International Journal of Radiology and Radiation Oncology
Medulloblastoma
Indu Rekha Meesa*
Cite this as
Meesa IR (2019) Medulloblastoma. Int J Radiol Radiat Oncol 5(1): 015-016. DOI: 10.17352/ijrro.000034Introduction
Pediatric brain tumors are the most common solid tumors that develop in children second only to leukemia. They also account for the most cancer deaths in this patient population [1]. 7% of all the brain tumors that were diagnosed between 2006 and 2010 in the United States were in patients younger than 20 years of age [2]. Infratentorial tumors account for 45%-60% of brain tumors in children [3]. Some of the most common pediatric posterior fossa tumors are medulloblastoma, ependymoma, pilocytic astrocytoma, and atypical teratoid rhabdoid tumors. Medulloblastoma will be discussed in this paper.
Medulloblastoma
Medulloblastoma is the most common malignant brain tumor in childhood accounting for 40% of all posterior fossa tumors [4]. They are the most common tumor in the 6 to 11 year age group and comprise about 25% of brain tumors affecting children in that age range. They are highly malignant tumors composed of primitive, undifferentiated small, round cells [5].
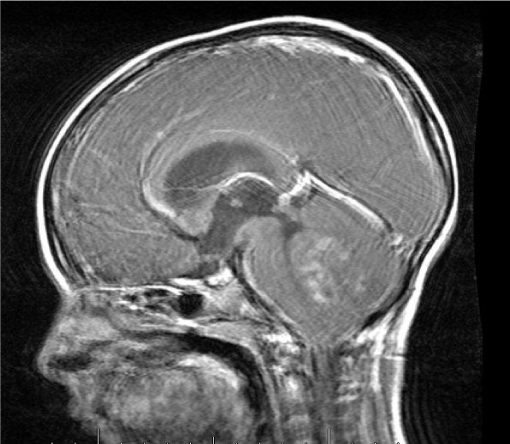
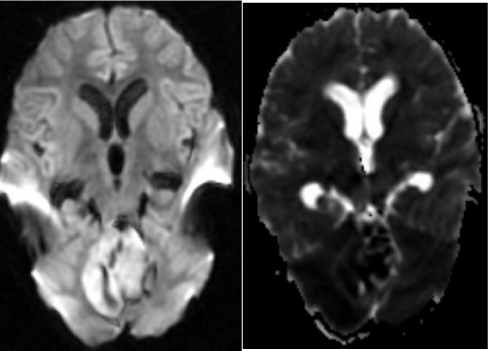
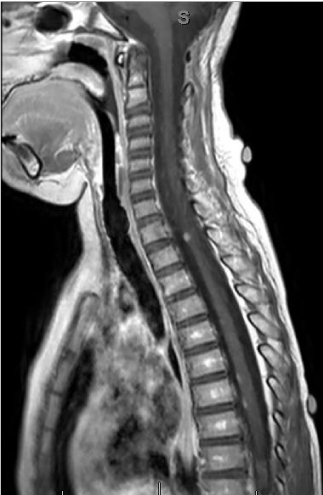
In general, they are midline tumors developing within the vermis and grow into the fourth ventricle. In adults and adolescents, the tumor can be located in the cerebellar hemispheres [6,7]. Common imaging features include a hyper dense mass on CT, low signal on T2 weighted MR images and enhancement following contrast administration [8]. Other features such as hemorrhage, necrosis, and cyst formation can be present but they are not distinguishing features from various subtypes or other tumors [9]. The entire craniospinal axis must also be screened to determine the extent of leptomeningeal involvement [10] (Figures 1-4).
It is important for the radiologist to be aware of some of the more common pediatric brain tumors and their imaging features in order to make an accurate diagnosis in a timely manner and recommend additional workup as needed.
Priyanka Meesa, Undergraduate student at Duke University
Akash Meesa, Undergraduate student at Duke University
- Gurney J, Smith M, Bunin G (1999) CNS and miscellaneous intra- cranial and intraspinal neoplasms. In: Ries L, Smith M, Gurney J (eds) Cancer incidence and survival among children and adolescents: United States SEER program 1975–1995 NIH publication no. 99–4649. National Cancer Institute SEER Program, Bethesda 51–63.
- Ostrom QT, Gittleman H, Farah P, Ondracek A, Chen Y, et al. (2013) CBTRUS statistical report: primary brain and central nervous system tumors diagnosed in the United States in 2006-2010. Neuro-Oncol 15:ii1-56. Link: http://bit.ly/38KpWaD
- Pollack IF (1994) Brain tumors in children. N Engl J Med 331: 1500-1507. Link: http://bit.ly/2U18qec
- Davis FG, McCarthy BJ (2000) Epidemiology of brain tumors. Curr Opin Neurol 13: 635-640.
- Rickert CH, Paulus W (2001) Epidemiology of central nervous system tumors in children and adolescence based on the new WHO classification. Childs Nerv Syst 17: 503-511. Link: http://bit.ly/2O3v15S
- Maleci A, Cervoni L, Delfini R (1992) Medulloblastoma in children and in adults: a comparative study. Acta Neurochir 119: 62-67. Link: http://bit.ly/2t5z7Dx
- Koci TM, Chiang F, Mehringer CM, Yuh WT, Mayr NA, et al. (1993) Adult cerebellar medulloblastoma: imaging features with emphasis on MR findings. Am J Neuroradiol 14: 929-939. Link: http://bit.ly/2uC4MNa
- Brandão LA, Young Poussaint T (2017) Posterior fossa tumors. Neuroimaging Clin N Am 27: 1-37. Link: http://bit.ly/31bbxC1
- Perreault S, Ramaswamy V, Achrol AS, Chao K, Liu TT, et al. (2014) MRI surrogates for molecular subgroups of medulloblastoma. Am J Neuroradiol 35: 1263-1269. Link: http://bit.ly/2vwcucl
- Hayes LL, Jones RA, Palasis S, Aguilera D, Porter DA (2012) Drop metastases to the pediatric spine revealed with diffusion-weighted MR imaging. Pediatr Radiol 42: 1009-1013. Link: http://bit.ly/37BD01V
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
