Journal of Cardiovascular Medicine and Cardiology
Anthropometric indices as predictors of 10-year cardiovascular risk among Sub-Sahara Africans with type 2 diabetes
Azeez TA1* Arinola Esan1, Ayobami Imole Yemitan2, Olumayowa Opeyemi Oluwasanjo3 and Mayowa Babatunde4
2Department of Medicine, College of Medicine, University of Ibadan, Nigeria
3Cardiology Unit, Department of Medicine, University College Hospital, Ibadan, Nigeria
4College of Medicine, University of Ibadan, Nigeria
Cite this as
Azeez TA, Esan A, Yemitan AI, Oluwasanjo OO, Babatunde M (2021) Anthropometric indices as predictors of 10-year cardiovascular risk among Sub-Sahara Africans with type 2 diabetes. J Cardiovasc Med Cardiol 8(4): 072-078. DOI: 10.17352/2455-2976.000174Copyright
© 2021 Azeez TA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Background: Body mass index, waist circumference, waist-hip ratio and waist-height ratio are simple clinical tools for determining obesity. Type 2 diabetes mellitus is often associated with multiple cardiovascular risk factors and increased cardiovascular death. The study was aimed at determining the relationship between these anthropometric indices and 10-year cardiovascular risk among sub-saharan Africans with type 2 diabetes mellitus.
Methods: It was a cross-sectional study involving 67 adults (with 50.7% females) managed for type 2 diabetes mellitus in a referral hospital in Nigeria. Ethical approval was obtained at the institution review board and the participants also gave written consent. Anthropometric indices were determined using standard protocols. Fasting lipid profile, fasting plasma glucose, glycated haemoglobin and plasma creatinine were assayed using standard laboratory techniques. Atherogenic index of plasma, estimated glomerular filtration rate and the WHO-ISH cardiovascular risk score were also determined. Data was analyzed with SPSS version 22. Pearson correlation coefficient, Students’ t test, Chi square test, ROC curve analysis were performed as appropriate.
Results: The mean age was 54.12±9.03 years. Obesity was found in 37.3%, 66.5%, 70.1% and 95.5% of the participants using BMI, WHR, WC and WHtR respectively. Intermediate/high cardiovascular risk was found in 38.2% and 24.2% of the males and females respectively. BMI and WC significantly correlated with blood pressure. There was no significant correlation between anthropometric indices and other cardiovascular risk factors studied. Using ROC curve analysis, BMI and WHtR had the highest AUC of 0.613 and 0.577 respectively.
Conclusion: Among sub-sahara Africans with type 2 diabetes mellitus, there is a significant association between WC and BMI with the blood pressure. BMI and WHtR have the highest 10-year cardiovascular risk predictability among the anthropometric indices in this cohort of individuals. Larger and prospective studies are needed to validate these findings.
Abbreviations
ADA: American Diabetes Association; AIP: Atherogenic Index of Plasma; AUC: Area Under Curve; BMI: Body Mass Index; Cr: Plasma Creatinine; DBP: Diastolic Blood Pressure; eGFR: Estimated Glomerular Filtration Rate; FPG: Fasting Plasma Glucose; HbA1c: Glycated Haemoglobin; HDL-C: High Density Lipoprotein-Cholesterol; LDL-C: Low Density Lipoprotein-Cholesterol; MDRD: Modification of Diet in Renal Disease; ROC: Receiver Operating Characteristics; SBP: Systolic Blood Pressure; TC: Total Cholesterol; TG: Fasting Triglyceride; WC: Waist Circumference; WHO-ISH: World Health Organization-International Society of Hypertension; WHR: Waist-Hip Ratio; WHtR: Weight-Height Ratio
Introduction
Anthropometric measurements and indices are clinically useful in estimating the distribution of fat in the body [1]. They are simple, practical and widely researched clinical tools. The distribution of fat in the body determines the predisposition of an individual to type 2 diabetes mellitus, hypertension, dyslipidaemia and cardiovascular disease [2]. Intra-abdominal fat has the highest cardiometabolic risk [3].
Due to genetic and environmental factors, the body fat architecture of the sub-sahara African population contrasts that of the Western world and Asians [4]. The implication of this inter-racial variance is that the clinical performance of anthropometric measurements in predicting cardiovascular disease might be different in the sub-sahara African populations compared with other parts of the world [3]. This becomes even more relevant as the prevalence of cardiovascular disease in sub-Saharan Africa is unprecedentedly high and continues to rise [5]. The commonly referenced anthropometric measurements and indices include body mass index (BMI), wait circumference (WC), waist-hip-ratio (WHR) and waist-height ratio (WHtR).
Body mass index, otherwise known as Quetelet index, was fist described by Dr. Lambert Adolph Quetelet in the 19th century [6]. The World Health Organization divided BMI into 4 categories – underweight, normal, overweight and obese [7]. So, BMI is widely used in the diagnosis of obesity [8]. Previous studies done among Caucasians and Asians have reported that BMI could predict the occurrence of cardiovascular disease [9,10]. However, there is paucity of such studies in sub-sahara Africa, especially among individuals with type 2 diabetes mellitus. Although BMI is the most commonly used anthropometric measurement to indicate obesity in epidemiological studies, available evidence is however pointing towards the better performance of other measures of adiposity such as waist circumference and waist-height-ratio in predicting cardiovascular disease [11,12].
Waist circumference is a perimetric measurement of the body girth at the abdominal level [13]. Studies have shown that waist circumference (WC) is better correlated with intra-peritoneal adiposity assessed with magnetic resonance imaging when compared with waist-to-hip ratio and BMI [14,15]. Other advantages that waist circumference has include simplicity of measurement, reduced error tendency and absence of additional calculations following measurement [16]. WC also has high reproducibility [13]. Despite all these advantages, it has been observed that WC is not commonly measured in clinical practice [17]. Researches involving populations outside of Africa have also shown that waist circumference could predict cardiovascular disease [8,13,18].
Waist-hip ratio (WHR) inculcates hip circumference as well as waist circumference to its formula and this makes it superior to other measures of adiposity [19]. This is because waist circumference measures central adiposity while hip circumference measures peripheral adiposity and this makes the WHR a complete indicator of an individual’s adipose tissue distribution. In fact, a landmark multicentric study, INTERHEART study, reported that among the common anthropometric indices, WHR was the best predictor of myocardial infarction [20]. In a large prospective study involving patients with type 2 diabetes, Czernichow, et al. concluded that WHR was superior to WC and BMI in predicting cardiovascular events and mortality in patients with type 2 diabetes mellitus [21].
Waist-to-height ratio (WHtR) is a simplified anthropometric index that has been associated with metabolic risk factors such as glucose intolerance [22]. It is an alternative indicator of abdominal adiposity. A study has suggested that WHtR is better than WC, WHR and BMI because its cut-off value is independent of ethnicity (unlike BMI) or gender (unlike WC and WHR) [23]. On this basis, it has been posited that WHtR could be more useful clinically as a screening tool irrespective of location. Studies done outside sub-sahara Africa have shown that WHtR is a reliable indicator of cardiovascular risk [11,24].
Cardiovascular disease is now the top-ranking cause of deaths worldwide [25]. This is probably due to the rising prevalence of traditional risk factors for cardiovascular disease such as hypertension, diabetes, dyslipidaemia, sedentary lifestyle and obesity [26,27]. Interestingly, in individuals living with type 2 diabetes, it is rather common to see a clustering of these traditional risk factors in the same person, a condition referred to as the metabolic syndrome [28]. Apart from these traditional risk factors, atherogenic index of plasma (AIP) is a composite index that has been richly validated and associated with 10-year cardiovascular risk among sub-sahara Africans living with type 2 diabetes mellitus [29]. Similarly, plasma creatinine has been associated with increased risk of coronary heart disease and cardiovascular death [30].
There are several documented cardiovascular risk calculators. However, most of these cardiovascular risk calculators have not been validated among sub-sahara Africans. Nevertheless, the World Health Organization- International Society of Hypertension (WHO-ISH) cardiovascular risk prediction charts for fatal and non-fatal cardiovascular disease stand out in this regards because some of the charts are specifically designed for sub-sahara Africans, with or without diabetes mellitus [31,32]. Some published works from the sub-region have actually used the WHO-ISH risk chart to predict the risk of having fatal and non-fatal cardiovascular disease [31,33,34].
Objectives of the study
The study was aimed at determining the association between anthropometric indices and cardiovascular risk factors as well as AIP. Also, it was done to demonstrate if anthropometric indices could predict the 10-year cardiovascular risk among sub-saran Africans with type 2 diabetes mellitus.
Methods
The study was a cross-sectional design involving 67 adults who were 40 years and above. The sample size was based on the availability of participants and limitation of resources. They were all previously diagnosed with type 2 diabetes mellitus. They were all attending a specialist diabetes clinic of a major referral hospital in southern Nigeria. Systematic random sampling was adopted in recruiting eligible participants. Inclusion criterion was adults (40 years and above) previously diagnosed with type 2 diabetes mellitus. Type 1 diabetes mellitus, previous diagnosis of cardiovascular disease (stroke, transient ischaemic attack, coronary heart disease and peripheral vascular disease), pregnancy, recent (within the preceding 3 months) hospital admission and metabolic decompensation were exclusion criteria. Ethical approval was obtained from the institution review board. The reference number of the review board was NHREC/05/01/2008a. The approval number was UI/EC/17/0284. Only individuals who gave a written consent for participation and publication were recruited into the study.
After instructing the participants to empty their pockets and remove their shoes (and soxes) as well as caps (or head gears), weight and height were measured using a D-339 Detecto Eye-level Physician Beam Scale (made in the USA) and a stadiometer respectively. Waist circumference was measured using a standard technique, as described by the WHO in the technical report on obesity, with a flexible inelastic tape measure [35]. It was measured across the abdomen at the midpoint between the inferior margin of the last rib and the iliac crest. WC greater than 94 cm in men or greater than 80 cm in women was considered as truncal obesity [36]. Hip circumference was also measured with a flexible inelastic tape measure. BMI, WHR and WHtR were determined using the formulae below.
Body mass index (BMI) = Weight (Kg)/Height (m2)
Waist-hip ratio (WHR) = Waist circumference (cm)/hip circumference (cm)
Waist-to-height ratio (WHtR) = waist circumference (cm)/height (cm)
WHR >0.9 in men and >0.85 in women were taken as truncal or abdominal obesity [37]. BMI greater than or eqaal to 30.0 kg/m2 was considered as obesity [18]. WHtR greater than 0.5 was regarded as abnormal [37].
Blood pressure was measured using a mercury sphygmomanometer (Accoson brand, made in England). This was done after the patient had sit for about 5 minutes and a standard technique, as described by the European Society of Hypertension, was strictly adhered to [38]. Blood pressure consisted of systolic blood pressure (SBP) and diastolic blood pressure (DBP).
The participants were instructed to fast overnight for 8 – 12 hours and present the following morning. Blood sample for fasting plasma glucose (FPG), fasting lipid profile, glycated haemoglobin (HbA1c) and plasma creatinine were obtained. Landwind C100plus AutoChemistry Analyzer (Accurex Biomedical, Mumbai, India) was employed in assaying FPG, FLP parameters and plasma creatinine (Cr) using the appropriate enzymatic methods. Automated glycohaemoglobin analyzer (Bio-Rad 220-0212, Hercules, California, USA) was employed in assaying HbA1c by using the high performance liquid chromatography method. Atherogenic index of plasma was determined by the formula below.
Estimated glomerular filtration rate (eGFR) was obtained by using the Modification of Diet in Renal Disease (MDRD) formula [39]. The formula is given below.
eGFR = 175 X (Cr)-1.154 X (Age)-0.203 X 0.742 (if female) X 1.212 (if black)
The 10-year risk of cardiovascular diseases (fatal or nonfatal stroke and myocardial infarction) was estimated with the World Health Organization-International Society of Hypertension (WHO-ISH) cardiovascular risk charts designed to be used in Africa, sub-region D (AFR D) [40]. Risk score below 10 was considered low while risk score greater than or equal to 10 was considered intermediate/high [31].
Data was checked for completeness and accuracy before analysis was done. Statistical Package for Social Sciences (SPSS) version 22 was used in performing the statistical analysis. Continuous variables were expressed as mean ± standard deviation. Nominal variables were expressed as frequencies and percentages. The difference in means of anthropometric indices across the gender was determined with the independent sample Student’s t test. Association between continuous variables was determined with Pearson’s correlation. The association between WHO-ISH risk category and gender was determined using Pearson’s chi square test. Receiver operating characteristics (ROC) curve for each anthropometric index was plotted using WHO-ISH risk score dichotomous categories of low and intermediate/high. The area under curve (AUC) of each index was also determined. p value of less than 0.05 was considered to be statistically significant.
Results
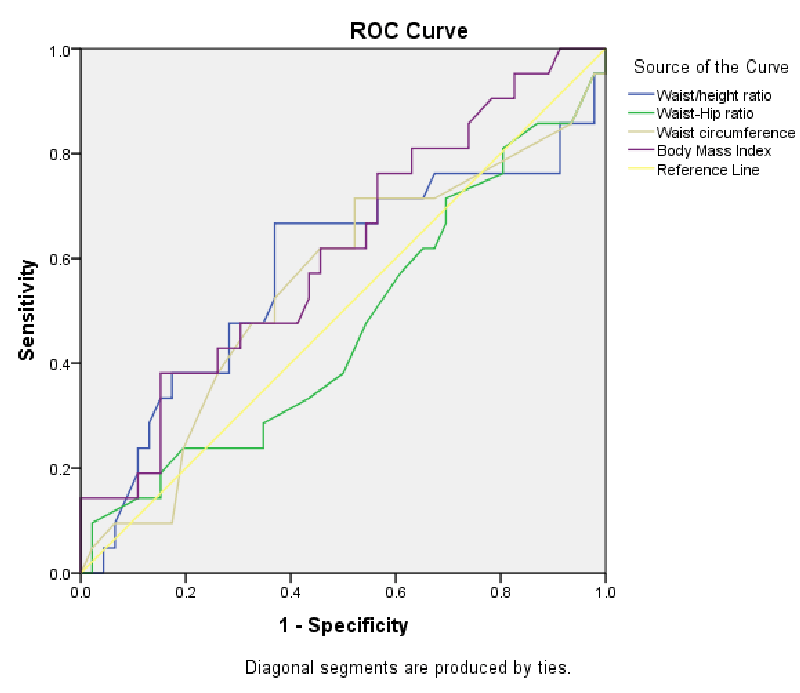
The study involved 67 adults. The mean age was 54.12±9.03 years. Females constituted 50.7% of the participants. Table 1 shows the anthropometric and clinical characteristics of the participants. The BMI was significantly higher in females while WC and WHR were significantly higher in males. Interestingly, there was no significant difference in the WHtR of males and females. Table 2 shows the laboratory characteristics of the participants. Figure 1 shows the WHO-ISH cardiovascular risk of the participants by compaing that of males with females. The proportion of participants with intermediate/high 10-year cardiovascular risk score was higher among males but the difference did not attain statistical significance (p=0.217). Figure 2 shows the frequency of overweight/obesity using the various anthropometric indices. Table 3 shows the correlation between anthropometric indices and cardiovascular risk factors. Among the cardiovascular risk factors studied, it was only the blood pressure that significantly correlated with some of the indices. There was a statistically significant positive correlation between BMI and SBP (r=0.441;p < 0.0001), BMI and DBP (r=0.314; p=0.010) as well as WC and DBP (r=0.246;p=0.044). Figure 3 shows the ROC curve to determine the ability of the anthropometric indices to predict 10 year cardiovascular risk of people living with type 2 diabetes mellitus. Table 4 shows the area under curve (AUC) of each index. BMI has the highest AUC, followed by WHtR.
Discussion
The average age of the participants was 54 years which suggests that they were mostly middle-aged. The average duration of diabetes was 6 years. This is consistent with the observation that diabetes mellitus is being increasingly diagnosed at middle age or even earlier in developing nations [41,42]. This implies that these individuals have a longer period of their lives potentially exposed to the adverse cardiometabolic milieu peculiar to type 2 diabetes mellitus. Therefore, an opportunity to be able to predict the risk of developing cardiovascular disease in these individuals with type 2 diabetes should be of clinical priority.
The mean FPG (6.35±0.88 mmol/L) and HbA1c (7.00±0.73%) of the participants are within acceptable limits, going by the ADA targets of care in type 2 diabetes mellitus [43]. In addition, their eGFR and average lipid profiles are largely within normal limit. These participants were attending a major referral hospital where they had the opportunity of seeing Endocrinologists, professional dieticians, licensed diabetes care educators and other supportive care providers. It may therefore be explained that the degree of expertise care they are exposed to have made a remarkable impact in their care. Previous studies have also reported that glucose control is remarkably improved when patients are exposed to multidisciplinary care [44,45]. This may however not reflect the glucose control patterns of the vast majority of type 2 diabetes patients who do not receive care at a specialist health facility therefore biasing the findings of this study.
BMI (Kg/m2) was significantly higher among females (25.40±2.35 vs 23.92±2.10; p=0.008). Previous studies have also documented a higher BMI among females [46,47]. Studies have shown that women have more body fat than men and oestrogen has been suggested to be the driver of efficient fat storage in women [48,49]. However, in terms of fat distribution, men had significantly higher truncal obesity which was reflected in their higher WC (94.97±4.77 cm Vs 90.85±7.09 cm; p=0.007) and WHR (0.99±0.008 Vs 0.94±0.008; p=0.016). This suggests that truncal distribution of adiposity was higher among males. This is unsurprising because previous studies have also corroborated this observation by reporting a higher prevalence of abdominal obesity (giving a centripetal or apple-shaped distribution) among males [49,50]. Interestingly, the WHtR was not remarkably different across the genders (p=0.996). WHtR has been documented to be similar in males and females such that a singular cut-off value is often applied to both genders in diagnosing truncal obesity [51].
The indices of truncal obesity (WHR, WC and WHtR) identified more participants with obesity (66.5%, 70.1% and 95.5% respectively) than BMI could identify. Type 2 diabetes is more associated with truncal obesity and this may explain the higher prevalence of truncal obesity in these participants. It was observed that while the frequency of truncal obesity identified with WC and WHR were comparable (66.5% vs 70.1%), that of WHtR was significantly more (95.5%). Some earlier studies had suggested that using a cut-off point of 0.5 for WHtR may not be suitable for African blacks and the one-size fits all approach needs to be reviewed [52,53].
This study also showed a higher proportion of males with intermediate-to-high cardiovascular risk compared with females (38.2% vs 24.2%). This is not unsurprising because previous studies have also alluded to the fact that men tend to have a higher cardiovascular risk compared to women. The female sex hormones and lower prevalence of harmful lifestyles have been proposed to be responsible for the gender differences in cardiovascular risk [54,55].
Among the cardiovascular risk factors studied, only blood pressure had significant correlation with BMI and WC. BMI had a statistically significant correlation with DBP (r=0.314; p=0.010) and SBP (r=0.441; p< 0.0001). Also, WC had a statistically significant correlation with DBP (r=0.246; p=0.044). It must however be stated that for each of the significant correlation, the strength of the association was not strong. Several studies have also reported a significant association between blood pressure and BMI [56–58]. This observation has informed the principle of losing weight as a lifestyle approach to lowering blood pressure [59]. Insulin resistance, altered renin-angiotensin-aldosterone system and increased sympathetic tone are some of the proposed mechanisms linking BMI with blood pressure [57]. In the same vein, waist circumference has been associated with blood pressure in a previous study [60].
In the ROC curve analysis, BMI had the highest AUC, WHR had the lowest AUC and WC as well as WHtR AUCs were in the middle. This suggests that BMI has the highest ability to predict 10 year cardiovascular risk among sub-sahara Africans with type 2 diabetes mellitus when compared with other anthropometric indices of obesity. This is closely followed by WHtR and WC. However, WHR may not be a preferred predictor of 10 year cardiovascular risk in type 2 diabetes, going by the results of the study. Although Czernichow, et al. had suggested that the indices of abdominal obesity (WC, WHR and WHtR) were better predictors of cardiovascular disease among the British compaed with the BMI, Huxler et al, who did an extensive review across ethnic groups, concluded that the results of studies comparing BMI with WC, WHR and WHtR as a predictor of cardiovascular disease were inconsistent.
Moreover, previous studies have suggested that the cut-off points for these indices of abdominal obesity may not be appropriate for African blacks and this may affect their clinical performance in such clinical scenarios [52,53,61]. Most of the studies through which the cut-off values of WC, WHR and WHtR were fixed, got carried out among Caucasians and the results may not be directly applicable to African blacks [61].
Limitations
A bigger sample size might yield a clearer outcome. Similarly, a prospective, community-based study might give a more reliable result.
Recommendations on future study
A case-control study with a higher sample size would be a better approach. It would also be more interesting and to analyze exclusively the association of anthropometrics and diabetes by different methods (ROC curves, DE etc.) after removing bias.
Conclusion
BMI and WC significantly correlate with blood pressure among sub-saharan Africans with type 2 diabetes mellitus. BMI, WHtR and WC could be used as predictors of 10-year cardiovascular risk among sub-sahara Africans with type 2 diabetes but a larger and prospectively designed study would be needed to support this observation.
Declarations
Ethical approval and consent to participate: Ethical approval was granted by the ethical committee of the Institute Advanced Medical Research and Training with the reference number NHREC/05/01/2008a. The ethical approval number for the study was UI/EC/17/0284. Also, the recruited participants gave written informed consent to partake in the study.
- Woldegebriel AG, Fenta KA, Aregay AB, Aregay AD, Mamo NB, et al. (2020) Effectiveness of Anthropometric Measurements for Identifying Diabetes and Prediabetes among Civil Servants in a Regional City of Northern Ethiopia: A Cross-Sectional Study. J Nutr Metab 2020: e8425912. Link: https://bit.ly/3oqfqyI
- Jensen MD (2008) Role of Body Fat Distribution and the Metabolic Complications of Obesity. J Clin Endocrinol Metab 93: S57–S63. Link: https://bit.ly/3H9KX0B
- Haregu TN, Oti S, Egondi T, Kyobutungi C (2016) Measurement of overweight and obesity an urban slum setting in sub-Saharan Africa: a comparison of four anthropometric indices. BMC Obes 3: 46. Link: https://bit.ly/3FbupmS
- Ettarh R, Van de Vijver S, Oti S, Kyobutungi C (2013) Overweight, Obesity, and Perception of Body Image Among Slum Residents in Nairobi, Kenya, 2008–2009. Prev Chronic Dis [Internet] 10. Link: https://bit.ly/3kxcsax
- Yuyun MF, Sliwa K, Kengne AP, Mocumbi AO, Bukhman G (2020) Cardiovascular Diseases in Sub-Saharan Africa Compared to High-Income Countries: An Epidemiological Perspective. Global Heart 15: 15. Link: https://bit.ly/3ogdZ60
- Nuttall FQ (2015) Body Mass Index. Nutr Today 50: 117–28. Link: https://bit.ly/31ULwLA
- Mohammadifard N, Nazem M, Sarrafzadegan N, Nouri F, Sajjadi F, et al. (2013) Body Mass Index, Waist-circumference and Cardiovascular Disease Risk Factors in Iranian Adults: Isfahan Healthy Heart Program. J Health Popul Nutr. 31: 388–397. Link: https://bit.ly/3Ce4k4F
- Tran NTT, Blizzard CL, Luong KN, Truong NLV, Tran BQ, et al. (2018) The importance of waist circumference and body mass index in cross-sectional relationships with risk of cardiovascular disease in Vietnam. PLOS ONE 13: e0198202. Link: https://bit.ly/3Cad5N6
- Huxley R, Mendis S, Zheleznyakov E, Reddy S, Chan J (2010) Body mass index, waist circumference and waist:hip ratio as predictors of cardiovascular risk—a review of the literature. Eur J Clin Nutr 64: 16–22. Link: https://bit.ly/30fcSLF
- Asia Pacific Cohort Studies Collaboration (2004) Body mass index and cardiovascular disease in the Asia-Pacific Region: an overview of 33 cohorts involving 310 000 participants. International Journal of Epidemiology 33: 751–758.
- Ashwell M, Hsieh SD (2005) Six reasons why the waist-to-height ratio is a rapid and effective global indicator for health risks of obesity and how its use could simplify the international public health message on obesity. Int J Food Sci Nutr. 56: 303–307. Link: https://bit.ly/3kxegQR
- Welborn TA, Dhaliwal SS (2007) Preferred clinical measures of central obesity for predicting mortality. Eur J Clin Nutr. 61: 1373–1379. Link: https://bit.ly/3oql7fY
- Klein S, Allison DB, Heymsfield SB, Kelley DE, Leibel RL, et al. (2007) Waist Circumference and Cardiometabolic Risk: A Consensus Statement from Shaping America’s Health: Association for Weight Management and Obesity Prevention; NAASO, The Obesity Society; the American Society for Nutrition; and the American Diabetes Association. Am J Clin Nutr 85: 1197-1202. Link: https://bit.ly/3c33a1o
- Chan DC, Watts GF, Barrett PHR, Burke V (2003) Waist circumference, waist-to-hip ratio and body mass index as predictors of adipose tissue compartments in men. QJM 96: 441–447. Link: https://bit.ly/3ClCRyp
- Janssen I, Heymsfield SB, Allison DB, Kotler DP, Ross R (2002) Body mass index and waist circumference independently contribute to the prediction of nonabdominal, abdominal subcutaneous, and visceral fat. Am J Clin Nutr Apr 75: 683–688. Link: https://bit.ly/2YF54SV
- Siren R, Eriksson JG, Vanhanen H (2012) Waist circumference a good indicator of future risk for type 2 diabetes and cardiovascular disease. BMC Public Health 12: 631. Link: https://bit.ly/3olPF2K
- Ross R, Neeland IJ, Yamashita S, Shai I, Seidell J, et al. (2020) Waist circumference as a vital sign in clinical practice: a Consensus Statement from the IAS and ICCR Working Group on Visceral Obesity. Nat Rev Endocrinol 16: 177–189. Link: https://bit.ly/3qwuVrF
- Adegbija O, Hoy WE, Dong B, Wang Z (2017) Body mass index and waist circumference as predictors of all-cause mortality in an Aboriginal Australian community. Obes Res Clin Pract 11: 19–26. Link: https://bit.ly/3c7fc9W
- Cao Q, Yu S, Xiong W, Li Y, Li H, et al. (2018) Waist-hip ratio as a predictor of myocardial infarction risk: A systematic review and meta-analysis. Medicine 97: e11639. Link: https://bit.ly/3D58wVP
- Yusuf S, Hawken S, Ôunpuu S, Bautista L, Franzosi MG, et al. (2005) Obesity and the risk of myocardial infarction in 27 000 participants from 52 countries: a case-control study. Lancet 366: 1640–1649. Link: https://bit.ly/3ky2VQz
- Czernichow S, Kengne A-P, Huxley RR, Batty GD, de Galan B, et al. (2011) Comparison of waist-to-hip ratio and other obesity indices as predictors of cardiovascular disease risk in people with type 2 diabetes: a prospective cohort study from ADVANCE. Eur J Cardiovasc Prev Rehabil 18: 312–319. Link: https://bit.ly/2YF65ud
- Son YJ, Kim J, Park H-J, Park SE, Park C-Y, et al. (2016) Association of Waist-Height Ratio with Diabetes Risk: A 4-Year Longitudinal Retrospective Study. Endocrinol Metab (Seoul) 31: 127–133. Link: https://bit.ly/3F7G1r8
- Browning LM, Hsieh SD, Ashwell M (2010) A systematic review of waist-to-height ratio as a screening tool for the prediction of cardiovascular disease and diabetes: 0·5 could be a suitable global boundary value. Nutr Res Rev 23: 247–269. Link: https://bit.ly/2YHOOAA
- Peng Y, Li W, Wang Y, Bo J, Chen H (2015) The Cut-Off Point and Boundary Values of Waist-to-Height Ratio as an Indicator for Cardiovascular Risk Factors in Chinese Adults from the PURE Study. PLOS ONE 10: e0144539. Link: https://bit.ly/3H9Pz6V
- Mc Namara K, Alzubaidi H, Jackson JK (2019) Cardiovascular disease as a leading cause of death: how are pharmacists getting involved? Integr Pharm Res Pract 8:1–11. Link: https://bit.ly/30c9y3M
- Hamid S, Groot W, Pavlova M (2019) Trends in cardiovascular diseases and associated risks in sub-Saharan Africa: a review of the evidence for Ghana, Nigeria, South Africa, Sudan and Tanzania. Aging Male 22: 169–176. Link: https://bit.ly/3oqkP8Y
- Petrie JR, Guzik TJ, Touyz RM (2018) Diabetes, Hypertension, and Cardiovascular Disease: Clinical Insights and Vascular Mechanisms. Can J Cardiol 34: 575–584. Link: https://bit.ly/3HfvAnq
- Regufe VMG, Pinto CMCB, Perez PMVHC (2020) Metabolic syndrome in type 2 diabetic patients: a review of current evidence. Porto Biomed J 5: e101. Link: https://bit.ly/3omEUgt
- Azeez TA (2021) Association between lipid indices and 10-year cardiovascular risk of a cohort of black Africans living with type 2 diabetes mellitus. Journal of Advances in Internal Medicine 10: 38–42. Link: https://bit.ly/3HgF819
- Sibilitz KL, Benn M, Nordestgaard BG (2014) Creatinine, eGFR and association with myocardial infarction, ischemic heart disease and early death in the general population. Atherosclerosis 237: 67–75. Link: https://bit.ly/30aoW0x
- Babatunde OA, Olarewaju SO, Adeomi AA, Akande JO, Bashorun A, et al. (2020) 10-year risk for cardiovascular diseases using WHO prediction chart: findings from the civil servants in South-western Nigeria. BMC Cardiovasc Disord 20: 154. Link: https://bit.ly/3n7V0Ly
- Pedro JM, Brito M, Barros H (2018) Cardiovascular Risk Assessment in Angolan Adults: A Descriptive Analysis from CardioBengo, a Community-Based Survey. Int J Hypertens e2532345. Link: https://bit.ly/3H9Rkkx
- Adje DU, Oparah AC, Megbolu T (2020) Cardiovascular risk assessment in Community Pharmacies in Warri, Nigeria. Journal of Pharmacy & Bioresources 17: 105–111. Link: https://bit.ly/3oh5rMa
- Edward AO, Oladayo AA, Omolola AS, Adetiloye AA, Adedayo PA (2013) Prevalence of traditional cardiovascular risk factors and evaluation of cardiovascular risk using three risk equations in Nigerians living with human immunodeficiency virus. N Am J Med Sci 5: 680-688. Link: https://bit.ly/3ooYFnK
- Anurhada R, Hemacnandran S, Ruma D (2012) The Waist Circumference Measurement: A Simple Method for Assessing the Abdominal Obesity. J Clin Diagn Res 6: 1510–1513. Link: https://bit.ly/3qLbBar
- Gierach M, Gierach J, Ewertowska M, Arndt A, Junik R (2014) Correlation between Body Mass Index and Waist Circumference in Patients with Metabolic Syndrome. ISRN Endocrinol. Link: https://bit.ly/3wD7s9k
- World Health Organization (2011) Waist circumference and waist-hip ratio: report of a WHO expert consultation, Geneva, 8-11 December 2008. Geneva: World Health Organization. Link: https://bit.ly/3oqnpfa
- Stergiou GS, Palatini P, Parati G, O’Brien E, Januszewicz A, et al. (2021) European Society of Hypertension practice guidelines for office and out-of-office blood pressure measurement. J Hypertens 39: 1293-1302. Link: https://bit.ly/3Fb3wiY
- Kumar BV, Mohan T (2017) Retrospective Comparison of Estimated GFR using 2006 MDRD, 2009 CKD-EPI and Cockcroft-Gault with 24 Hour Urine Creatinine Clearance. J Clin Diagn Res 11: BC09-BC12. Link: https://bit.ly/3F7THT1
- WHO. Cardiovascular diseases [Internet]. [cited 2021 May 7].
- Olokoba AB, Obateru OA, Olokoba LB (2012) Type 2 Diabetes Mellitus: A Review of Current Trends. Oman Med J 27: 269–273. Link: https://bit.ly/3or6lWF
- Balogun WO, Onasanya AS, Azeez TA (2020) Prevalence and clinical characteristics of Nigerian patients with early-onset Type 2 diabetes. Nigerian Journal of Medicine 29: 49–54. Link: https://bit.ly/3CalJv2
- Association AD (2021) 2. Classification and Diagnosis of Diabetes: Standards of Medical Care in Diabetes—2021. Diabetes Care 44: S15–S33. Link: https://bit.ly/3kvk7X7
- Zwar N, Hasan I, Hermiz O, Vagholkar S, Comino E, et al. (2008) Multidisciplinary care plans and diabetes--benefits for patients with poor glycaemic control. Aust Fam Physician 37: 960–962. Link: https://bit.ly/3C4N6qp
- Tourkmani AM, Abdelhay O, Alkhashan HI, Alaboud AF, Bakhit A, et al. (2018) Impact of an integrated care program on glycemic control and cardiovascular risk factors in patients with type 2 diabetes in Saudi Arabia: an interventional parallel-group controlled study. BMC Fam Pract. Link: https://bit.ly/3C7lqkP
- Tauqeer Z, Gomez G, Stanford FC (2018) Obesity in Women: Insights for the Clinician. J Womens Health (Larchmt) 27: 444–457. Link: https://bit.ly/3FfDNpT
- Garawi F, Devries K, Thorogood N, Uauy R (2014) Global differences between women and men in the prevalence of obesity: is there an association with gender inequality? Eur J Clin Nutr 68: 1101–1106. Link: https://bit.ly/30h2bsn
- Karastergiou K, Smith SR, Greenberg AS, Fried SK (2012) Sex differences in human adipose tissues – the biology of pear shape. Biol Sex Differ 3: 13. Link: https://bit.ly/3om53w3
- Jackson AS, Stanforth PR, Gagnon J, Rankinen T, Leon AS, et al. (2002) The effect of sex, age and race on estimating percentage body fat from body mass index: The Heritage Family Study. Int J Obes Relat Metab Disord 26: 789–796. Link: https://bit.ly/3Da7cBd
- Kim K-B, Shin Y-A (2020) Males with Obesity and Overweight. J Obes Metab Syndr 29: 18–25. Link: https://bit.ly/3qBIxC9
- Alshamiri MQ, Mohd A Habbab F, AL-Qahtani SS, Alghalayini KA, Al-Qattan OM, et al. (2020) Waist-to-Height Ratio (WHtR) in Predicting Coronary Artery Disease Compared to Body Mass Index and Waist Circumference in a Single Center from Saudi Arabia. Cardiol Res Pract. Link: https://bit.ly/3wGtlUY
- Mabchour AE, Delisle H, Vilgrain C, Larco P, Sodjinou R,et al. (2015) Specific cut-off points for waist circumference and waist-to-height ratio as predictors of cardiometabolic risk in Black subjects: a cross-sectional study in Benin and Haiti. Diabetes Metab Syndr Obes 8: 513–523. Link: https://bit.ly/3om7bUz
- Matsha TE, Kengne A-P, Yako YY, Hon GM, Hassan MS, et al. (2013) Optimal Waist-to-Height Ratio Values for Cardiometabolic Risk Screening in an Ethnically Diverse Sample of South African Urban and Rural School Boys and Girls. PLOS ONE 8: e71133. Link: https://bit.ly/3quRjBG
- Wakabayashi I (2017) Gender differences in cardiovascular risk factors in patients with coronary artery disease and those with type 2 diabetes. J Thorac Dis 9: E503–E506. Link: https://bit.ly/3okgZyo
- Bots SH, Peters SAE, Woodward M (2017) Sex differences in coronary heart disease and stroke mortality: a global assessment of the effect of ageing between 1980 and 2010. BMJ Global Health 2: e000298. Link: https://bit.ly/3n8o99v
- Shuger SL, Sui X, Church TS, Meriwether RA, Blair SN (2008) Body mass index as a predictor of hypertension incidence among initially healthy normotensive women. Am J Hypertens 21: 613–619. Link: https://bit.ly/3DcpDVB
- Gelber RP, Gaziano JM, Manson JE, Buring JE, Sesso HD (2007) A prospective study of body mass index and the risk of developing hypertension in men. Am J Hypertens 20: 370–377. Link: https://bit.ly/3HipJ0D
- Drøyvold WB, Midthjell K, Nilsen TIL, Holmen J (2005) Change in body mass index and its impact on blood pressure: a prospective population study. Int J Obes (Lond) 29: 650–655. Link: https://bit.ly/3Caq1Ta
- Harsha DW, Bray GA (2008) Weight Loss and Blood Pressure Control (Pro). Hypertension 51: 1420–1425. Link: https://bit.ly/3c5q6x3
- Andeansah M, Afiatin M, Sukandar H (2015) Correlation between Waist Circumference and Hypertension in Jatinangor. Journal of Hypertension 33: e14. Link: https://bit.ly/3Ce0bxM
- Okafor CI, Raimi TH, Gezawa ID, Sabir AA, Enang O, et al. (2016) Performance of waist circumference and proposed cutoff levels for defining overweight and obesity in Nigerians. Ann Afr Med 15: 185–193. Link: https://bit.ly/3wMef0n

Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.
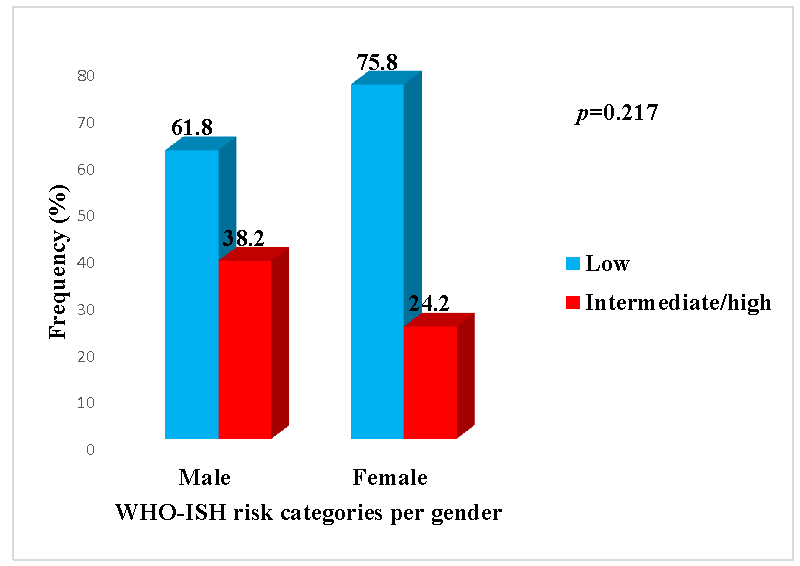

 Save to Mendeley
Save to Mendeley
