International Journal of Spine Research
Criteria for radiological evaluation of incorporation of stand-alone expandable cervical vertebral body replacement devices
Hassan Allouch1*, Sándor Kónya2, Mootaz Shousha1,3 and Heinrich Boehm1
2Zentralklinik Bad Berka, Center for Diagnostic & Interventional Radiology and Neuroradiology, Bad Berka, Germany
3Department of Orthopedics, Alexandria University, Alexandria, Egypt
Cite this as
Allouch H, Kónya S, Shousha M, Boehm H (2020) Criteria for radiological evaluation of incorporation of stand-alone expandable cervical vertebral body replacement devices. A technical note and preliminary report. Int J Spine Res 2(1): 046-050. DOI: 10.17352/ijsr.000013Introduction: Corpectomy is an important treatment option for various cervical pathologies and evaluation of treatment success on imaging can be even more difficult than for interbody fusion. Since for routine postoperative courses CT scanning seems not justified for evaluation of the fusion status this paper proposes markers for detailed evaluation of new on plain radiographs.
Methods: In a retrospective analysis of prospectively collected consecutive patients were included from whom a minimum 2 year clinical and radiological follow-up was available of stand-alone VBR after cervical corpectomy for degenerative stenosis. All patients received an expandable cage of rectangular shape. For assessment of bony incorporation of VBR devices we introduce the footprint sign in addition to McAfee´s sentinel sign. Three observers evaluated the lateral x-rays of the patients.
Results: 36 male and 33 female patients (mean age 61,9 years) underwent one-, two- or three-level anterior cervical corpectomy and fusion (29, 31 and 9 patients respectively). Radiological outcome was assessed at a mean follow-up of 44.5 months. Combined cranial and caudal footprint sign denoting fusion could be detected in 94% of the cases. A positive sentinel sign anterior or posterior was denoting fusion in 47 out of 68 evaluable cases. Four cases (5.9%) showed no sufficient anterior or posterior bridging after 2 years and were rated as pseudoarthrosis.
Conclusion: For routine patients with no or minor symptoms after cervical VBR the sentinel- and footprint-sign on standard x-rays is a good indicator of successful treatment. Once reached no additional (flex-ex or CT) diagnostics seems necessary.
Introduction
There is consensus that solid bony fusion yields the best long-term solution for severely diseased index levels. There is disagreement whether and to what extent Vertebral Body Replacement (VBR) devices are incorporated - or even are hindering bony bridging. This is a particular concern in expandable VBR, which reduce fusion space due to the necessary extension mechanism. Depending on design of those implants the fixation to anchor vertebrae does cost further space. In the cervical spine the relation of implant vs. vertebral body volume is particularly unfavourable, which can be a reason for undesired outcomes or failures.
Above that the number of interbody-fusion procedures performed worldwide stands in substantial contrast to the number of consented methods for evaluation of treatment success. In a systematic review [1], tried to determine the best criteria for radiological determination of postoperative anterior subaxial cervical fusion. The authors found only moderate evidence that the interspinous process distance method is more reliable than either the Cobb angle method or the evaluation of a static radiograph for bridging bone. When embarking on measuring the interspinous process distance in flexion-extension x-rays they recommend to “set at less than 1 mm for the determination of fusion on plain radiographs”. Evaluating advanced imaging methods they found that CT scans seem to be superior to the interspinous process distance method but do caution in respect of increased radiation and the risk of overestimation of the presence of fusion. Other authors did confirm this problem, particularly in the early postoperative phase [2-4]. There is evidence that with any method the reliability of assessing cervical fusion improves with the time span elapsed from the index procedure.
These aspects taking into account and acknowledging the fact, that corpectomy defects as well as implants are larger and fusion supposedly more difficult to determine than in interbody situations this paper proposes a more detailed evaluation of new bone formation on plain radiographs. Besides the sentinel sign, introduced by McAfee [5], we introduce bony incorporation of either corner of a VBR interfacing the host as the Footprint Sign (FS). To our knowledge this is the first study that in detail evaluates bony incorporation of expandable VBR in the cervical spine.
Methods
In this study the authors systematically evaluated postoperative radiographs of patients who underwent purely stand-alone VBR after cervical corpectomy. The aim of this study was to determine the interobserver agreement on the stage of the incorporation and bony fusion of the grafted material with the help of a novel radiological sign, termed footprint sign. The form of the study was a retrospective analysis of prospectively collected cases, the study cohort comprised a total of 69 consecutive patients. Only those individuals were included from whom a minimum 2 year clinical and radiological follow-up was available. Underlying pathology was degenerative cervical stenosis in every case. In order to have a “pure sample” all cases with additional anterior or posterior fixation devices (e.g. anterior plates, posterior rod-screw systems as used in instability cases) were excluded. Likewise those patients with hybrid solutions of corpectomy plus adjacent interbody cages were not included. The study was approved by the local ethics committee.
The operation strategy was alike in all cases. Standard decompression technique as described by our previous study [6]. The VBR utilized in all cases was an expandable cage of rectangular shape with a design that requires resection only of the median third of the stenotic vertebral bodies. This usually allows a sufficient and safe approach for decompression of retrocorporal and foraminal bony stenosis while retaining a large surface of vascular bone alongside of the VBR. After thorough decompression the resulting barrel-shaped defect was closed and the spinal cord shielded by insertion and expansion of the implant. Due to the open design during all stages of insertion and extension the dura can be controlled under direct vision, which proved advantages particularly in the cervico-thoracic region where intraoperative lateral x-rays sometimes are inconclusive. The open design further allows decortication of the non-weight-bearing endplate-sections as well as filling with (corpectomy-derived) bone chips after the implant is positioned and spreaded to its final height. The amount of distraction was titrated to correct preoperative kyphosis and to fully engage the spikes of the implant´s footprints into the adjacent vertebrae. If after distraction the mechanical stability of the construct was regarded not sufficient, additional anchoring screws or fixation devices were applied; (the latter were excluded from this analysis).
In spite of the fact that bony incorporation in most cases was achieved earlier, only patients with a complete clinical and radiological 2y-FU were included in this study. The rationale behind this was to probe this method by identifying potential cases of false positive fusion judgment by comparing the postop course of footprint and sentinel sign over time.
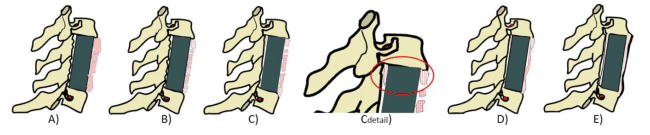
The most suitable approach for this observational study was to compare the interobserver agreement on the proposed sign and categorize the observations into binary categories. Three observers, 1 orthopedic surgeon, 1 neurosurgeon and one independent radiologist evaluated the lateral x-rays of all patients. In addition to the sentinel sign by McAfee [5] we proposed to use a cranial and caudal footprint sign as another sufficient criterion for fusion (Figure 1). Depending on the antero-posterior position or the antero-posterior size of the VBR a sentinel sign might be absent in spite a mechanically stable interfacing bone between implant and anchor vertebra. New bridging bone formation in comparison with previous postoperative images, detected around the anterior or posterior edge of the implant´s footprint, constitutes a cranial or caudal anterior or posterior footprint sign. Simultaneous occurrence of the footprint sign at both ends of the cage thus denotes absence of mechanical movability and can be regarded as fusion.
Results
Of 69 Patients with an average age of 61.9 years (ranging 41.1-83.0) 33 were female and 36 male. Degenerative stenosis was the exclusive pathology in this series, of which two patients suffered from pseudoarthrosis and persisting stenosis after ACDF. Clinical and radiological follow up was available for 2 to 9.9 years. One body was replaced in 29, two in 31 and 3 in 9 individuals; the locations are displayed in Table 1.
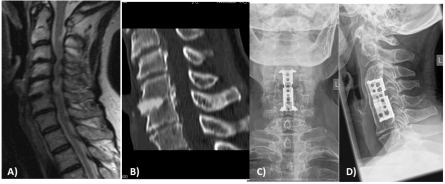
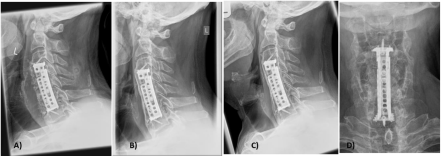
All surgeries had been performed under vision of an operative microscope. In 53 of the 69 patients anchoring screws fixing the implant to the adjacent vertebral body were used. The purchase of the footprint of the implant in the remaining 16 patients after expansion of the cage was considered that strong, that the surgeon did not add any anchoring screw for additional fixation (Figure 2). In all cases expandable titanium cages with a rectangular shape were used, however after the first 8 cases the locking mechanism was changed and this improved model used ever since. Since this adjustment did not involve any modification of the configuration or shape of the weight bearing parts of the cages, moreover the locking mechanism in both cases provided a firm, completely stable bonding, resulting in the same contour of the cage and equal filling volumes in both versions, we felt it justified to be included in this study on fusion/incorporation (Figure 3).
Assessment of fusion / incorporation was performed on lateral standing radiographs by 3 reviewers. The results of those two of them who remained blinded to the clinical situation, one an independent radiologist, are given in Table 2. That table notes the agreement after reevaluating differing judgements on the fusion status. Therefore in addition to the evaluation of the last x-ray of the follow up at mean 44,5 (24-120) months the complete postoperative series was analysed. In 2 cases an available CT scan confirmed the decision.
Combined cranial and caudal footprint sign denoting fusion could be detected in 95% of the cases. In six cases (9.7%) the caudal footprint could not be judged properly due to insufficient visibility of the posterior caudal interface. Four of these 6 however could be grouped according to a positive anterior sentinel sign.
A positive sentinel sign anterior or posterior was denoting fusion in 47 out of 68 evaluable cases. Four cases (5,9%) showed no sufficient anterior or posterior bridging after 2years and were rated as pseudoarthrosis.
Complications
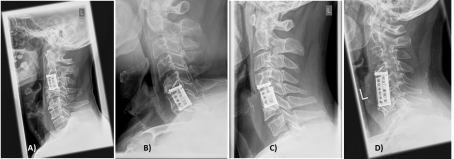
If one rates it as complication when the goal of bony fusion by the method proposed here could not be reached, then 4 patients with incomplete fusion have to be mentioned (Figure 4). Three out of four are single level corpectomies. The fact, that more than half (38 out of 69) of the patients required two- or three corpectomies the cage design seems to downsize the risk of increased complications in oligosegmental procedures as reported by authors using a cylindrical design [7]. An unsolved question – beyond the scope of this article-is, when an additional posterior fixation is indicated for the index procedure. Retrospectively in the cases A) and D) of figure 4 primary front and back surgery would have been well indicated.
Discussion
For many patients with few or even no symptoms it seems not justified to perform radiation-intensive diagnostics to prove restoration of full weight-bearing capacity. On the other hand for patient and physician the information is important to determine when after corpectomy the reconvalescence and treatment safely can end. Due to tremendous failure rates in the past with tricortical or fibular grafts [8-10] and less, but still significant in non-expandable cages [11,12], expandable cages were introduced. The mayor advantages over fixed length cages are greater ease of implantation with less risk of damage to the endplates and greater potential to restore lordosis. However in a metaanalysis [13], the additional risk is pointed out regarding too powerful expansion leading to overdistraction and increased subsidence. Though it was not the topic of this analysis, subsidence did occur in a substantial amount of patients. Usually it remained without consequences and did foster rather than impair bony incorporation. Regarding subsidence an important biomechanical aspect was raised [14] in proving reverse of load transfer through multilevel struts by anterior plating. The unloading effect in flexion and excessive load increase in extension due to an anterior plate seems to be an important trigger for overload and resulting complications of either implant or anchor vertebrae. Thus VBR with a design that do not require an anteriorly spanning plate are avoiding these additional sources of complications. Regarding fusion and ultimately bony incorporation of a VBR two aspects are beneficial: 1) a large contact area of vascularized bone with the implant and 2) short distances to be overcome for ongrowth and ingrowth of bone. Therefore, the design of the expandable cage should play an important role for fusion. This may be the reason why in actual study the finding of many authors, that complication rate increases significantly in more than 1 level corpectomies could not be confirmed regarding the topic of fusion: the nonunion after 2 years occurred after C3, C5 and C6 single corpectomy and one case where C5+C6 were replaced.
Regarding criteria of fusion the static radiography method is rated inferior to dynamic radiography with the interspinous process measurement method [4,15,16] and CT- based evaluation. In a detailed review [1] answers were sought for the questions: What is the accuracy and reliability of radiographs for assessing cervical fusion? Is there a superior plain radiographical method? And: What is the accuracy and reliability of advanced imaging methods for assessing cervical fusion? Is there a method superior to radiography? The authors recommend that flexion-extension radiographs using the interspinous process method (<1-mm motion difference) be the intitial method of determining subaxial anterior cervical fusion regardless of graft or instrumentation type. If further imaging is needed to assess anterior fusion on indeterminate radiographs, CT is recommended.
We agree to the safety concerns of these and other authors regarding the use of ionizing radiation wherever it seems not absolutely important for a patient´s treatment. We further find it difficult in clinical practice to ensure that flexion-extension images are produced reproducible enough to measure distances of less than a millimeter. Above that the advances of machine learning in image recognition are promising to draw more information out of the routine follow up imaging. We therefore tried to advance the methods of evaluation of static radiographs by systematic and detailed analysis of the implant-vertebral body-interface and in cases of doubt draw further information on the tendency of bone formation from previous imaging. The results, including the interobserver agreement values are promising and in our opinion warrant further studies with comparisons to more advanced imaging methods.Limitations
As with all studies, the current study had several limitations. First, the sample size was small and potential selection bias may exist due to the fact that hybrid and antero-posterior cases were excluded. Second a biological and geometric obstacle for comparison with solutions using anterior plates is the limited space anterior to the VBR in those conditions. Third, this was a retrospective study without a control group. A future multicenter study is planned in order to get a larger group of patients with an additional control group.
- Rhee JM, Chapman JR, Norvell DC, Smith J, Sherry NA, et al. (2015) Radiological Determination of Postoperative Cervical Fusion: A Systematic Review. Spine (Phila Pa 1976) 40: 974-991. Link: https://bit.ly/3itNbva
- Carreon LY, Glassman SD, Schwender JD, Subach BR, Gornet MF, et al. (2008) Reliability and accuracy of fine-cut computed tomography scans to determine the status of anterior interbody fusions with metallic cages. Spine J 8: 998-1002 Link: https://bit.ly/38qAn45
- Song KS, Chaiwat P, Kim JH, Mesfin A, Park SM, et al. (2013) Anterior cervical fusion assessment using reconstructed computed tomographic scans: surgical confirmation of 254 segments. Spine (Phila Pa 1976) 38: 2171-2177. Link: https://bit.ly/2ArKmd9
- Park DK, Rhee JM, Kim SS, Enyo Y, Yoshiok K (2015) Do CT scans overestimate the fusion rate after anterior cervical discectomy and fusion? J Spinal Disord Tech 28: 41-46. Link: https://bit.ly/3eWK2Sp
- McAfee PC, Boden SD, Brantigan JW, Fraser RD, Kuslich SD, et al. (2001) Symposium: a critical discrepancy-a criteria of successful arthrodesis following interbody spinal fusions." Spine (Phila Pa 1976) 26: 320-334. Link: https://bit.ly/2YW6C8i
- Shousha M, Ezzati A, Boehm H (2012) Four-level anterior cervical discectomies and cage-augmented fusion with and without fixation. Eur Spine J 12: 2512-2519. Link: https://bit.ly/38lSDMf
- Brenke C, Fischer S, Carolus A, Schmieder K, Ening G (2016) Complications associated with cervical vertebral body replacement with expandable titanium cages. J Clin Neurosci 32: 35-40. Link: https://bit.ly/31HsGoP
- Vaccaro AR, Balderston RA (1997) Anterior plate instrumentation for disorders of the subaxial cervical spine. Clin Orthop Relat Res 112-121. Link: https://bit.ly/2C2iTzb
- Sasso RC, Ruggiero RA, Reilly TM, Hall PV (2003) Early reconstruction failures after multilevel cervical corpectomy. Spine (Phila Pa 1976) 28: 140-142. Link: https://bit.ly/2C3UtoI
- Epstein NE (2012) Iliac crest autograft versus alternative constructs for anterior cervical spine surgery: Pros, cons, and costs. Surg Neurol Int 3: S143-156. Link: https://bit.ly/2BYV77d
- El Saghir H, Boehm H (2000) Anterior versus posterior plating in cervical corpectomy. Arch Orthop Trauma Surg 120: 549-554. Link: https://bit.ly/2Br2d4x
- Ji C, Yu S, Yan N, Wang J, Hou F, et al. (2020) Risk factors for subsidence of titanium mesh cage following single-level anterior cervical corpectomy and fusion. BMC Musculoskelet Disord 21: 32. Link: https://bit.ly/3dWC5vx
- Elder BD, Lo SF, Kosztowski TA, Goodwin RC, Lina IA, et al. (2016) A systematic review of the use of expandable cages in the cervical spine. Neurosurg Rev 39: 1-11. Link: https://bit.ly/38nOVBH
- DiAngelo DJ, Foley KT, Vossel KA, Rampersaud YR, Jansen TH (2000) Anterior cervical plating reverses load transfer through multilevel strut-grafts. Spine (Phila Pa 1976) 25: 783-795. Link: https://bit.ly/2NQU5Nh
- Tuli SK, Chen P, Eichler ME, Woodard EJ (2004) Reliability of radiologic assessment of fusion: cervical fibular allograft model. Spine 29: 856-860. Link: https://bit.ly/38mtn8q
- Song KS, Piyaskulkaew C, Chuntarapas T, Buchowski JM, Kim HJ, et al. (2014) Dynamic radiographic criteria for detecting pseudarthrosis following anterior cervical arthrodesis. J Bone Joint Surg Am 96: 557-563. Link: https://bit.ly/3eVD9RD
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
