International Journal of Spine Research
Prader-Willi Syndrome: Kyphoscoliosis is an underdiagnosed problem in young patients
Tahboub S1*, Gross-Tsur V2,3, Hirsch JH2,3 and Arzi H1,2
2The Israel Multidisciplinary Prader-Willi Syndrome Clinic, Shaare Zedek Medical Center, Jerusalem, Israel
3Department of Neuropediatrics, Shaare Zedek Medical Center, Jerusalem, Israel
Cite this as
Tahboub S, Gross-Tsur V, Hirsch JH, Arzi H (2021) Prader-Willi Syndrome: Kyphoscoliosis is an underdiagnosed problem in young patients. Int J Spine Res 3(1): 001-003. DOI: 10.17352/ijsr.000018Prader-Willi Syndrome (PWS) is a complex, neurogenetic, multisystem disorder with a prevalence of 1:15000 to 1:30000, caused by lack of expression of genes in the paternally inherited chromosome 15q 11.2-q13. In this report we aim to characterize and increase awareness of kyphoscoliosis in these children. Routine orthopedic examination for young children with PWS is essential in order to avoid medical complications and minimize the need for surgery.
Introduction
PWS is characterized by dysmorphic features, hypotonia, impaired satiety leading to morbid obesity, cognitive and behavioral abnormalities, endocrine disorders, and multiple orthopedic abnormalities. Almost all children receive growth hormone and vitamin D [1-3]. Orthopedic problems such as kyphoscoliosis, hip dysplasia and fractures due to osteopenia (22%) [4] are common in children and adolescents with PWS. The incidence and prevalence of scoliosis is approximately 40% and the prevalence increases with age (infants and juveniles: 30%, adolescents: 80%) [5-7]. Vertebral rotation is responsible for the asymmetry of the chest wall seen during forward bending, usually the first sign of scoliosis. Scoliosis is often diagnosed late in PWS due to less vertebral rotation than seen in other children with scoliosis [8]. The child with PWS may have a moderate curve radiographically, but only mild findings clinically [8]. Two types of scoliosis are identified [9]: 1) “Long C curve type” Scoliosis (LCS) which appears most commonly under four years of age and 2) “idiopathic” scoliosis (IS) which appears primarily around 10 years of age. Children with LCS are more hypotonic than those with IS [9]. Treatment of the spine deformity depends on age of presentation and curve magnitude. Conservative treatment using physiotherapy is recommended in infants younger than 3 years with curves under 20 degrees.
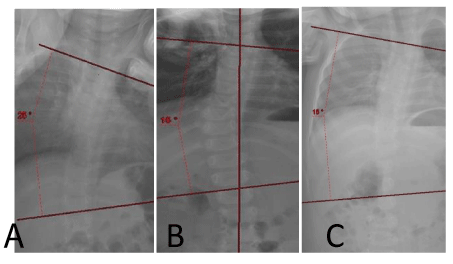
In our National Multidisciplinary PWS clinic we recently evaluated a one-year-old boy with PWS who was treated with growth hormone and vitamin D from 6 months of age. He had started to crawl but did not yet sit on his own. The parents noticed some asymmetry of his back and an orthopedic examination revealed upper thoracic lordosis and lower right thoracic hump. Cervical spine range of motion and hips were normal. Radiologic evaluation revealed a C-shaped scoliosis of 25 degrees (Figure 1-A) and some thoraco-lumbar kyphosis. He began a program of intensive physiotherapy and at 16 months an x-ray performed while sitting showed that the curve was reduced to 15 degrees (B) a curve that remained stable at a follow-up at 22 months (C).
Casting (Mehta technique) is recommended for curves above 20 degrees. Casts are changed every 2 months under the age of 2 and every 3 months in children over the age of 3. Bracing (Thoracic-Lumbar-Sacral Orthosis “TLSO”) should be considered for curves over 20 degrees in children under 10 years of age and for curves over 25 degrees in children 10 years or older. Follow-up out-of-brace radiographs should be obtained every 4 to 6 months [10].
Surgical intervention is usually needed in children with progressive scoliosis that cannot be maintained under 50 degrees. There are two types of expandable implants: “growth rods” or “Non-Fusion Spinal Instrumentation” (NFSI) and the “Vertical Expandable Prosthetic Titanium Rib” (VEPTR) device. Because of osteopenia in PWS, the NFSI which has greater hardware stability has been shown to be superior to VEPTR in this population [10]. Definitive spinal fusion should be performed for curves exceeding 50 degrees out-of- brace in older children since a curve of this size has a 95% chance of progressing, even after skeletal maturity. Since children with PWS may have delayed skeletal maturation, and it is advantageous to wait until 12 years of age for girls and 14 years for boys before performing definitive spinal fusion [8].
Overall, 15% of curves diagnosed before 4 years of age will eventually require surgical treatment and 41% of curves diagnosed after 4 years of age require surgical correction [8]. Conservative treatment should be the preferred treatment option for non-progressive scoliosis curves within certain limits (usually < 50 degrees), considering the lack of evidence for the long term outcome of surgery and the high risks of surgical intervention such as hardware failure due to osteopenia, skin picking and poor quality of the soft tissues resulting in high rates of wound dehiscence and related deep infections (19% and 38% of cases) [10,11]. Postoperatively PWS patients can experience life-threatening complications such as protracted ileus and stomach rupture due to overeating and chronic constipation. Because PWS individuals often suffer from sleep apnea (80%) and narcolepsy (30%) a pre-operative pulmonary evaluation including a sleep study is necessary to assess the need for BPAP or CPAP in the post-operative recovery period [10,12].
Discussion
Orthopedic examination should be part of the multidisciplinary approach for individuals with PWS. Routine spinal X-rays should begin when the child first sits independently. The goal should be to avoid surgery by means conservative treatment consisting of physiotherapy, casting and braces. It is important to remember that there is a high risk of complications in patients with PWS undergoing surgery and the benefits of surgery in this population remain controversial [9,12].
Conclusion
In order to diagnose kyphoscoliosis as early as possible in children with PWS, an annual systematic back examination is recommended in children less than four years of age [13]. The effect of growth hormone treatment on the natural history of scoliosis has not yet been determined, and careful monitoring during treatment is recommended [11,14]. With early diagnosis and conservative treatment, children with PWS and scoliosis may be able to avoid the need for surgical intervention with their possible complications.
- Cassidy SB, Schwartz S, Miller JL, Driscoll DJ (2012) Prader-Willi syndrome. Genet Med 14: 10-26. Link: https://bit.ly/3jqTRLH
- Fraccaro M, Zuffardi O, Buhler EM, Jurik LP (1977) 15/15 translocation in Prader-Willi syndrome. J Med Genet 14: 275-276. Link: https://bit.ly/36REh6x
- Mattei JF, Mattei MG, Giraud F (1983) Prader-Willi syndrome and chromosome 15. A clinical discussion of 20 cases. Hum Genet 64: 356-362. Link: https://bit.ly/3jrOlbD
- Gross-Tsur V, Altarescu G, Eldar-Geva T, Pollak Y, Hirsch HJ (2016) The Incidence of Fractures in Prader Willi Syndrome across the Age Spectrum. J Pediatric Endocrinol 1: 1008.
- van Bosse HJP, Butler MG (2020) van Bosse and Merlin G. Butler: Clinical Observations and Treatment Approaches for Scoliosis in PWS. Genes 11: 260. Link: https://bit.ly/2YSB2HB
- Nagai T, Obata K, Ogata T, Murakami N, Katada Y, et al. (2006) Growth hormone therapy and scoliosis in patients with Prader-Willi syndrome. Am J Med Genet A 140: 1623-1627. Link: https://bit.ly/2YWgy0U
- Kroonen LT, Herman M, Pizzutillo PD, Macewen GD (2006) Prader-Willi syndrome: clinical concerns for the orthopaedic surgeon. J Pediatr Orthop 26: 673-679. Link: https://bit.ly/3aDGROM
- van Bosse HJP (2010) Guidelines on Scoliosis Monitoring and Treatment for Children with Prader-Willi Syndrome. PWSA. Link: https://bit.ly/2Z1iZ1X
- Accadbled F, Odent T, Moine A, Chau E, Glorion C, et al. (2008) Complications of scoliosis surgery in Prader-Willi syndrome. Spine 33: 394-401. Link: https://bit.ly/3p7qyiB
- , Butler MG (2020) Clinical Observations and Treatment Approaches for Scoliosis in PWS. Genes 11: 260. Link: https://bit.ly/3aNayNg
- Weiss HR (2007) Is there a body of evidence for the treatment of patients with Adolescent Idiopathic Scoliosis (AIS)? Scoliosis 2: 19. Link: https://bit.ly/2LA9Ri0
- Oore J, Connell B, Yaszay B, Samdani A, Hilaire TS, et al. (2019) Growth friendly surgery and serial cast correction in the treatment of early onset scoliosis for patients with Prader-Willi syndrome. J Pediatr Orthop 39: e597–e601. Link: https://bit.ly/3aI9mej
- Weiss HR (2007) Best Practice in conservative scoliosis care. 2nd edition. Edt. Pflaum, Munich 2007 .
- (2002) Disease management of Prader-Willi syndrome. Expert Opin pharmacother 3: 1451-1459. Link: https://bit.ly/3rxW7ni
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
