International Journal of Spine Research
The Lateral Approach in Lumbar Total Disc Replacement: A Literature Review
Ahmad Amer1, Yazan Issa1, Devan O Higginbotham2*, Abdul Zalikha2 and Scott McCarty2
2Department of Orthopedic Surgery, Detroit Medical Center, Detroit, MI 48201, USA
Cite this as
Amer A, Issa Y, Higginbotham DO, Zalikha A, McCarty S (2021) The Lateral Approach in Lumbar Total Disc Replacement: A Literature Review. Int J Spine Res 3(1): 004-010. DOI: 10.17352/ijsr.000019Lumbar disc replacement has become an area of interest for many practicing spine surgeons. As newer technology emerges focusing on motion sparing devices, novel techniques are being employed to better serve patients and increase post-operative outcomes. Traditionally, the anterior approach is utilized in total disc arthroplasty of the lumbar spine, although many are beginning to favor the use of a lateral approach. The lateral approach not only allows for the maintenance of the Anterior Longitudinal Ligament (ALL), but also avoids the great vessels during surgery which are encountered in the traditional anterior approach. Research has shown the lateral approach in total disc replacements (TDR) of the lumbar spine to be a not inferior alternative to the anterior approach, with long-term pain relief and a low complication rate.
Introduction
Lumbar Total Disc Replacement (TDR) has been shown to be safe and effective treatment of lumbar discogenic Low Back Pain (LBP) caused by Degenerative Disc Disease (DDD). The efficacy and safety of lumbar TDR devices has been demonstrated in studies recorded over the past decade [1-4]. The fundamental rationale for performing Total Disc Replacement (TDR) instead of fusion is preservation of motion. Theoretically, preservation of segmental motion may prevent the development of Adjacent Level Degeneration (ALD) seen in long-term follow-up of fusions [5].
Thousands of lumbar TDRs are conducted in the United States every year, costing approximately $23,000-35,000 per patient [6,7]. There is a growing consensus that lumbar TDR is a durable and appropriate surgical option for lumbar degenerative disc disease, especially for those who are younger and have less co-morbidities [8-10]. Lumbar TDR could be an improved alternative treatment for lumbar disc degenerative disease from traditional lumbar fusion procedures, since it has yielded better clinical success and patient satisfaction, reduced rates of adjacent segment degeneration, need for additional surgery, shorter hospital stay and operative time, less pain, and lower complication rates than lumbar fusion [11,12] Traditionally, TDR devices are implanted via the anterior approach, with the primary indication being symptomatic degenerative disc disease (DDD) [13] Dr. Ulf Fernstrom first implanted a lumbar disc prosthesis in the 1950s via the anterior approach. The degenerated nucleus was excised and a steel ball implanted to maintain disc height and motion [13].
However, new procedures have been devised to circumvent the inherent disadvantages of the anterior approach. One major drawback of the anterior approach is the need to conduct an extensive annulotomy and excise the anterior longitudinal ligament (ALL) to properly remove the nucleus for implantation of the device [14]. In doing so, the biomechanics of the spine can be negatively impacted, leading to worsened patient outcomes [14]. Anteriorly implanted devices are therefore unstable due to the removal of the ALL and annulus, with this instability manifesting itself as increased range-of-motion (ROM)thereby increasing facet stresses [14]. In lumbar total disc replacements, infection and severe dislocations have been reported as the most frequent causes of anterior revisions [15], Other reported complications include sympathetic dysfunction, vascular injury, somatic neural injury, sexual dysfunction, prolonged ileus, wound incompetence, deep vein thrombosis, acute pancreatitis, and bowel injury [16]. These issues elicited the need for a novel approach to TDR procedures, namely, the lateral approach. The posterior approach has seen recent interest in being utilized. Sielatycki has been able to show at 1 year, the LTJR cohort showed significant improvement in ODI and NRS back and leg pain as compared to TLIF [17].
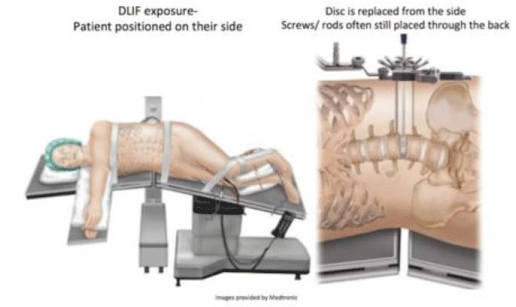
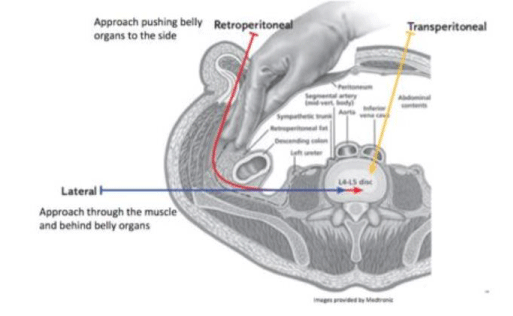
The lateral approach was first described by Bertagnoli and Vazquez (2003)[18]. The procedure is conducted as follows: first, the patient is placed in a 90° lateral decubitus position on a radiolucent breaking table. The table is slightly flexed to arch the patient on their side (Figure 1). K-wire and C-arm fluoroscopy are used to identify the exact location of the target disc. An incision is made in the lateral region over the target disc and the latero-abdominal muscles are bluntly dissected (Figure 2). The retroperitoneal area is then accessed and followed to the psoas muscles, where the muscle fibers are dilated to access the target disc. The annulus is cut and a flap is created allowing the surgeon to excise the nucleus pulposus and implant the TDR into the disc cavity. The flap is then sutured over the nucleus and the wound closed [18]. Other researchers report conducting a box annulotomy followed by a discectomy, not the creation of a flap [19,20].
The lateral approach is beneficial in three main areas according to the International Society for the Study of the Lumbar Spine: surgical approach, biomechanics, and invasiveness.19 The approach avoids the great vessels, eliminating associated complications and the need for an access surgeon [19].
Regarding biomechanics, the lateral approach maintains the stabilizing ligaments, including the ALL. Maintaining the ALL is theorized to prevent wear debris, decrease central stenosis, and protect against adjacent level degeneration and facet joint degradation [19] The third advantage is the minimal invasiveness compared to other approaches. Studies have shown those who underwent lateral procedures experienced less blood loss, less muscle atrophy, and shorter hospital stays and recovery times [19]. The lateral approach does carry drawbacks. Because the iliac crest prohibits lateral access to the spine, this approach does not work for surgeries at the L5-S1 segment. Therefore, an alternative approach must be employed. The presence of a rising psoas can also increase the risk for nerve injuries and is a contraindication to this approach [19].
This review aims to gather all existing literature on the lateral approach to lumbar disc replacement to help determine the viability of that approach and compare it to the traditional anterior approach. A summary of key clinical findings is found in Table 1.
The Anterolateral TransPsoatic Approach (ALPA): A New technique for implanting prosthetic disc-nucleus devices (2003) [18].
Bertagnoli and Vazquez [18] are considered the pioneers of the lateral approach to lumbar TDRs. The development of this method came from their perceived need to avoid damage to the posterior structures of the spine and to more easily implant the TDR device [18]. They analyzed patients with DDD at L2-L4 and did not respond to conservative treatment. Eight patients were selected with seven receiving implants at L4-L5 and one at L2-L3. The devices were implanted and the patients were kept in a recumbent position for a day in postoperative care.
Several complications were reported post-procedure. Four patients experienced transient neuropraxia in the psoas muscle that dissipated after three months. The authors speculated this was due to disruption of muscle fibers and associated nerves during dissection of the psoas muscle. However, prevalence of these neurological symptoms decreased as the surgeon gained experience with the procedure. Forward protrusions of the device were reported in three patients, two of which had “small” disc spaces and should have been implanted with one rather than two devices. In one of those patients, the device was removed and a fusion conducted due to endplate subsidence and a decrease in disc height.
The researchers monitored pain, work capability, and disc height in the other seven patients for a year. They reported significant improvements in Oswestry and Prolo scores and increases in disc height. Two patients, including the patient whose device was explanted, were considered failures due to poor clinical outcomes.
The results of this study suggest the lateral approach is a strong alternative to the anterior and posterior approaches. The researchers point to three main advantages: 1) Minimized disturbance to posterior structures, 2) A simplified procedure that does not need an access surgeon, and 3) Maintaining the annulus and posterior longitudinal ligament prevented the device from moving into the spinal canal.
Charité lumbar artificial disc retrieval: use of a lateral minimally invasive technique (2006)[20] 8.8% of patients implanted with the Charité lumbar artificial disc require replacement or revision of the device due to loosening, instability, early wear, or infection [18]. Approaches to revision of TDRs closely follows that of the implantation of the device. In 2006, Pimenta, et al. sought to investigate the effectiveness of a lateral, minimally invasive technique for Charité artificial disc retrieval and revision in a case series of two patients [20]. The devices of both patients were originally placed anteriorly.
The first case was a 39-year-old woman with L4–5 DDD and back pain due to TDR instability. The second was a 50-year-old woman with L3-4 disease with lumbar pain due to improper positioning of her implanted device. The first patient recovered well with no infection or neurological symptoms in the post-operative period. At the one-year follow-up, the patient was well and without complaints or pain. The second patient developed idiopathic transitory weakness in a knee-raising exercise that was resolved by the third day of recovery. No issues or complaints were reported at the ten-month follow-up.
This study demonstrated that the lateral approach provides sufficient exposure for removal and revision of a lumbar TDR device. This lateral approach allowed surgeons to avoid adhesions created by the anterior approach and does not require movement of the great vessels.
Access strategies for revision or explantation of the Charité lumbar artificial disc replacement (2006) [21].
In 2006, Wagner, et al. performed a retrospective case series of 19 patients with prior disc implantation requiring either repositioning or removal [21]. The discs were removed/revised successfully in all patients. 3/12 of the L5-S1 procedures were done using the retroperitoneal (anterolateral) approach that was used for the initial implantation. One of the three was changed to a transperitoneal approach to avoid adhesions. Four of the L4-5 procedures were conducted using the original approach while five were done through the lateral, transpsoas approach. The only procedure conducted at L3-4 was through the lateral, transpsoas approach. Some minor complications were reported but all resolved soon afterwards with no cases of permanent neurologic issues, deep vein thrombosis, or death [21].
Major arterial/venous injuries occur in 2-5% of anterior lumbar procedures. Repeat exposure of the lumbar spine via the anterior approach significantly increases the risk of retrograde ejaculation, probably due to the bilateral mobilization of sympathetic fibers. This issue as well as denervation injuries in general are not associated with the lateral approach. The lateral approach allows for leaving the L4-5 region undisturbed for future surgeries, in case the need arises. Therefore, the surgeons reported that the best way to conduct revisions of the Charité device at L3-4 and L4-5 is through the lateral approach.
A Comparison of two retroperitoneal surgical approaches for total disc arthroplasty of the Lumbar Spine (2008) [22]
Bendo, et al. sought to determine whether there is a significant difference between the midline rectus (MR) and paramedian lateral rectus (PLR) approach and to establish that a suboptimal implant position affects clinical outcomes [22]. All procedures were performed by one of two surgeons. One surgeon exclusively used the MR approach for L5-S1 cases, while the other used the MR approach for L5-S1 cases and PLR approach for L4-L5 cases. For all patients, measurements were taken for displacement from the midline in the coronal and sagittal planes as well as for quality of life, the Oswestry Disability Index (ODI), and Visual Analog Scale (VAS) [22].
In the coronal plane, there was no significant difference between the approaches in midline displacement. However, there was a significant difference in the sagittal plane. The PLR showed an average anterior displacement of 3.3 mm compared to 1.6 mm with the MR. The authors argued that this indicates a superiority of the MR approach.
XLIF--a New technique of the lumbar vertebra disc replacement: Initial experience (2010) [23]
Hrabálek, Wanek, and Adamus (2010), Czech researchers at the University Hospital Olomouc conducted clinical trials of the XLIF technique for lumbar disc replacements [23]. The surgeons briefly discussed their thoughts on the lateral approach to lumbar TDR in a published abstract. Eleven patients with either symptomatic DDD or failed back surgery syndrome enrolled in their study. The surgeons reported that lateral access to the lumbar spine avoids major vessels and nerves that are at risk with an anterior approach. Additionally, they conclude it allows placement of the implant in the anterior and bilateral position, providing sagittal and coronal plane imbalance correction, contributing to the maintained stability of the lumbar spine [23].
Lumbar total disc replacement from an extreme lateral approach: Clinical experience with a minimum of 2 years’ follow-up (2011) [24]
Pimenta, et al. investigated the clinical and radiographic outcomes of the lateral approach to lumbar TDR by conducting a prospective, single-center study. 36 patients diagnosed with DDD underwent TDR via the true lateral, retroperitoneal, transpsoas approach (XLIF) [24]. Outcome measurements included pain, function and ROM. Data was recorded before, after, and up to two years after the procedure. The surgeries included 15 single-level TDR procedures at L3-4 or L4-5, three 2-level TDR procedures spanning L3-4 and L4-5 and 18 hybrid procedures (anterior lumbar interbody fusion at L5-S1 and TDR at L4-5 or L3-4)[24].
Most patients were walking within 12 hours of the surgery and discharged within 1.5 days. Post-surgery neurological exams were conducted with patients reporting psoas weakness (5, 13.8%), anterior thigh numbness (3, 8.3%), and other musculoskeletal problems (5, 13.8%). All post-surgical complications were resolved within weeks of being discharged with no lasting neurological symptoms at the 2-year point. VAS pain scores decreased significantly and as per the Odom criteria, 80% of patients had “good” or “excellent” results at the 2-year follow-up.
Radiographic outcomes were similarly positive with evidence of proper device placement and restoration of disc height, foraminal volume, and sagittal balance. ROM did not increase significantly pre- and post-operatively, suggesting maintained spinal stability.
This study demonstrates pain relief and improved functionality. The unique advantages of the lateral approach to the lumbar spine including minimal morbidity, the preservation of stability through preservation of the ALL, a more biomechanically stable orientation, and more revision options. These advantages make the lateral transpsoas approach a strong alternative to the traditional anterior approach.
Lumbar total disc replacement by less invasive lateral approach: A report of results from two centers in the US IDE clinical trial of the XL TDR device (2015) [25]
While early reports of the lateral approach involved revision of anterior TDR devices, the lateral approach has increasingly become the primary method of TDR in attempt to decrease the morbidity associated with disc fusion. This follow-up study reports results from a two-center study focusing on the lateral approach as the primary treatment for 64 patients [22]. After initial baseline measurements before, during, and after surgery, measurements were also taken 1.5, 3, 6 and 12 months later, then annually up to three years. Measures included the VAS for pain, ODI, and mental and physical component satisfaction scores as well as radiography to check for disc height and placement [25].
All time points and measures showed a significant improvement from baseline, starting at six weeks. By the two-year Follow Up Point (FUP), VAS pain scores were improved in 47/60 patients and 40/60 patients for back and leg pain respectively, with 26/30 and 19/30 at the three-year FUP. ODI scores improved in 53/60 patients at and 27/30 at two- and three-year FUP respectively. SF-36 MCS and PCS scores were improved in 35/60 and 52/60 respectively at two years, and 19/30 and 26/30 at three. The researchers noted that among post-op patients, 22/60 reported using no pain medication, up from 10/60 at baseline, as well as narcotic use decreasing from 31/60 at baseline to 16/60 at last FUP.
Radiography showed the average disc height increased post-op from 7.2mm (SD 2.0) to 12.1mm (SD 1.9), and at three-year FUP was 10.7mm (SD 1.0). Only three patients showed HO interfering with segmental motion, with no mention of HO without interference. No significant change in flexion/extension range was reported compared to baseline, and at three years FUP was 5.9(SD 4.8). Further complications included one patient with significant subsidence, who otherwise reported no pain at the three-year FUP.
1 patient presented with significant back pain (rated 82/100) and right leg pain (92/100) due to disc collapse, foraminal stenosis, and DDD. Post-op disc height increased from 3.8mm to 12.4mm and at three-year FUP, the patient reported 0/100 pain for both measures, with intact flexibility and 10/10 satisfaction with the treatment.
Overall, the study showed significant improvements in patient satisfaction and supported the idea that the lateral approach provides a low complication and morbidity rate.
Controlled motion with the XL-TDR lateral-approach lumbar total disk replacement: In Vitro kinematic investigation (2015) [26]
Pimenta, et al. [26] reported on the kinematics of the XL-TDR device in cadavers. They conducted a cadaveric study to investigate the kinematics of the XL-TDR device and the contribution of the ALL and annulus to spinal stability, thereby assessing the lateral transpsoas and anterior approaches to the lumbar spine in TDR. L2-S1 were dissected from six cadavers and excess muscle and fat tissue was removed [16].
Intervertebral motions were tracked three-dimensionally using an optoelectronic system and each specimen underwent nondestructive multidirectional testing with the protocol devised by Panjabi, et al. [26]. Specimens were tested in the intact condition in flexion-extension, left-right lateral bending, and left-right axial rotation to moments of 8 nm. The range of motion (ROM) of the entire specimen in each direction was recorded. Afterwards, a number of conditions were tested to compare procedure techniques: XL-TDR at L4-5 and XL-TDR at L4-5 with resection of the ALL and annulus. Both of the test conditions underwent three full motion cycles in each direction and the neutral zone (NZ) and ROM values were recorded. The NZ is defined as the physiologic range of motion of high laxity, being the movement performed with minimal internal resistance. A higher NZ relates to a less stable spine segment.
There were statistically significant increases in both ROM and NZ when the ALL and annulus were resected versus when they remained intact. This was the case in all tested directions. The lateral approach XL-TDR device decreased ROM in all directions, with a NZ closer to intact in all movements as well. These results demonstrated the stabilizing role of the ALL and annulus and the benefit of maintaining them after a TDR procedure is conducted.
Two-level lumbar total disc replacement: Functional outcomes and segmental motion after 4 years (2015) [27]
Trincat, et al. sought to evaluate the complications and outcomes in patients who had undergone two-level TDR. This was a retrospective study on patients who had received a two-disc replacement at either L4/L5+L5/S1 or L3/L4+L4/L5. Both procedures were done through the left, right, or bilateral anterolateral approach [27].
In both categories, patients showed significant decreases in ODI (25 to 12), lumbar VAS (7.1 to 2.8), and radicular VAS scores (5.4 to 2.6) post-op. Motion was preserved in both levels in 74% of cases, preserved in one in 21% of cases, and in neither in 7% of cases.
There were three implant-related complications: one unclipping of the device core and two patients experienced implant subsidence. The other 17 complications included 3 iliac vein wounds, 4 retroperitoneal hematomas, 5 UTIs, 1 L5 radicular deficiency, 1 dura mater wound, 2 DVTs, and 1 wound dehiscence. 2.8% of patients required an early revision to fusion.
While devices showed decreases in pain and disability indexes, the researchers noted that 7% of patients did have complete disc freezing. The common cause of this issue was the quality of device positioning and its distance from the spinal midline.
Early experience with lateral lumbar total disc replacement: Utility, complications and revision strategies (2017) [28].
This prospective cohort study of 12 patients sought to focus on the viability of the lateral approach using the XL-TDR device and provide cases and examples of outcomes, revisions, and complications. 12 patients received a disc replacement, and investigations were made into pain and disability measures (VAS and ODI), flexion/extension, CT to look for facet arthropathy, MRI for neural compression, bone scan to identify any disc pathology, and bone density scans [25].
Initial clinical scores show significant improvement in all measures. VAS for back and leg decreased from 6.5 (SD 1.8) and 4.7 (SD 2.1) pre-op to 1.7 (SD 2.5) and 1.8 (SD 2.0) respectively at last follow up point. ODI scores showed decreases from a pre-op score of 53.0 (SD 18.7) to 16.5 (SD 16.4). Physical and mental satisfaction scores increased from 30.8 (SD 5.9) and 37.3 (SD 14.1) pre-op to 46.3 (SD 8.8) and 52.0 (SD 11.9), respectively. Patients showed an average return to work time of 18.8 weeks. Among the ten patients who retained their disc replacement, six returned to their presurgical work, three returned to alternative employment, and 1 was unable to return to work. None were taking opiate analgesics at last follow up.
Complications occurred in 6 patients. 1 patient had a wound infection and 2 patients experienced thigh dysesthesia that resolved within three months. 1 patient had a new motor extremity deficit, which the researchers make no mention of resolving, and 2 required a conversion to fusion due to early dislocation.
1 case-study included a 41-year-old male with a 13-year history of back pain. Previous abdominal hernia repairs meant a contraindicated anterior approach, making the lateral approach the only option. The patient ceased all opiate analgesia by four weeks post-operation and returned to work at 14 weeks, with VAS and ODI scores of 0 by 12 months. Another case involved a 39-year-old male with a history of 1.5 years of back pain due to a work injury. By two weeks post-op, all opiate analgesics had ceased, and the patient returned to work six months later.
2 cases show complications in dislocation requiring revision to a fusion. A 28-year-old female underwent a TDR, and two days post-op suffered a dislocation that required revision due to undersizing of the prosthesis. She presented with sudden onset left abdominal and flank pain with left hip radiation. Imaging showed dislocation into the left psoas muscle. In another case, a 27-year-old farmer suffered a dislocation 8-weeks post-op while performing manual labor due to under-sizing of the prosthetic. The patient delayed coming into the clinic until 14 months post-op where CT showed dislocation of the prosthetic into the right psoas muscle.
The researchers concluded that, overall, the lateral approach is a minimally invasive and viable alternative to the anterior approach.
Lumbar Total Disc Replacement by the Lateral Approach - Up to 10 Years Follow-Up (2019) [28]
Porkorny, et al. [28] performed a prospective study of 60 patients with a focus on the stability provided by the lateral approach’s lack of ALL and great vessel mobilization. Up to five-year follow-ups were conducted after a lateral transpsoas TDR. Clinical end points included patient-reported assessments, clinical examination using VAS and ODI scores, and radiography to measure heterotopic ossification (HO) and track device migration over time [29].
VAS scores declined at week one follow-up, from an average of 88/100 to 25/100, then a slight increase to 33/100 at the five-year follow-up. The ODI dropped from 55.4 to 31.1 at week one, then again to 22.1 at five-years. HO has been a common issue in TDRs. The largest group of patients (31%) showed osteocyte growth along plate lines that did not inhibit movement. Overall, 82% of patients had HO that did not interfere with motion. Interestingly, while every patient with HO present had HO occur in the lateral part of the disc, 64% had it occur in the contralateral side to the approach, with 33% bilateral HO and only 3% ipsilateral.
5 discs required full retrieval and revision. 4 due to pain (2 attributed to incorrect disc sizing) and one due to an allergic reaction to the prosthesis. Other issues included stenosis at the interbody fusion levels (1 patient), untreatable pain at the sacroiliac joint (1 patient), and adjacent lumbar disease (2 patients).
The authors concluded that the procedure showed sustained and immediate pain relief alongside a low rate of revision and complications in treating DDD. Furthermore, while 91% of patients showed some grade of HO, it was not directly correlated with poorer outcomes.
Discussion
Multiple studies [20,25,29] have shown the lateral approach allows for quick mobilization post-operation, faster recovery times, significant decreases in pain, and improvements in quality of life. This is partially due to the lateral approach making it unnecessary to mobilize the great vessels and avoiding damage to the ALL. Furthermore, its utility in revisions for replacement by both the anterior and lateral approach can prevent further adhesions and complications. However, multiple issues remain. Despite the low complication rate, the complications share a similar etiology. The operation depends heavily on the exact placement of the prosthetic in the middle of the spine rotational axis. There remains no reproducible, consistent method of measuring exact placement, as it heavily relies on surgeon experience [29]. Similarly, researchers found that lateral dislocation of the prosthetic led to severe acute pain and required revisions and fusions. However, there were no noted long-term complications of these dislocations [28,30]. The underlying issue is commonly attributed to prosthesis under-sizing, and no standardized way of measuring and fitting disc prosthetics has been described. Furthermore, gaps exist on how heterotopic ossification (HO) can be minimized to prevent long term calcification, however Pokorny, et al. [28] showed little correlation between extent of HO and worsened outcomes.
A randomized control study has yet to be performed directly comparing the anterior and lateral approaches and remains difficult to determine which is superior. Bendo, et al. [22], argues that the lateral approach may be inferior, as it leads to worse mid-axial deviation and therefore worsened outcomes. Furthermore, while TDR is seeing an increased use, fusion still remains the gold standard for DDD and there is no research directly comparing the two methods, nor the inverse indicating replacement over fusion. Overall, the literature shows the lateral approach to a TDR to be a safe, effective, and not inferior method of treating DDD when compared to the anterior approach.
Conclusion
This review documents the evolution and close follow up of patients who have undergone lumbar total disk replacement since inception. Lumbar total disk replacement via the lateral approach has proven to be a non-inferior technique with fewer complications and greater pain relief for index procedures. Utilization of the lateral approach should be based upon a surgeon’s familiarity and experience to achieve best outcomes. Additional higher-level studies comparing both the anterior and lateral approach in lumbar total disk replacement is warranted as implant design continues to improve.
- Guyer RD, McAfee PC, Banco RJ, Bitan FD, Cappuccino A, et al. (2009) Prospective, randomized, multicenter Food and Drug Administration investigational device exemption study of lumbar total disc replacement with the CHARITE artificial disc versus lumbar fusion: five-year follow-up. Spine J 9: 374–386. Link: https://bit.ly/3A1YTpM
- Gornet MF, Burkus JK, Dryer RF, Peloza JH, Schranck FW, et al. (2019) Lumbar disc arthroplasty versus anterior lumbar interbody fusion: 5-year outcomes for patients in the Maverick disc investigational device exemption study. J Neurosurg Spine 31: 347–356. Link: https://bit.ly/3h5Wmnf
- Zigler JE, Delamarter RB (2012) Five-year results of the prospective, randomized, multicenter, Food and Drug Administration investigational device exemption study of the ProDisc-L total disc replacement versus circumferential arthrodesis for the treatment of single-level degenerative disc disease. J Neurosurg Spine 17: 493–501. Link: https://bit.ly/35YA9Rn
- Guyer RD, Pettine K, Roh JS, Dimmig TA, Coric D, et al. (2016) Five-Year Follow-Up of a Prospective, Randomized Trial Comparing Two Lumbar Total Disc Replacements. Spine 41: 3–8. Link: https://bit.ly/3w1I3nF
- Huang RC, Tropiano P, Marnay T, Girardi FP, Lim MR, et al. (2006) Range of motion and adjacent level degeneration after lumbar total disc replacement. Spine J 6: 242-247. Link: https://bit.ly/3gYjX96
- Saifi C, Cazzulino A, Park C, Laratta J, Louie PK, et al. (2018) National Trends for Primary and Revision Lumbar Disc Arthroplasty Throughout the United States. Global Spine J 8: 172–177. Link: https://bit.ly/3jmwg0C
- Levin DA, Bendo JA, Quirno M, Errico T, Goldstein J, et al. (2007) Comparative charge analysis of one- and two-level lumbar total disc arthroplasty versus circumferential lumbar fusion. Spine 32: 2905–2909. Link: https://bit.ly/3qu9SE5
- Kurtz SM, Lau E, Ianuzzi A, Schmier J, Todd L, et al. (2010) National revision burden for lumbar total disc replacement in the United States: epidemiologic and economic perspectives. Spine 35: 690–696. Link: https://bit.ly/3hdRATb
- Perfetti DC, Galina JM, Derman PB, Guyer RD, Ohnmeiss DD, et al. (2021) Risk factors for reoperation after lumbar total disc replacement at short-, mid-, and long-term follow-up. S1529-9430(21)00107-8. Link: https://bit.ly/3A8mrcv
- Zigler J, Gornet MF, Ferko N, Cameron C, Schranck FW, et al. (2018) Comparison of Lumbar Total Disc Replacement With Surgical Spinal Fusion for the Treatment of Single-Level Degenerative Disc Disease: A Meta-Analysis of 5-Year Outcomes From Randomized Controlled Trials. Global Spine J 8: 413–423. Link: https://bit.ly/3vZ5Fti
- Li YZ, Sun P, Chen D, Tang L, Chen CH, et al. (2020) Artificial Total Disc Replacement Versus Fusion for Lumbar Degenerative Disc Disease: An Update Systematic Review and Meta-Analysis. Turkish Neurosurgery 30: 1–10. Link: https://bit.ly/3x5i5RB
- Buser Z, Chung AS, Abedi A, Wang JC (2019) The future of disc surgery and regeneration. International orthopaedics 43: 995–1002. Link: https://bit.ly/3qwikmd
- Salzmann SN, Plais N, Shue J, Girardi FP (2017) Lumbar disc replacement surgery-successes and obstacles to widespread adoption. Curr Rev Musculoskelet Med 10: 153–159. Link: https://bit.ly/3xRmp74
- Marchi L, Oliveira L, Coutinho E, Pimenta L (2012) The importance of the anterior longitudinal ligament in lumbar disc arthroplasty: 36-Month follow-up experience in extreme lateral total disc replacement. Int J Spine Surg 6: 18–23. Link: https://bit.ly/35SKHSe
- Cecchinato R, Bourghli A, Obeid I (2020) Revision surgery of spinal dynamic implants: a literature review and algorithm proposal. Eur Spine J 29: 57–65. Link: https://bit.ly/3qtjr64
- Pimenta L, Turner A, Oliveira L, Marchi L, Cornwall B (2015) Controlled motion with the XL-TDR lateral-approach lumbar total disk replacement: in vitro kinematic investigation. J Neurol Surg A Cent Eur Neurosurg 76: 133–138. Link: https://bit.ly/3gXVdhm
- Alex Sielatycki J, Devin CJ, Pennings J, Koscielski M, Metcalf T, et al. (2021) A novel lumbar total joint replacement may be an improvement over fusion for degenerative lumbar conditions: a comparative analysis of patient-reported outcomes at one year. Spine J 21: 829–840. Link: https://bit.ly/2TfuOT9
- Bertagnoli R, Vazquez RJ (2003) The Anterolateral TransPsoatic Approach (ALPA): a new technique for implanting prosthetic disc-nucleus devices. J Spinal Disord Tech 16: 398–404. Link: https://bit.ly/3jfJ1tU
- Plais N, Girardi F (2020) Lateral Approaches to the Lumbar Spine. In: Lumbar Spine Online Textbook. International Society for the Study of the Lumbar Spine. Link: https://bit.ly/2UbYukk
- Pimenta L, Díaz RC, Guerrero LG (2006) Charité lumbar artificial disc retrieval: use of a lateral minimally invasive technique. Technical note. J Neurosurg Spine 5: 556–561. Link: https://bit.ly/3A8nzNh
- Wagner WH, Regan JJ, Leary SP, Lanman TH, Johnson JP, Rao RK, et al. (2006) Access strategies for revision or explantation of the Charité lumbar artificial disc replacement. J Vasc Surg 44: 1266–1272. Link: https://bit.ly/3qxk2nf
- Bendo JA, Quirno M, Errico T, Spivak JM, Goldstein J (2008) A comparison of two retroperitoneal surgical approaches for total disc arthroplasty of the lumbar spine. Spine 33: 205–209. Link: https://bit.ly/3dkOOux
- Hrabálek L, Wanek T, Adamus M (2010) XLIF--nová technika náhrady meziobratlové ploténky bederní pátere: první zkusenosti [XLIF--a new technique of the lumbar vertebra disc replacement: initial experience]. Rozhledy v chirurgii : mesicnik Ceskoslovenske chirurgicke spolecnosti 89: 784–788.
- Pimenta L, Oliveira L, Schaffa T, Coutinho E, Marchi L (2011) Lumbar total disc replacement from an extreme lateral approach: clinical experience with a minimum of 2 years' follow-up. Journal of neurosurgery 14: 38–45.
- Tohmeh AG, Smith WD (2015) Lumbar total disc replacement by less invasive lateral approach: a report of results from two centers in the US IDE clinical trial of the XL TDR® device. Eur Spine J 24: 331–338. Link: https://bit.ly/3h2pQCq
- Panjabi MM, Greenstein G, Duranceau J, Nolte LP (1991) Three-dimensional quantitative morphology of lumbar spinal ligaments. J Spinal Disord 4: 54–62. Link: https://bit.ly/3x37iqX
- Trincat S, Edgard-Rosa G, Geneste G, Marnay T (2015) Two-level lumbar total disc replacement: functional outcomes and segmental motion after 4 years. Orthop Traumatol Surg Res OTSR 101: 17–21. Link: https://bit.ly/2UJeD0O
- Pokorny G, Marchi L, Amaral R, Jensen R, Pimenta L (2019) Lumbar Total Disc Replacement by the Lateral Approach-Up to 10 Years Follow-Up. World Neurosurg 122: e325–e333. Link: https://bit.ly/2U6adRp
- Malham GM, Parker RM (2017) Early experience with lateral lumbar total disc replacement: Utility, complications and revision strategies. Journal of Clinical Neuroscience 39: 176–183. Link: https://bit.ly/3A7V4iG
- Janssen M, Garcia R, Miller L, Reed W, Zigler J, et al. (2017) Challenges and Solutions for Lumbar Total Disc Replacement Implantation. Spine 42: S108–S111. Link: https://bit.ly/3zZ77Pz
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
