Journal of Cardiovascular Medicine and Cardiology
Novel use of contegra valved conduits in idiopathic bilateral brachiocephalic vein stenosis
Suraj Wasudeo Nagre1*and Krishnarao Narayanrao Bhosle2
2Ex Professor and Head of CVTS, Grant Medical College, Mumbai, India
Cite this as
Nagre SW, Bhosle KN (2021) Novel use of contegra valved conduits in idiopathic bilateral brachiocephalic vein stenosis. J Cardiovasc Med Cardiol 8(2): 038-040. DOI: 10.17352/2455-2976.000167Thromboses of the upper limp and neck veins are rare in comparison with those of the lower extremities. Innominate Vein Thrombosis (IVT) is an elusive vascular disease that is rarely seen, with potentially lethal complications such as sepsis and pulmonary embolism. It is usually secondary to intravenous drug abuse, prolonged central venous catheterization or deep head-neck infections or trauma. The history and examination in patients with an IVT may be vague and misleading. Patients may present with a painful swelling of the neck but they may also be absolutely asymptomatic.
Initial medical treatment of the patients includes thrombolytic, anticoagulant and steroid drug therapies. If the patient’s symptoms do not improve with medication, surgical or endovascular interventions are performed. The indications for open, surgical revascularization are rare and usually reserved for patients whose symptoms are refractory to anticoagulation and endovascular treatment.
We report successful decompression of severe venous hypertension of head, neck, face and bilateral upper limb of a 39 year old male patient having symptoms such as facial, neck and bilateral shoulder intermittent edema, occasional dyspnea, chest pain, and headache since 1 year. CT Venography s/o bilateral brachiocephalic vein [Innominate vein] and left subclavin vein stenosis. After all investigations for searching cause of thrombosis all reports normal, nothing found so we called it as idiopathic. We used two contegra valved bovine conduits. Proximal end of the first contegra valve conduit was anastamosed to right distal IJV and distal end to the SVC. The another contegra graft’s proximal end was anastamosed to the left distal IJV and distal end to the first contegra graft distal to its valve. It provided promt and effective venous outflow, with complete resolution of the venous engorgement over the face and upper limb, and also a patent graft six months postoperatively.
Introduction
Thrombosis of the upper limb and neck are rare in comparison with those of the lower extremities. Innominate and Internal Jugular Vein Thrombosis (IJVT) is an exclusive vascular disease that is rarely seen, with potentially lethal complications such as sepsis and pulmonary embolism. Hereditary and acquired conditions predispose to thrombotic phenomena [1]. IJVT is rarely spontaneous, which means there is no apparent predisposing factor for thrombosis (Unsal, et al. 2003) [2]. We report a case of successful decompression of severe venous hypertension of head, neck, face and bilateral upper limb of a 39 year old male patient treated by IJV-SVC bypass using two contegra valved conduit.
Case report
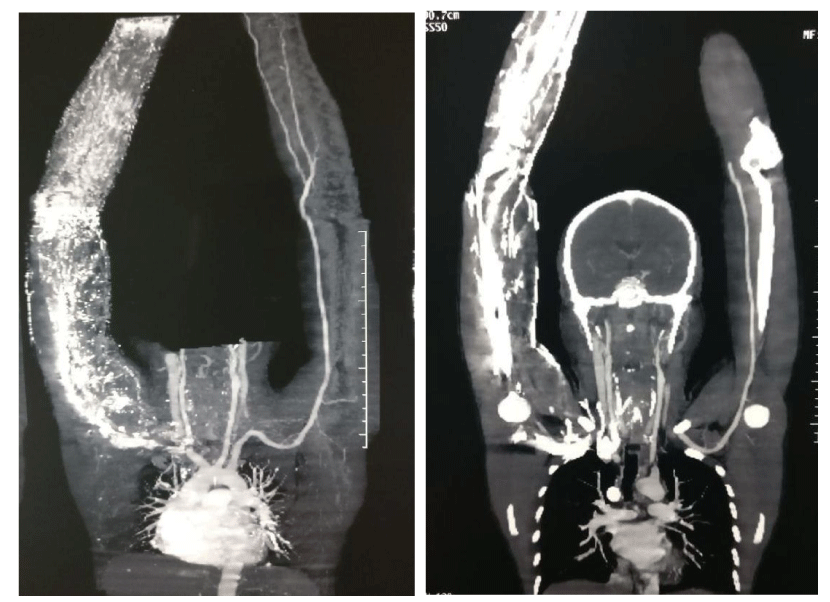
A 39 year-old male patient has a history of facial flushing and puffiness in the supine position and also while bending down. He also gives history of engorgement of veins over neck and left upper limb in head down position which get resolved when head is up. Colour doppler study revealed obstruction in bilateral innominate and left subclavin veins with dilated superficial veins of neck and upper limb. CT Venography showed bilateral brachiocephalic vein [Innominate vein] and left subclavin vein stenosis with resultant dilatation of bilateral superior intercostal vein and multiple diated superficial venous channels of left upper limb (Figure 1).
After all investigations for searching cause of thrombosis all reports normal, nothing found so we called it as idiopathic. Patient symptoms not relieved by medicines and intervention radiologist was not able to pass guidewire across the stenosis. Hence the decision of open surgical venous bypass was taken.
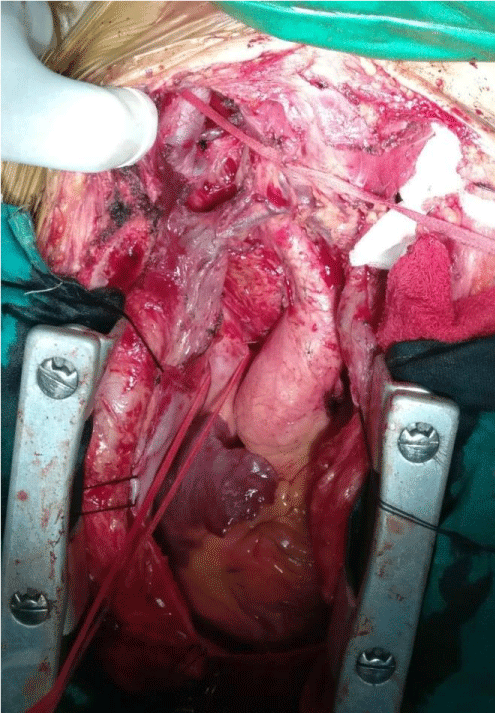
Patient was operated via a midline sternotomy, with the incision extending upwards till lower part of thyroid cartilage. Adequate exposure of the SVC and bilateral internal jugular veins was meticulously performed (Figure 2A).
The thrombosed veins were carefully palpated and the extent of bypass decided. After 100 IU/kg heparinisation two contegra bovine valved conduits; 12 mm X 10 cm were used. Proximal end of the first contegra valve conduit was anastamosed to right distal IJV and distal end to the SVC. The another contegra graft’s proximal end was anastamosed to the left distal IJV and distal end to the first contegra graft distal to its valve in end to side fashion (Figure 2B). Adequacy of flow was confirmed after releasing the clamps.
Patient was started post operatively on inj heparin 5000 IU six hourly and tab warfarin 5 mg once daily at 6 pm. Heparin was discontinued once the INR reached between 2 to 3. The engorgement of the upper limb and neck veins disappeared on post opt day two and also there was no facial flushing as evident earlier when patient becomes supine or bend down. A repeat colour Doppler of the neck was done on 6th post-operative day, which revealed adequate flow in the bilateral IJV to SVC bypass grafts. Patient was discharged on the 8th post opt day on advice of regular follow up with INR report every monthly.
Discussion
On deciding on which would be the ideal graft for effective decompression of the venous system of upper limb we would require a graft that would match with the diameters of the IJV and SVC [3]. A routinely practiced the GSV would not be effective for bilateral decompression as the diameters were too discordant, being 6-7mm that of GSV, as compared to 12-14mm that of IJV and SVC in our pt.
In our cardiovascular setup we usually use Contegra bovine valved graft for surgical correction of severe pulmonic and infundibular stenosis/atresia and use it as a right ventricle to pulmonary artery bypass conduit graft. No use of contegra valved conduit has been discussed in literature history previously for similar cases. Contegra (Medtronic Inc, Minneapolis, MN), a biological valved conduit consisting of a zero-pressure glutaraldehyde preserved heterologous bovine jugular vein with a trileaflet venous valve with natural sinuses [4]. The claimed advantages of this conduit are constant off the shelf availability, a large variety of sizes available, easy tailoring and suturing, adequate hemodynamics thanks to a favorable effective orifice area, no need for proximal or distal extension, and reduced cost. Added advantage was unidirectional flow [5].
Conclusion
Balloon dilation and stenting is a safe and effective treatment for brachicephalic vein stenosis and should be considered the first line treatment.But the role of bypass grafting can not be ignored in cases where stenting not possible or the stent was thrombosed. Use of contegra valved conduit was never reported.Cost of contegra and lifelong anticoagulation are the factors should be discussed with patient before surgery.Also our study report is of only a single case with just six months followup. Using contegra graft more frequently with long term followup will give us a better alternative to the PTFE graft in cases where the unidirectional flow is beneficial and mandatory.
Consent
Informed consent has been obtained from patient.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
- Patnaik MM, Haddad T, Morton CT (2007) Pregnancy and thrombophilia. Expert Review of Cardiovascular Therapy 5: 753-765. Link: https://bit.ly/2Q3segQ
- Unsal EE, Karaca C, Ensarí S (2003) Spontaneous internal jugular vein thrombosis associated with distant malignancies. Eur Arch Otorhinolaryngol 260: 39-41. Link: https://bit.ly/39LR9g6
- Davis D, Petersen J, Feldman R, Cho C, Stevick CA, et al. (1984) Subclavian venous stenosis. JAMA 252: 3404-3406. Link: https://bit.ly/3rNE8c4
- Gloviczik P, Pairolero PC, Toomey BT (1992) Reconstruction of large veins for nonmalignant venous occlusive disease. J Vasc Surg 16: 750-756. Link: https://bit.ly/3uieC0i
- Schillinger F, Schillinger D, Montagnac R, Milcent T (1991) Post catheterisation vein stenosis in haemodialysis: comparative angiographic study of 50 subclavian and 50 internal jugular accesses. Nephrol Dial Transplant 6: 722-724. Link: https://bit.ly/3wy9R4s

Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
