International Journal of Vascular Surgery and Medicine
Iliac Vein Injury during Total Hip Replacement: A Rare Iatrogenic Complication and its Successful Surgical Treatment
Ayhan Müdüroğlu1, Taha Oğuz Kayhan2 and Ahmet Yüksel3*
2Department of Emergency, Beylikduzu State Hospital, Istanbul, Turkey
3Department of Cardiovascular Surgery, Bursa State Hospital, Bursa, Turkey
Cite this as
Müdüroğlu A, Kayhan TO, Yüksel A (2017) Iliac Vein Injury during Total Hip Replacement: A Rare Iatrogenic Complication and its Successful Surgical Treatment. Int J Vasc Surg Med 3(2): 033-035. DOI: 10.17352/2455-5452.000025Vascular injury during total hip replacement is a rare condition with the incidence varying between 0.1% and 0.3%. However when develops, it has a potential of serious complications such as extremity loss and even death. Prompt identification and appropriate surgical management of this condition are crucial and may decrease the rate of morbidity and mortality. In this report, we presented a case of iatrogenic iliac vein injury during total hip replacement and its successful surgical management.
Introduction
Vascular injury during total hip replacement (THR) is an uncommon phenomenon, but when occurs it may threaten both the extremity and the life of the patient. The most common affected vessels from a vascular injury during THR are external iliac artery and vein, and common femoral artery and vein [1,2]. The early complications of a major vascular injury are mainly bleeding and ischemia, while the late complications are arteriovenous fistula and pseudoaneurysm formation [1,3]. If a bleeding occurs as an early complication, the main indicator of mortality depends on whether the patient is in shock or not [4]. Here, it was reported a case of iatrogenic iliac vein injury during THP, which was successfully treated with appropriate surgical approach. We decided to present this subject as it is seen very rarely.
Case Presentation
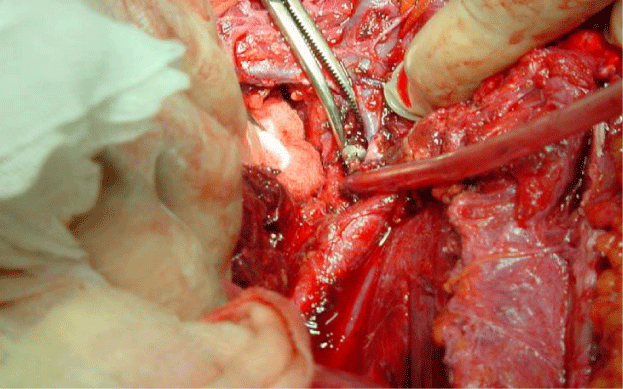
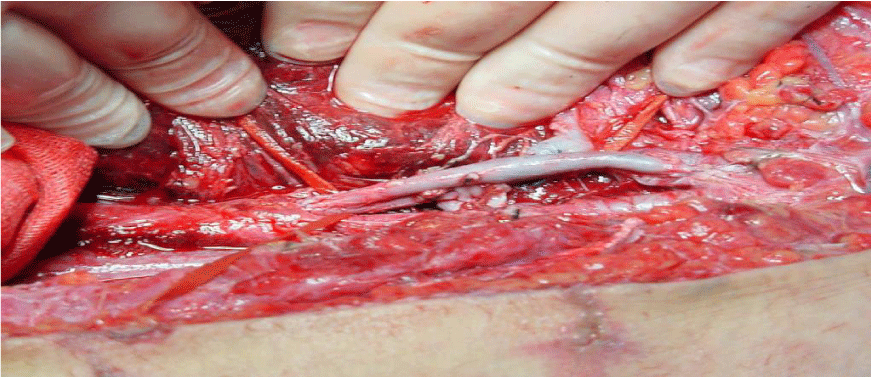
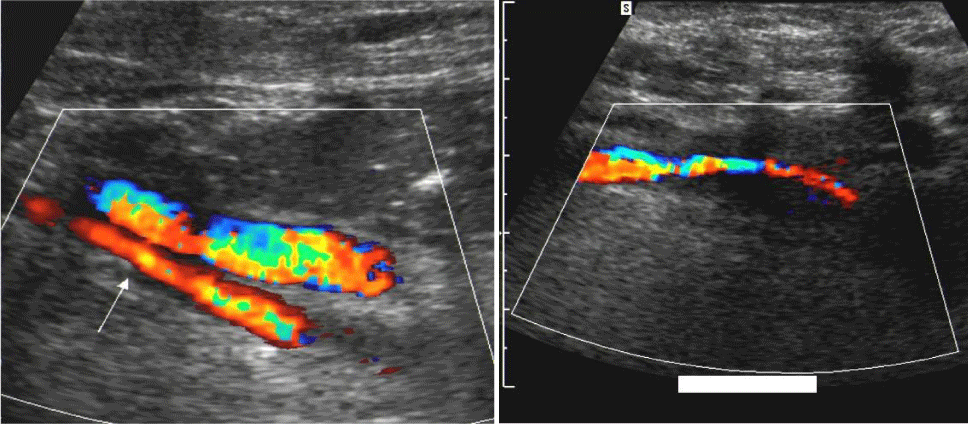
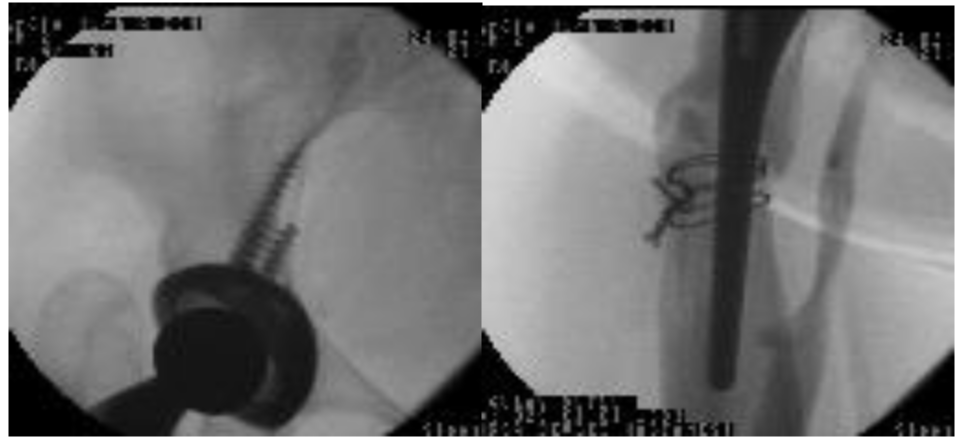
An 18 year-old female patient has undergone THR and shortening procedures in Orthopedic Department due to congenital hip dislocation (CHD). She was consulted to our Cardiovascular Surgery Department because of the existence of hemodynamic instability in the early postoperative period. When the patient examined immediately, it was decided to perform an urgent operation, since there was a strong suspicion of the existence of a massive retroperitoneal hemorrhage. After a right para median incision, the retroperitoneal space was accessed via Tran’s peritoneal approach (Figure 1). Prompt blood transfusion was employed simultaneously. Massive and diffuse hemorrhage precluded the identification of the source of the bleeding. Following employing the packing, the operation was ended. Afterwards, a significant amount of fluid and blood product replacement was administered with both crystalloid and colloid solutions and a total of 18 units of erythrocyte suspension and 18 units of fresh frozen plasma transfusions during early postoperative period. Fluid and electrolyte balances were closely monitored at that time. She was explored surgically with the stable situation hemodynamically at postoperative third day. It was observed that there was no active bleeding in surgical site and the proximal portion of the external iliac vein was injured by the screw-tip drilled to the pelvic bone to fix the metal back of the cup (Figure 2). The screw-tip was cut, and a 5 cm of saphenous vein was harvested from the contralateral leg. In order to prevent embolization, iliocaval junction was externally compressed digitally and thrombi in the proximal venous system with the assistance of a fogarty catheter and the ones in the distal venous tree with external compression were evacuated. The severed iliac vein was bleeding from both ends. Following irrigating with heparinized solutions, both ends of the external iliac vein were ligated and continuity was established by interposition of the saphenous vein (Figure 3). Hemostasis was acquired and the incised surgical layers were sewed seemly. She was well both in the early postoperative period and at the follow up visits. Twenty six months after the operation, Doppler ultrasound and venography examinations revealed the patency of the saphenous vein graft, although due to the surrounding fibrosis it was externally compressed and led to the formation of collateral circulation on the right side (Figures 4, 5). Neither clinically like pain, cramp, oedema and diameter difference between the legs nor radio logically like thrombosis of the saphenous vein or deep veins and post thrombotic findings, any problem was observed at last follow-up visit.
Discussion
Vascular injury as a complication of THR surgery is very rare with an incidence range varying between 0.1% and 0.3% in the literature [1,5-7]. However, when develops it may cause a catastrophic clinical status including extremity loss and even mortality [1,6]. These hazards can be higher particularly in patients required revision surgery. Early identification and appropriate management of this condition can reduce the rate of morbidity and mortality [1,6,8-10]. Since these risks will increase during revision surgery it has been postulated that in such cases retroperitoneal exposure or to decrease the rate of vascular injuries perioperative angiography should be employed on a routine basis [11]. Lately the frequent use of three-dimensional computed tomography has enabled localizing the vessels surrounding the acetabulum thus aiding the planning of the surgical procedure and avoiding any possible vascular injury [12,13]. The most common affected vessels are the external iliac vein and artery and the femoral artery and vein [1,2,14]. In the literature, Pan et al. reported three vascular injuries in 721 THR operations. Two of them were iliac vein injury, while the third one was femoral artery injury [14]. According to the study performed by Schoenfeld et al., in 68 patients with vascular injury during THR, the reported rate of mortality and extremity loss were 7% and 15%, respectively [1]. In another study performed by Beguin et al., similarly, it was stated that the rate of mortality and possible functional squeal following vascular injury were 7% and 19%, respectively [6]. The drilling of the anteriosuperior quadrant of the acetabulum in the cement less THR massive retroperitoneal bleeding can occur due to the injury of the external iliac vein. In a study with cadavers posterior inferior and posterior superior quadrants were found to be more suitable drilling [15]. Siegel et al. advocated that their case which dynamic hip drilling was used was one of the few people cases in the literature and was not the first fatal case. Their case was stable in the postoperative period before suddenly displaying circulatory collapse and eventually did not respond to resuscitation. Postmortem evaluation had disclosed massive hemorrhage due to external iliac vein injury [16].
As a result, it should be keep in mind that the vascular injuries can be still unavoidable in THR surgery despite planning with preoperative further tests and employing appropriate surgical techniques. Although the risk of development of vascular injury after THR surgery may be very low, its results could be catastrophic if it occurs. It should be emphasized that the most important factor is to suspect for prompt identification of this condition. Early diagnosis and quick surgical intervention can reduce both mortality and morbidity.
- Shoenfeld NA, Stuchin SA, Pearl R, Haveson S (1990) the management of vascular injuries associated with total hip arthroplasty. J Vasc Surg 11: 549-555. Link: https://goo.gl/LQeykp
- Dietze S, Perka C, Baecker H (2014) Blood vessel and nerve damage in total hip arthroplasty. Orthopade 43: 64-69. Link: https://goo.gl/R3MZH7
- Avisar E, Elvey MH, Bar-Ziv Y, Tamir E, Agar G (2015) severe vascular complications and intervention following elective total hip and knee replacement: A 16-year retrospective analysis. J Orthop 12: 151-155. Link: https://goo.gl/visN0t
- Haan J, Rodriguez A, Chiu W, Boswell S, Scott J, et al. (2003) Operative management and outcome of iliac vessel injury: a ten-year experience. Am Surg 69: 581-586. Link: https://goo.gl/Tk2WYy
- Fruhwirth J, Koch G, Ivanic GM, Seibert FJ, Tesch NP (1997) Vascular lesions in surgery of the hip joint. Unfallchirurg 100: 119-123. Link: https://goo.gl/xCP1WW
- Beguin L, Feugier P, Durand JM, Chalencon F, Gresta G, et al. (2001) Vascular risk and total hip arthroplasty. Rev Chir Orthop Reparatrice Appar Mot 87: 489-498. Link: https://goo.gl/Pphksg
- Calligaro KD, Dougherty MJ, Ryan S, Booth RE (2003) acute arterial complications associated with total hip and knee arthroplasty. J Vasc Surg 6: 1170-1177. Link: https://goo.gl/RicjWO
- Sharma DK, Kumar N, Mishra V, Howell FR (2003) Vascular injuries in total hip replacement arthroplasty: a review of the problem. Am J Orthop 32: 487-91. Link: https://goo.gl/TS5ht9
- Novotný K, Pádr R, Landor I, Sosna A (2011) vascular injuries in joint replacement surgery. Acta Chir Orthop Traumatol Cech 78: 200-207. Link: https://goo.gl/F08A82
- Alshameeri Z, Bajekal R, Varty K, Khanduja V (2015) iatrogenic vascular injuries during arthroplasty of the hip. Bone Joint J 97: 1447-1455. Link: https://goo.gl/NpEdui
- Riouallon G, Zilber S, Allain J (2009) Common femoral artery intimal injury following total hip replacement. A case report and literature review. Orthop Traumatol Surg Res 95: 154-158. Link: https://goo.gl/6vITzR
- Kawasaki Y, Egawa H, Hamada D, Takao S, Nakano S, et al. (2012) Location of intrapelvic vessels around the acetabulum assessed by three-dimensional computed tomographic angiography: prevention of vascular-related complications in total hip arthroplasty. J Orthop Sci 17: 397-406. Link: https://goo.gl/SsyH2j
- Fukunishi S, Okahisa S, Fukui T, Nishio S, Fujihara Y, et al. (2014) Significance of preoperative 3D-CT angiography for localization of the femoral artery in complicated THA. J Orthop Sci 19: 457-464. Link: https://goo.gl/lbHwdl
- Pan B, Zhang G (1997) severe vascular injuries following total hip replacement. Zhonghua Wai Ke Za Zhi 35: 453-455. Link: https://goo.gl/9EYjUw
- Hwang SK (1994) vascular injury during total hip arthroplasty: the anatomy of the acetabulum. Int Orthop 18: 29-31. Link: https://goo.gl/2drSWK
- Siegel A, Schulz F, Puschel K (2001) fatal pelvic vein injury caused by guide wire used with the dynamic hip screw. Unfallchirurg 104: 182-186. Link: https://goo.gl/Gf6X2i
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
