International Journal of Radiology and Radiation Oncology
An isolated intra-cranial rosai-dorfman disease radiologically mimicking the meningioma
Imtiaz Ali*, Ashok Kumar, Rizwan Ajmal, Danial Khalid, Bushra Shamim and Mahum Zaidi
Cite this as
Ali I, Kumar A, Ajmal R, Khalid D, Shamim B, et al. (2022) An isolated intra-cranial rosai-dorfman disease radiologically mimicking the meningioma. Int J Radiol Radiat Oncol 8(1): 001-004. DOI: 10.17352/ijrro.000047Copyright License
© 2022 Ali I, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Rosai-Dorfman disease is an uncommon benign non-Langerhans cell histiocytosis proliferative disorder. It commonly involves the lymph nodes and is classically presented with massive cervical lymphadenopathy. It can also involve the extra-nodal sites of the body and is reported in 43% of Rosai-Dorfman disease cases. The central nervous system is rarely involved in Rosai-Dorfman disease from which intra-cranial is more common than spinal lesions. An isolated dural-based intra-cranial Rosai-Dorfman disease is extremely rare. It usually mimics meningioma on radiological imaging. It is very difficult to diagnose the Rosai-Dorfman disease on imaging and intra-operative appearances of the lesion. We present a histopathologically proven case of an isolated Rosai-Dorfman disease involving the central nervous system in 49 years old female patient which was radiologically mimicking the meningioma.
Introduction
Rosai-Dorfman disease is an uncommon lymphoproliferative benign non-Langerhans cells histiocytosis disorder with pathognomonic histological and immune-histo-chemical characteristics [1-15]. Typically patients present with non-specific painless, significant massive lymphadenopathy, commonly involving the cervical lymph nodes, less likely other lymph nodes including axillary, mediastinal, retroperitoneal, and inguinal regions. Other systematic symptoms include fever, malaise, weight loss, subcutaneous masses, bony pain, and anemia. Baseline investigations can show elevated Erythrocyte Sedimentation Level (ESR), inflammatory markers, leukocytosis, and polyclonal hypergamaglobulinima [1,2,4,9]. It is more commonly seen in children and young adults and rarely in older adults with no definite sex predilection. It can also involve the extra-nodal sites of the body and is reported in 43% of Rosai-Dorfman disease cases, most of which are skin and central nervous system [4]. Central nervous system is rarely involved in Rosai-Dorfman disease from which intra-cranial is more common than spinal lesions. Only a few cases have been reported in the spinal cord [5,6]. To the best of our knowledge isolated intra-cranial Rosai-Dorfman disease is extremely rare [5,15] Common presentation of CNS-Rosai-Dorfman disease is dural based extra-axial enhancing lesions on radiological imaging [15]. Therefore we highlight the histopathologically proven case of isolated Rosai-Dorfman disease presented to our hospital and was treated successfully.
Case report
49 years old female known case of diabetes mellitus presented to the outpatient department of neuro-medicine with complaints of on and off headache and nausea, she had also a history of one episode of generalized tonic-clonic seizures. Her general physical and neurological examinations were unremarkable. She was advised MRI of her brain with contrast to rule out the possibility of a space-occupying lesion or any other cause of headache.
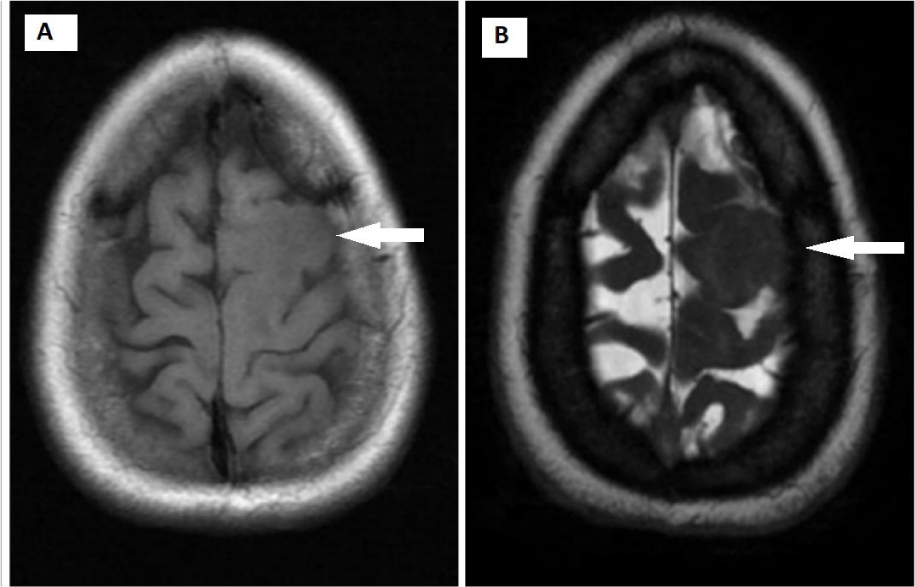
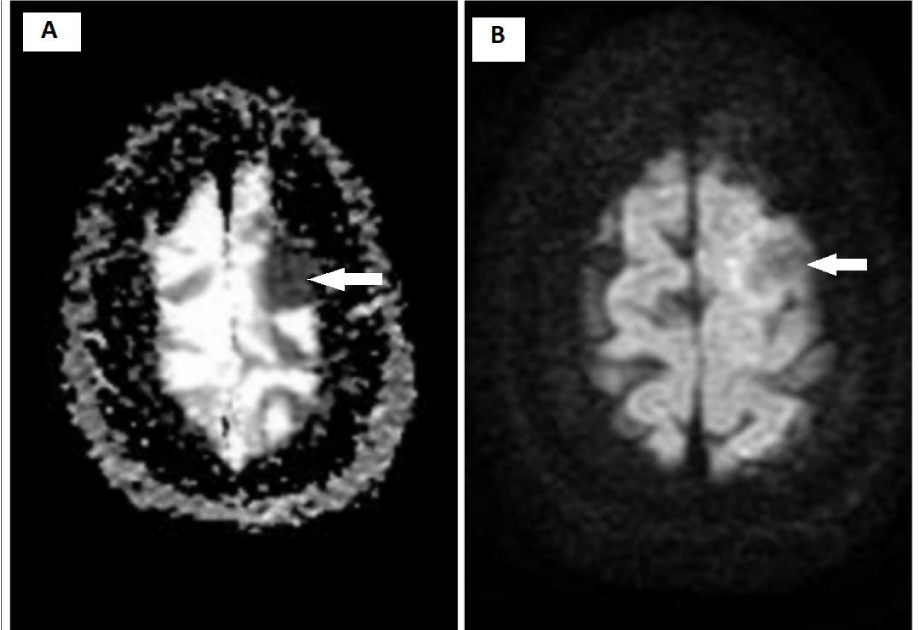
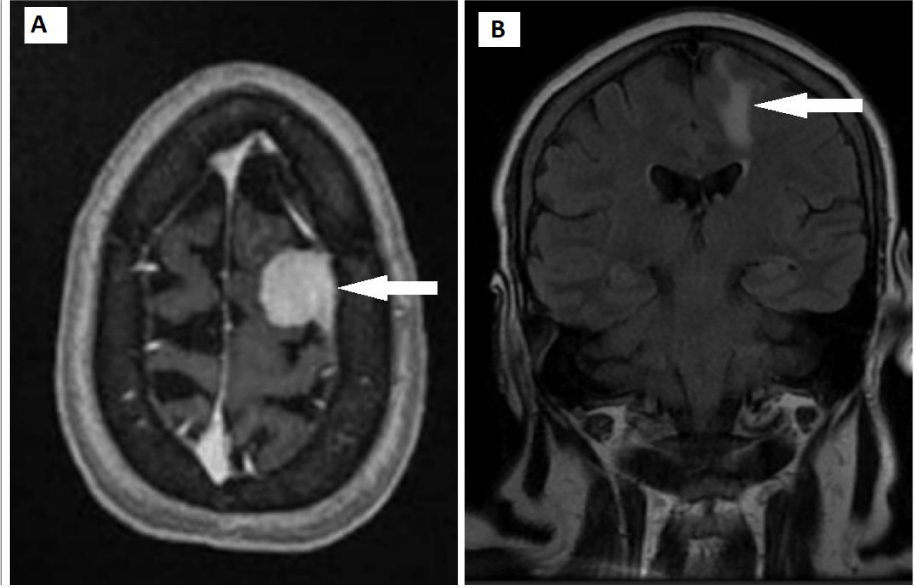
MRI brain with contrast showed an extra-axial, dural-based mass in the left superior frontal region. It appeared iso-intense on T1w and T2w images and showed homogenous enhancement on post-contrast images. This lesion was associated with gyriform finger-like edema of adjacent brain parenchyma on the Fluid Attenuated Inversion Recovery (FLAIR) image. There was no evidence of restricted diffusion on Apparent Diffusion Coefficient (ADC) and Diffusion-Weighted Image (DWI) images. (Figures 1-3). This was reported as Meningioma.
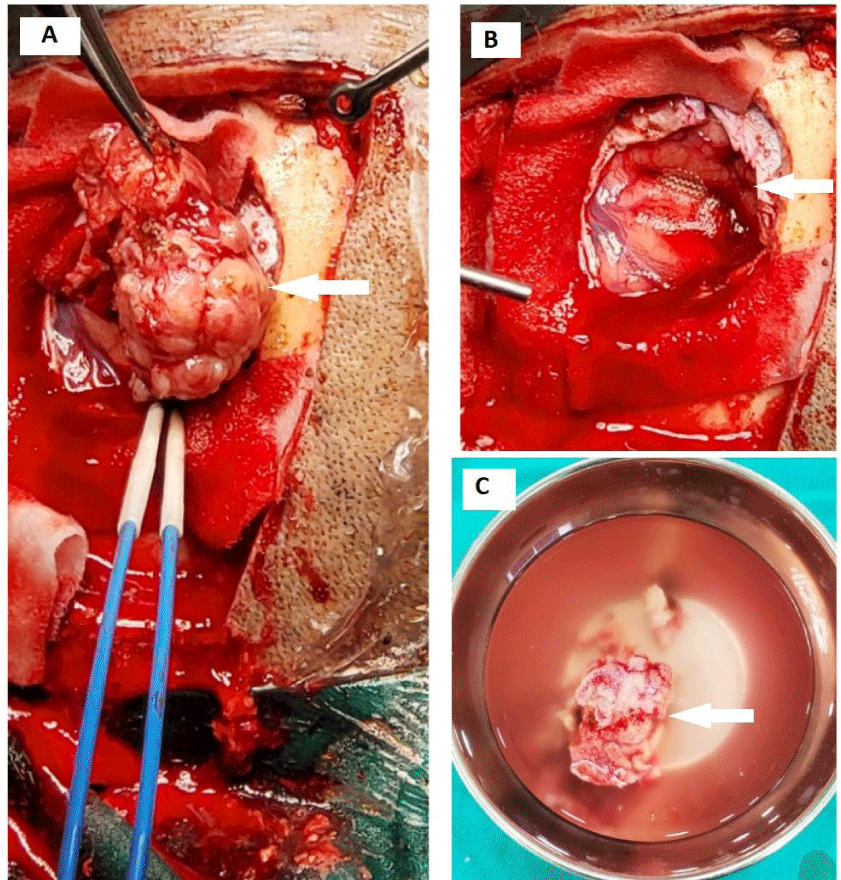
After baseline investigations, pre-operative workup, and general anesthesia fitness, she was booked for elective intracranial surgery and shifted to the operation theater. She underwent complete lesion excision and duraplasty. Her operative findings demonstrated well-circumscribed extra-axial mass inseparable from adjacent dura, close proximity to the falx cereberi relatively avascular, and hard in consistency slightly compressing the adjacent brain parenchyma. (Figure 4). The sample was sent for a histopathology examination.
Microscopic histopathological examination revealed brain tissue with a multi-nodular mass composed of dense mixed inflammatory infiltrates including large pale histiocytes, numerous lymphocytes, plasma cells, some neutrophils, and variable fibrosis. Periodic Acid-Schiff staining with diastase (PAS-D), Fite, Zeihl-Neelsen (ZN) were negative for infection organisms and von kossa was negative for Michaelis- Gutman bodies. Immunohistochemical studies demonstrated Positive S100 protein and CD 68. (Figure 5). This was reported as Rosai-Dorfman disease.
The patient was undergone Hybrid imaging Positron emission tomography, Computed Tomography (PET CT) examination of the whole body to rule out the possibility of lymphadenopathy as this is the common presentation of the disease. Positron emission tomography, Computed tomography (PET CT) showed no evidence of significant lymphadenopathy during the entire examination and recurrence or residual at the site of surgery (Figure 6). Therefore this intra-cranial lesion was considered an isolated CNS-Rosai-Dorfman disease. The patient had treated with adjuvant chemotherapy and corticosteroid drugs after surgery and she was followed in the Outdoor Patient Department (OPD) with no complaints of neurological symptoms and focal deficit. A Follow-up MRI brain with contrast showed no recurrent or residual lesion. (Not shown here).
Discussion
Rosai-Dorfman disease is a rare histiocytic disorder that was first reported in 1965 by Pierre Louis Lucien destombes [3,5,6,10] later by Rosai and Dorfman in 1969 as sinus histiocytosis with massive lymphadenopathy benign and lymphoproliferative disorder [3-6]. Extra-nodal involvement was discovered later in 1990 [11]. CNS-Rosai-Dorfman diseases is still rare presentation [11] It is an extremely uncommon disease with an incidence of about 1:200,000 peoples [6,4] commonly involve the cervical lymph nodes and less likely the axillary, mediastinal, retroperitoneal, and inguinal lymph nodes, predominantly affecting children and young adults (mean age is of 20.6 years) although it has been also reported in older age patients [3,4,7]. Rosai-Dorfman diseases can involve the nodal and extra-nodal sites [2]. Extra-nodal involvement is rarely seen in Rosai-Dorfman disease and has been reported in 43% of Rosai-Dorfman disease cases with the most common sites being skin, orbit, upper respiratory tract, bones, and CNS [4,14]. Less than 5% involvement is seen in CNS from which 75% in intra-cranial and 25% in spinal cord lesions [1,4,14]. CNS involvement in Rosai-Dorfman disease can be seen in both adult and pediatric population with a mean age of 39 years [1]. It usually presents as a dural-based lesion which can be single or multiple and mistakenly diagnosed as meningiomas on the radiological and clinical background and should be considered in differentials of meningiomas [1,8,9] Intracranial intra-axial lesions are extremely rare and mimicking the lymphoma or tuberculoma [1].
The typical presentation of the patient is bilateral non-tender massive cervical lymphadenopathy with less frequent involvement of peripheral lymph nodes and systematic constitutional symptoms like fever, weight loss, night sweet and malaise [1-3]. Laboratory analysis may show elevated ESR, leukocytosis, polyclonal hyper-globulinemia, normocytic or microcytic anemia [1,3,7]. In CNS-Rosai-Dorfman disease patient can present with seizures, focal neurological deficits, and weakness of lower limbs and headache depending on the size and location of the lesion [1].
Aetiopathology of the disease is still not clearly understood and is uncertain [4,5,14], several different theories in the literature described the causes of the disease [5]. Some literature had mentioned that dysfunction of the immune system, immunodeficiency, autoimmune diseases, infections, gene mutations, and the neoplastic process can be the causes of the disease [4,5] Some researchers had described that viruses such as the Epstein-Barr virus, and Human herpes virus may be associated with the occurrence of disease [1,5,7]. Rosai-Dorfman diseases are often misdiagnosed as Meningiomas on a radiological investigation like CT scan and MRI [1]. Therefore it is important to understand the features of Rosai-Dorfman disease on imaging. Meningiomas appear as hyper-iso-hypo intense on T2w images, with well-demarcated margins [1], bony changes like hyperostosis, bone destruction, or intra-lesional calcification. It appears as a hyper vascular lesion on Digital Subtraction Angiography (DSA) imaging [1]. While Rosai-Dorfman disease lesions are commonly hypointense on T2w images, with irregular margins or involvement of subarachnoid space, sulcal effacement, absence of adjacent bony changes like hyperostosis, and destruction. It appears as a hypovascular lesion on Digital subtraction angiography (DSA) imaging [1]. Both of these lesions appear as hyper-dense lesions on non-contrast CT scans and show homogenous post-contrast enhancement with perilesional edema of adjacent brain parenchyma [1]. On MRI examination best diagnostic radiological feature of Rosai-Dorfman disease is a hypo-intense lesion on T1w images due to high fibrous tissue. It can also show low relative cerebral blood flow (rCBV) on perfusion imaging. But these features are non-specific [1,5].
On pathological gross specimens, CNS-Rosai-Dorfman disease lesion appears as a hard, white, gray, or yellowish-brown color mass. A rapid pathological examination can still misdiagnose the lesion [13]. Final diagnosis is often on histology and immune-histo-chemistry [1,5,8,13] Microscopically hallmark of the disease is the emperipolesis phenomenon of lymphocytic cells with a background of plasma cells and lymphocytes [2,7]. Lymph nodes reveal the dilated sinuses with histiocytes and plasma cells [7]. These histiocytes express the CD68 and S-100 protein and negative CD1a [2,7].
There are multiple treatment options for Rosai-Dorfman disease that includes surgery, radiotherapy, chemotherapy and corticosteroids [5,8]. Clinical courses of the disease depend on the extent and distribution of the lesions involved in the various systems of the body [4]. The first therapeutic preferred treatment option for localized lesion or isolated CND-Rosai-Dorfman disease is surgical resection [1,12]. Intracranial surgical excision without any adjuvant therapy may show recurrence of disease because complete resection is not always possible [6,12]. Radiotherapy is a therapeutic option in case of post-surgical recurrences because CNS-RDD is radiosensitive [1]. The optimal or confined treatment strategy has yet to be determined [8,12,13]. Neurosurgical excision with radiosurgery is a better option for CNS-Rosai-Dorfman disease to obtain a favorable result and prognosis [6].
Conclusion
CNS-Rosai-Dorfman disease is difficult to diagnose on isolated radiological investigations and as well as macroscopically after surgical resection of the lesion. MRI brain with contrast shows dural-based lesions, it also definitively reveals the exact location and extent of the disease, but a definite diagnosis will be done on histopathological examination and immune-chemical examination. Once the diagnosis or differential diagnosis has been made as Rosai-Dorfman disease or Meningiomas, lesions must be treated with the surgical approach as same in cases of Meningiomas or other extra-axial lesions. Adjuvant chemotherapy and radiotherapy can be given in the case of CNS-Rosai-Dorfman disease to obtain better results and prognosis than just an isolated surgical approach. Therefore radiologists should keep in mind the differential diagnosis of CNS-Rosai-Dorfman disease in cases of meningioma, extra-axial lymphoma, and other dural-based lesions.
Ethical review
This case report was written and images of the patient’s scan were added after taking consent from the patient and the patient’s identity is not shown here and will be kept confidential.
- Varrassi M, Corridore A, Tommasino E, Saltelli G, Bruno F, et al. (2021) MR imaging of cerebral involvement of Rosai–Dorfman disease: a single-centre experience with review of the literature. Radiol Med 126: 89-98. Link: https://bit.ly/3DPJew1
- Wen JH, Wang C, Jin YY, Xu D, Jiang B, et al. (2019) Radiological and clinical findings of isolated meningeal Rosai–Dorfman disease of the central nervous system. Medicine 98: e15365. Link: https://bit.ly/3NRAHgF
- Bruce-Brand C, Schneider JW, Schubert P (2020) Rosai-Dorfman disease: an overview. J Clin Pathol 73: 697-705. Link: https://bit.ly/3x7PaiL
- Zhang Y, Liu J, Zhu J, Zhou X, Zhang K, et al. (2020) Case report: Rosai-Dorfman disease involving sellar region in a pediatric patient: a case report and systematic review of literature. Front Med (Lausanne) 7: 613756. Link: https://bit.ly/3r89zjK
- Xia L, Zhang L, Xiang Y, Liu L, Jing Z (2021) Intracranial Rosai-Dorfman disease mimicking isolated meningioma: a case report and review of the literature. Int J Clin Exp Pathol 14: 827-830. Link: https://bit.ly/3je3AG0
- Tatit RT, Raffa PE, de Almeida Motta GC, Bocchi AA, Guimaraes JL, et al. (2021) Rosai-Dorfman disease mimicking images of meningiomas: Two case reports and literature review. Surgical Neurology International 12. Link: https://bit.ly/3NWG9ig
- Aziz PA, Raja RA, Khimani V, Nasir Z, Aziz PA, et al. (2016) Isolated intracranial Rosai Dorfman disease without nodal involvement. 2016: 1972594. Link: https://bit.ly/3jgzXnc
- Raslan O, Ketonen LM, Fuller GN, Schellingerhout D (2008) Intracranial Rosai-Dorfman disease with relapsing spinal lesions. J Clin Oncol 26: 3087-3089. Link: https://bit.ly/38nNVl0
- Abdel-Razek M, Matter GA, Azab WA, Katchy KC, Mallik AA (2013) Isolated intracranial Rosai-Dorfman disease: report of two cases and a review of the literature. Turk Neurosurg 23: 509-513. Link: https://bit.ly/3r8sICf
- Lungren MP, Petrella JR, Cummings TJ, Grant GA (2009) Isolated intracranial Rosai-Dorfman disease in a child. American Journal of Neuroradiology 30: E148- E149. Link: https://bit.ly/3v3Tug8
- Adeleye AO, Amir G, Fraifeld S, Shoshan Y, Umansky F, et al. (2010) Diagnosis and management of Rosai–Dorfman disease involving the central nervous system. Neurol Res 32: 572-578. Link: https://bit.ly/38As5Lp
- Qin G, Ye J, Lan S, Liang Y, Xu P, et al. (2019) Rosai-Dorfman disease with spinal and multiple intracranial involvement: a case report and literature review. Br J Neurosurg 1-5. Link: https://bit.ly/3r6Yj7a
- Luo Z, Zhang Y, Zhao P, Lu H, Yang K, et al. (2017) Characteristics of Rosai-Dorfman disease primarily involved in the central nervous system: 3 case reports and review of literature. World Neurosurg 97: 58-63. Link: https://bit.ly/375VZqe
- Xu H, Zhang F, Lu F, Jiang J (2017) Spinal Rosai–Dorfman disease: case report and literature review. Eur Spine J 26: 117-127. Link: https://bit.ly/3r7PcDu
- Catalucci A, Lanni G, Ventura L, Ricci A, Galzio RJ, et al. (2012) A Rare Case of Intracranial Rosai-Dorfman Disease Mimicking Multiple Meningiomas: A Case Report and Review of the Literature. Neuroradiol J 25: 569-574. Link: https://bit.ly/3r4MsXm
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.



 Save to Mendeley
Save to Mendeley
