International Journal of Oral and Craniofacial Science
The effect of radiation dose on CBCT measurements of maxillary gingival thickness
Hiba Khateeb1, Eli E Machtei1,2 and Jacob Horwitz1,2*
2Department of Periodontology, School of Graduate Dentistry, Rambam Health Care Campus, Haifa, Israel
Cite this as
Khateeb H, Machtei EE, Horwitz J (2022) The effect of radiation dose on CBCT measurements of maxillary gingival thickness. Int J Oral Craniofac Sci 8(2): 026-031. DOI: 10.17352/2455-4634.000056Copyright License
© 2022 Khateeb H, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Purposes: 1. to measure Gingival Thickness (GT) both directly and with CBCT using various exposure times, and compare them. 2. to compare hard tissue measurements between different exposure times within each CBCT system. The study hypothesis was that accuracy of CBCT GT measurement is impaired when reducing exposure time. Methods: 8 fresh pig maxillae were utilized for each of two CBCT scan systems (SysA and SysB). Eight disposable dental needles were inserted into the gingival tissue of each jaw until reaching resistance from the underlying bone. A mark on each needle at its entrance point into the soft tissue was created using a permanent marker. Jaws were scanned twice, using low (RadL) and high (RadH) exposure times. The needles were extruded, and an electronic caliper was used to measure the length of the penetrated portion of the needle in mm (Cli). Radiographic GT was measured on cross sectional images, produced in the axial direcion of the 3D location of the needles (Rad) in two software systems (R and I). Descriptive statistics, t-test and ANOVA were performed. Significance was set at 5%. Results: Software I mean Cli was 2.22mm ± 0.54mm, RadL and RadH were 2.34mm ± 0.47mm and 2.34mm ± 0.52mm. Software R RadL and RadH were 2.16mm ± 0.50mm and 2.23mm ± 0.49mm, respectively. Using pairwise comparisons, both soft and hard tissue RadL and RadH were not statistically different. There was a good correlation between clinical and radiographic measurements of gingival thickness and essentially no significant difference between higher and lower radiation doses. Conclusions: Reducing CBCT radiation may be possible without affecting accuracy of radiographic gingival thickness measurements , thus opening the way to a wider utilization of CBCT in dentistry.
Clinical relevance: Reducing radiation dose may enable a wider utilization of CBCT in dentistry.
Abbreviations
3D: Three Dimensional; ANOVA: Analysis of Variance; CBCT: Cone Beam Computed Tomography; Cli: Clinical; DICOM: Digital Imaging and Communications in Medicine; SD: Standard Deviation; Mm: millimeter; Sec: Second
Introduction
Gingival thickness is generally accepted to be associated with health and stability of soft and hard tissues both around dental implants [1,2], and around teeth, especially when considering orthodontic therapy [3], periodontal plastic surgery [4] and fixed dental prosthesis [5]. Indeed, thickening of thin peri-implant keratinized mucosa by connective tissue grafting seems to reduce long-term recession around dental implants [6]. Treatment planning for soft tissue grafting requires direct clinical measurement of soft tissue thickness [7], which is an invasive and discomforting procedure; as such, alternative techniques may be more acceptable by patients and clinicians.
Cone beam computed tomography (CBCT) is used for examination and evaluation of the dento-facial region, including the developing and developed dentition, dental caries diagnosis, periodontal and periapical assessment, endodontics, dental trauma, and surgical applications, such as dental implants [8]. Although primarily indicated for osseous diagnosis, the usefulness of CBCT can be expanded at no additional investment to soft tissue assessment and gingival thickness measurements in particular [9-11].
CBCT incurs exposure to x-ray radiation, therefore, minimizing radiation dose is an essential component of its application [12]. CBCT systems have pre-defined protocols using various exposure times; however, there is currently no data on the effect of the lower exposure setting on soft tissue measurements. The importance of the study lies in the additional benefit to patients in using reduced radiation dose for soft tissue measurements alongside the principal indication of hard tissue diagnosis Therefore, the aim of the present study was to measure gingival thickness, both directly and in CBCT using various exposure times, and compare them.
The study hypothesis was that accuracy of CBCT to assess gingival thickness is impaired when reducing the radiation dose by shortening exposure times. The primary aims of the study were: 1. to quantitatively evaluate and compare clinical (trans-gingival) and radiographic buccal gingival thickness using high and low exposure protocols. 2. to evaluate radiographic gingival thickness measurements in two different CBCT scan systems. The present study focused on soft tissues, however, since CBCT is primarily intended for diagnosis of hard tissues, a secondary aim was to compare hard tissue measurements between different exposure times within each CBCT system in order to verify that lower exposure times did not negatively affect the accuracy of hard tissue measurements.
Materials and methods
The study was performed on fresh pig maxillary jaws which were obtained from a butchery. Scanning was done using two commercially available CBCT systems A (SysA)1 and B (SysB)<2. SysA radiographic data was then processed with a proprietary software associated with SysA<3 (I) as well as a stand-alone software4 (R). SysB data was processed only with software R.
___________________________
- 1i-CAT 17-19™ imaging system, 120kV, 3-7 mA and 0.5mm focal spot, 3600 rotation. Previously: I-CAT Imaging Sciences International, Inc. 2800 Crystal Drive, Hatfield, PA, 19440. Currently: KaVo Kerr, 200 S Kraemer Blvd, Building E2, Brea, CA 92821
- 2NewTom VGI EVO, 75-110 kV, 1-32 mA and 0.3mm focal spot 3600 rotation. CEFLA Società Cooperativa, Via Selice Provinciale N. 23/A Imola, Italy.
- 3iCat Vision, Imaging Sciences International, Inc. 2800 Crystal Drive, Hatfield, PA, 19440.
- 4RADIANT DICOM viewer, Medixant, Promienista 25, 60-288 Poznań, Poland
As a preliminary phase, six maxillae were utilized; each was measured twice by the same examiner (HK) for training and sample size calculation. Assuming 95% confidence level (CL), relying on the equation for sample size calculation: N≥(z/m)2×p(1−p) where N was used to describe the sample size, z received a value of 1.96 corresponding to the assumed 95% CL, while m represented margin of error, which in this case was approximated to be 5%, p represented the proportion which was assumed to be 5%; finally, 64 sites to be measured repeatedly for each experimental arm, would be needed for the study.
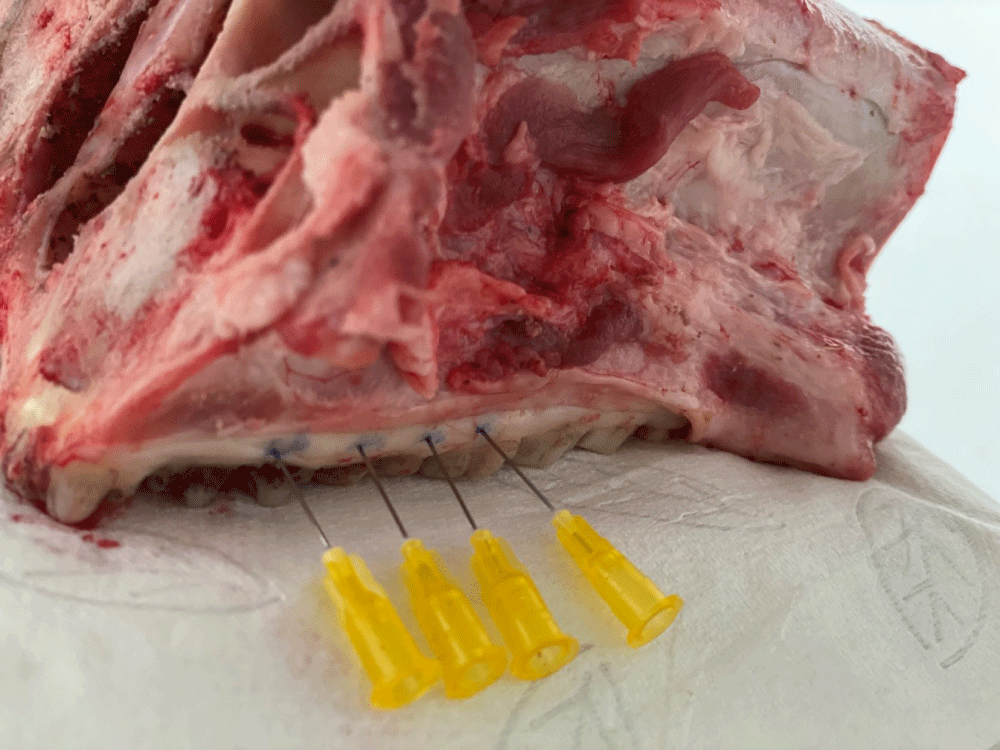
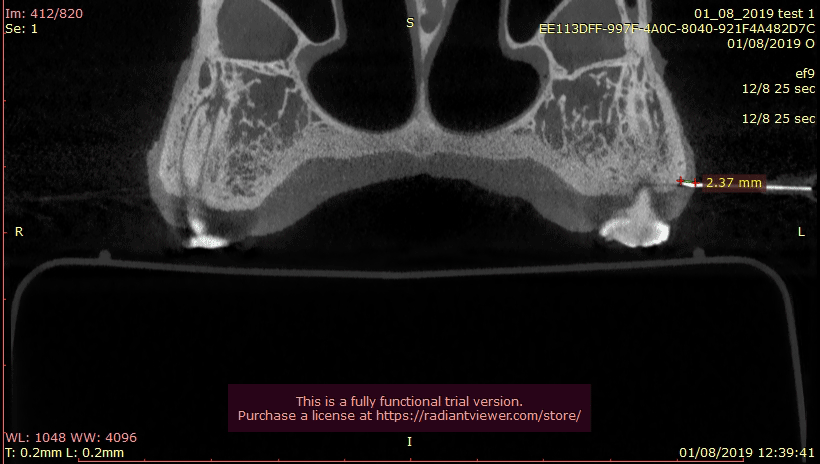
The study was performed on eight pig maxillary jaws. Eight disposable dental needles (Gauge 27) in each jaw were used for a total of 64 sites. Needles were inserted into the gingival tissue of the pig maxillary jaw until reaching resistance from the underlying bone. A mark on each needle at its entrance point into the soft tissue was made, using a permanent marker (Figure 1). Next, the jaws were scanned twice, using two scan protocols, defined as low exposure (Rad L) and High exposure (Rad H) protocols. System A protocols consisted of 8 seconds (18.54mAs, 120KVP) (RadL) and 26 sec (37.07mAs, 120KVP) (RadH). System B protocol settings were 18 seconds (12.97mAs, 110KVP) (RadL) and 25 seconds (18.01mAs, 110KVP) (RadH). Following scanning, the needles were extruded, and an electronic caliper5 was used to measure the length of the penetrated portion of the needle in millimeters (Cli) (Figure 2). DICOM files of the scans were then processed with software R (Figure 3). Additional measurements were also done using the proprietary I software for SysA only. The needles were identified in the CBCT by adjusting the cross sectional view parallel to the axis of the needle. Radiographic gingival thickness (in millimeters) was measured on cross sectional images, produced in the 3D location of the needles (RadL and RadH). All measurements were performed twice, tabulated6 and used for statistical analysis. Hard tissues were evaluated by measuring the width of cortical bone in CBCT images, using the location of the needle as a reference point. Hard tissue measurements in both exposure times were compared in each system. The two CBCT systems were in two separate facilities, therefore two separate groups of 8 jaws each were utilized for each CBCT system (16 jaws in total).
Statistical Analysis: Statistical analysis was performed using a statistical software7. Data was examined for normality using the Kolmogorov-Smirnov Test. Repeated measurements were compared using t-test. Once no significant differences were found, their average was computed and used for descriptive statistics. Analyses of variance (ANOVA) was used to compare the clinical and radiographic measurements. Results were expressed in mm as mean ± standard deviation (mean ± SD).
___________________________
- 5ABSOLUTE Digimatic Caliper, Mitutoyo, 965 Corporate Boulevard, Aurora, Illinois 60502
- 6Excel, Microsoft.
- 7SPSS statistical software,version 27 for Windows, International Business Systems Corp. New Orchard Road, Armonk, New York 10504.
Results
Soft tissue measurements
SysA radiographic data were examined with softwares I and R. Clinical and radiographic measurements were all normally distributed (using One-Sample Kolmogorov-Smirnov Test). There were no significant differences between repeated measurements (using t-test for repeated measurements), therefore, averages of repeated measurements were calculated and used for further statistical analyses.Average Cli was 2.22mm ± 0.54mm. Using software I, mean radiographic RadL gingival thickness was 2.34mm ± 0.47mm and mean RadH was 2.34mm ± 0.52mm. Software R respective measurements were, 2.16mm ± 0.50mm for RadL and 2.23mm ± 0.49mm. for RadH (Table 1). A one-way repeated measures ANOVA with Bonferroni adjustments revealed that Cli, RadL and RadH were all not statistically different (p = 0.073 and 0.067 for software I and software R, respectively) (Tables 2,3).
SysB radiographic data were examined with software R. using One-Sample Kolmogorov-Smirnov Test, clinical and radiographic data were not normally distributed (D =.16856, p = .046), however, mean, median and mode values were similar and graphs showed a symmetrical distribution pattern. Therefore, we used averages of repeated measurements for descriptive statistics and ANOVA. Cli was 2.27mm ± 0.54mm, compared to 2.17mm ± 0.49mm for RadL and 2.21mm ± 0.49mm for RadH (Table 1). ANOVA revealed a significant difference between Cli and RadL (p = 0.046) but not between Cli and RadH (p = 0.098) (Table 4).
Hard tissue measurements
Similar to the above, Sys A hard tissue measurements were examined with softwares I and R and Sys B data- with software R. All radiographic measurements were normally distributed (using One-Sample Kolmogorov-Smirnov Test), with no significant differences between repeated measurements (using t-test for repeated measurements), therefore, averages of repeated measurements were calculated and used for further pairwise comparisons (t-test). SysA Software I RadL was 2.31mm ± 0.55mm and RadH was 2.32mm ± 0.51mm. )p = 0.96); while for software R RadL was 2.32mm ± 0.54mm and RadH 2.32mm ± 0.50mm (p = 0.99). For SysB Software R RadL was 2.18mm ± 0.47mm and RadH was 2.25mm ± 0.52mm (p = 0.71), Table 5.
Discussion
In the present study, there was a good correlation between clinical and radiographic measurements of gingival thickness and essentially no significant difference between higher and lower doses in an experimental model consisting of pig jaws. Furthermore, there were no significant differences between two softwares. Also, and equally as important, there were no significant differences in hard tissue measurements between lower and higher radiation times. The study hypothesis was therefore refuted.
CBCT use in the dental profession has been constantly on the growth in recent years, increasing patient exposure to radiation hazards. Therefore, the aim of reducing radiation doses is of increasing importance and the present study results present a promising opportunity. The significant associations between soft tissue thickness and outcomes of periodontal treatments such as root coverage procedures [4] and implant therapy [13,14], highlight the importance of pre-treatment soft tissue assessment. CBCT is principally used for evaluating hard tissues but may be potentially used for non-invasive soft tissue evaluation as a secondary outcome. There have been several attempts to find an alternative to the invasive trans-gingival needle technique with varying success. Poor to weak agreement was found between photo assessment, a periodontal probe inserted inside the sulcus; and the real thickness measured with a needle [15]. In a human study there were no significant differences between a digital vernier caliper (invasive measurement) and ultrasonography [16], however, this method may be suitable only in experimental settings and not in clinical practice. Measuring radiographic gingival thickness was already shown to be accurate in a pig jaw model using a high-resolution high radiation dose [17]. In a study by Alves et al. comparing probe transparency, transgingival assessment (needle), photographic assessment and CT scanning in 12 patients, the best correlation was found between the CT and the trans-gingival method [18]. These results are in correlation with our study, in which differences between Cli and Rad were not statistically significant. In contrast, there were significant differences between CBCT and trans-gingival measurements with an acupuncture needle in an ex-vivo study that evaluated gingival thickness on incisors in 20 porcine mandibles [10]. The clinical significance, however, seems to be negligible (the mean difference CBCT-needle being 0.14mm). Efforts to reduce radiation dose are constantly being done in various medical disciplines such as orthopedics [19], trauma [20] as well as the dental field [21]. It seems that dose reduction is usually achieved by amperage reduction, use of partial rotations, reducing the number of projections, and increasing voxel sizes, but seldom by kV reduction or exposure time reduction [21]. In a 2016 systematic review of CBCT exposure parameters, mixed results were reported, but in the majority of studies altering the exposure parameters, including exposure time, had no impact on diagnostic accuracy or pathology detection [22]. In this review soft tissue assessment was not reported. Also, the authors graded most of the included studies as having a low/very-low GRADE score [23]. Since there is a 100 times difference in effective doses for different CBCT devices between the lowest and highest recommended doses [24], and considering all the above, further efforts should be made in low-dose radiation research.
In spite of the advantage of reduced radiation caution should be exercised when interpreting the results of the present study. CBCT was performed on maxillae and not entire heads, therefore there was significantly less interference from adjacent anatomical structures. Patients, differently from pig jaws, may have metal in dental implants and restorations, which produce significant artefacts that may affect radiographic interpretation. Cheek inflation during CBCT acquisition, similar to the study of Alves et al. (the patients closed their lips together and inflated their mouth during the scan to move cheek and lips away from the jaws) may be helpful in demarcation and separation of the gingiva from other soft tissues, thus improving accuracy. Finally, considering the wide variety of CBCT devices and protocols, the results of the present study should not be directly extrapolated to other CBCT systems. Further studies on methods to reduce radiation dose should assess CBCT image quality from regarding technical image quality as well as the diagnostic point of view. The strenght of the present study is its uniform data collection while the major weakness is the in vitro nature of the study which excluded some major confounders, such as patient movement, artifacts that may affect clear identification of gingival margins (dental restorations, lips, cheeks). Therefore further clinical studies should be performed before extrapolating the results to clinical practice.
In conclusion, reduction in radiation dose during CBCT scans may be possible without affecting accuracy of radiographic gingival thickness measurements and thus opens the way to a wider utilization of CBCT in dentistry.
The authors gratefully acknowledge the assistance of Ms. Ronit Leiba, Bio-statistician, from the Unit of Epidemiology at the Rambam Health Care Campus, for the statistical analysis.
Compliance with ethical standards
Conflict of Interest: Author HK, EEM and JH declare that they have no conflict of interest.
Funding: The work was self-funded.by the authors.
Ethical approval: This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent: For this type of study, formal consent is not required.
Author contribution
Heba Khateeb: Data curation, formal analysis, investigation, methodology and validation.
Eli E Machtei: Conceptualization, supervision, writing-review and editing.
Jacob Horwitz: Conceptualization, formal analysis, methodology, supervision, visualization, writing-original draft, review and editing.
- Thoma DS, Naenni N, Figuero E, Hämmerle CHF, Schwarz F, Jung RE, Sanz-Sánchez I. Effects of soft tissue augmentation procedures on peri-implant health or disease: A systematic review and meta-analysis. Clin Oral Implants Res. 2018 Mar;29 Suppl 15:32-49. doi: 10.1111/clr.13114. PMID: 29498129.
- Saglanmak A, Gultekin A, Cinar C, Szmukler-Moncler S, Karabuda C. Effect of soft tissue thickness on crestal bone loss of early loaded implants with platform switching: 1- and 5-year data. Quintessence Int. 2021;0(0):426-433. doi: 10.3290/j.qi.b912613. PMID: 33491391.
- Ashfaq M, Sadiq A, Sukhia RH, Fida M. Association of hard and soft tissue factors with gingival recession in orthodontically treated patients: A retrospective study. Int Orthod. 2021 Mar;19(1):60-66. doi: 10.1016/j.ortho.2020.12.001. Epub 2020 Dec 30. PMID: 33388278.
- Holtzman LP, Blasi G, Rivera E, Herrero F, Downton K, Oates T. Gingival Thickness and Outcome of Periodontal Plastic Surgery Procedures: A Meta-regression Analysis. JDR Clin Trans Res. 2021 Jul;6(3):295-310. doi: 10.1177/2380084420942171. Epub 2020 Jul 27. PMID: 32718265.
- Avetisyan A, Markaryan M, Rokaya D, Tovani-Palone MR, Zafar MS, Khurshid Z, Vardanyan A, Heboyan A. Characteristics of Periodontal Tissues in Prosthetic Treatment with Fixed Dental Prostheses. Molecules. 2021 Mar 2;26(5):1331. doi: 10.3390/molecules26051331. PMID: 33801337; PMCID: PMC7958327.
- Avetisyan A, Markaryan M, Rokaya D, Tovani-Palone MR, Zafar MS, Khurshid Z, Vardanyan A, Heboyan A. Characteristics of Periodontal Tissues in Prosthetic Treatment with Fixed Dental Prostheses. Molecules. 2021 Mar 2;26(5):1331. doi: 10.3390/molecules26051331. PMID: 33801337; PMCID: PMC7958327.
- Manjunath RG, Rana A, Sarkar A. Gingival Biotype Assessment in a Healthy Periodontium: Transgingival Probing Method. J Clin Diagn Res. 2015 May;9(5):ZC66-9. doi: 10.7860/JCDR/2015/13759.5956. Epub 2015 May 1. PMID: 26155566; PMCID: PMC4484158.
- European Commission. Evidence-Based Guidelines on Cone Beam CT for Dental and Maxillofacial Radiology. Office for Official Publications of the European Communities. Radiation Protection 172: 2012; Cited December 2013. http://ec.europa.eu/energy/nuclear/radiation_protection/doc/publication/172.pdf.
- Fourie Z, Damstra J, Gerrits PO, Ren Y. Accuracy and reliability of facial soft tissue depth measurements using cone beam computer tomography. Forensic Sci Int. 2010 Jun 15;199(1-3):9-14. doi: 10.1016/j.forsciint.2010.02.018. Epub 2010 Mar 16. PMID: 20236780.
- Gkogkos A, Kloukos D, Koukos G, Liapis G, Sculean A, Katsaros C. Clinical and Radiographic Gingival Thickness Assessment at Mandibular Incisors: an Ex Vivo Study. Oral Health Prev Dent. 2020 Jun 8;18(1):607-617. doi: 10.3290/j.ohpd.a44925. PMID: 32700514.
- Wang J, Cha S, Zhao Q, Bai D. Methods to assess tooth gingival thickness and diagnose gingival phenotypes: A systematic review. J Esthet Restor Dent. 2022 Jun;34(4):620-632. doi: 10.1111/jerd.12900. Epub 2022 Mar 16. PMID: 35297167.
- Horner K, Islam M, Flygare L, Tsiklakis K, Whaites E. Basic principles for use of dental cone beam computed tomography: consensus guidelines of the European Academy of Dental and Maxillofacial Radiology. Dentomaxillofac Radiol. 2009 May;38(4):187-95. doi: 10.1259/dmfr/74941012. PMID: 19372107.
- Giannobile WV, Jung RE, Schwarz F; Groups of the 2nd Osteology Foundation Consensus Meeting. Evidence-based knowledge on the aesthetics and maintenance of peri-implant soft tissues: Osteology Foundation Consensus Report Part 1-Effects of soft tissue augmentation procedures on the maintenance of peri-implant soft tissue health. Clin Oral Implants Res. 2018 Mar;29 Suppl 15:7-10. doi: 10.1111/clr.13110. PMID: 29498127.
- Tavelli L, Barootchi S, Avila-Ortiz G, Urban IA, Giannobile WV, Wang HL. Peri-implant soft tissue phenotype modification and its impact on peri-implant health: A systematic review and network meta-analysis. J Periodontol. 2021 Jan;92(1):21-44. doi: 10.1002/JPER.19-0716. Epub 2020 Aug 9. PMID: 32710810.
- Aguilar-Duran L, Mir-Mari J, Figueiredo R, Valmaseda-Castellón E. Is measurement of the gingival biotype reliable? Agreement among different assessment methods. Med Oral Patol Oral Cir Bucal. 2020 Jan 1;25(1):e144-e149. doi: 10.4317/medoral.23280. PMID: 31880279; PMCID: PMC6982987.
- Sharma S, Thakur SL, Joshi SK, Kulkarni SS. Measurement of gingival thickness using digital vernier caliper and ultrasonographic method: a comparative study. J Investig Clin Dent. 2014 May;5(2):138-43. doi: 10.1111/jicd.12026. Epub 2013 Jan 25. PMID: 23355379.
- Lau SL, Chow LK, Leung YY. A Non-Invasive and Accurate Measurement of Gingival Thickness Using Cone-Beam Computerized Imaging for the Assessment of Planning Immediate Implant in the Esthetic Zone-A Pig Jaw Model. Implant Dent. 2016 Oct;25(5):619-23. doi: 10.1097/ID.0000000000000437. PMID: 27280737.
- Alves PHM, Alves TCLP, Pegoraro TA, Costa YM, Bonfante EA, de Almeida ALPF. Measurement properties of gingival biotype evaluation methods. Clin Implant Dent Relat Res. 2018 Jun;20(3):280-284. doi: 10.1111/cid.12583. Epub 2018 Jan 19. PMID: 29350855.
- Yel I, Booz C, Albrecht MH, Gruber-Rouh T, Polkowski C, Jacobi M, Lenga L, Schulz M, Frank J, Marzi I, Vogl TJ, Eichler K, Kaltenbach B. Optimization of image quality and radiation dose using different cone-beam CT exposure parameters. Eur J Radiol. 2019 Jul;116:68-75. doi: 10.1016/j.ejrad.2019.04.005. Epub 2019 Apr 22. PMID: 31153576.
- Hooper T, Eccles G, Milliken T, Mathieu-Burry JR, Reed W. Dose reduction in CT imaging for facial bone trauma in adults: A narrative literature review. J Med Radiat Sci. 2019 Jun;66(2):122-132. doi: 10.1002/jmrs.319. Epub 2019 Feb 1. Erratum in: J Med Radiat Sci. 2019 Dec;66(4):300. PMID: 30706691; PMCID: PMC6545476.
- Yeung AWK, Jacobs R, Bornstein MM. Novel low-dose protocols using cone beam computed tomography in dental medicine: a review focusing on indications, limitations, and future possibilities. Clin Oral Investig. 2019 Jun;23(6):2573-2581. doi: 10.1007/s00784-019-02907-y. Epub 2019 Apr 25. PMID: 31025192.
- Goulston R, Davies J, Horner K, Murphy F. Dose optimization by altering the operating potential and tube current exposure time product in dental cone beam CT: a systematic review. Dentomaxillofac Radiol. 2016;45(3):20150254. doi: 10.1259/dmfr.20150254. Epub 2016 Jan 6. PMID: 26732433; PMCID: PMC4846147.
- Guyatt GH, Oxman AD, Vist GE, Kunz R, Falck-Ytter Y, Alonso-Coello P, Schünemann HJ; GRADE Working Group. GRADE: an emerging consensus on rating quality of evidence and strength of recommendations. BMJ. 2008 Apr 26;336(7650):924-6. doi: 10.1136/bmj.39489.470347.AD. PMID: 18436948; PMCID: PMC2335261.
- Bornstein MM, Scarfe WC, Vaughn VM, Jacobs R. Cone beam computed tomography in implant dentistry: a systematic review focusing on guidelines, indications, and radiation dose risks. Int J Oral Maxillofac Implants. 2014;29 Suppl:55-77. doi: 10.11607/jomi.2014suppl.g1.4. PMID: 24660190.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.



 Save to Mendeley
Save to Mendeley
