Journal of Clinical Research and Ophthalmology
Minimal-invasive explantation of sulcus-fixated toric-multifocal additional intraocular lenses despite excellent visual measurements: A case report
Jens Schrecker1* and Achim Langenbucher2
2Chair of Experimental Ophthalmology, Saarland University, Homburg/Saar, Germany
Cite this as
Schrecker J, Langenbucher A (2022) Minimal-invasive explantation of sulcus-fixated toric-multifocal additional intraocular lenses despite excellent visual measurements: A case report. J Clin Res Ophthalmol 9(2): 025-028. DOI: 10.17352/2455-1414.000100Copyright License
© 2022 Schrecker J, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.A 40-year-old male patient was referred to our hospital for cataract surgery in both eyes with the explicit wish to get simultaneously rid of his eyeglasses. To allow for postoperative flexibility, we performed a bilateral implantation of a monofocal intraocular ‘standard’ lens in combination with an additional toric-multifocal lens. During the postoperative examinations the patient complained about pronounced halos in twilight and darkness.
Visual acuity was excellent for distance, intermediate and near distances. Both IOLs were well centered and showed no tilt or other morphological discrepancies. Despite our extensive treatment efforts, including supportive training for neural adaptation, the patient perceived no signs of improvement. Finally, we had to explant both additional IOLs.
The primary corneal incisions were bluntly reopened and the additional IOLs were removed in a minimal traumatic procedure. With the retained IOL in the capsular bag and subsequently ordained progressive eyeglasses the patient obtained full vision at all distances.
Our preoperative planning to compensate for presbyopia with a separate IOL, proved to be a good decision. Otherwise, the explantation of a multifocal IOL, ingrown in the capsular bag, could have entailed a number of complications. In such delicate cases, additional IOL may offer a very save and simple alternative.
Introduction
The patient’s wish for excellent distance, near and intermediate visual acuity with simultaneous independence of eyeglasses or contact lenses is the reason for the development and permanent improvement of a variety of multifocal (or accommodative) optics. Over the last two decades excellent results after the implantation of multifocal IOLs (diffractive, refractive or hybrid) have been reported in many studies [1-5]. However, despite the most modern and standardized surgical technics and IOL-calculation methods postoperative deviations from the target refraction can occur and may decisively impair the patient’s primary objective to get rid of their eyeglasses. Furthermore, after the implantation of multifocal optics, visual dysfunction may occur due to a reduced contrast sensitivity or disturbing photic phenomena like halos, glare or starbursts [6]. Based on neural adaptive mechanisms in most cases there is an adaptation to these side effects within some weeks or months after surgery. There is also the possibility to reduce such phenomena by the application of mild miotic eye drops.
Nevertheless, in rare cases patients are not amenable to these measures and the only option is the explantation of the multifocal optic. The removal of an IOL out of the capsular bag can pose significant problems to the surgeon, especially when a long period of time has passed since the primary procedure and the haptics have already strongly grown together with the capsular bag. IOL-systems consisting of an IOL in the capsular bag and an additional multifocal IOL in the sulcus offer a solution for such cases. Because there is no adhesion between the haptics and the surrounding sulcus tissue the removal or the exchange of an additional IOL can be carried out in a gentle procedure and relatively easy procedure [7]. Moreover, there is no time restriction for these IOL if an explantation becomes necessary.
Case report
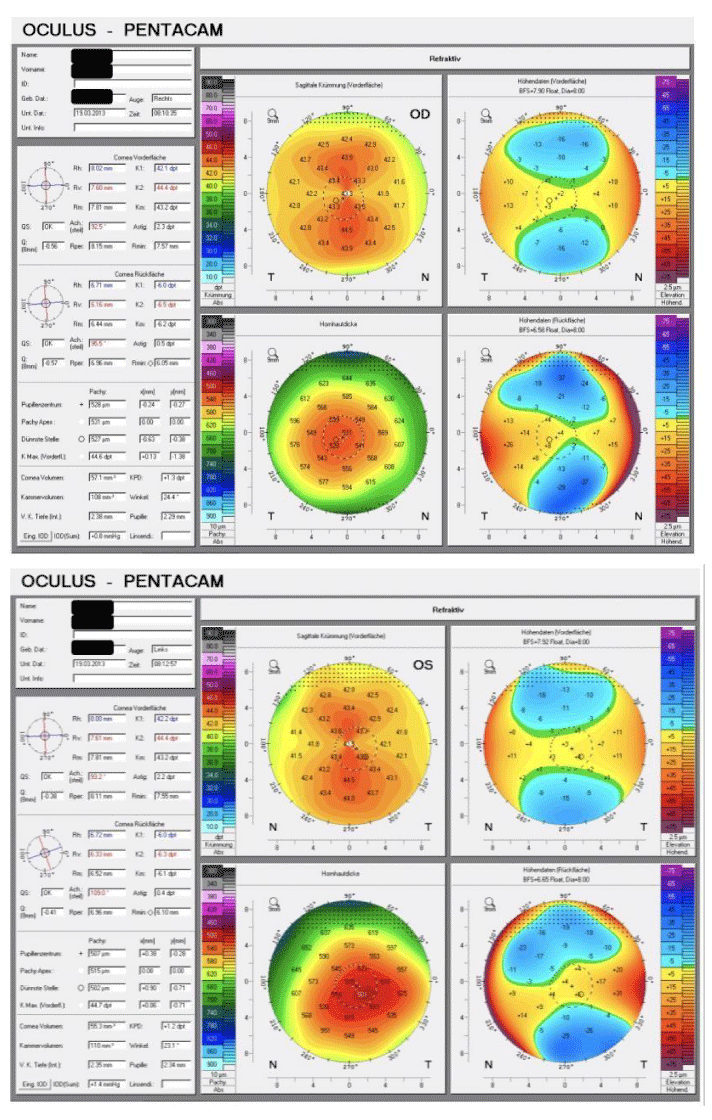
A 40-year-old man with cataract and corneal astigmatism presented in our hospital for cataract surgery with the explicit wish to get also rid of his eyeglasses. At that time the subjective refraction was -1.5 D + 1.5 D × 85° for the right eye (OD) and -3.25 D + 0.75 D × 95° for the left eye (OS). The eyes showed no further pathology. Both pupils had normal size and a normal light reaction (photopic/mesopic/scotopic diameter: 2.5mm/3.0mm/6.0mm in both eyes). The corneal topography (Pentacam HR, Oculus Optikgeräte, Germany) showed a regular astigmatic configuration (Figure 1) and corneal astigmatism (IOL Master 500, Carl Zeiss Meditec, Germany) was 2.22 D at 90° for the right eye and 2.45 D at 92° for the left eye.
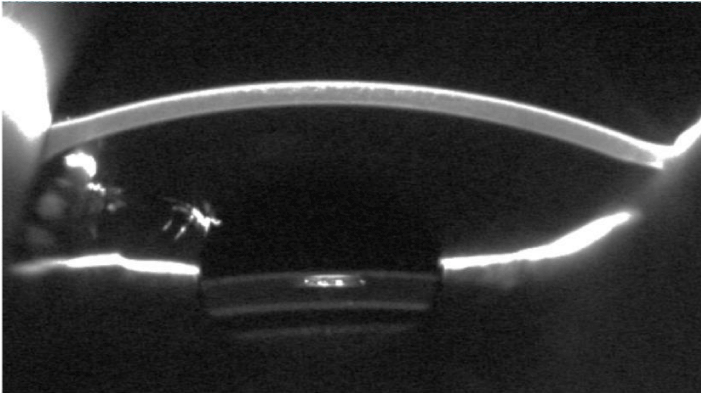
The thorough and detailed anamnesis revealed no specific hints regarding contraindications for a multifocal compensation of presbyopia. After discussing thoroughly different options for refractive procedures we decided in favor of the implantation of a lens system. A simultaneous implantation of a monofocal IOL (MC 6125 AS, HumanOptics, Germany) in the capsular bag and a toric-multifocal additional IOL (Sulcoflex 653Z, Rayner Surgical) in the ciliary sulcus was planned. Uneventful IOL surgery of both eyes was performed with lens powers of + 19.5 D (in the bag IOL) and -1.5 D cyl + 3.0 D (additional IOL) in the right eye and + 19.0 D combined with -1.0 D cyl + 2.0 D in the left eye. All IOLs showed no decentration or tilt and a uniform gap between their opposing surfaces (Figure 2).
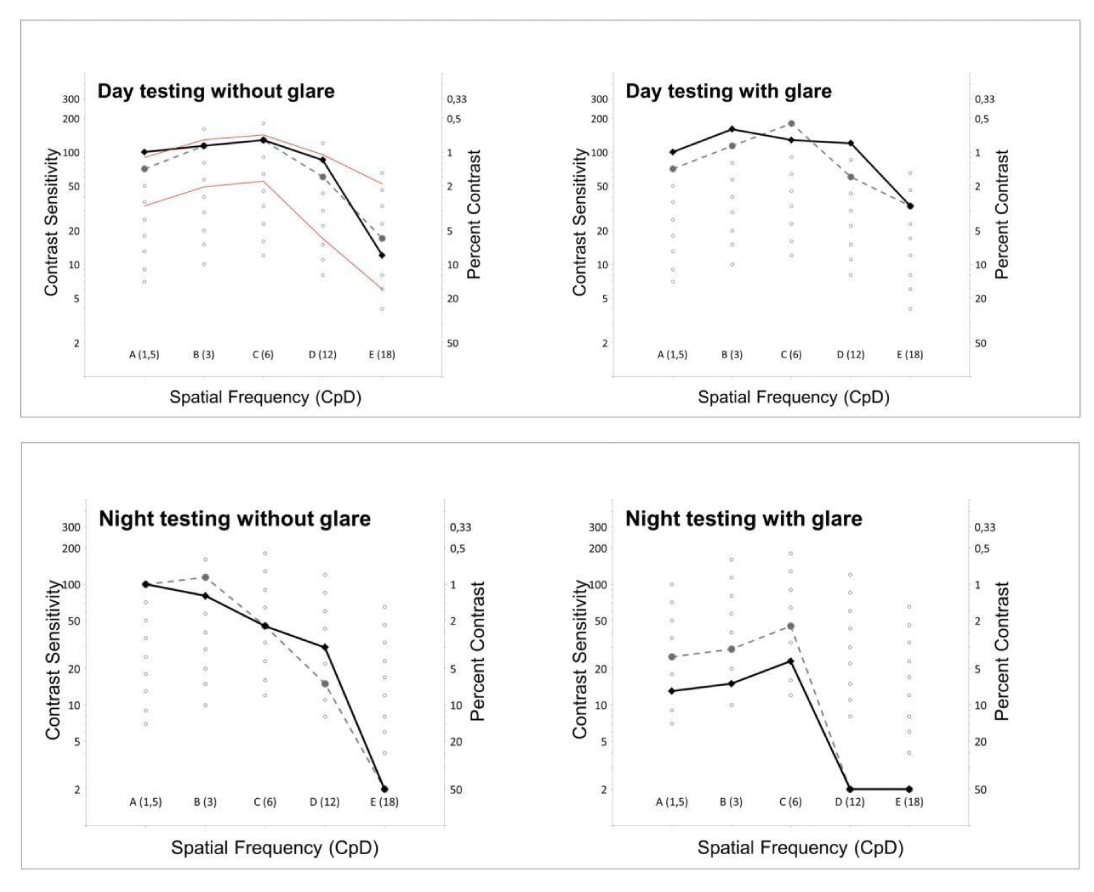
Forty and 28 days after primary surgery of the right and left eye, uncorrected distance visual acuity (UDVA) and uncorrected intermediate visual acuity (UIVA) was 0.0 logMAR for both eyes. Uncorrected near visual acuity (UNVA) of the right and left eye was -0.1 and 0.0 logMAR, respectively. Eyeglasses did not further improve these values. In Figure 3 contrast sensitivity (Contrast Sensitivity Tester 1800, CST 1800, Vision Sciences Research Corporation, San Ramon, CA, USA) at 2 different luminance levels (85 candela (cd)/m2: ‘high photopic´ and 6 cd/m2: ´low photopic´) is displayed with and without glare. Under daylight conditions and in night testing without glare the patient showed very good results. In night testing with glare the results were noticeably worse.
Despite all these excellent results, the patient was extremely disappointed and unsatisfied because of disturbing halos during twilight and darkness. At first, we repeatedly explained the optical principle used, in particular with regard to potential side effects and the long-term process of an expected neural adaptation. Because the complaints only occurred in darkness, we firstly treated with brimonidine 0.2% eye drops and afterwards we switched to pilocarpine 1.0% to narrow the pupils. The miotic effect was clearly visible in slit lamp examination. Visual acuity values stayed the same for all 3 distances tested. Within the first days after beginning local medication with pilocarpine the patient complained about persistent pain in his eyes and refused further treatment with any miotic eye drops, especially because he had felt no distinct improvement of his photic phenomena. In the further course the patient was not amenable to any additional attempts to minimize his complaints and explantation of the additional lenses was planned on both eyes.
The surgical procedure passed without any complications: The primary cataract incision and paracentesis could easily be reopened and the anterior chamber, especially the sulcus ciliaris, was filled with a higher-viscous viscoelastic (Healon GVâ, Abbott Medical Optics, Santa Ana, USA). The pupil had been dilated by mydriatic eye drops and the haptics of the additional lens were gently luxated in front of the iris with an iris hook and a spatula. Through the preexisting limbal incision of 2.8 mm the additional IOL was simply pulled out by means of straight forceps with serrated tips (Geuder, Heidelberg, Germany). After aspiration of the viscoelastic material the 2 incisions were hydrated. Postoperative local therapy was the same as after standard cataract surgery (with antibiotics and steroids). The postoperative course was uneventful for both eyes. Position and stability of the IOLs in the capsular bag remained unaffected.
Discussion
The most common causes for dissatisfaction after implantation of multifocal IOLs are residual ametropia, especially astigmatism, higher order aberrations like coma and spherical aberration, a large pupil size, decentration or tilt of the IOL(s), posterior capsule opacification, dry eye syndrome [6] or the lack of neural adaptation. Furthermore, multifocal optics cause a reduction in contrast sensitivity and induce photic phenomena like glare, halos or starbursts [9,10]. A combination of several of these effects is particularly unfavorable.
Preoperatively, a comprehensive diagnostic and an elaborate consultation about the therapeutic options, potential risks and side effects of the considered refractive surgical procedures are mandatory. The patient's individual expectations relating to postoperative results must be thoroughly discussed and specifically taken into account. A realistic assessment on achievable results is an essential precondition for the postoperative satisfaction of patient and doctor.
In the case described above, the patient was preoperatively interested in the ‘best’ possible treatment with ‘good’ vision for far, intermediate and near distances without glasses. He only reached an uncorrected distance visual acuity of 0.3 LogMAR with the right eye and 0.4 LogMAR with the left eye. According to anamnesis, he used his glasses very rarely. The obvious potential for improvement of visual acuity and the quite tolerant attitude supported our assumption of good preconditions for multifocal optics. Furthermore, all clinical findings, including corneal topography, mesopic pupil diameter, and precorneal tear film were inconspicuous.
At first after the IOL implantation, the patient was very satisfied with his improved visual ability. Contrast sensitivity (except for night conditions with glare) was in the upper range of healthy eyes. But from the patient's point of view, the disturbing halos during twilight and darkness dwarfed all the objectively measured excellent results. Unfortunately, despite extensive explanations with guidance for vision training, for the patient there was no perceptible effect of neural adaptation. Our conservative efforts to minimize his complaints and to allow for more time for adaptation were not successful. Retrospectively, the primary decision to implant an optical system with the multifocal part separated with the Add-on-IOL gave us at least the opportunity of reacting in an appropriate manner with minimal surgical trauma.
Due to this experience, we believe it is important to consider all available options. Despite thorough anamnesis and checking for possible contraindications of multifocal optics and even with excellent visual outcomes, patients might be unsatisfied due to photic phenomena. This might be especially true in younger patients with high demands of their vision at twilight and darkness. With explanting the add-on IOL we could satisfy the patients’ needs after all. This would have been more challenging had we implanted a multifocal IOL instead of the combination.
Conclusions
The use of multifocal additional sulcus lenses offers a valuable escape procedure with a gentle reversibility option in case of intolerance of the multifocal optic. Irrespective of the time interval after the implantation, potential complications associated with ingrown IOLs in the capsular bag can be avoided.
- Dexl AK, Zaluski S, Rasp M, Grabner G. Visual performance after bilateral implantation of a new diffractive aspheric multifocal intraocular lens with a 3.5 D addition. Eur J Ophthalmol. 2014 Jan-Feb;24(1):35-43. doi: 10.5301/ejo.5000315. Epub 2013 Jun 2. PMID: 23787450.
- Cillino G, Casuccio A, Pasti M, Bono V, Mencucci R, Cillino S. Working-age cataract patients: visual results, reading performance, and quality of life with three diffractive multifocal intraocular lenses. Ophthalmology. 2014 Jan;121(1):34-44. doi: 10.1016/j.ophtha.2013.06.034. Epub 2013 Aug 14. PMID: 23953097.
- van der Linden JW, van Velthoven M, van der Meulen I, Nieuwendaal C, Mourits M, Lapid-Gortzak R. Comparison of a new-generation sectorial addition multifocal intraocular lens and a diffractive apodized multifocal intraocular lens. J Cataract Refract Surg. 2012 Jan;38(1):68-73. doi: 10.1016/j.jcrs.2011.06.034. Epub 2011 Nov 10. PMID: 22078117.
- Lane SS, Javitt JC, Nethery DA, Waycaster C. Improvements in patient-reported outcomes and visual acuity after bilateral implantation of multifocal intraocular lenses with +3.0 diopter addition: multicenter clinical trial. J Cataract Refract Surg. 2010 Nov;36(11):1887-96. doi: 10.1016/j.jcrs.2010.05.028. PMID: 21029897.
- Zelichowska B, Rekas M, Stankiewicz A, Cerviño A, Montés-Micó R. Apodized diffractive versus refractive multifocal intraocular lenses: optical and visual evaluation. J Cataract Refract Surg. 2008 Dec;34(12):2036-42. doi: 10.1016/j.jcrs.2008.06.045. PMID: 19027556.
- de Vries NE, Webers CA, Touwslager WR, Bauer NJ, de Brabander J, Berendschot TT, Nuijts RM. Dissatisfaction after implantation of multifocal intraocular lenses. J Cataract Refract Surg. 2011 May;37(5):859-65. doi: 10.1016/j.jcrs.2010.11.032. Epub 2011 Mar 11. PMID: 21397457.
- Liekfeld A, Ehmer A, Schröter U. Visual function and reading speed after bilateral implantation of 2 types of diffractive multifocal intraocular lenses: Add-on versus capsular bag design. J Cataract Refract Surg. 2015 Oct;41(10):2107-14. doi: 10.1016/j.jcrs.2015.10.055. PMID: 26703286.
- Hohberger B, Laemmer R, Adler W, Juenemann AG, Horn FK. Measuring contrast sensitivity in normal subjects with OPTEC 6500: influence of age and glare. Graefes Arch Clin Exp Ophthalmol. 2007 Dec;245(12):1805-14. doi: 10.1007/s00417-007-0662-x. Epub 2007 Aug 11. PMID: 17694315.
- Montés-Micó R, Alió JL. Distance and near contrast sensitivity function after multifocal intraocular lens implantation. J Cataract Refract Surg. 2003 Apr;29(4):703-11. doi: 10.1016/s0886-3350(02)01648-6. PMID: 12686237.
- Häring G, Dick HB, Krummenauer F, Weissmantel U, Kröncke W. Subjective photic phenomena with refractive multifocal and monofocal intraocular lenses. results of a multicenter questionnaire. J Cataract Refract Surg. 2001 Feb;27(2):245-9. doi: 10.1016/s0886-3350(00)00540-x. PMID: 11226790.

Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
