International Journal of Spine Research
Surgical treatment of spinal tumors with modified laminoplasty: Preliminary study
Idiris Altun
Cite this as
Altun I (2022) Surgical treatment of spinal tumors with modified laminoplasty: Preliminary study. Int J Spine Res 4(1): 001-008. DOI: 10.17352/ijsr.000021Copyright License
© 2022 Altun I. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Objective: We aimed to present our experience with a modified laminoplasty technique that allows stabilization of the spine without instrumentation during tumor surgery.
Methods: This retrospective study was performed in the neurosurgery department of a university hospital and data were collected from the medical files who were treated surgically for spinal tumors. The same surgical team operated on the patients using the same procedure without any instrumentation for stabilization of the spine. Demographic and clinical data were collected. It was checked whether radiological and clinical instability developed at the 6th and 12th months postoperatively.
Results: Our series comprised 41 patients (20 females, 21 males) with an average age of 47.122±20.33 (range: 11 to 86 years). The most common complaints detected in this series were diminution of motor power in lower extremities (20,47.62%), radicular pain (9,21.43%), and hypoesthesia (2,4.76%). The most frequent sites of involvement were L1-L2 (5,11.90%), L2 (4,9.52%), and T5-T6-T7 (2,4.76%), respectively. Histopathologically, schwannoma (8,19.94%), ependymoma (7,16.64%), meningioma (6,14.28%), and metastatic carcinoma (5,11.90%). The distribution of tumors was intradural and extramedullary (27,64.28%), intradural and intramedullary (13,30.95%), and extradural and extramedullary (2,4.77%), respectively.
Conclusion: Our results imply that stability of the spinal cord can be preserved without fixation or instrumentation during surgical procedures for spinal tumors. However, longer periods of follow-up, as well as prospective, controlled, multi-centric trials on larger populations, are warranted to evaluate the safety and efficacy of the novel technique.
Introduction
Surgery has significant benefits over other treatments to resolve spinal cord compression, alleviate pain, and improve quality of life while posing few risks in the management of primary and metastatic tumors of the spinal cord [1,2].
Decompression and stability are the main goals of spinal surgery [1]. Typically, the procedure serves only as a palliative measure [2]. Surgery is occasionally utilized for curative care of primary and, even more rarely, secondary tumors [1,2]. Surgery is preferred 1) when there are neurologic complications related to local tumor development with local compression or fracture, 2) when there is a mechanical complication with a fracture or axial destabilization, 3) when pain does not respond to medical treatment, surgical treatment of spinal metastasis is recommended, 4) in cases of radioresistant cancers (e.g., renal cell carcinoma that does not respond to chemotherapy or radiotherapy; tumor recurrence after prior radiotherapy) [2,3]. We must carefully consider suitable biomechanical qualities for the three columns during reconstruction [3].
In the treatment of spinal malignancies, ensuring spinal stability and mobility is a difficulty that typically necessitates meticulous surgical planning [4]. The treatment of spinal metastatic illness includes spinal stabilization surgery [4,5]. Because of their overall prognosis and concurrent therapy, patients with spinal oncology are unlikely to achieve bone fusion [5]. For these patients, stabilization surgery without fusion may be a viable option. There is a scarcity of research on the effectiveness of this strategy [5].
Although spinal tumors are treated using a variety of surgical procedures, the goal of each treatment, however, is the same: to restore spinal stability and decompress neural tissues, such as the spinal cord and nerve roots [6]. The traditional surgical approach in the treatment of spinal tumors was laminectomy, which can provide an adequate surgical field [6,7]. However, this surgical approach is associated with some complications such as spinal deformity and spinal instability [7]. Laminoplasty, which reconstructs the lamina using instruments such as a titanium plate, T-saw, or translaminar screw, is widely applied in patients with spinal tumors [8]. Some studies have shown that collapse and displacement of the laminae may occur in patients undergoing laminoplasty [8,9]. In osteoporotic or elderly patients, the fixed titanium screw may loosen easily and cause secondary spinal stenosis, resulting in spinal cord injury [9]. We aimed to share our experience with our novel operative technique that allows stabilization without instrumentation in the surgical management of spinal tumors together with a brief review of current literature.
Materials and methods
Study design
This retrospective study was carried out in the neurosurgery department of a tertiary care center after the approval of the local institutional review board (2021/26/03). Data were gathered from the hospital database an average age of 47.122±20.33 (range: 11 to 86 years) treated surgically for spinal tumors. The baseline descriptives, clinical and radiological information, operative and histopathological data were recorded. The variables under investigation included age, sex, radiological data derived from Magnetic Resonance Imaging (MRI), neurological findings, the level of surgical procedure, histopathological diagnoses, and radiological instability. A single senior neurosurgeon (IA) carried out the consecutive spinal procedures in our center during a 3 year period (between 2017 and 2020). Strobe guideline was used in writing this manuscript.
Patients with spinal tumors who underwent laminectomy at level 2 or more were included in the study (Figure 1). Patients who had a single-level laminectomy, hemilaminectomy, or had significant preoperative instability were excluded from the study. Patients with multiple myeloma were excluded from this study because this disease has biological characteristics that differ from metastatic lesions and solid tumors, especially in terms of the probability of bone repair [6].
Surgical procedure
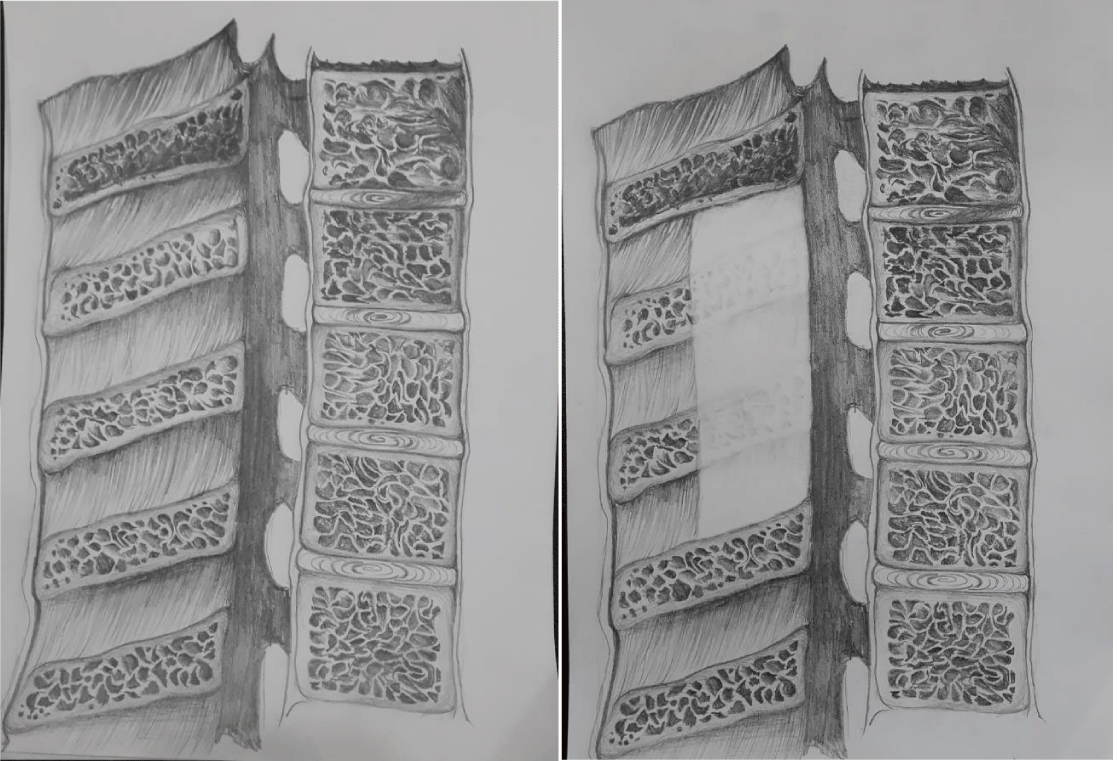
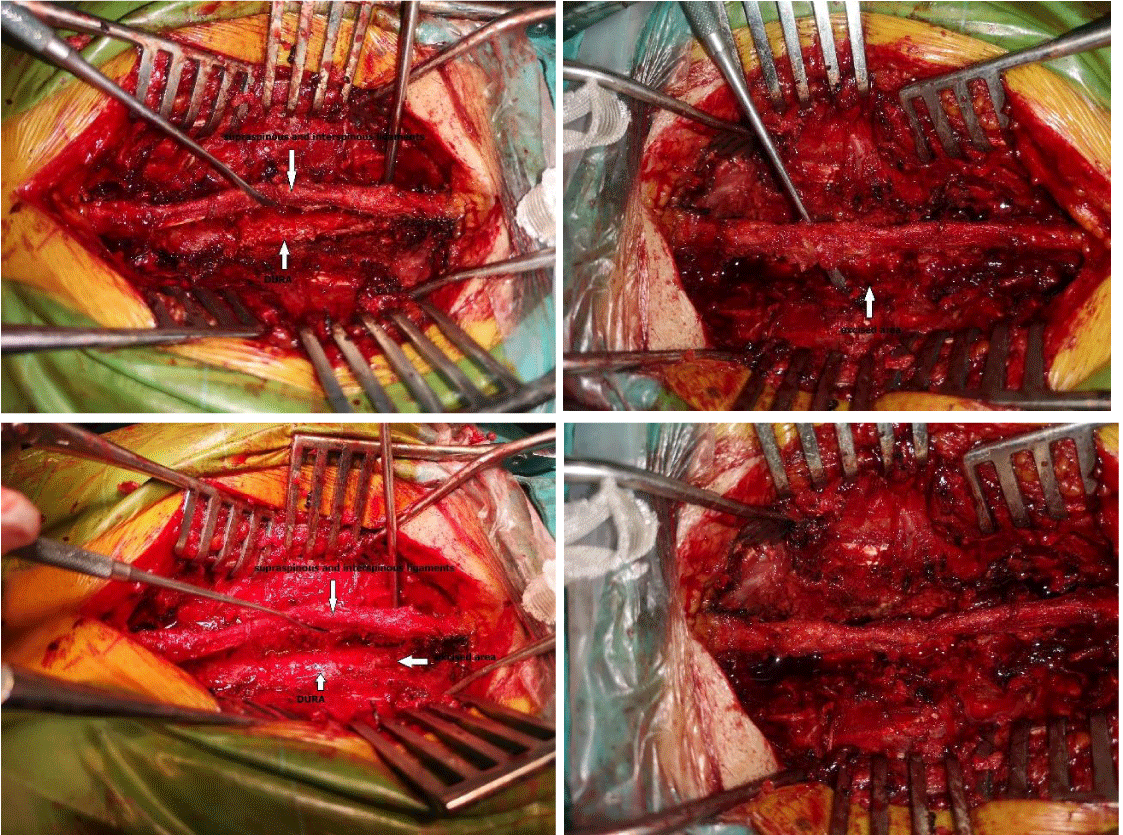
In our novel surgical method, we maintained stability without instrumentation during surgery for spine tumors. For this purpose, supraspinous ligament, interspinous ligament, and the upper part of the spinous process (1-1.5cm depending on the case) were preserved, and total laminectomy, as well as excision of the lower part of the spinous process and ligament flavum, were performed (Figures 1,2). A total laminectomy is performed by preserving the spinous process and ligaments on the laminae over the mass. The ligament was lateralized to provide wide exposure to the dura. In intradural lesions, the distal part of the preserved ligament was cut, and the proximal part was maintained (Figure 3). The lesion was excised by allowing a wide field of view for the dura and the distal part was sutured. The patients were given a corset or cervical collar for 2 months in the postoperative period.
Outcome parameters
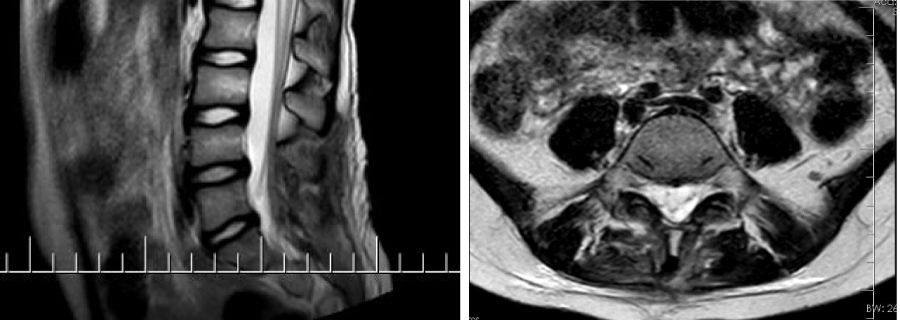
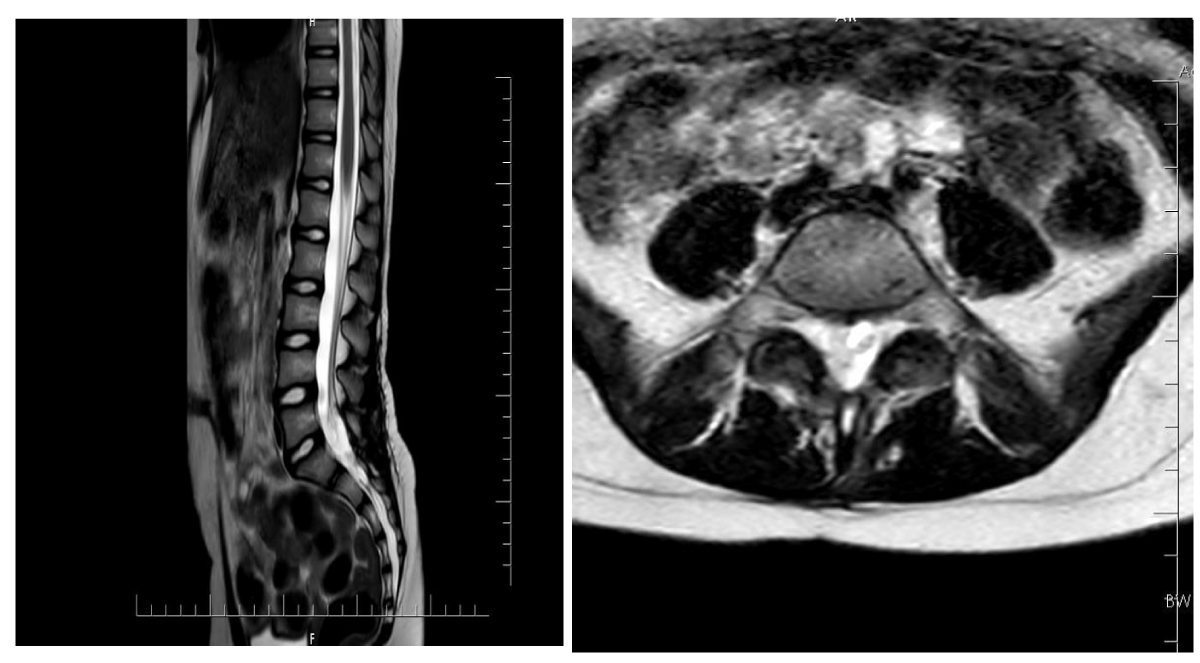
It was checked whether radiological and clinical instability developed at the 6th and 12th months postoperatively (Figures 4-6). Postoperatively, patients were asked whether they had low back and foot pain, and it was checked whether additional neurological deficits developed. In controls, it was checked whether instability developed in the spine in radiological imaging.
Statistical analysis
The data were analyzed using Statistical Package for Social Sciences program version 20.0 for Windows (SPSS, Inc., Chicago, Illinois, USA) program. Descriptive data were expressed as mean, standard deviation, minimum, and maximum values for quantitative variables, while categorical variables were shown as numbers and percentages.
Results
Our patient population consisted of n=41 patients (n=20 females, n=21 males) with an average age of 47.122±20.33 (range: 11 to 86 years). The most common complaints detected in this series were diminution of motor power in lower extremities (n=20, 47.62%), radicular pain (n=9, 21.43%), and hypoesthesia (n=2, 4.76%). The most frequent sites of involvement were L1-L2 (n=5, 11.90%), L2 (n=4, 9.52%), and T5-T6-T7 (n=2, 4.76%), respectively. Histopathologically, schwannoma (n=8, 19.94%), ependymoma (n=7, 16.64%), meningioma (n=6, 14.28%), and metastatic carcinoma (n=5, 11.90%). The distribution of tumors was intradural and extramedullary (n=27, 64.28%), intradural and intramedullary (n=13, 30.95%), and extradural (n=2, 4.77%), respectively. In 6 patients, the medial facet was removed on the side of the tumor. Bilateral facetectomy was not performed in any of the patients. Tension bands were preserved in all patients, no instability was detected during follow-up on the 6th and 12th months after surgery. Magnetic resonance imaging was performed routinely to evaluate the extension of spinal tumors. An overview of detailed demographic, clinical, radiological, and histopathological data is demonstrated in Table 1.
Discussion
This study describes the patient group in which spinal stability is preserved without instrumentation in patients who were operated on for a spinal tumor. Analysis of data collected from our patients yielded promising results with this novel procedure. The significance and worth of this procedure will become obvious as we gather further knowledge and competence about the indications and efficacy of our unique way of surgery for tumors of the spine through larger research. This method allows avoidance of instrumentation failure and associated morbidity due to additional interventions for fusion and instrumentation on spinal bones that are already fragile due to adverse effects of chemotherapy and corticosteroids on bone mineral density. In our series, the minimum duration of follow-up was 12 months.
Postoperative radiation and chemotherapy are commonly given to patients with spinal metastatic illness, which can hinder new bone development [10]. Corticosteroid therapy can lower bone mineral density and impair osseous healing potential [11]. The dietary deficiency seen in cancer patients may enhance the occurrence of complications associated with instrumentation and fusion more likely [10].
The utility of our technique, which avoids instrumentation, may diminish the operative time and amount of blood loss. Moreover, the risk of destabilization of the spinal column due to posterolateral decortication as a part of fusion will be omitted [12]. The likelihood of stimulation of tumor cells by instruments or fusion substrate may be avoided. The lack of instrumentation will save an important cost and decrease the financial burden [13]. The implementation of surgical outcome studies can be difficult when studying a condition with a low survival rate [14]. Although there is a growing tendency toward minimally invasive and short-segment constructions, such surgical procedures can lead to failure of instrumentation [15].
Patients with spinal metastatic illness are diverse. Because of their unique features, such as pathophysiology, chemotherapy regimens, and metastasis, they constitute a tough population to examine. The goals of treatment vary remarkably in these patients [5].
When there is progressive discomfort owing to spinal instability, or when either vertebral collapse or metastatic development produces spinal cord compression, surgical therapy is recommended [16]. Instability-related pain and loss of motor power are the most common presenting symptom, and it was noted in the vast majority of our patients[12].
As a result, when considering whether surgery is the best treatment, the realistic aim of pain control must be considered. The second major purpose of surgery is to decompress neural tissues so that neurologic function can be restored or preserved [6]. In patients with spine tumors, the more intensive treatment seems not to have much effect on survival [6].
Thus, less invasive, safer, and more practical procedures may be more suitable in this selected group. The expected survival rate is critical during the selection of the surgical intervention in patients with metastases. In comparison to conservative care, various studies have shown that even palliative surgery can improve the prognosis in such individuals [17]. When compared to the radiation monotherapy group, a higher percentage of operated patients kept or regained their ability to walk and required lower corticosteroid and analgesic doses, shifting the therapeutic paradigm for spinal tumors [18]. Patients with spinal tumors may have various primary pathologies, shorter survival times, and inconsistent follow-up due to morbidities or debilitation, as well as exposure to a variety of pharmacologic drugs [18]. Therefore, surgical techniques, instruments, and radiation protocols differ significantly in this subgroup [18].
Primary Spinal Cord Tumors ((SCT) are relatively uncommon in adulthood, accounting for just 2% to 4% of all primary central nervous system cancers [19,20]. Extradural SCTs account for 60% of all SCTs, 30% of intradural SCTs, and 10% of SCTs with both intradural and extradural components [4]. Within the intradural space, SCT can be divided into two types: intradural extramedullary (70%) and intradural intramedullary (30%) [19,20]. The distribution of our series was similar to these aforementioned reports.
The guidelines for fixation and instrumentation in the management of patients with spinal tumors do not currently exist. Total surgical excision is the chosen treatment for SCT because it has the best long-term results [21]. Some surgical interventions such as facetectomy [22,23] and surgery involving a spinal junction [24], are well documented to cause instability after spine surgery. Minimally invasive surgery for spinal tumors is a valuable procedure that can successfully generate good clinical results while reducing non-surgical costs when appropriate surgical indications exist [20,25]. It’s crucial to achieve a balance between the short-term morbidity risks of vigorous resection and the long-term recurrence risks of incomplete resection.
Patients with spinal tumors need a careful surgical technique and patient-specific evaluation based on cost-effectivity and minimizing risks associated with additional morbidity due to malignancy. Resection of the lesion and preservation or restoration of the structural integrity of the spine must be taken into account during tailoring the treatment plan [4].
Instrumentation, fusion, and other interventions may bring about additional risks for the fragile structure of the spine in patients with tumors[10]. Thus, we speculate that our method can be a safe and straightforward surgical alternative in selected cases with spinal tumors.
The most prevalent location of metastatic bone disease is the spinal column[19]. More than 90% of spinal cancers are metastatic lesions, with the most common sources of metastasis being the lung, breast, prostate, and kidney [26-28]. The thoracic and thoracolumbar spines are the most common sites for metastases inside the spinal neural axis (70%), followed by the lumbar spine and sacrum (20%), and the cervical spine is the least common [29]. Our results are in parallel with this report.
Neural compression and spinal fracture can occur as a result of spinal metastases, resulting in excruciating pain and neurologic impairment[28]. Decompression surgery and spinal stabilization are crucial in the treatment of spinal metastatic disease [28].
Attributed to their overall prognosis and concurrent medications, the goals of care for spinal oncology patients may differ from those for non-oncology patients [30,31]. Patients with spinal metastatic disease may not live long enough to achieve bone fusion or experience hardware failure [32,33]. As a result of constant chemotherapy, radiation therapy, and low nutritional status, their bone’s healing potential is frequently impaired [34].
Pain reduction, neurologic function preservation, prevention of progressive spinal deformity, and improved overall survival and quality of life are all goals of spine stabilization in oncology patients[26]. Fusion may not be necessary to achieve these aims in patients with spinal metastatic disease [26]. While the spine is being fused, instrumentation can only stabilize and maintain its alignment. Therefore, the implanted hardware cannot replace bony parts of the spine [35]. Instrumentation for the establishment of stability may result in loosening or fracture due to the amount of stress at the bone-screw interface, which may lead to instrument loosening or fracture [36]. There is a scarcity of research on the effectiveness of spinal stabilization without fusion or instrumentation in individuals with tumors of the spine [5].
Spinal instability was not observed in patients who underwent laminectomy at 2 levels or more with the surgical technique we applied. We anticipate that our technique will pave the way for more research into better surgical planning, care safety, patient outcomes, and cost-cutting in the medical treatment of patients with spinal tumors. However, some limitations of the current study must be remembered during the extrapolation of our results to larger populations. Retrospective and single-center design, single surgeon, heterogeneous type of tumors, Lack of clinical data such as outcomes and radiographic parameters, lack of a control group and evaluation of the quality of life after surgery, relatively short duration of follow-up, and possible impacts of socioenvironmental factors and ethnicity are weaknesses of this study.
Conclusion
To conclude, surgical management of spinal tumors is difficult, although it can provide positive, even good results. Complications and recurrence must be minimized to the greatest extent feasible, emphasizing the importance of thorough preoperative evaluations, precise surgical techniques, and knowledge-based on previous resections or surgical procedures. Our preliminary results with a novel technique that allows maintenance of stability without instrumentation yielded promising outcomes in selected patients. However, further multi-centric trials on larger series are warranted to achieve more accurate conclusions.
Statement of ethics
We declare that this research complies with the guidelines for human studies and it was conducted ethically in accordance with the World Medical Association Declaration of Helsinki.
Author contributions
İdiris Altun: Design of the study, collection of data, statistical analysis, writing, critical revision, and approval of the final version of the manuscript.
- Falicov A, Fisher CG, Sparkes J, Boyd MC, Wing PC, et al. (2006) Impact of surgical intervention on quality of life in patients with spinal metastases. Spine (Phila Pa 1976) 31: 2849-2856. Link: https://bit.ly/3v9tWQm
- Ibrahim A, Crockard A, Antonietti P, Boriani S, Bünger C, et al. (2007) Does spinal surgery improve the quality of life for those with extradural (spinal) osseous metastases? An international multicenter prospective observational study of 223 patients. Invited submission from the Joint Section Meeting on Disorders of the Spine and Peripheral Nerves, March 2007. J Neurosurg Spine 8: 271-278. Link: https://bit.ly/3sdfd5b
- Mazel C, Balabaud L, Bennis S, Hansen S (2009) Cervical and thoracic spine tumor management: surgical indications, techniques, and outcomes. Orthop Clin North Am 40: 75-92, vi-vii. Link: https://bit.ly/3LQTh7I
- Ramme AJ, Smucker JD (2011) Balancing spinal stability and future mobility in the cervical spine: surgical treatment of a case of osteoblastoma with secondary aneurysmal bone cyst. Spine J 11: e5-12. Link: https://bit.ly/3JOWOBO
- Drakhshandeh D, Miller JA, Fabiano AJ (2018) Instrumented Spinal Stabilization without Fusion for Spinal Metastatic Disease. World Neurosurg 111: e403-e409. Link: https://bit.ly/3vbiROM
- Gallazzi E, Cannavò L, Perrucchini GG, Morelli I, Luzzati AD, et al. (2019) Is the Posterior-Only Approach Sufficient for Treating Cervical Spine Metastases? The Evidence from a Case Series. World Neurosurg 122: e783-e789. Link: https://bit.ly/35ki3fy
- Nath PC, Mishra SS, Deo RC, Satapathy MC (2016) Intradural spinal arachnoid cyst: a long-term postlaminectomy complication: a case report and review of the literature. World Neurosurg 85: 367. e1-e4. Link: https://bit.ly/3t4NbrA
- Miyakoshi N, Hongo M, Kasukawa Y, Shimada Y (2015) En-bloc resection of thoracic calcified meningioma with inner dural layer in recapping T-saw laminoplasty: a case report. BMC Surg 15: 82. Link: https://bit.ly/3BHAabq
- Sun S, Li Y, Wang X, Lu G, She L, et al. (2019) Safety and Efficacy of Laminoplasty Versus Laminectomy in the Treatment of Spinal Cord Tumors: A Systematic Review and Meta-Analysis: World Neurosurg 125: 136-145. Link: https://bit.ly/3pbEH10
- Itshayek E, Cohen JE, Yamada Y, Gokaslan Z, Polly DW, et al. (2014) Timing of stereotactic radiosurgery and surgery and wound healing in patients with spinal tumors: a systematic review and expert opinions. Neurol Res 36: 510-523. Link: https://bit.ly/3JMOXEO
- Sawin PD, Dickman CA, Crawford NR, Melton MS, Bichard WD, et al. (2001) The effects of dexamethasone on bone fusion in an experimental model of posterolateral lumbar spinal arthrodesis. J Neurosurg 94: 76-81. Link: https://bit.ly/3vbtj9g
- Dai LY, Jiang LS, Jiang SD (2009) Posterior short-segment fixation with or without fusion for thoracolumbar burst fractures. a five to seven-year prospective randomized study. J Bone Joint Surg Am 91: 1033-1041. Link: https://bit.ly/3paGaEz
- Wang ST, Ma HL, Liu CL, Yu WK, Chang MC, et al. (2006) Is fusion necessary for surgically treated burst fractures of the thoracolumbar and lumbar spine?: a prospective, randomized study. Spine 31: 2646-2652. Link: https://bit.ly/36t7ozL
- Tian NF, Wu YS, Zhang XL, Wu XL, Chi YL, et al. (2013) Fusion versus nonfusion for surgically treated thoracolumbar burst fractures: a meta-analysis. PLoS One 8: e63995. Link: https://bit.ly/3hew8he
- Logroscino CA, Proietti L, Tamburrelli FC (2009) Minimally invasive spine stabilisation with long implants. Eur Spine J 18: 75-81. Link: https://bit.ly/36t7szv
- Quan GM, Vital JM, Pointillart V (2011) Outcomes of palliative surgery in metastatic disease of the cervical and cervicothoracic spine. J Neurosurg Spine 14: 612-618. Link: https://bit.ly/3sf38fY
- Mavrogenis AF, Guerra G, Romantini M, Romagnoli C, Casadei R, et al. (2012) Tumours of the atlas and axis: a 37-year experience with diagnosis and management. Radiol Med 117: 616-635. Link: https://bit.ly/3h7ccgz
- Harel R, Chao S, Krishnaney A, Emch T, Benzel EC, et al. (2010) Spine instrumentation failure after spine tumor resection and radiation: comparing conventional radiotherapy with stereotactic radiosurgery outcomes. World Neurosurg 74: 517-522. Link: https://bit.ly/3JNlp9R
- Chamberlain MC, Tredway TL (2011) Adult primary intradural spinal cord tumors: a review. Curr Neurol Neurosci Rep 11: 320-328. Link: https://bit.ly/3vbiLqo
- Avila MJ, Walter CM, Skoch J, Abbasifard S, Patel AS, et al. (2015) Fusion after intradural spine tumor resection in adults: A review of evidence and practices. Clin Neurol Neurosurg 138: 169-173. Link: https://bit.ly/3tkRhwf
- Zadnik PL, Gokaslan ZL, Burger PC, Bettegowda C (2013) Spinal cord tumours: advances in genetics and their implications for treatment. Nat Rev Neurol 9: 257-266. Link: https://bit.ly/3HdegOy
- Jaumard NV, Welch WC, Winkelstein BA (2011) Spinal facet joint biomechanics and mechanotransduction in normal, injury and degenerative conditions. J Biomech Eng 133: 071010. Link: https://bit.ly/3Id7qdd
- Kiapour A, Ambati D, Hoy RW, Goel VK (2012) Effect of graded facetectomy on biomechanics of Dynesys dynamic stabilization system. Spine (Phila Pa 1976) 37: E581- E589. Link: https://bit.ly/352hpnk
- Steinmetz MP, Miller J, Warbel A, Krishnaney AA, Bingaman W, et al. (2006) Regional instability following cervicothoracic junction surgery. J Neurosurg Spine 4: 278-284. Link: https://bit.ly/3vftm3F
- Zong S, Zeng G, Du L, Fang Y, Gao T, et al. (2014) Treatment results in the different surgery of intradural extramedullary tumor of 122 cases. PLoS One 9: e111495. Link: https://bit.ly/3v5CCaC
- Lee CS, Jung CH (2012) Metastatic spinal tumor. Asian Spine J 6: 71-87. Link: https://bit.ly/3IgkBdt
- Ciftdemir M, Kaya M, Selcuk E, Yalniz E (2016) Tumors of the spine. World J Orthop 7: 109-116. Link: https://bit.ly/35mK1Y3
- Klimo P, Schmidt MH (2004) Surgical management of spinal metastases. Oncologist 9: 188-196. Link: https://bit.ly/3HiBL8J
- Fanous AA, Fabiano AJ (2017) Surgical management of spinal metastatic disease. J Neurosurg Sci 61: 316-324. Link: https://bit.ly/3saCB3i
- McPhee IB, Williams RP, Swanson CE (1998) Factors influencing wound healing after surgery for metastatic disease of the spine. Spine 23: 726-732. Link: https://bit.ly/3BNatpZ
- Sundaresan N, Rothman A, Manhart K, Kelliher K (2002) Surgery for solitary metastases of the spine: rationale and results of treatment. Spine (Phila Pa 1976) 27: 1802-1806. Link: https://bit.ly/3sdMEon
- Onimus M, Papin P, Gangloff S (1996) Results of surgical treatment of spinal thoracic and lumbar metastases. Eur Spine J 5: 407-411. Link: https://bit.ly/3JQuqyS
- Wibmer C, Leithner A, Hofmann G, Clar H, Kapitan M, et al. (2011) Survival analysis of 254 patients after manifestation of spinal metastases: evaluation of seven preoperative scoring systems. Spine (Phila Pa 1976) 36: 1977-1986. Link: https://bit.ly/3hbk4gY
- Vrionis FD, Small J (2003) Surgical management of metastatic spinal neoplasms. Neurosurg Focus 15: E12. Link: https://bit.ly/3HbrmMb
- Nouh MR (2012) Spinal fusion-hardware construct: Basic concepts and imaging review. World J Radiol 4: 193-207. Link: https://bit.ly/352hmYG
- Galbusera F, Volkheimer D, Reitmaier S, Berger-Roscher N, Kienle A, et al. (2015) Pedicle screw loosening: a clinically relevant complication? Eur Spine J 24: 1005-1016. Link: https://bit.ly/3LWtn2k
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.



 Save to Mendeley
Save to Mendeley
