Journal of Cardiovascular Medicine and Cardiology
A rare form of complex cardiac anomaly
Kritika1, Rajaram Sharma2*, Tapendra Tiwari2 and Saurabh Goyal2
2Assistant Professor, Radio-Diagnosis, Pacific Institute of Medical Sciences (PIMS), Umarda, Udaipur, Rajasthan, India
Cite this as
Kritika, Sharma R, Tiwari T, Goyal S (2022) A rare form of complex cardiac anomaly. J Cardiovasc Med Cardiol 9(3): 014-015. DOI: 10.17352/2455-2976.000179Copyright License
© 2022 Kritika et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Description
Congenital corrected Transposition Of Great Arteries (TGA) is one of the rarest complex cardiac anomalies, comprising 1% of Congenital Heart Disease (CHD) and 20% of cases of fetal TGA [1,2]. It is characterized by an atrioventricular discordance with a concurrent ventricular-arterial discordance. Its features include the aorta, which arises from the left-sided morphologic right ventricle, anterior and left of the pulmonary artery. The pulmonary artery arises from the right-sided morphologic left ventricle and VSD (Ventricular Septal Defect) [3]. The moderator band, the anatomical landmark for the right ventricle, is present on the left side. Associated cardiac defects are also common, including a VSD, pulmonary stenosis or atresia, Atrial Septal Defect (ASD), Double Outlet Right Ventricle (DORV), tricuspid valve anomalies and situs inversus. Our case of a complex cardiac anomaly is nearly related to the congenital incomplete corrected category.
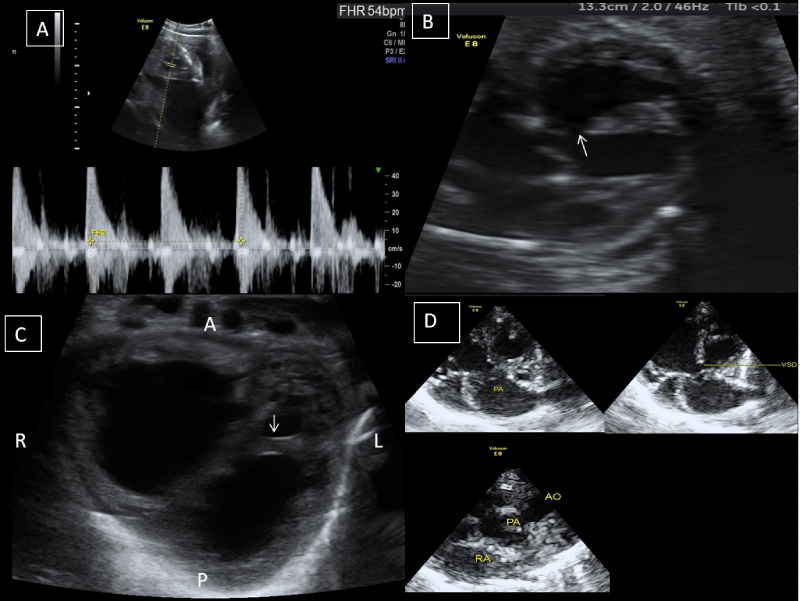
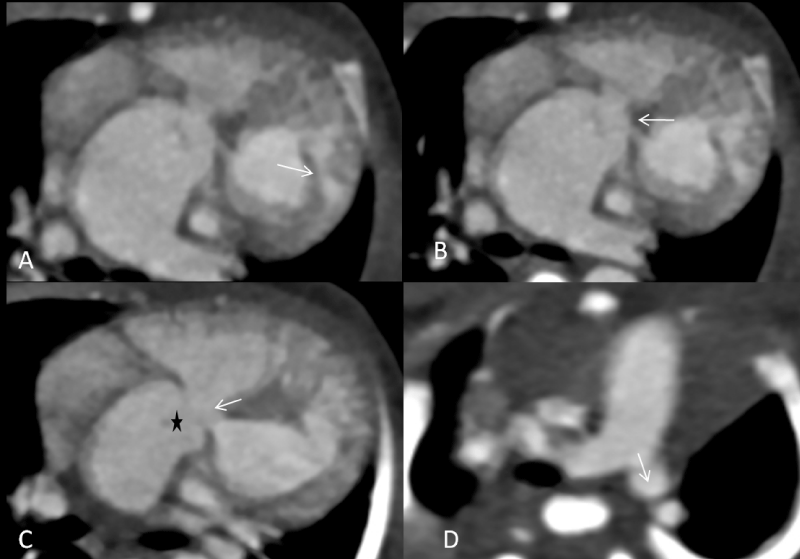
A 21-year-old primigravida female came to our department for her first antenatal ultrasonography, revealing a single live fetus of 27 weeks gestational age with persistent fetal bradycardia (meagre heart rate of 54/minutes) and VSD [Figure 1A & 1B]. There was also a single arterial trunk noted overriding the VSD. Based on the above findings, the possibility of pulmonary atresia/hypoplasia or (Tetralogy of Fallot) TOF was initially suggested. On the follow-up, the baby was born at 35 weeks of gestation with a low birth weight (approximately 2.4 kg). On physical examination, the baby had tachypnea and a low oxygen saturation level. Postnatal echocardiography (echo) was prescribed, revealing a moderator band in the left-sided ventricle; therefore, it was labelled the morphologically right ventricle [Figure 1C]. There was a membranous VSD observed, and a single trunk of the vessel was noted overriding the VSD, which was now somewhat clear that it was a pulmonary artery as the aorta was seen on the left and anterior to the pulmonary artery [Figure 1D]. To confirm the stated findings in echo, cardiac Computed Tomography (CT) scan with contrast was performed. It precisely depicted a visceroatrial situs solitus and anatomical and morphological appropriate atria. The IVC and SVC were draining into the right atrium, which was placed on the right side and the pulmonary veins were draining into the left atrium, which is anatomically placed on the left side. On various reconstructions in the cardiac CT, a moderator band was seen in the morphologically right ventricle. The right and left atrium were intact, which was confirmed by their shape size [Figure 2A]. The pulmonary artery was overriding the VSD (4 mm in dimension) [Figure 2B & 2C]. The aorta was also arising from the morphologic right ventricle, confirmed as neck vessels were arising from it [Figure 2D & Video 1]. A pre ductal coarctation of the aorta was noted along with a patent ductus arteriosis [Video 1]. To summarise all the above findings, our case had atrioventricular discordance and ventricular-arterial discordance with malpositioning of great vessels with ventricles. It was a rare type of complex cardiac anomaly for which corrective surgery was advised however the parents refused it.
Learning points
- Cardiac assessment is an essential component of antenatal ultrasonography for every pregnant female to rule out these anomalies on time.
- In the postnatal period, a cardiac CT scan is the modality of choice to define these anomalies properly and to plan for surgery.
- Tandon A, Bose R, Yoon AD, Schussler JM. Isolated congenitally corrected transposition of the great arteries with dextroversion discovered incidentally in a patient with cocaine-induced acute myocardial infarction. Proc (Bayl Univ Med Cent). 2016 Apr;29(2):171-3. doi: 10.1080/08998280.2016.11929404. PMID: 27034558; PMCID: PMC4790560.
- Kaya A, Tanboga IH, Kurt M, Işik T, Ozgokce M, Topçu S, Aksakal E. Corrected transposition of the great arteries with previously unreported cardiac anomalies. Cardiovasc J Afr. 2012 Jun 12;23(5):e5-7. doi: 10.5830/CVJA-2011-049. PMID: 22732931.
- Chang DS, Barack BM, Lee MH, Lee HY. Congenitally corrected transposition of the great arteries: imaging with 16-MDCT. AJR Am J Roentgenol. 2007 May;188(5):W428-30. doi: 10.2214/AJR.05.0636. PMID: 17449738.

Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
