Journal of Clinical Research and Ophthalmology
Removal of Flanged Sutureless Scleral Fixated Intraocular Lens
Remzi Karadag*
Cite this as
Karadag R (2020) Removal of Flanged Sutureless Scleral Fixated Intraocular Lens. J Clin Res Ophthalmol. 7(1): 031-032. DOI: 10.17352/2455-1414.000069Introduction
Recently, sutureless scleral-fixated intraocular lens (SSF-IOL) techniques have become popular in clinical practice [1]. These methods are newer and have been developed to eliminate the suture-related complications of sutured scleral fixation methods [2-5]. These methods base on fixation of the IOL haptics within the sclera. The stability of IOLs is provided by the scar tissue that constitutes around the haptics [1]. Although there are some intraoperative and postoperative complications have been reported in the literature, short and moderate term results of these techniques are acceptable [2,3,6,7]. These complications generally are depended on types of SSF-IOL technique that are included hyphema, corneal edema, IOL dislocation, exposure of haptic, iris capture of IOL, break of IOL haptic, subconjunctival haptic, elevated intraocular pressure, hypotony, choroidal detachment, vitreous hemorrhage, and cystoids macular edema [1-8]. To our best knowledge, there is no article about removal of flanged sutureless scleral-fixated IOL in the literature.
In this article, it was aimed to present the technique of removal of flanged sutureless scleral-fixated IOL in traumatic and vitrectomized eye that had excessive fibrous membrane around the IOL.
Case report
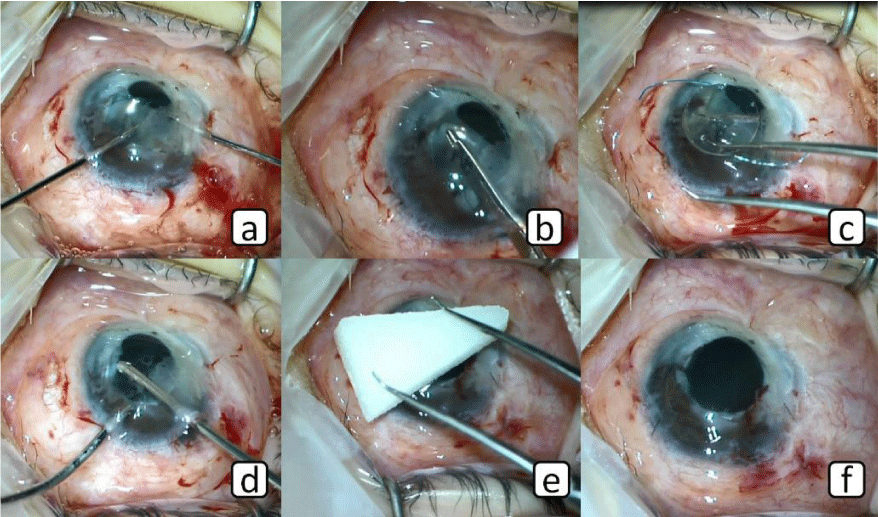
An 8-year-old male patient who underwent cataract and vitrectomy surgery due to traumatic eye injury approximately 12 months ago. After then, flanged sutureless scleral-fixated IOL implantation surgery with 26-gauge needle was performed in our clinic, because patient had insufficient capsular support. Four months after this surgery, intense fibrous membrane was developed around the IOL (Figure 1a). Therefore, it was planned the cleaning of the fibrous membrane and extraction of the IOL. Surgery was performed as briefly described below: The conjunctiva was opened with the scissor and tips of the haptics became visible (Figure 1b). The tips of the haptics (flanged parts) were cut by scissor (Figure 1c,d). Main corneal incision and two paracenteses were made with 3.0 and MVR knives. The anterior chamber was filled with Ocular Viscoelastic Device (OVD). Intense fibrous membrane was cut with the 23 gauge retinal knife and was removed (Figure 1e,f). The IOL was turned clockwise with two 23 gauge retinal forceps (Figure 2a). Thus, the haptics were taken from the scleral tunnels to the anterior chamber. After then, IOL was cut by IOL cutter scissor and was removed from the main corneal incision (Figure 2b,c). OVD was taken out of the eye with aspiration and inspiration cannulas (Figure 2d). The main and paracentesis incisions were sutured with 10-0 nylon suture. At the end of the surgery, EDDA solution was applied for band keratopathy (Figure 2e,f). No complications were seen intraoperatively or postoperatively. After 4 months follow-up period eye was seen stabilized.
Discussion
SSF-IOL implantation methods are usually performed as implantation of the IOL in aphakic eyes with insufficient capsular support [1-10]. These techniques are becoming more widespread as short and moderate term results are acceptable [2,3,6,7]. There are a lot of studies about these methods in the literature [1-3,6]. They were reported some complications. Some of them were intra-operative complications that were included hyphema, vitreous hemorrhage, haptic breakage, haptic dislocation during surgery, and conjunctival laceration [1-3,6]. Postoperative complications were included haptic exposure, corneal edema, ocular hypertension, iris capture of IOL, IOL decentration, macular edema, hypotony, vitreous hemorrhage, and choroidal detachment [1-8]. Although there are so many complications reported [1-10], no complications have been reported that would require removal of the IOL in postoperative follow-up period. Because in this case eye underwent several procedures and had severe uveitic reaction, intense fibrous membrane developed around the IOL. This membrane and IOL were removed because it affected the patient’s vision. During removal of the IOL, first, after the conjunctiva was opened and the haptics become visible, the flanged tips of the haptics were cut. This procedure was done for two reasons. First reason: The haptics were covered with scar tissue. Due to the scar tissue, it would be very difficult to move through the sclera for the haptics with flanged tips. Second reason: Flanged tips of the haptics could damage to the intraocular tissues including retina and ciliary body. Because the flanged tips of the haptics were cut, they easily moved within the sclera and did not damage to the surrounding tissue.
Conclusion
This technique is a suitable and safe surgical method for removal of the IOL with flanged tips of haptics
- Karadag R, Celik HU, Bayramlar H, Rapuano CJ (2016) Sutureless Intrascleral Fixated Intraocular Lens Implantation. J Refract Surg 32: 586-597. Link: https://bit.ly/3ggMCny
- Totan Y, Karadag R (2013) Two techniques for sutureless intrascleral posterior chamber IOL fixation. J Refract Surg 29: 90-94. Link: https://bit.ly/36lV3cK
- Abbey AM, Hussain RM, Shah AR, Faia LJ, Wolfe JD, et al. (2015) Sutureless scleral fixation of intraocular lenses: outcomes of two approaches. The 2014 Yasuo Tano Memorial Lecture. Graefes Arch Clin Exp Ophthalmol 253: 1-5. Link: https://bit.ly/2ZvyGju
- Prenner JL, Feiner L, Wheatley HM, Connors D (2012) A novel approach for posterior chamber intraocular lens placement or rescue via a sutureless scleral fixation technique. Retina 32: 853-855. Link: https://bit.ly/3cYbBKa
- Totan Y, Karadag R (2012) Trocar-assisted sutureless intrascleral posterior chamber foldable intra-ocular lens fixation. Eye (Lond) 26: 788-791. Link: https://bit.ly/36qN120
- Kumar DA, Agarwal A, Packiyalakshmi S, Jacob S, Agarwal A (2013) Complications and visual outcomes after glued foldable intraocular lens implantation in eyes with inadequate capsules. J Cataract Refract Surg 39: 1211-1218. Link: https://bit.ly/2XmV4cf
- Scharioth GB, Prasad S, Georgalas I, Tataru C, Pavlidis M (2010) Intermediate results of sutureless intrascleral posterior chamber intraocular lens fixation. J Cataract Refract Surg 36: 254-259. Link: https://bit.ly/36q3J1I
- Matsui Y, Matsubara H, Hanemoto T, Kondo M (2015) Exposure of haptic of posterior chamber intraocular lens after sutureless intrascleral fixation. BMC Ophthalmol 15: 104. Link: https://bit.ly/3cW2MAx
- Karadag R, Bayramlar H, Azari AA, Rapuano CJ (2016) Trocar-Assisted, Sutureless, Scleral-Fixated Intraocular Lens Implantation Combined with Penetrating Keratoplasty. Cornea 35: 1261-1265. Link: https://bit.ly/36A6Owp
- Totan Y, Karadag R (2014) New approach: removal of silicone oil and trocar assisted sutureless scleral fixated intraocular lens implantation at the same session. Int J Ophthalmol 7: 734-736. Link: https://bit.ly/2A5keE5

Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
