Journal of Clinical Research and Ophthalmology
A case series on ocular manifestations in Steven Johnson Syndrome and their varied presentation-Review of literature
Nagalakshmi Narayana-Swamy1* and Alhaj Farhath Tasneem2
2Professor, Department of Ophthalmology, Vydehi Institute of Medical Sciences and Research Center, Bangalore, India
Cite this as
Swamy NN, Tasneem AF (2020) A case series on ocular manifestations in Steven Johnson Syndrome and their varied presentation-Review of literature. J Clin Res Ophthalmol 7(1): 004-007. DOI: 10.17352/2455-1414.000063Purpose: To discuss the possible ocular manifestations of Steven Johnson Syndrome and their management among different cases.
Case: Patients aged 9, 15, 43years with Steven- Johnson Syndrome were reviewed for severity of ocular involvement. These patients presented with fever and involvement of skin, oral mucosa and conjunctiva.
Case 1: Secondary to use of? Mefenamic acid, treated conservatively.
Case 2: Secondary to use of carbamazepine, treated conservatively.
Case 3: Secondary to use of cotrimoxazole, had adhesion of both upper and lower eyelids and part of lower bulbar conjunctiva to the lower eye lid.Treated by ocular surface reconstruction with mucus membrane graft.
Conclusion: All the three patients with Steven Johnson Syndrome had varied manifestations requiring different treatment modailites.Appropriate intervention during acute ocular presentation and careful vigilance aids management.
Introduction
Steven-Johnson Syndrome (SJS) is a rapidly progressive mucocutaneous reaction charecterised by immune mediated cell death with extensive epidermal necrosis resulting in severe morbidity and mortality secondary to drugs, infection, Graft versus host reaction [1]. usually presents as a non-specific febrile illness with malaise, headache, and rhinorrhea with polymorphic lesions on the skin and mucus membrane.
The incidence has been estimated to be around 1-9/1,000,000 persons per year with a mortality rate upto 5%.Many drugs have been identified as the etiological agents such as sulfonamide derivatives, anticonvulsants such as phenytoin, carbamazepine, Non-steroidal anti-inflammatory drugs and oxide inhibitors such as allopurinol [2,3].
Infections have also been recognized to have a role in occurrence of Steven Johnson Syndrome. Common pathogens noted are Mycoplasma Pneumoniae, Enterovirus, Hepatitis B virus, Group A Streptococcus and Mycobacterium Tuberculosis [4].
The exact pathophysiology involved is yet to be elucidated. It is thought to be a autocrine or paracrine interaction between Fas and Fas Ligand (FasL) produced by keratinocytes and peripheral mononuclear cells (Soluble type of FasL) resulting in apoptosis of keratinocytes and paucity of T Cell infiltrates [5,6]. And in an drug induced SJS the possible mechanism is the expression of specific MHC alleles by the keratinocytes on direct contact with granzyme and perforis relased by Drug-specific CD8+ cytotoxic T-cells.
Steven-Johnson Syndrome commonly involves the oral mucosa and conjunctiva. Various studies have shown involvement of the conjunctiva in about 49%-81% [7]. And the treatment aims at restoration of the anatomical and physiological properties of the ocular surface [8].
The present case series is aimed at describing the various ocular manifestation of Steven Johnson Syndrome in different age groups, caused by different agents of variable severity requiring different principles of management.
Case history
Three Patients aged 9, 15, 43years females with Steven-Johnson Syndrome secondary to various agents were reviewed for severity of ocular involvement over a duration of one year {DECEMBER 2018-DECEMBER 2019} at the Ophthalmology outpatient unit. Patients were included in the report after an informed oral consent. These patients presented with fever, skin rash, sloughing of skin, erythematous macules with ocular presentation of variable severity. All patients had mild-moderate lid oedema, conjunctival injection, chemosis & membranous conjunctivitis with discharge.
Visual acuity was recorded using snellen’s chart, near vision by roman test type charts and color vision by Ishihara chart.
Case 1
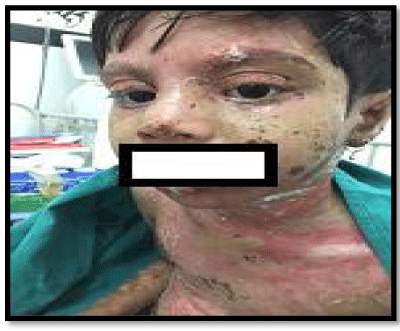
A 9 year old female presented with features of Steven Johnson syndrome on slit lamp examination such as mild grade lid edema, mild conjunctival injection with mucoid discharge present secondary to use of syrup mefenamic acid for abdominal pain. Her visual acuity was 20/20 both eyes with normal near vision and color vision. Ocular fundus was normal on direct ophthalmoscopy. Patient was managed conservatively with topical antibiotics and artificial tears with supportive care. Patient was followed up regularly and had no further ocular complaints (Figure 1).
Case 2
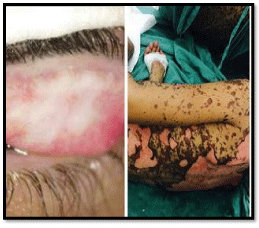
A 15 year old female presented with features of Steven Johnson syndrome consistent with above mentioned ocular features of severe lid edema, chemosis,conjunctival congestion with discharge, with a small corneal epithelial defect on slit lamp examination secondary to use of carbamazepine for seizure disorder. Her vision and fundus features could not be assessed initially due to severe blepharospasm .She was managed conservatively with glass rod sweeping, topical antibiotics and artificial tears with supportive care. Patient was followed up and vision of 20/20 was noted, Normal ocular fundus with regular follow up (Figure 2).
Case 3
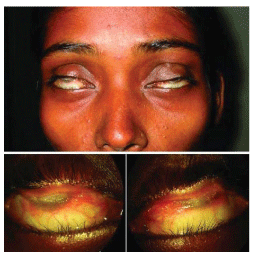
A 43 year old female with late sequelae of cotrimoxazole induced Steven Johnson Syndrome for further management. At the time of presentation her vision was hand movements close to face in both eyes. She presented with symblepharon of upper eyelid involving upto 1/2-3/4th of cornea and a part of lower bulbar conjunctiva with lower eye lid bilaterally. Ocular fundus was normal on B scan. Digital Intraocular pressure was normal. Further ocular examination could not be done due to symblepharon. Routine blood investigations were normal.
Conjunctivo-corneal adhesions were released by superficial lamellar dissection and ocular surface reconstruction (both superior bulbar conjunctiva and lower bulbar conjunctiva) was done using buccal mucus membrane graft harvested from the lower lip after injecting Lignocaine 2% with adrenaline (1 in 2,0000 units) in both eyes and was secured with vicryl sutured. Graft size was 22×5mm in right eye and 18×4mm in Left eye applied over superior bulbar conjunctiva. And to the lower bulbar conjunctiva MMG of size of 12×2 was used and secured with sutures. A bandage contact lens was placed over the cornea and a conformer was placed to prevent further adhesions. She was kept on oral antibiotic coverage (Oral Levofloxacin 500mg ODX 5days, topical fluroquinolones, Topical low potent steroids and artificial tears postoperatively. The graft took up well giving her a vision of 20/80 over 3month follow up and maintained over time (Figure 3).
Discussion
The exact aetiopathogenesis of Steven Johnson Syndrome is not known. The role of drugs as an etiological agent is important. The common causative agent have been reported to be drugs belonging to class of long acting sulfonamides and chloroquine [9,10]. And the understanding of ocular adnexal involvement has been limited so far.
In the acute phase they present with bilateral membranous conjunctivitis and in late stages with alteration ocular surface morphology such as symblepharon, entropion, conjunctival inflammation, corneal neovascularization with severe xerosis [11,12].
The major aim of early intervention is to prevent further complication and in late phases of Steven Johnson Syndrome is reconstruction of ocular surface to correct the chronic inflammation [8]. The management of late sequelae remains a challenge because of the irreversible alteration in the ocular surface.
Various surgical approaches have been tried and among these, mucus membrane graft is the simplest [13] and the best option when a healthy conjunctival tissue is not available. Amniotic membrane grafting can also be considered for grafting due to its immense role in maintaining the physiology [14].
Conclusion
The definitive management of Steven Johnson Syndrome remains to be established. The Role of supportive care and identification, with-drawl and reporting of these potential offending drugs is underscored; these are the measures that provide the most proven benefit. There is no active therapeutic regimen with unequivocal benefit for treatment of this condition.
It is important for establishment of a definitive treatment protocol and an active awareness among clinician’s for a safe practice.
Statement of Consent
The consent to publish the images of the patients and consent by guardian in case of minors has been obtained before disclosure.
We sincerely thank our patients for being the reflections in this work.
- Burns T, Breathnach S, Cox N, Griffiths C (2004) Rooks Textbook of Dermatology. 7th edition Oxford: Blackwell Science 4568. Link: http://bit.ly/2U84fgE
- French LE (2006) Toxic epidermal necrolysis and Steven Johnson syndrome: Our current understanding. Allergol Int 55: 9-16. Link: http://bit.ly/2u2GADM
- Deore SS, Dandekar RC, Mahajan AM, Shiledar VV (2014) Drug induced-Stevens Johnson syndrome: A case report. Int J Sci Stud 2: 84-87. Link: http://bit.ly/2uHaNbA
- Sah R, Neupane S, Khadka S, Poudyal S, Paneru HR, et al. (2019) A Case Study of Stevens-Johnson Syndrome-Toxic Epidermal Necrolysis(SJS-TEN) Overlap in Mycoplasma pneumonia-Associated Tracheobronchitis. Case Rep Infect Dis 2019:5471765. Link: http://bit.ly/36Fe7Ru
- Kinoshita Y, Saeki H (2016) A review of the pathogenesis of toxic epidermal necrolysis. J Nippon Med Sch 83: 216-222. Link: http://bit.ly/2uGPRBx
- Labreze CL, Lamireau T, Chawki D, Maleville J, Taieb A (2000) Diagnosis,classification, and management of erythema multiforme and Steven-Johnson syndrome. Arch Dis Child 83: 347-352.
- Arstikatis MJ. Ocular aftermath of Stevens Johnson syndrome: review of 33cases. Ophthalmology 1973; 90: 376-79. Link: http://bit.ly/2O7GTny
- Shimazaki Y, Yang HY, Tsubota K (1997) Amniotic membrane transplantation for ocular surface reconstruction in patients with thermal and chemical burns.Ophthalmology 104: 2068-2076. Link: https://bit.ly/2UcyanV
- Bianchine JR, Macareg PV, Lasang LI, Azarnff DL, Brunk SF, et al. (1968) Drugs as etiological factors in SJ Syndrome. Am J Med 44: 390-405. Link: https://bit.ly/3aSLh3y
- Beedimoni RS, Rabhimaiah S (2004) Oral cholorquine – induced Stevens Johnson Syndrome. Indian J Pharmacol 36: 1. Link: https://bit.ly/36AIAAt
- Stewart MG, Duncan NO, Frankin DJ, Friedman EM, Sulek M (1994) Head and neck manifestations of erythema multiforme in children. Otolaryngol Head Neck Surg 111: 236-242. Link: https://bit.ly/37I092W
- Tsubota K, Satake Y, Kaido M, Shinozaki N, Shimmura S, et al. (1999) Treatment of severe ocular surface disorders with corneal epithelial stem-cell transplantation. N Engl J Med 340: 1697-703. Link: https://bit.ly/2uJr7Zd
- Henderon HWA, Collin JRO (2008) Mucous Membrane grafting .IN: Geerling G, Brewitt H,editors. Surgery for the Dry Eye.Vol 41. Basel Karger: Dev Ophthalmol 230-242. Link: https://bit.ly/315M7Wh
- Shimazaki J, Shinozaki N, Tugboat K (1998) Transplantation of amniotic membrane and limbal autograft for patients with recurrent pterygium associated with symblepharon. Br J Ophthalmol 82: 235-240. Link: https://bit.ly/36Dl8Cv

Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.
 Save to Mendeley
Save to Mendeley
