Journal of Biology and Medicine
Suppurrative prostatitis with symptomatic benign prostatic hyperplasia: A case report and revi1ew of literature
Paul E Ngwu1*, Cornelius C Chukwuegbo2 and George O Achor1,3
2Department of Histopathology, Federal Medical Center, Umuahia, Nigeria
3Department of Surgery, Abia state University Teaching Hospital, Aba, Nigeria
Cite this as
Ngwu PE, Chukwuegbo CC, Achor GO (2019) Suppurrative prostatitis with symptomatic benign prostatic hyperplasia: A case report and revi1ew of literature. J Biol Med 3(1): 034-036. DOI: 10.17352/jbm.000011Introduction: The diagnosis of suppurrative prostatitis is rare affecting men mostly in their 5th or 6th decades. Suppurative prostatitis can co-exist with symptomatic benign prostatic hyperplasia (BPH) making diagnosis and treatment much more challenging.
Observation: We report a case of a 75 years old man that presented initially with lower urinary tract symptoms, was placed on alpha adrenergic blockers and lost to follow up for 4 years before presenting with acute urinary retention. He subsequently had open prostatectomy with a histological diagnosis of suppurrative prostatitis and benign prostatic hyperplasia.
Conclusion: Suppurrative prostatitis should be considered in elderly patients presenting with lower urinary tract symptoms especially when there are risk factors for its occurrence.
Introduction
The prostate is an uncommon site for suppuration [1]. The occurrence of Suppurative prostatitis with symptomatic Benign prostatic hyperplasia (BPH) is very rare. Suppurative prostatitis usually occur in men in their 5th or 6th decades [2]. The presentation of suppurative prostatitis can be non-specific and in some cases mimicking the lower urinary tract symptoms of patients with BPH thereby making the diagnosis difficult.
Case Presentation
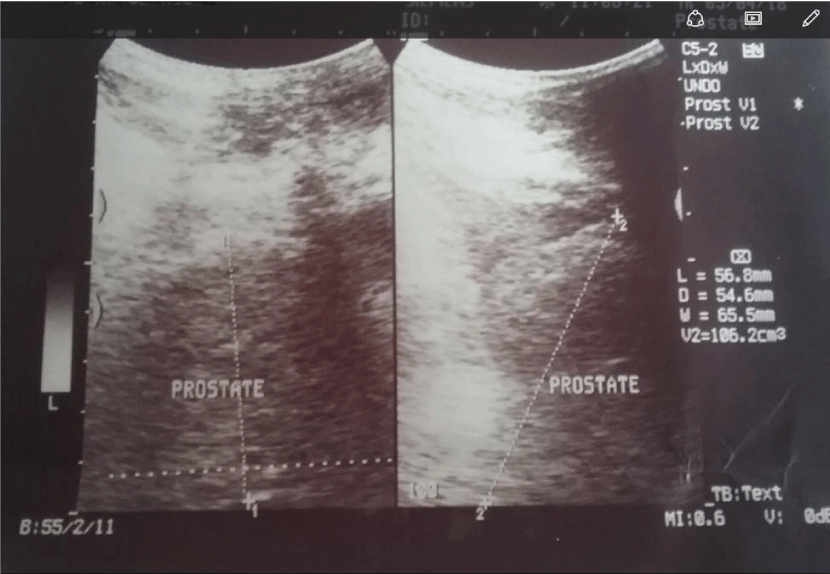
The patient is a 75 year old man that initially presented in 2014 with storage and voiding lower urinary tract symptoms (LUTS). Prostate specific antigen (PSA) was 16ng/ml for which he had digitally guided prostate needle biopsy with histological diagnosis of BPH. He was commensed on tamsulosin, an alpha adrenergic blocker but was lost to follow up. He however re-presented in march 2018 in acute urinary retention and after a failed urethral catheterization was offered suprapubic cystostomy. He was still having LUTS but no suprapubic or perineal pain. Digital rectal examination (DRE) revealed an enlarged prostate with benign features. Abdominopelvic ultrasound scan revealed an enlarged prostate with a volume of 106.2cm3 with a heterogenous echotexture and smooth outline, no mass,cyst or calcification noted. Urine culture yielded mixed growth of Pseudomonas species and enterococcus species sensitive to augmentin,gentamicin,erythromycin, PSA was 26ng/ml. He was treated with Augmentin and Genticin and a repeat culture showed a resolution of infection. He had transvesical prostatectomy, hematuria stopped on the 2nd post operative day but patient developed heamuria on the 5th post operative day, urine culture yeided heavy growth of pseudomonas for which he was managed by bladder irrigation and administration of levofloxacin and genticin based on sensitivity pattern. Hematuria stopped by 7th day post operation, catheter removed and patient discharged.
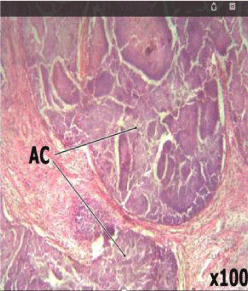
On pathological examination, the prostate weighed 102g with a nodular grayish white appearance and bosselated surface. Cut sections revealed multiple cysts giving a spongy appearance. On microscopy,prostatic tissue showed a biphasic lesion consisting of acinar and fibromuscular proliferation. Within the stroma were foci of abscess composed of abundant neutrophils and necrotic debris. There was no typia. A histologic diagnosis of nodular hyperplasia with suppurative prostatitis was made.
First and second post-operative clinical visits were all uneventful.
Discussion
Suppurrative prostatitis is rare and difficult to diagnose1 and its coexistence with symptomatic BPH makes its diagnosis even more difficult. Suppurative prostatitis usually occur in middle-aged men in their 5th or 6th decades and are more common in individuals who are immunocompromised, diabetic, on hemodialysis, who have indwelling catheters or following prostate needle biopsy[2-5]. A study done by Tiwari et al puts diabetics and prolonged catheterization as the most common causes. The index patient was on indwelling catheter prior to his surgery and prostate biopsy is unlikely playing a role here since he had it four years earlier.
Our patient was having LUTS but the classical findings of fever,dysuria, perineal or suprapubic pain as well as a tender and fluctuant prostate on DRE were all absent making the diagnosis of suppurative prostatitis remote based on clinical findings.The urine culture of our patient showed mixed growth of pseudomonas species and enteroccocus species. Aerobic gram-negative bacilli are the predominant pathogens in bacterial prostatitis, E. coli accounts for 50%–80% of these cases, Enterococcus species 5%–10% of cases, and non fermenting gram-negative bacilli eg Pseudomonas species <5% of cases [6].
Other forms of suppurative prostatitis have also been reported in the literature including tuberculous prostatitis and emphysematous prostatitis [7,8]. Though transrectal ultrasound scan is the ideal for the diagnosis of suppurative prostatitis, it was not available at the time of this study, the abdominopelvic ultrasound scan that was done did not detect the suppuration. Though Tiwari et al [4], in their study indicated that 50% of the patients in their study had their suppuration detected on abdominopelvic ultrasound scan( those with abscess cavities greater than 1cm ) Suppuration was only seen in the index case on the gross specimen following sectioning of the prostate and confirmed on histological analysis as shown in the slides. Treatment options for suppurative prostatitis include transurethral unroofing, transurethral or transperineal ultrasound guided puncture or conservative management with only antibiotics for the patients with small monofocal abscess cavity that is less than 1cm in diameter [4,9]. Our patient had transvesical prostatectomy,developed hematuria on the 5th post operative day which could be regarded as secondary hemorrhage from infection considering the urine culture result (Figures 1-3).
Conclusion
Suppurrative prostatitis is rare and presentation can be non-specific as seen in the index case. The coexistence of suppurative prostatitis with BPH could pose even more
Diagnostic challenge. A high index of suspicion is required to make the diagnosis.
- Jacobsen JD, Kvist E (1993) Prostatic abscess. A review of literature and a presentation of 5 cases. Scand J Urol Nephrol 27: 281-4. Link: http://bit.ly/2Kb0RvX
- Lummus WE, Thompson I (2001) Prostatitis. Emerg Med Clin North Am 19: 691-707. Link: http://bit.ly/2YHKMWG
- Benway BM, Moon TD (2008) Bacterial prostatitis Urol Clin North Am 35: 23-32. Link: http://bit.ly/2YiT345
- Tiwari P, Pal DK, Tripathi A, Kumar S, Vijay M, et al. (2011) Prostatic abscess: Diagnosis and management in the modern antibiotic era. Saudi J Kidney Dis Transpl 22: 298-301. Link: http://bit.ly/2Zpe6P7
- Dell'atti L (2013) Prostatic abscess after transrectal ultrasound-guided prostate biopsy. Case report. G Chir 34: 260-262. Link: http://bit.ly/2MtfJaO
- Lipsky B, Byren I, Hoey C (2010) Treatment of Bacterial Prostatitis. Clinical Infectious Diseases 50: 1641-1652. Link: http://bit.ly/2SZieTv
- Eduardo Kaiser Ururahy Nunes Fonseca, Oskar Grau Kaufmann, Layra Ribeiro de Sousa Leão, Cassia Franco Tridente, et al. (2018) Incidentally detected tuberculous prostatitis with microabscess. International braz j urol 44: 397-399 Link: http://bit.ly/2OxyZX7
- Bae GB, Kim SW, Shin BC, Oh JT, Do BH,et al. (2003) Emphysematous prostatic abscess due to Klebsiella pneumoniae: report of a case and review of the literature. J Korean Med Sci 18: 758-60. Link: http://bit.ly/2Myz9uR
- Ludwig M, Schroeder-Printzen I, Schiefer HG, Weidner W (1999) Diagnosis and therapeutic management of 18 patients with prostatic abscess. Urology 53: 340-345. Link: http://bit.ly/2Ym5qfC
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
