Journal of Civil Engineering and Environmental Sciences
Assessment of immigrant detention centers and detainees health status in Libya
Adel El Taguri1,2* and Aisha Nasef3,4
2Community Department, University of Tripoli, Libya
3Authority of Natural science Research and Technology, Libya
4Scientific Council of Laboratory Medicine, Medical Specialty council, Libya
Cite this as
Taguri AE, Nasef A (2021) Assessment of immigrant detention centers and detainees health status in Libya. J Civil Eng Environ Sci 7(1): 025-030. DOI: 10.17352/2455-488X.000041Migrants are extremely vulnerable to various risks including the lack of physical and mental health care. The weakness of the health system in Libya is further undermined by the fragile, insecure, limited access, threats to health care workers and the increased social and economic challenges. This study studied the general environment of Detention Centers (DCs) of migrants in Libya and their health. Information were collected by during visits to DCs using to assess the structure, organization, financing, processes occurring in the center upon arrival of detainees, accommodation, water, sanitation and hygiene, food and nutrition, health-care services, and health status of detainees including their general health, chronic conditions, acute challenges as infections including TB, STD/HIV, hepatitis and malaria, and violence. Mental health was assessed using standard tools. Special questions were constructed for pregnant females and under five children. Sixteen DCs were visited. Thirteen of them had children in their premises, while ten detained women. Of the 427 interviewed, more than half were younger than 25 years of age. Overall environment and amenities were inadequate or poor. In more than half of DCs, deliveries did occur inside the DC itself. According to DCs managers, most common causes of death were TB, malnutrition and depression. The prevalence of acute and chronic illnesses including mental conditions were determined. Specific actions are proposed to each in particularly establishing/reviving a dedicated health center to meet the individual and public health needs of migrants.
Introduction
The world is currently facing what seems to be the largest ever wave of Displaced-Immigrant-Refugee “DIR” population in history. The Eastern Mediterranean Region (EMR) is carrying the largest burden as more than half of these are in this region. Libya has always been an attractive departure point for economic migrants from Africa and the Middle East. With the longest coast on the Mediterranean in its northern border and the long and difficult to protect other borders, Libya became a major cross-road to Southern Europe not only for human traffic and irregular immigration. At the end of the previous decade, it was estimated that there were more than one and half million immigrants in Libya. The environment for humanitarian actors in countries of the the whole region is fragile, insecure with limited access; threats to health care workers; and increased social and economic challenges. Libya is a particular case in the region as most of these migrants are of mixed origin populations that are coming from even remote areas and for many variable reasons.
As DIR are extremely vulnerable to human rights abuses, particularly the lack of/or denial of physical and mental health care, protection services should be made available and strengthened to vulnerable migrants with particular emphasis on victims of trafficking (VoTs); Unaccompanied Migrant Children (UMC); migrants with serious medical conditions (including HIV/AIDS); and other categories of those at-risk.
Despite the current situation consisting of insecurity, a lack of rule of law and the loss of financial stability, Libya is still an important transit and destination country for migrants. In certain instances, migrants remain stranded in Libya and are caught by the authorities, or they become easy targets for the smuggling networks which promise safe travel to desperate people willing to embark on a dangerous trip by sea to Europe.
Since 2014 transiting migrants, primarily from East and West Africa have continued to exploit Libyan political instability and weak border controls and use the country as a primary departure point to migrate across the central Mediterranean to Europe [1]. The total population of migrants in Libya had been about 700,000 – 1 million people, mainly coming from Egypt, Niger, Sudan, Nigeria, Bangladesh, Syria, and Mali. The constant tragedies in the Mediterranean, coupled with the deteriorating situation of the local population, make it necessary to address the instability in Libya through various interventions. The Department for Combating Illegal Migration (DCIM), affiliated to the Interior Ministry, managed the formal migrant detention centers. Of note, there are non-formal migrant detention centers ran by smugglers and traffickers.
Libya’s health sector capacity has been burdened and under-resourced. The repeated emergencies have not allowed a proper recovery of public sector services. A Service Availability and Readiness Assessment survey, conducted by the WHO and the ministry of health, showed that health system has practically collapsed [2]. Although Libya’s health system is largely a public-health oriented health system, it is weak in essence, with debilitated Primary Health-Care (PHC) network, and neglected health services. There were only few previous activities for assessment of migration and of Detention Centers (DCs) conditions that were performed [3]. These assessments concluded that more services should be tailored to these vulnerable Migrants.
In this study, a survey was designed to assess objectively the general environment in and surrounding the DCs in Libya and the corresponding health situation of the detained immigrants.
Materials and Methods
Population and data collection
Information was collected by different qualitative and quantitative means. It include structured visits to DCs all over Libya using standard questionnaires and discussion with detainees. The focus of the current survey is the status of immigrants in DCs. The list includes all DCIM affiliated and not affiliated DCs to construct a better picture of the situation and challenges facing Immigrants in Libya.
It should be noted that these would only represent a fraction of the total number of immigrants in the country as thousands of immigrants are employed and are contributing actively in Libyan society. The assessment done involved all stakeholders and included accommodation, water, sanitation and hygiene, food and nutrition, health-care services, and health status of detainees.
Assessment tools
The survey involved two questionnaires. First questionnaire was designed to gather data about DCs. The second questionnaire was designed to collect data from detainees.
Detention centers tool
First questionnaire contains general data about visited centers including structure, organization, financing, processes occurring in the center upon arrival of detainees and how is health taken care of in addition to shelter and hygiene (Appendix 1).
Detainees tool
Second questionnaire contains questions addressed to detainees in order to assess their general health, chronic conditions, acute diseases in particular infections and violence that they might have been exposed to. Other data obtained regarding general health and some of the most important infections as tuberculosis, STD/HIV, hepatitis and malaria. mental health using standard mental health tools. Special appendices were constructed for pregnant females and under five children and added to this tool.
Results
Detention centers
Sixteen DCs were visited. Fifteen of these DCs are recognized as affiliated to the designed authority by the Libyan government (DCIM), and one non- affiliated and permitted visiting and surveying of detainees. Ten (62.50%) DCs find that the budget was not enough the last year. Thirteen DCs (81.25%) have children in their premises. Three (18.75%) of these contain more than 50 children. Ten (62.50%) of these centers also detain women. One center contains 520 women.
Among DCs, only three centers were considered part of National program for Immunization, two centers for TB and only one center for HIV. In 12 of these DCs, the health Unit works only during official working hours (Till 14hr). Water supply was considered adequate in 13 DCs (81.3%). Five (31.25%) of DCs have visible fissures in the walls and/or ceilings. Humidity (molds) was visible to naked eye in one of DCs. There is evidence of dense presence of insect and/or rodents in seven (46.7%) DCs. In only two DCs, bed linen and covertures were appropriate. They were regularly cleaned and replaced in seven (43.8%) DCs. Enough beds were reported in five (less than 1/3) of the visited DCs.
Detainees are allowed in open air in all DCs. In six (43.8%) DCs, they are allowed just one hour or less. The remaining DCs allow detainees to stay in open air for more than two hours per day. Detainees in almost 2/3 of DCs work during their detention. In most of the cases this happens inside the DCs.
In only five DCs, food presented was of enough quantity. One third of DCs receive food donations, but this occurs less than twice per month. Premises where food is prepared was not considered suitable in more than 3/4 of DCs. Forty three percent of food handlers are not trained. Soap was not available in 42.9% of food distribution halls. In two DCs, hygiene in food halls was poor or very poor.
Only in three DCs, the medical unit supervises hygiene in DC premises. In quarter of DCs, there are no regular visits by medical staff. Two-fifth of DCs refers sick detainees to privet clinics and 1/3 to public hospitals.
It is necessary to have a pre-requested permission to seek medical advice in seven (43.8%) of DCs. Two-Thirds find that this permission to seek medical advice was fast and more than 90% found it easy enough to obtain the permission.
There was an isolation room in 71.4% of DCs. According to staff, 84.6% consider that they need more drugs. In only nine DCs, newcomers are subjected to medical assessment at entry. In more than half of DCs, deliveries did occur inside the DC itself. More than 3/4 of DCs have reported cases of scabies and/or pediculosis. In two DCs, detainees were reported to have scorpion/snake bites. More than 2/5 detainees reported exposure to some form of violence, half of them outside the DC before his arrival. In only two DCs there were health promotion activities which were devoted to mental health.
More than 90% do not keep files for patients, but half keep registers for them. In about 2/3 of DCs the access to these documents are not limited to physicians. Informed consent is only requested in three DCs before blood investigations were performed. Most common causes of death among detainees are Tuberculosis, malnutrition and depression according to DCs managers.
Detainees
Number of detainees interviewed was 427. The highest number was in Gharian DC, where 90 detainees were met. Tajoura follows (71 detainees) and Zwara (61 detainees). Most of detainees were from Sudan (Darfur in particular) followed by Eretria and Somalia (86, 54, and 52 respectively).
The age range of detainees in DCs is 13-63 years. More than half of them are younger than 25 years of age. More than half of detainees (62.2%) spent more than a year in the DCs. Although 224 (52.46%) of them either did not have a job before arrival or did not specify it, the job range of detainees varied widely. Some of detainees were farmers, construction workers, nurses, engineers, English teachers, clothes designers, and carpenters.
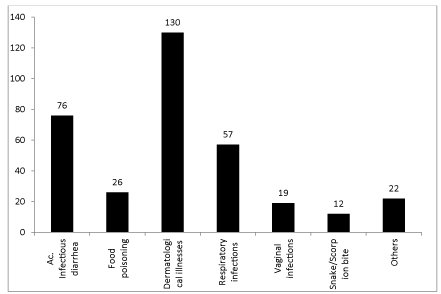
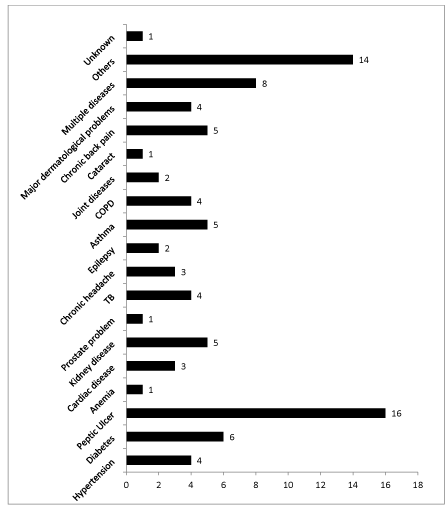
Two-fifth of detainees had acute diarrhea in the six months preceding the survey and about 7% had food poisoning. While one third had skin diseases as scabies and/or pediculosis, 14.7% had respiratory infections and 3% reported snake/scorpion bites during the same period (Figure 1). Seventy three detainees (17.10%) reported having a chronic disease. The types of illness and the number of detainees affected are shown in DCs (Figure 2).
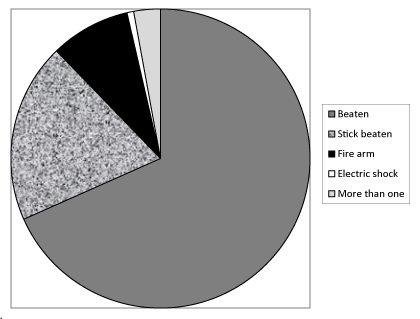
One hundred fifty (35.10%) detainees reported that they were exposed to some form of physical violence from the start of the journey till arrival to DC. The majority of these incidents of abuse (125) had been exposed to violence during the journey either outside Libya (30 detainees, 7.0%) or inside Libya (90 detainees, 21.1%) or in both (five detainees, 3.6%). The remaining 25 detainees had been exposed to violence during arrest or inside current or previous DC. The type of physical violence they were exposed to is shown in (Figure 3).
One-third (52 detainees) had depression according to PHQ2 screening tool while half had anxiety (Table 1) and only 7% had Post traumatic Stress Disorders (PTSD). More than half of detainees were not satisfied with the medical services delivered to them.
There were 32 pregnant women. About half of them (46.9%) did not have antenatal visits. The non-presence of complications and the non-availability of the service were the most common reasons (almost 1/3 for each of them).
Fifty one children under five years of age were approached. Almost 1/3 had diarrhea and 2/5 had cough and respiratory difficulty in the two weeks preceding the survey. Symptoms of stress among children as difficulty sleeping (41.2%) and frequent and easily crying (29.4%) were also frequent.
Discussion
This survey tried to look to the issue of migration from different complementary perspectives including the inner environment in the DCs. Thought, the focus of the survey is the status of immigrants in DCs, it should be noted that “detainees” would only represent a small fraction of the total number of real immigrants.
Infections are usually considered as major environmental hazard in mass gathering. All shelter residents should use “General Infection Prevention Measures” to reduce the spread of infections and infectious diseases [4]. Standard precautions should be applied to all residents in DCs to protect residents and staff alike. Personal protective equipment (e.g., gloves, masks, and gowns) should be provided for healthcare personnel who staff the special-needs shelter. Each resident should be screened at the time of entry to the special needs shelter to detect any conditions necessitating isolation and/or use of Transmission-Based Precautions [5].
Of paramount importance is the appropriate practice of Hand Hygiene. In addition, proper techniques to use when washing your hands with soap and water and techniques for hand washing with alcohol-based products should be followed.
Protein-Energy-Malnutrition (PEM) remains the most common nutritional problems. In recent years more and more micronutrient deficiency diseases are recognized among migrant populations entirely dependent on external food aid.
While humanitarian aid usually focuses on the immediate physical needs of migrants like clean water, food, and shelter, it often overlooks mental health. Violence and displacement increases the need for mental health services, especially for women and children. Both questionnaires for detainees and workers in the current survey used standard validated mental health tools (PHQ9, GAD7 and PC-PTSD). The full version of the PHQ-9 and GAD-7 that were used screened for the presence of depression and anxiety, but also to assess their severity. Major issues and general measures to tackle them are presented in the following tables (Tables 2,3). Psychiatric disorders, like Post Traumatic Stress Disorder, mental exhaustion and chronic fatigue syndrome effect many migrants [6]. These disorders greatly affect the long-term quality of life for migrants.
Non-Communicable Diseases (NCD) also constitute a major health threat for displaced populations and for migrants who have found themselves at increasing risk of deteriorating health status. A significant number of migrants suffer from chronic diseases such as hypertension, cardiovascular diseases, diabetes and cancer, all requiring costly and long-term treatment. The most frequently observed NCDs are asthma/chronic obstructive pulmonary disease (COPD), diabetes, hypertension and cardiovascular diseases.
It has to be clearly stated that migrants are coming from different physical and social environmental backgrounds. They had left their places of origin due to many reasons. In much of the cases, this is due to unfavorable socioeconomic conditions. These unfavorable conditions would particularly further increase health risks before, during, and after migration. This is particularly so for infections, nutrition and mental health issues. For chronic illnesses, the loss of the continuity of management would further contribute to health hazards if not properly taken care off.
Specific actions to be proposed, process owner(s) and other stakeholders to be discussed according to the nature of these measures, to input from the various stakeholders and depending upon local circumstances. It’s of paramount importance strategically to establish a dedicated health center to meet the individual and public health needs, as most of these proposed measures would be effectively and efficiently realized by such center. In addition to the unfamiliarity and low level of knowledge among care provider regarding the pathologies the migrants are particularly exposed to, the vulnerability of migrants to many of the illness they are exposed to before, during and after migration would require a particular set of skills. The presumed center would implement the executive functions handled to them by the currently established division at the Ministry of Health and implemented by many fragmented service providers. It could also function as a house of experience for these morbidity and mortality pattern in the country and in the whole region.
- European Commission (2017) European Civil Protection and Humanitarian Aid Operations – Libya. European Commission. Link:
- Zarocostas J (2018) Libya: war and migration strain a broken health system. Lancet 391: 824-825. Link: https://bit.ly/2SkF8Z7
- Bisrat F, Berhane Y, Mamo A, Asefa E (1995) Morbidity Pattern Among Refugees in Eastern Ethiopia. East Afr Med J l 72: 728-730. Link: https://bit.ly/3edd7eD
- Center for Disease Control and Prevention. General Infection Prevention Techniques. Infection Control Prevention Guidance for Community Shelters Following Disasters. Department of Health and Human Services, Atlanta, 2005.
- Center of Disease Control and Prevention. Transmission-Based Precautions.
- Bisrat F, Berhane Y, Mamo A, Asefa E (1995) Morbidity Pattern Among Refugees in Eastern Ethiopia. East African Medical Journal 72: 728-730. Link: https://bit.ly/3nHC7Og
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
