;18(2):109-18. doi: 10.1111/j.1365-2591.1985.tb00427.x. PMID: 2860072.
- Beer R, Baumann MA, Kielbassa AM. Ilustrowane kompedium endodoncji. Lublin: Wydawnictwo Czelej; 2009. 22.
- Sołkiewicz E, Sokalski J, Sidorowicz K, Lipińska M, Resorpcja zewnętrzna korzeni drugiego zęba trzonowego szczęki spowodowana nieprawidłowym wyrzynaniem się zęba mądrości, Dental Forum, 2016 t. XLIV. 87-89.
- Jańczuk Z, Arłukowicz E, Dembowska E, Suszczewicz A, Próba leczenia prawie całkowitej resorpcji pourazowej korzeni górnych siekaczy przyśrodkowych, Mag Stom. 2005: 82–86.
- Jiang F, Chen J, Kula K, Gu H, Du Y, Eckert G. Authors' response. Am J Orthod Dentofacial Orthop. 2018 Jan;153(1):6. doi: 10.1016/j.ajodo.2017.11.004. PMID: 29287653.
- Jurczak A, Kołodziej J, Kościelniak D, Słowik J. Resorpcja zewnętrzna zamienna korzenia zęba jako późne powikłanie pourazowe i pacjentów w wieku rozwojowym, Implantoprotetyka. 2009; 4:41-43.
- Żuchowska L, Żuchowski J. Biologiczne leczenie miazgi, ozębnej i okostnej zębów stałych. Katowice: Wyd. Elamed; 2005; 73-80.
- Fuss Z, Tsesis I, Lin S. Root resorption--diagnosis, classification and treatment choices based on stimulation factors. Dent Traumatol. 2003 Aug;19(4):175-82. doi: 10.1034/j.1600-9657.2003.00192.x. PMID: 12848710.
- Lu J, Liu H, Lu Z, Kahler B, Lin LM. Regenerative Endodontic Procedures for Traumatized Immature Permanent Teeth with Severe External Root Resorption and Root Perforation. J Endod. 2020 Nov;46(11):1610-1615. doi: 10.1016/j.joen.2020.07.022. Epub 2020 Jul 28. PMID: 32730858.
- Fuss Z, Tsesis I, Lin S. Root resorption--diagnosis, classification and treatment choices based on stimulation factors. Dent Traumatol. 2003 Aug;19(4):175-82. doi: 10.1034/j.1600-9657.2003.00192.x. PMID: 12848710.
- Rabinovich IM, Snegirev MV, Markheev CI. Rezorbtsiia kornia zuba - étiologiia, patogenez, lechenie [Dental root resorption etiology, diagnosis and treatment]. Stomatologiia (Mosk). 2019;98(3):109-116. Russian. doi: 10.17116/stomat201998031109. PMID: 31322606.
- Tarabinejad M, Walton RE, [Red. pol. Borczyk R.], Endodoncja, Urban and Partner, Wrocław 2010. 198-200.
- Jasiński P, Sobiech P, Koprowicz E. Resorpcja zewnętrzna korzenia spowodowana urazem – opis przypadku, Nowa Stomatologia, 2011; 157-160.
- Krupiński J. Endodoncja praktyczna, Kwintesencja Warszawa. 2008; 36.
- Andreasen JO, Andreasen FM, Bakland LK, Flores MT, Kaczmarek U [red], Pourazowe uszkodzenia zębów. Wrocław: Urban & Partner. 2005; 47-83.
- Al-Momanii Z, Nixon P, Resorpcja wewnętrzna i zewnętrzna korzenia zęba – etiologia, rozpoznawanie i możliwości leczenia. Med Prakt Stom. 2013; 51-58.
- Świder K, Matys J, Flieger R, Zastosowanie lasera Er:YAG i materiału MTA w leczeniu zewnętrznej resorpcji korzenia – opis przypadku, Twój Przegląd Stomatologiczny. 2015; 30-32.
- Levander E, Malmgren O. Evaluation of the risk of root resorption during orthodontic treatment: a study of upper incisors. Eur J Orthod. 1988 Feb;10(1):30-8. doi: 10.1093/ejo/10.1.30. PMID: 3162877.
- Bargholz C, Hör D, Zirkel Ch [red. pol. Jańczuk Zb.], Endodoncja. Urban and Partner Wrocław 2007; 63-66.
- Yoshpe M, Einy S, Ruparel N, Lin S, Kaufman AY. Regenerative Endodontics: A Potential Solution for External Root Resorption (Case Series). J Endod. 2020 Feb;46(2):192-199. doi: 10.1016/j.joen.2019.10.023. Epub 2019 Dec 6. PMID: 31813579.
- Jiang F, Chen J, Kula K, Gu H, Du Y, Eckert G. Authors' response. Am J Orthod Dentofacial Orthop. 2018 Jan;153(1):6. doi: 10.1016/j.ajodo.2017.11.004. PMID: 29287653.
- Wu JY, Li X, Wang CL, Ye L, Yang J. [Research progress on the pathogenesis of inflammatory external root resorption]. Hua Xi Kou Qiang Yi Xue Za Zhi. 2019 Dec 1;37(6):656-659. Chinese. doi: 10.7518/hxkq.2019.06.015. PMID: 31875446; PMCID: PMC7030755.
- Mona M, Abbasi Z, Kobeissy F, Chahbandar A, Pileggi R. A Bioinformatics Systems Biology Analysis of the Current Oral Proteomic Biomarkers and Implications for Diagnosis and Treatment of External Root Resorption. Int J Mol Sci. 2021 Mar 20;22(6):3181. doi: 10.3390/ijms22063181. PMID: 33804739; PMCID: PMC8003910.
- Lai Y, Pan WL, Liu C, Huang JY, Hua CG. [Prognosis of teeth with external root resorption caused by adjacent impacted teeth]. Hua Xi Kou Qiang Yi Xue Za Zhi. 2019 Jun 1;37(3):280-284. Chinese. doi: 10.7518/hxkq.2019.03.010. PMID: 31218862; PMCID: PMC7030087.
- Gregorczyk-Maga I, Szustkiewicz-Karoń A, Kaszuba M, Januszek R, Rahnama M, Jurczak A, Maga P. Prognostic markers of post-traumatic dental external root resorption in children-a pilot study. Dent Traumatol. 2021 Oct;37(5):699-705. doi: 10.1111/edt.12682. Epub 2021 May 10. PMID: 33970554.
- van der Sleen-Schulte WE, Polder BJ. Gegeneraliseerde externe apicale wortelresorptie: etiologie in 3 röntgenologisch vergelijkbare casussen [Generalised external apical root resorption: aetiology in 3 radio-graphically comparable cases]. Ned Tijdschr Tandheelkd. 2020 Nov;127(11):607-615. Dutch. doi: 10.5177/ntvt.2020.11.20005. PMID: 33252602.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
