Journal of Cardiovascular Medicine and Cardiology
Cardiac arrest due to intentional yew tree (Taxus baccata) ingestion
Dorota Ochijewicz1*#, Anna Fojt1#, Jakub Zieniewicz2 and Robert Kowalik1
2Department of Anesthesia and Intensive Care, Medical University of Warsaw, Warsaw, Poland
#Contributed Equally to the Study
Cite this as
Ochijewicz D, Fojt A, Zieniewicz J, Kowalik R (2022) Cardiac arrest due to intentional yew tree (Taxus baccata) ingestion. J Cardiovasc Med Cardiol 9(3): 020-021. DOI: 10.17352/2455-2976.000181Copyright License
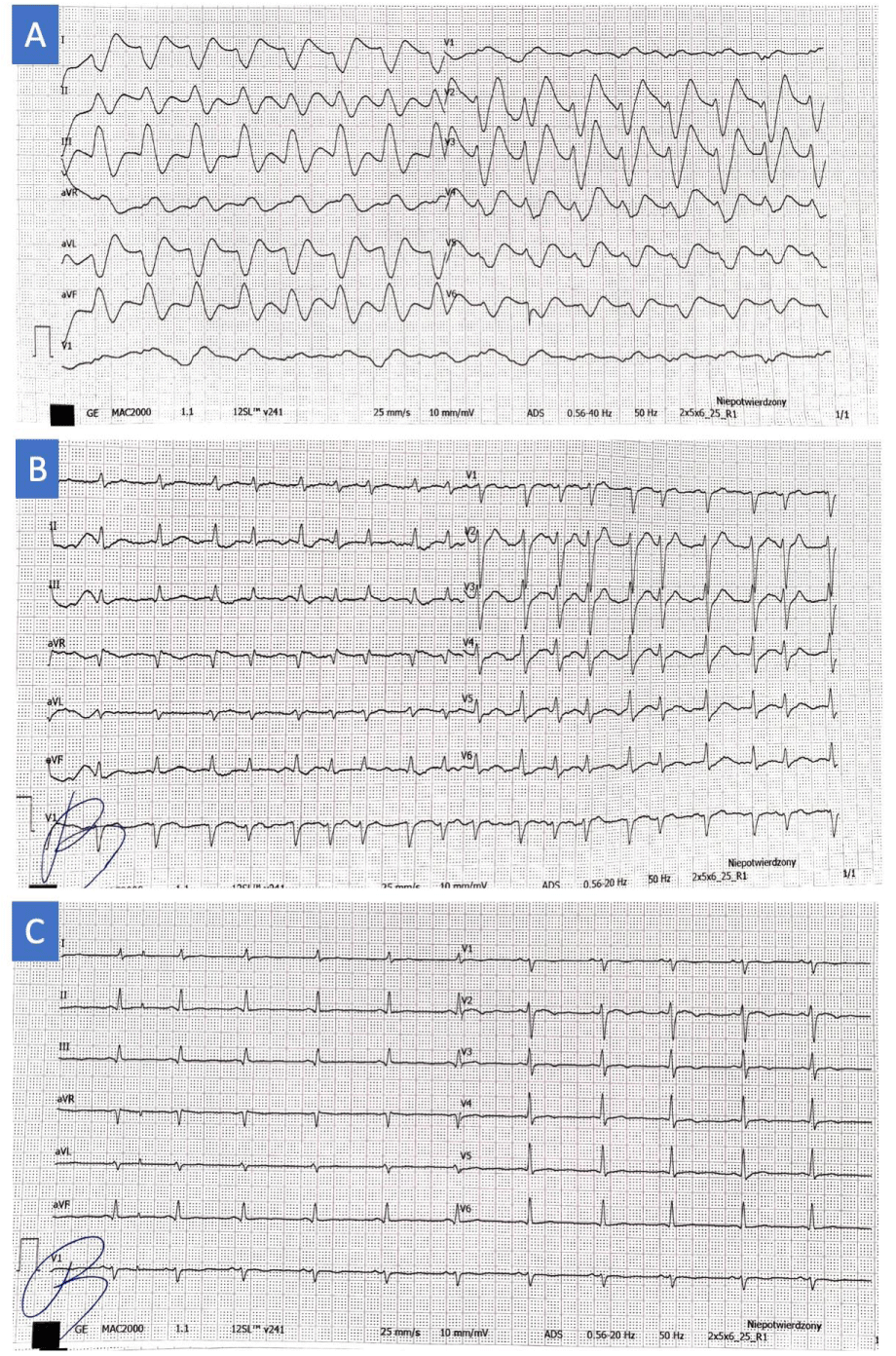
© 2022 Ochijewicz D, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.A 22-year-old woman with a history of bulimia, depression, and one suicidal attempt was admitted to the Emergency Department (ED) after out of hospital cardiac arrest. Her co-workers were proceeding with basic life support with an automated external defibrillator. After the arrival of the emergency service, advanced life support proceeded and ventricular fibrillation was the first rhythm recorded. Return of spontaneous circulation was obtained after defibrillation shock (200 Joules). During transport to the hospital, the patient had another cardiac arrest. Cardiopulmonary resuscitation (CPR) was commenced with The LUCAS 3 device and the patient was intubated and ventilated. In the ED CPR has been continued. Arterial blood gas analysis showed acidosis (pH 7,1), respiratory failure (PO2 29 mmHg, pCO265 mmHg, hypokalemia (3,2 mmol/l), and elevated lactates (7 mmol/l). She was defibrillated three times and received adrenaline, potassium chloride, amiodarone, magnesium sulfate, sodium bicarbonate, and atropine without heart rhythm stabilization. Propofol and ketamine were used for anesthesia prior to intubation. Transthoracic echocardiography (TTE) showed a depressed and desynchronized, ‘vermicular’-like left ventricular contraction pattern and an enlarged right ventricle with systolic dysfunction (Supplementary videos 1,2). During the diagnostic process, she had several cardiac arrests with intermittent episodes of return of spontaneous circulation after defibrillation. The ECG showed monomorphic broad complex tachycardia (Figure 1A) accompanied by a significant peripheral pulse deficit. After a few minutes, she developed bradycardia 30 beats per minute, and hypotension. External and internal electric stimulation was attempted, but the heart rhythm was still not captured. After stabilization, the ECG showed atrial fibrillation (Figure 1B). Toxicological testing of blood and urine detected only atropine and ketamine (administered in the ED) without signs of chronically taken antidepressants (vortioxetine, trazodone) or any other toxins. The following day, TTE showed mildly reduced left ventricular ejection fraction and normal right ventricular size and function. After extubation, she vomited up yew twigs and needles, which she had collected in the forest for weight loss and “suicide attempt by the way”. Before the cardiac arrest, she had visual disturbances. The ECG on the next day showed sinus rhythm with a normal QT interval (Figure 1C). After 10 days the patient was transferred to a psychiatric hospital without neurological deficits.
The yew tree contains a complex mixture of alkaloids, taxane derivatives, and glycosides [1]. Taxines (taxine A and B) cause dose-dependent cardiotoxicity through the blockade of calcium and sodium channels, resulting in pronounced QRS prolongation, ventricular tachycardia, prolonged atrioventricular conduction, and decreased myocardial contractility. Intoxication is known to be resistant to standard treatments with no effective antidote [1]. Minimum lethal doses in humans are reported to range from 0.6 to 1.3 g yew leaves/kg body weight [1]. All parts of the yew are poisonous, except for the red aril of the berries. The biological half-life of taxine metabolites ranges between 11 and 13 h [2]. Data on effective treatment interventions are scarce. Atropine, amiodarone, lidocaine, electrical cardioversion, or external/internal pacing are generally ineffective. Hemodialysis or hemodiafiltration can be considered to improve acid-base balance and stabilize volume overload but not to remove the toxins because of high molecular weights and low water solubility [2-4]. The utility of extracorporeal support for the treatment of acute yew poisonings, as a bridge to recovery, has been shown in patients not responsive to conventional treatments [2].
Intentional yew poisoning can result in life-threatening cardiac toxicity and require aggressive supportive care.
- Labossiere AW, Thompson DF. Clinical Toxicology of Yew Poisoning. Ann Pharmacother. 2018 Jun;52(6):591-599. doi: 10.1177/1060028017754225. Epub 2018 Jan 24. PMID: 29363354.
- Hermes-Laufer J, Meyer M, Rudiger A, Henze J, Enselmann K, Kupferschmidt H, Müller D, Herzog A, Bettex D, Keller DI, Krüger B, Engeler J. Extracorporeal life support as bridge to recovery in yew poisoning: case reports and literature review. ESC Heart Fail. 2021 Feb;8(1):705-709. doi: 10.1002/ehf2.12828. Epub 2020 Nov 24. PMID: 33232574; PMCID: PMC7835583.
- G N, Chan M, Gue YX, Gorog DA. Fatal heart block from intentional yew tree (Taxus baccata) ingestion: a case report. Eur Heart J Case Rep. 2019 Dec 23;4(1):1-4. doi: 10.1093/ehjcr/ytz226. PMID: 32128497; PMCID: PMC7047065.
- Rutkiewicz A, Schab P, Kubicius A, Szeremeta F, Małysz F, Dadok J, Misiewska-Kaczur A. Yew poisoning - pathophysiology, clinical picture, management and perspective of fat emulsion utilization. Anaesthesiol Intensive Ther. 2019;51(5):404-408. doi: 10.5114/ait.2019.89952. PMID: 31769262.

Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
